- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Introduction
A caesarean section is the delivery of a baby through a surgical incision in the abdominal and uterine wall(s).
Over the past couple of decades, the rates of caesarean sections have increased significantly in western countries. In the United Kingdom, 25-30% of births were delivered by caesarean section in 2015. In women who have had at least one previous caesarean section, the rate of deliveries by this method increases to 67%.1
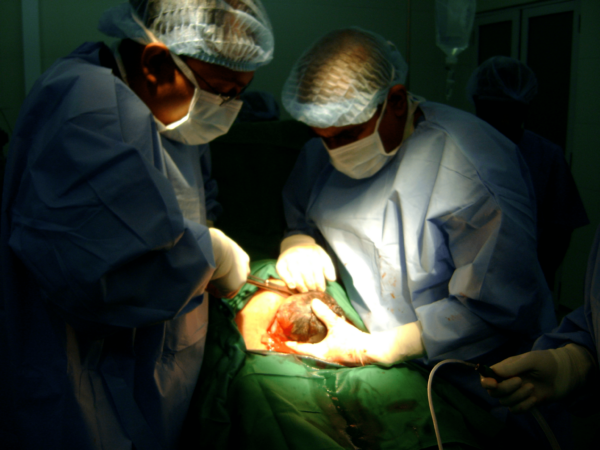
In this article, we will discuss the classification and indications for caesarean sections, plus provide an overview of the procedure and associated complications.
Classification
Caesarean sections can be classified into elective or emergency:1
- Category 1 – immediate (“crash”): these are performed when there is an immediate threat to the life of the woman or fetus. Delivery should take place as soon as possible. The Royal College of Obstetricians and Gynaecologists recommends that a category 1 section should be performed within 30 minutes of making the decision for caesarean delivery.
- Category 2 – urgent: these are indicated when there is maternal or fetal compromise, which is not immediately life-threatening. To be performed as soon as possible, and within 75 minutes of decision for delivery.
- Category 3 – scheduled: this category of C-section is indicated where there is no maternal or fetal compromise, but early delivery is required.
- Category 4 – elective: the timing of this delivery is planned to suit the woman and staff.
Indications
Indications for a category 1 (crash) caesarean section include:
- Cord prolapse
- Sustained fetal bradycardia
- Fetal hypoxia (scalp pH < 7.20)
- Placental abruption
- Uterine rupture
Indications for a category 2 (urgent) caesarean section include:
- Failure to progress in labour with pathological CTG
Indications for a category 3 (scheduled) caesarean section include:
- Intrauterine growth restriction with poor fetal function tests
- Failed induction of labour
- Breech in labour
Indications for a category 4 (elective) caesarean section include:
- Previous caesarean section
- Breech presentation
- Other malpresentations
- Twin pregnancy where the first twin is not a cephalic presentation
- Placenta praevia
- Maternal HIV
- Primary genital herpes in the third trimester
- Previous hysterotomy or “classical” caesarean section
- Maternal diabetes with an estimated fetal weight >4.5kg in cases where vaginal delivery is unlikely to be successful
- Maternal request
Elective caesarean sections are normally planned around 39 weeks gestation. This is to reduce the risk of the neonate developing respiratory distress in neonates born at earlier gestations, known as transient tachypnoea of the newborn.
Procedure
Peri-operative and anaesthetic concerns
Before a caesarean section, there are several steps and investigations that should be performed to reduce morbidity associated with the procedure:
- Pre-operative haemoglobin check and correction of anaemia. A group & save should also be taken.
- H2-receptor antagonists or proton pump inhibitors (currently off license) +/- anti-emetics like metoclopramide. Metoclopramide is a prokinetic anti-emetic agent, and this can help reduce the risk of aspiration of gastric contents.
- Women should be risk-assessed and appropriate thrombo-prophylaxis should be prescribed. This includes compression stockings, hydration, early mobilisation and low-molecular-weight heparin as appropriate.
- Prophylactic antibiotics should be given immediately prior to the skin incision.
- In cases of ruptured membranes, an iodine-based vaginal wash is recommended pre-operatively to reduce the risk of endometritis.
