- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Introduction
Blood is a critical body fluid that circulates through the vascular system.
It is responsible for transporting oxygen and nutrients to tissues, bringing waste products to the liver, contributing to body temperature regulation, and acting as both a reservoir and mode of transport for immune cells. Blood can also form clots, stopping excessive blood loss in times of injury.1,2
The average human adult has more than five litres of blood, and it makes up 7-8% of body weight.1,3
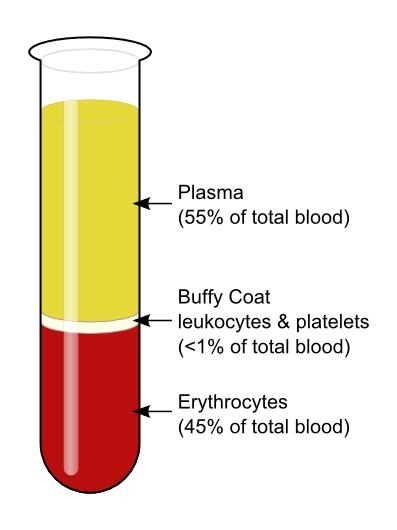
Blood has four main components: red blood cells, white blood cells, plasma, and platelets.
Red blood cells
Red blood cells, or erythrocytes, are biconcave-shaped cells that makeup 40-45% of blood by volume.1
They contain haemoglobin, a metalloprotein with haem groups which can bind to oxygen for transport.
Erythrocytes are 6µm in size, allowing them to travel through small capillaries to deliver oxygen to tissues. They have no nucleus, mitochondria, or other organelles. Instead, they use their volume to pack in hundreds of millions of haem molecules.4
Erythrocytes do not contain DNA and cannot synthesise RNA. Their lifespan is limited due to their restricted repair capabilities. Erythrocytes have a lifespan of approximately 120 days, after which ageing cells are targeted for phagocytosis by macrophages of the reticuloendothelial system.1,4
Blood typing categorises individuals into blood groups based on the presence or absence of antigens on the surface of their erythrocytes. For more information, see the Geeky Medics guide to the ABO and Rh blood group systems.
White blood cells
White blood cells, or leukocytes, are immune cells found in the blood. Using cell lineage, leukocytes can be classified as myeloid or lymphoid cells. Myeloid cells include neutrophils, monocytes, eosinophils, mast cells, and basophils. Lymphoid cells, or lymphocytes, include T cells, B cells, and natural killer (NK) cells.
Neutrophils are the most numerous of the leukocytes. They have a multilobed nucleus and are key in the acute phase of infections, particularly bacterial infections. They can function as phagocytes at sites of inflammation.
Lymphocytes are the most common agranular leukocyte. B cells produce circulating antibodies, T cells go on to become cytotoxic, helper or suppressor cell-mediated immune cells, and NK cells eradicate virus-infected cells.
Monocytes are a diverse group of myeloid cells. They can migrate to tissues, where they can differentiate into macrophages and phagocytose potential pathogens. There are specialised names for macrophages groups found in certain tissues, such as Kupffer cells of the liver, or microglia of the central nervous system.
Eosinophils are granular leukocytes that act as mediators of allergic responses, and participate in immune responses, particularly against parasitic infections.
Basophils are the least common type of granulocyte and are responsible for inflammatory reactions during immune responses. They also function in allergic reactions.2
For a comprehensive breakdown of leukocytes, see the Geeky Medics article on the immune response.
Clinical relevance: hyperviscosity syndrome
Hyperviscosity syndrome is a triad of symptoms caused by an increase in the viscosity of the blood. This can be caused by diseases that change the fractions of blood components, such as increased erythrocytes in polycythaemias, increased leukocytes in leukaemia, or increased proteins in monoclonal gammopathies. Sickle cell disease can also contribute, as deformed erythrocytes hinder their ability to traverse through the vasculature.
Increased blood viscosity translates to decreased blood flow, which can cause decreased microvascular circulation and tissue hypoperfusion. Patients with hyperviscosity syndrome can present with the triad of visual changes (due to retinopathy), mucosal bleeding, and neurological symptoms ranging from headache to seizures and coma.
Short-term treatment can include supportive therapy with fluids, elective phlebotomy, and plasma exchange or plasmapheresis. The definitive treatment involves treating the underlying cause of the hyperviscosity.5
Plasma
Plasma is the liquid portion of blood, making up approximately 55-60% of blood by volume. It tends to be clear to straw yellow in colour.
Plasma is mostly water, but also contains:6
- Amino acids
- Electrolytes
- Gases
- Nitrogenous waste
- Nutrients: including glucose and fat particles
- Proteins: including albumin, globulins, enzymes, clotting factors like fibrinogen, and hormones
Platelets
Platelets, or thrombocytes, are cell fragments that circulate until removed by the spleen, or are recruited to a site of injury and activated to participate in the clotting process.
Platelets also play a role in immunity, directly interacting with antibodies as well as secreting proinflammatory and procoagulant mediators to connect the adaptive and innate immune responses.7
Key points
- Blood has four main components: red blood cells, white blood cells, plasma, and platelets.
- Changes to the normal ratio of blood components can signal a pathological process.
Editor
Dr Chris Jefferies
References
- American Society of Hematology. Blood basics. Published in 2021. Available from: [LINK].
- JT Hansen. Netter’s clinical anatomy. Published in 2021. ISBN: 9780323826624
- L Dean. Blood groups and red cell antigens. Published in 2005. Available from: [LINK].
- L Barbalato, LS Pillarisetty. Histology, red blood cell. Published in 2021. Available from: [LINK].
- AP Rogers, M Estes. Hyperviscosity syndrome. Published in 2021. Available from: [LINK].
- J Mathew, P Sankar, M Varacallo. Physiology, blood plasma. Published in 2021. Available from: [LINK].
- RA Ali, LM Wuescher, RG Worth. Platelets: essential components of the immune system. Published in 2016. Available from: [LINK].
Image references
- KnuteKnudsen at English Wikipedia. Blood centrifugation scheme. Licence: [CC BY 3.0].




