- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
This guide provides an overview of the recognition and immediate management of opioid overdose using an ABCDE approach.
The ABCDE approach is used to systematically assess an acutely unwell patient. It involves working through the following steps:
- Airway
- Breathing
- Circulation
- Disability
- Exposure
Each stage of the ABCDE approach involves clinical assessment, investigations and interventions. Problems are addressed as they are identified, and the patient is re-assessed regularly to monitor their response to treatment.
This guide has been created to assist healthcare students in preparing for emergency simulation sessions as part of their training. It is not intended to be relied upon for patient care.
Opioids and opioid overdose
Opioid abuse is a significant global problem. The World Health Organisation (WHO) estimates that 500,000 deaths worldwide are attributed to drug use, with more than 21% attributed to opioid overdose.
The terms opiate and opioid are often used interchangeably. However, they have different meanings:
- An opiate is a naturally occurring alkaloid drug derived from the opium poppy (e.g. morphine and codeine)
- An opioid is any synthetic or semi-synthetic drug derived from the opium poppy (e.g. fentanyl and oxycodone)
Opioid is used as the broad term for any substance that binds opioid receptors to produce an opiate-like toxidrome.
Clinical features
The typical triad of features in an opioid overdose is:
- Decreased level of consciousness
- Respiratory depression
- Pin-point pupils (miosis)
Other symptoms may include:
- Nausea
- Vomiting
- Confusion
Suspecting an opioid overdose
Opioid overdose can occur in several distinct patient groups:
- Individuals with a history of drug use
- Patients who have been prescribed opioid medications, including those currently admitted to hospital: especially elderly patients and those with reduced renal function
- Cases of deliberate self-harm
It is crucial to always consider the possibility of opioid overdose in any patient presenting with a reduced level of consciousness.
Tips before you begin
General tips for applying an ABCDE approach in an emergency setting include:
- Treat problems as you discover them
- Re-assess regularly and after every intervention to monitor a patient’s response to treatment
- If the patient loses consciousness and there are no signs of life, put out a crash call and commence CPR
- Make use of the team around you by delegating tasks where appropriate
- All critically unwell patients should have continuous monitoring equipment attached
- Clearly communicate how often you would like the patient’s observations relayed to you by other staff members
- If you require senior input, call for help early using an appropriate SBAR handover
- Review results as they become available (e.g. laboratory investigations)
- Use local guidelines and algorithms to manage specific scenarios (e.g. acute asthma)
- Any medications or fluids must be prescribed at the time (you may be able to delegate this to another staff member)
- Your assessment and management should be documented clearly in the notes. However, this should not delay management. The A-E approach can also form the structure for documenting your assessment.
Initial steps
Acute scenarios typically begin with a brief handover, including the patient’s name, age, background and the reason the review has been requested.
You may be asked to review a patient with opioid overdose due to agitation, bradypnoea and/or reduced level of consciousness.
Introduction
Introduce yourself to whoever has requested a review of the patient and listen carefully to their handover.
Interaction
Introduce yourself to the patient, including your name and role.
Ask how the patient is feeling, as this may provide useful information about their current condition.
If the patient is unconscious or unresponsive, and there are no signs of life, start the basic life support (BLS) algorithm as per resuscitation guidelines.
Preparation
Ensure the patient’s notes, observation chart, and prescription chart are easily accessible.
Ask for another clinical member of staff to assist you if possible.
Airway
Clinical assessment
Can the patient talk?
Yes: if the patient can talk, their airway is patent, and you can move on to the assessment of breathing.
No:
- Look for signs of airway compromise: angioedema, cyanosis, see-saw breathing, use of accessory muscles
- Listen for abnormal airway noises: stridor, snoring, gurgling
- Open the mouth and inspect: look for anything obstructing the airway, such as secretions or a foreign object
Interventions
Regardless of the underlying cause of airway obstruction, seek immediate expert support from an anaesthetist and the emergency medical team (often called the ‘crash team’). You can perform basic airway manoeuvres to help maintain the airway whilst awaiting senior input.
Head-tilt chin-lift manoeuvre
Open the patient’s airway using a head-tilt chin-lift manoeuvre:
- Place one hand on the patient’s forehead and the other under the chin
- Tilt the forehead back whilst lifting the chin forwards to extend the neck
- Inspect the airway for obvious obstruction. If an obstruction is visible within the airway, use a finger sweep or suction to try and remove it. Be careful not to push it further into the airway.