An indwelling urinary catheter should be inserted for the duration of the procedure to prevent over-distension. This reduces the risk of damage to the bladder during the surgery. The catheter can be removed once the woman is mobile after regional anaesthesia, but no sooner than 12 hours after the last “top-up” dose of anaesthetic.
Regional anaesthesia is preferred to general anaesthesia. Most caesarean sections are performed under a spinal or “topped-up” epidural anaesthesia.
Caesarean section under general anaesthesia is reserved for cases where there is a maternal contraindication for regional anaesthesia, where spinal or epidural anaesthesia fails to achieve an adequate block or more commonly for category 1 sections where there is an immediate concern for fetal wellbeing.
General anaesthesia for an emergency caesarean section should include pre-oxygenation, cricoid pressure and rapid sequence induction to reduce the risk of aspiration of gastric contents.
All types of anaesthetic require a left lateral tilt of up to 15 degrees for uterine displacement to prevent maternal hypotension (e.g. via insertion of a wedge cushion).
Types of caesarean section
Lower uterine segment incision
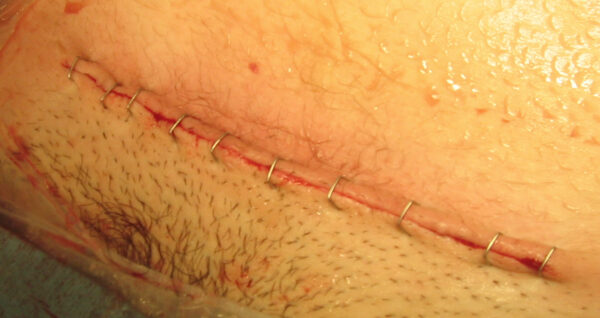
There are two types of skin incisions for this type of caesarean section: the Pfannenstiel incision (Figure 2) and a Joel-Cohen incision.
NICE recommends a Joel-Cohen incision, defined as a straight horizontal incision above the symphysis pubis. Subsequent layers are opened bluntly. This allows for a shorter operating time and reduces the incidence of postoperative febrile illness.
Abdominal wall layers
The layers of the abdominal cavity opened and closed during a caesarean section include:
- Skin
- Subcutaneous tissue (including Scarpa’s fascia)
- Rectus sheath
- Rectus muscle
- Parietal peritoneum
- Uterus including visceral peritoneum
Classical caesarean section
This procedure is rarely performed as it involves a vertical incision into the upper uterine segment.
A classical caesarean section may be indicated in the following cases:
- Structural abnormality of the uterus
- Difficult access to the lower uterine segment due to adhesions or fibroids
- Where hysterectomy will follow caesarean delivery (e.g. in cases of morbidly adherent placenta)
- Post-mortem caesarean section where the fetus is viable
- Cervical cancer
- Anterior placenta previa with abnormally vascular lower uterine segment
- Transverse lie with ruptured membranes
- Very preterm fetus where the lower uterine segment is poorly formed
Classical caesarean sections are associated with greater rates of adhesions and infections compared to lower uterine segment incisions.
The closure of a classical caesarean section is more complicated and takes longer to complete. Following dissection of the abdominal and uterine walls, and delivery of the fetus, five units of oxytocin are given to the woman to aid the delivery of the placenta by controlled cord traction. Once the uterine cavity has been emptied, the uterus is closed with two layers. The rectus sheath and skin are closed either with continuous or interrupted sutures or staples.
Complications
When compared to vaginal delivery, caesarean section has lower rates of perineal trauma and pain. However, primary caesarean section has a higher incidence of abdominal pain, venous thromboembolism, bladder or ureteric injury and hysterectomy.
Complications of caesarean section can further be divided into intraoperative and postoperative complications.
Intraoperative complications
Intraoperative complications occur in 12-15% of caesarean sections and are more common in women undergoing an emergency caesarean section. These may include:4
- Anaesthetic side effects (e.g. hypotension, nausea)
- Haemorrhage sometimes requiring blood transfusion and, rarely, hysterectomy (7-8/1000)
- Uterine or uterocervical lacerations
- Bladder or bowel lacerations +/- repair
- Ureteral injury
The risk of haemorrhage is increased in women with a high BMI, placenta praevia or placental abruption or in cases of very high or low birthweight.
