- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Introduction
Tooth extraction is a common procedure. It involves removal of the tooth, or root, from its socket in the alveolar bone by widening the space between the tooth and alveolar bone and severing the periodontal ligament. Complications can occur for various medical, anatomical, and iatrogenic reasons. This article aims to provide an overview of common complications of extractions and their management.
Dry socket (alveolar osteitis)
Dry socket is a painful condition that occurs after tooth extraction due to loss of the initial blood clot or healing epithelium from the extraction socket, leading to exposure of the alveolar bone. It occurs in approximately 3% of all extractions, and around 30% of all impacted mandibular third molar extractions. 1
Risk factors
Risk factors for dry socket include:
- Smoking
- Oral contraceptives
- Female gender
- Traumatic extraction
- Bacterial involvement
- Bone/root fragments2
Clinical presentation
History
Typical findings in the history of a patient with dry socket include:
- Recent extraction in the past 1-3 days with increasingly severe pain over this period
- Pain may radiate around the affected side of the face
Examination
Typical findings on examination include:
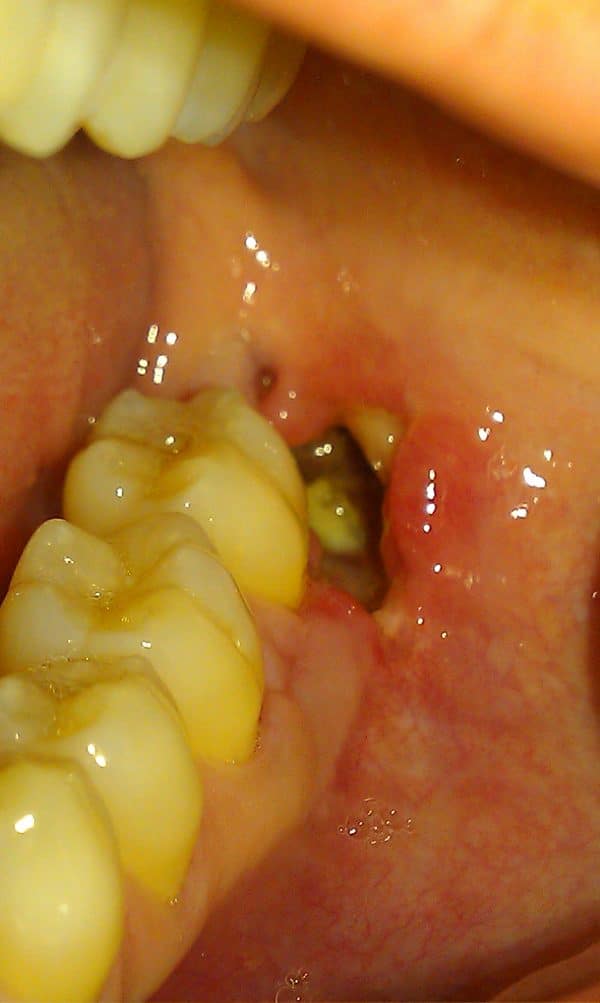
- At the extraction site, there will be an empty socket with bare bone and no visible blood clot
- There may be food packing into the socket which helps cause distinct halitosis
- The gingival margin may also be inflamed
Investigations
Clinical examination of the socket is usually diagnostic without the requirement for radiographs or other imaging.
Management
Management can be performed with or without local anaesthetic. Any bony fragments should be removed and copious irrigation of the socket with saline or chlorhexidine is required to remove food debris and bacteria. Once clean, a suitable dry socket medication should be placed into the socket (e.g. Alvogyl/Septodont)4 to help soothe and protect the socket, prevent further food packing/bacterial infiltration and encourage epithelial healing. A suture may also be placed to aid retention of the dressing. These patients often require frequent review to replace the dressing and review healing.5
Bleeding complications
Bleeding after an extraction is normal within the first half-hour while waiting for the clot to form and blood-stained saliva can also be expected for up to 8 hours post-extraction. The onset of bleeding complications can vary from immediately post-extraction up to a week after the extraction.