Jaw thrust
If the patient is suspected of having suffered significant trauma with potential spinal involvement, perform a jaw-thrust rather than a head-tilt chin-lift manoeuvre:
- Identify the angle of the mandible
- Place two fingers under the angle of the mandible (on both sides) and anchor your thumbs on the patient’s cheeks
- Lift the mandible forwards
Other interventions
Airway adjuncts are helpful and, in some cases, essential to maintain a patient’s airway. They should be used in conjunction with the manoeuvres mentioned above.
An oropharyngeal airway is a curved plastic tube with a flange on one end that sits between the tongue and hard palate to relieve soft palate obstruction. It should only be inserted in unconscious patients as it may induce gagging and aspiration in semi-conscious patients.
A nasopharyngeal airway is a soft plastic tube with a bevel at one end and a flange at the other. NPAs are typically better tolerated in partly or fully conscious patients than oropharyngeal airways.
Re-assessment
Make sure to re-assess the patient after any intervention.
Breathing
Clinical assessment
Observations
Review the patient’s respiratory rate:
- A normal respiratory rate is between 12-20 breaths per minute
- Bradypnoea is a common clinical feature of an opioid overdose
Review the patient’s oxygen saturation (SpO2):
- A normal SpO2 range is 94-98% in healthy individuals and 88-92% in patients with COPD at high risk of CO2 retention
- Hypoxaemia may occur in opioid overdose due to respiratory depression
See our guide to performing observations/vital signs for more details.
Inspection
Inspect the patient from the end of the bed:
- Cyanosis: bluish discolouration of the skin due to poor circulation or inadequate oxygenation
Auscultation
Auscultate the chest to screen for evidence of other respiratory pathology (e.g. coarse crackles may be present if the patient has developed aspiration pneumonia).
Investigations and procedures
Arterial blood gas
Take an ABG if indicated (e.g. low SpO2) to quantify the degree of hypoxia.
Patients may develop type 2 respiratory failure (i.e. low PaO2 and raised CO2) following an opioid overdose due to respiratory depression.
Chest X-ray
A chest X-ray may be indicated if abnormalities are noted on auscultation (e.g. reduced air entry, coarse crackles) to screen for evidence of aspiration pneumonia. A chest X-ray should not delay the emergency management of opioid overdose.
See our CXR interpretation guide for more details.
Interventions
Ventilation
Respiratory depression is common in opioid overdose, which can lead to critical hypoxia. If breathing is inadequate (<10 breaths per minute), support breathing with bag-valve-mask ventilation and call for senior clinical support.
Oxygen
Administer oxygen to all critically unwell patients during your initial assessment. This typically involves using a non-rebreathe mask with an oxygen flow rate of 15L. You can then trial titrating oxygen levels downwards after your initial assessment.
Naloxone
Naloxone is used to treat opioid-induced respiratory depression by blocking the effect of opioids.
The initial dose is 400 micrograms IV. If there is no response, two subsequent doses of 800 micrograms can be given at 1-minute intervals. Naloxone can also be administered via the subcutaneous or intramuscular route. However, the intravenous route has the quickest onset of action.
Naloxone has a short half-life, and some patients may require a naloxone infusion after a discussion with a senior clinician.
Naloxone rapidly reverses the effects of opioids, and as a result, it can precipitate symptoms of opioid withdrawal, including pain, confusion and agitation. Consider involving the drug and alcohol team to discuss appropriate opioid replacement therapy to treat symptoms of withdrawal.
Re-assessment
Make sure to re-assess the patient after any intervention.
Circulation
Clinical assessment
Blood pressure
Hypotension is also a common clinical feature of opioid overdose.
Capillary refill time
Capillary refill time may be prolonged in the context of opioid overdose.
Investigations and procedures
Intravenous cannulation
Insert at least one wide-bore intravenous cannula (14G or 16G) and take blood tests as discussed below.
See our intravenous cannulation guide for more details.
Blood tests
Request a full blood count (FBC), urea & electrolytes (U&E) and liver function tests (LFTs) for all acutely unwell patients. In the context of an opioid overdose, also request:
- CRP: to screen for evidence of infection
- Lactate: to screen for evidence of reduced end-organ perfusion
- Coagulation studies: to screen for coagulopathy
- Toxicology screen (including paracetamol levels): to screen for other drugs which may have been taken as part of a mixed overdose
Interventions
Fluid resuscitation
Hypovolaemic patients require fluid resuscitation:
- Administer a 500ml bolus Hartmann’s solution or 0.9% sodium chloride (warmed if available) over less than 15 mins.