Postoperative complications
Postoperative complications can occur in up to one-third of women. These include:
- Pain: opioid analgesia is used first-line +/- laxatives. This is stepped down to paracetamol and non-steroidal anti-inflammatory drugs (NSAID) use once pain is adequately controlled.
- Infection: endometritis, wound infection and urinary tract infections. Occurs in approximately 8% of women undergoing caesarean section. Where the woman’s body mass index is greater than 35, negative pressure dressings may be considered to decrease the risk of wound infection.
- Venous thromboembolism
- Pulmonary atelectasis
- Return to theatre for another procedure
- Longer hospital stay compared to vaginal delivery
Complications affecting future pregnancies may include:
- Abnormal placentation (e.g. accreta spectrum/praevia)
- Uterine rupture
- Repeat caesarean section
For women who have had a previous caesarean section, the risk of placenta praevia and placenta accreta increases in subsequent pregnancies. There is also a higher risk of antepartum stillbirth in subsequent pregnancies and this risk increases with each successive caesarean section performed.5
Fetal/neonatal complications may include:
- Fetal laceration risk of 2%
- Transient tachypnoea of the newborn
- Admission to a neonatal unit
Vaginal birth after caesarean section (VBAC)
Vaginal birth after caesarean section is an appropriate option and may be offered to women who have a singleton pregnancy with a cephalic presentation at 37 weeks who had a single lower uterine segment caesarean section in the past, with or without previous vaginal deliveries.6
VBAC is contraindicated in women who have had a previous uterine rupture or classical caesarean section, or for women where vaginal delivery is contraindicated irrespective of the presence of a scar (e.g. in major placenta praevia).
A planned VBAC is associated with a 0.05% risk of uterine rupture.
The success rate of planned VBAC is 72-75%, however, may be as high as 90% in women who have had a previous successful vaginal delivery, which is the greatest predictor of a successful VBAC.
Continuous fetal monitoring should be utilised during the delivery as a change in fetal heart rate can be an early sign of impending uterine scar rupture.
Women should be counselled that the risk of uterine rupture increases two to three-fold with the use of uterotonic agents or prostaglandins in induced or augmented labour.
Key points
- A caesarean section is the delivery of a baby through a surgical incision in the abdominal wall and the uterine wall and accounts for 25-30% of births in the United Kingdom.
- The main indications are a previous C-section, fetal compromise, failure to progress in labour and breech presentation.
- Caesarean sections are commonly performed through a Pfannenstiel incision with access to the uterine cavity through a transverse lower uterine incision.
- Caesarean sections are associated with a reduced risk of perineal pain and trauma.
- Caesarean sections are associated with an increased risk of abdominal pain, venous thromboembolism, and bladder or ureteric injury. There is an increased risk associated with stillbirth and placental insertion disorders in subsequent pregnancies.
- VBAC is an option for women in future pregnancies but should be performed after careful consideration due to the risk associated with uterine rupture.
Reviewer
Dr Barbara Burke
Registrar in Obstetrics and Gynaecology
Cork University Maternity Hospital
Editor
Dr Chris Jefferies
References
- National Institute for Health and Care Excellence. Caesarean birth. March 2021. Available from: [LINK]
- Mediajet. Caesarean section. License: [CC BY-SA]
- DRosenbach. Pfannensteil incision. License: [CC BY-SA]
- Shellhaas, Cynthia S et al. “The frequency and complication rates of hysterectomy accompanying cesarean delivery.” Obstetrics and gynecology 114,2 Pt 1 (2009): 224-229.
- Keag, Oonagh E et al. Long-term risks and benefits associated with cesarean delivery for mother, baby, and subsequent pregnancies: Systematic review and meta-analysis. 2018. Available from: [LINK]
- Royal College of Obstetricians and Gynaecologists, Birth after caesarean section: Green top guideline no.45. 2015 Available from: [LINK]
- Collins S, Arulkumaram S et al, Oxford Handbook of Obstetrics and Gynaecology 3rd Edition, Oxford University Press, 2013




