- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
This article provides a brief overview of signs that may be found on the hands during clinical examination.
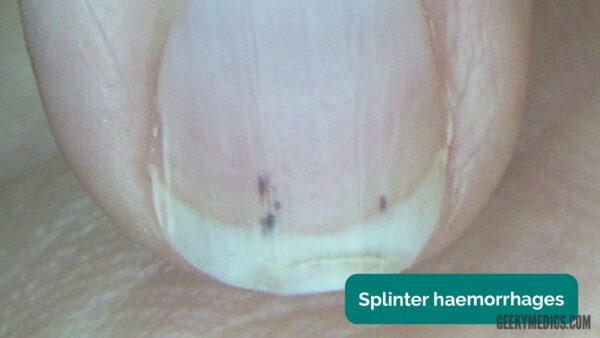
Splinter haemorrhages
Splinter haemorrhages are caused by small emboli becoming lodged in nailbed capillaries causing secondary haemorrhage.
Causes include:
- Local trauma
- Infective endocarditis
- Sepsis
- Vasculitis
- Psoriatic nail disease
Osler’s nodes
Osler’s nodes are red-purple, slightly raised, tender lumps that often have a pale centre. These lesions are typically found on the fingers or toes and are associated with infective endocarditis.

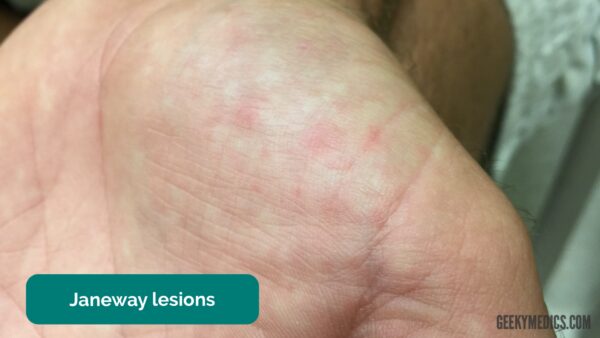
Janeway lesions
Janeway lesions are non-tender, haemorrhagic lesions that occur on the thenar and hypothenar eminences of the palms and soles. Janeway lesions are typically associated with infective endocarditis.
Fingertip pallor
Fingertip pallor refers to a white and waxy appearance that occurs as a result of vasoconstriction or vascular obstruction.
Conditions associated with this sign include:
- Peripheral vascular disease
- Raynaud’s phenomenon
- Buerger’s disease
- CREST syndrome

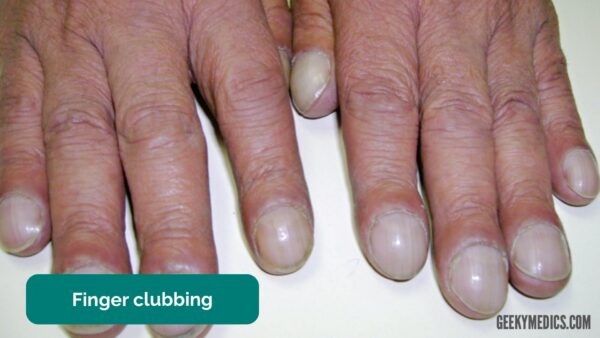
Causes of finger clubbing
Finger clubbing involves uniform soft tissue swelling of the terminal phalanx of a digit with subsequent loss of the normal angle between the nail and the nail bed.
Finger clubbing is associated with several underlying disease processes including:
- Congenital cyanotic heart disease
- Infective endocarditis
- Atrial myxoma
- Bronchiectasis
- Lung cancer
- Cystic fibrosis
- Inflammatory bowel disease
Asterixis
Asterixis (also known as ‘flapping tremor’) is a type of negative myoclonus characterised by irregular lapses of posture causing a flapping motion of the hands.
Causes of asterixis include:
- CO2 retention (e.g. COPD)
- Uraemia
- Hepatic encephalopathy