- Administer 250ml boluses in patients at increased risk of fluid overload (e.g. heart failure).
After each fluid bolus, reassess for clinical evidence of fluid overload (e.g. auscultation of the lungs, assessment of JVP).
Repeat administration of fluid boluses up to four times (e.g. 2000ml or 1000ml in patients at increased risk of fluid overload), reassessing the patient each time.
Seek senior input if the patient has a negative response (e.g. increased chest crackles) or isn’t responding adequately to repeated boluses (i.e. persistent hypotension).
See our fluid prescribing guide for more details on resuscitation fluids.
Re-assessment
Make sure to re-assess the patient after any intervention.
Disability
Clinical assessment
Consciousness
Reduced consciousness is a common feature of opioid overdose.
Assess the patient’s level of consciousness using the ACVPU scale:
- Alert: the patient is fully alert
- Confusion: the patient has new onset confusion or worse confusion than usual
- Verbal: the patient makes some kind of response when you talk to them (e.g. words, grunt)
- Pain: the patient responds to a painful stimulus (e.g. supraorbital pressure)
- Unresponsive: the patient does not show evidence of any eye, voice or motor responses to pain
If a more detailed assessment of the patient’s level of consciousness is required, use the Glasgow Coma Scale (GCS).
Pupils
Assess the patient’s pupils:
- Inspect the size and symmetry of the patient’s pupils: pin-point pupils are associated with opioid overdose
- Assess direct and consensual pupillary responses: pupillary reflexes may be reduced
Drug chart review
Review the patient’s drug chart for medications which may cause neurological abnormalities (e.g. opioids, sedatives, anxiolytics).
Investigations
Blood glucose and ketones
Measure the patient’s capillary blood glucose level to screen for other causes of a reduced level of consciousness (e.g. hypoglycaemia or hyperglycaemia).
A blood glucose level may already be available from earlier investigations (e.g. ABG, venepuncture).
The normal reference range for fasting plasma glucose is 4.0 – 5.8 mmol/l.
Hypoglycaemia is defined as a plasma glucose of less than 3.0 mmol/l. In hospitalised patients, a blood glucose ≤4.0 mmol/L should be treated if the patient is symptomatic.
If the blood glucose is elevated, check ketone levels which, if also elevated, may suggest a diagnosis of diabetic ketoacidosis (DKA).
See our blood glucose measurement, hypoglycaemia and diabetic ketoacidosis guides for more details.
Imaging
Request a CT head if intracranial pathology is suspected after discussion with a senior clinician.
See our guide on interpreting a CT head for more details.
Interventions
Maintain the airway
Alert a senior clinician immediately if you have concerns about a patient’s consciousness level.
A GCS of 8 or below, or a P or U on the ACVPU scale, warrants urgent expert help from an anaesthetist. In the meantime, you should re-assess and maintain the patient’s airway, as explained in the airway section of this guide.
Correct hypoglycaemia
Hypoglycaemia should always be considered in patients presenting with a reduced level of consciousness, regardless of whether they have diabetes. The management of hypoglycaemia involves the administration of glucose (e.g. oral or intravenous).
See our hypoglycaemia guide for more details.
Re-assessment
Make sure to re-assess the patient after any intervention.
Exposure
Exposing the patient during your assessment may be necessary. Remember to prioritise patient dignity and the conservation of body heat.
Clinical assessment
Inspection
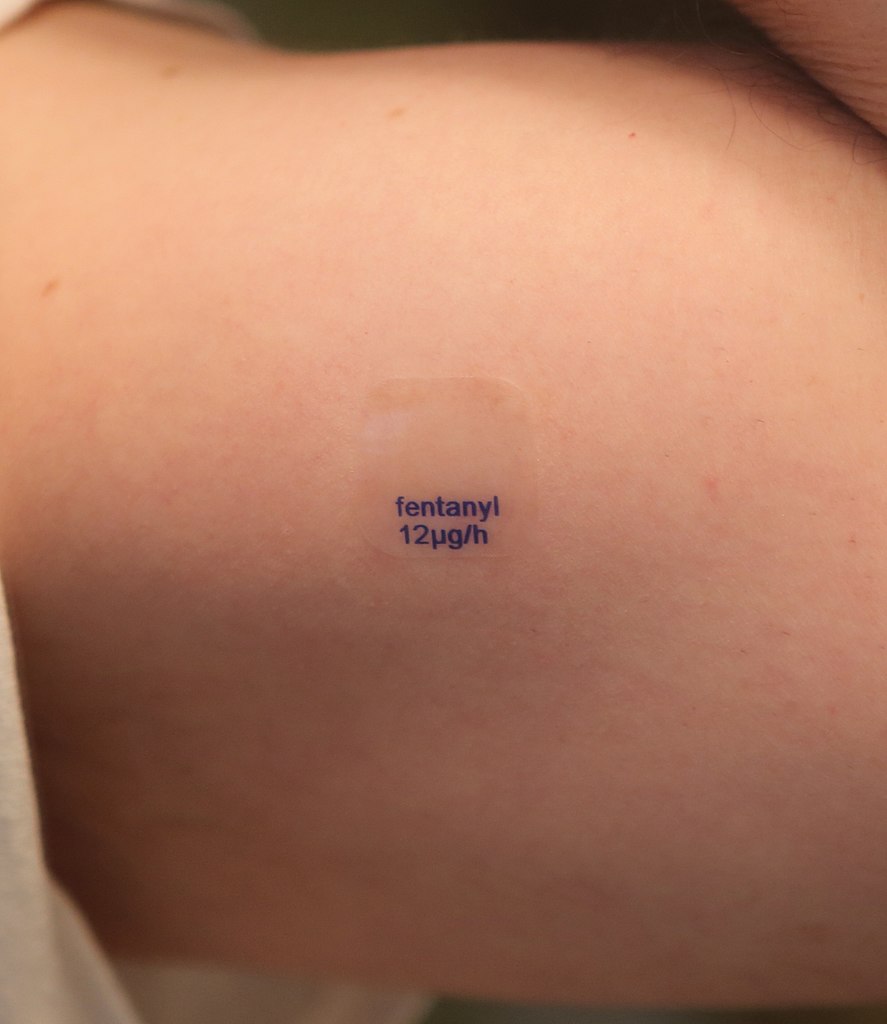
Inspect the patient’s skin for evidence of medication patches (Figure 1), injection sites, injuries or infection (e.g. erythema).
Review the output of the patient’s catheter and any surgical drains.
Temperature
Measure the patient’s temperature:
- If fever is present, consider co-existing infection (e.g. infective endocarditis is more common in intravenous drug users)
Interventions
Remove medication patches
Remove any opioid-containing medication patches (Figure 1).
Re-assessment
Make sure to re-assess the patient after any intervention.
Re-assessment and escalation
Re-assess the patient using the ABCDE approach to identify any changes in their clinical condition and assess the effectiveness of your previous interventions.
Any clinical deterioration should be recognised quickly and acted upon immediately.
Seek senior help if the patient shows no signs of improvement or if you have any concerns.
Escalation
Patients unresponsive to naloxone will require senior medical input to consider a naloxone infusion. Haemodynamically unstable patients will require urgent critical care input.
Use an effective SBAR handover to communicate the key information to other medical staff.
Next steps
Take a history
Revisit history taking to explore relevant medical history. If the patient is confused, you might be able to get a collateral history from staff or family members as appropriate.
See our history taking guides for more details.
Review medical records
Review the patient’s notes, charts and recent investigation results.
Review the patient’s current medications and check any regular medications are prescribed appropriately.
Document
Clearly document your ABCDE assessment, including history, examination, observations, investigations, interventions, and the patient’s response.
See our documentation guides for more details.
Discuss
Discuss the patient’s clinical condition with a senior clinician using an SBAR handover.
Questions which may need to be considered include:
- Are any further assessments or interventions required?
- Does the patient need a referral to HDU/ICU?
- Does the patient need reviewing by a specialist?
- Should any changes be made to the current management of their underlying condition(s)?
The next team of clinicians on shift should be informed of any acutely unwell patient.
References
- Patient.co.uk. Opiate poisoning. Available from: [LINK].
- British National Formulary. Naloxone. Available from: [LINK].
- British National Formulary. Poisoning, emergency treatment. Available from: [LINK]
Image references
- Figure 1. DanielTahar. A generic fentanyl transdermal patch, with a release rate of 12mcg per hour, applied to the skin (cropped). License: [CC BY-SA]