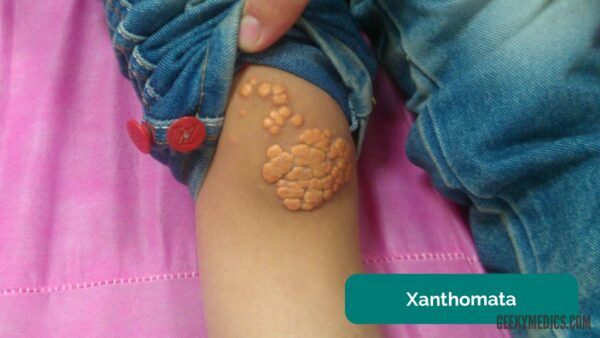
Xanthomata
Xanthomata are raised yellow cholesterol-rich deposits that are often noted on the palm, tendons of the wrist and elbow.
Xanthomata are associated with hyperlipidaemia (typically familial hypercholesterolaemia), an important risk factor for cardiovascular disease.
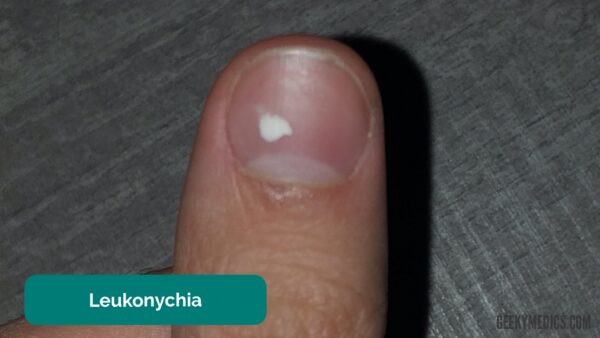
Leukonychia
Leukonychia involves whitening of the nail bed.
Causes include:
- Nailbed trauma
- Hypoalbuminaemia (e.g. end-stage liver disease, protein-losing enteropathy)
- Chemotherapy
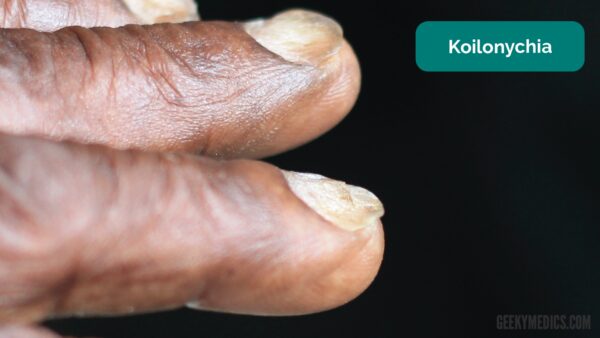
Koilonychia
Koilonychia refers to spoon-shaped nails.
Causes include:
- Iron deficiency anaemia (e.g. Crohn’s disease)
- Lichen planus
- Rheumatic fever
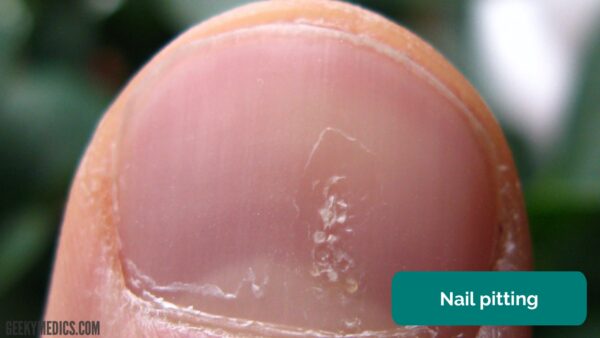
Nail pitting
Nail pitting involves punctate depressions of the nail plate.
It is most commonly associated with psoriasis.
Dupuytren’s contracture
Dupuytren’s contracture is a benign and progressive disorder of the hand. It involves the development of cords within the palmar fascia leading to contracture and flexion deformity, often localised to the ring finger.
Although a specific cause has not been established, a number of risk factors have been identified:
- Excessive alcohol intake
- Manual work: especially involving vibrational machinery
- Smoking: smokers are 3 times more likely to develop the condition
- Diabetes mellitus: 1 in 5 diabetic patients develop the condition
- 70% of patients have a hereditary component

Palmar erythema
Palmar erythema refers to redness involving the heel of the palm.
Causes include:
- Chronic liver disease
- Pregnancy
- Hyperthyroidism
References
- Adapted by Geeky Medics. Roberto J. Galindo. Osler’s nodes. Licence CC BY-SA.
- Adapted by Geeky Medics. Warfieldian. Janeway lesions. Licence: CC BY-SA.
- Intermedichbo [CC BY-SA 3.0] via Wikimedia Commons
- Adapted by Geeky Medics. Desherinka. Finger clubbing. Licence: CC BY-SA.
- Adapted by Geeky Medics. Min.neel. Xanthoma in a child. Licence: CC BY-SA.
- Adapted by Geeky Medics. BrotherLongLegs. Leukonychia. Licence: CC BY-SA.
- Adapted by Geeky Medics. CHeitz. Koilonychia. Licence: CC BY 2.0.
- Seenms. Adapted by Geeky Medics. Nail pitting. Licence: CC BY-SA.
- Adapted by Geeky Medics. Frank C. Müller. Dupuytren’s. Licence: CC BY-SA.