Post-extraction bleeding is considered abnormal if:6
- it lasts longer than 12 hours after the extraction
- it causes the patient to seek help from their dentist or attend a hospital emergency department
- a large haematoma or ecchymosis forms within the oral soft tissues
- the patient requires a blood transfusion
Risk factors
Risk factors for post-extraction bleeding include:
- Mandibular extraction
- Traumatic extraction
- Bone bleeding
- Coagulation disorders
- Platelet problems
- Medication-related (e.g. anti-coagulant or anti-platelet drugs)6
Clinical presentation
History
The patient will have had a recent extraction, usually within the past 24 hours, and have a bleeding extraction socket.
Key details to gather when taking a history include:
- Time and date of extraction
- Duration of bleeding
- Volume of bleeding
- Relevant past medical history (e.g. bleeding disorders)
- Relevant medication history (e.g. antiplatelets, anticoagulants)
Examination
Good visualisation of the bleeding area is essential. Aspiration and good lighting are a necessity to directly visualise the site and magnification is also beneficial.
Key things to assess during examination include:
- Patency of the airway (i.e. ensure there is no compromise due to haematoma or active bleeding)
- Rate/volume of bleeding from the socket
- Clot formation
Investigations
Clinical examination is usually diagnostic. If the bleeding is heavy, blood tests (FBC, LFTs, coagulation screen, group and save) may be needed. If the airway is compromised an MRI may be required (once the airway is secured).
Management
The aim is to stop the bleeding and prevent any further blood loss. Firm pressure with damp gauze over the socket for 10 minutes will help blood clot formation. Packing the socket with Surgicel and suturing it in place is a common and effective local haemostatic measure. A tranexamic acid mouthwash can also be used. If the bleeding is more intense, local anaesthetic with a vasoconstrictor can be used as a temporary measure while more definitive treatment is carried out. This can involve bone wax over bleeding bone, and electro or chemical cautery.
A patient with a coagulation disorder may require systemic intervention and if the blood loss is severe a blood transfusion may be required. These patients should be urgently referred to a hospital emergency department.6,7
Root fracture
It is important to be able to identify when root fractures occur and how to manage them. Roots can also remain present in the mouth as retained roots. These may be visible or found incidentally on radiographs.
Risk factors
Risk factors for root fracture include:
- Thin roots
- Excess force during extraction/ lack of luxation
- Gross caries
- Dense bone
Clinical presentation
History
Often the operator will be aware of the fracture. A crack is frequently heard, as well as a sudden increase in movement of the coronal portion of the tooth.
Examination
When the mobile portion of the tooth is delivered the roots may not be present, or fragments may be missing. These fragments may be visible in the socket. Running a finger over the roots will allow you to feel for any sharp fractured edges. Aspiration and good lighting are necessary to aid visualisation of any fragments.
Investigations
A pre-op radiograph of the tooth being extracted should be available. This should give all the information regarding root morphology and any relevant nearby anatomy. If the fragment is not visible or palpable a new radiograph, ideally a periapical (PA) view should be taken to locate it.
Management
Root fracture can either be managed by removal of the fragment, or by leaving the fragment in situ and regularly reviewing.
Factors to consider in deciding if the root should be removed:
- Size of the fragment
- Why is the tooth being extracted? (e.g. large pathology, implants, orthodontics etc)
- Any nearby anatomy (e.g. maxillary sinus, inferior alveolar nerve)
- Patient factors (e.g. tolerance, pain)
- Operator factors (e.g. skill level, equipment available)8
Fragments can usually be removed with careful luxation and elevation using Couplands and Cryer’s elevators around the root. Root forceps can be used to deliver the root. If the root fragment is unable to be removed in this way a surgical approach involving raising a flap and bone removal can be used. This may require referral to a specialist oral surgery service.
There is the potential for the fragment to be left in place, however, the potential complications must first be discussed with the patient. The fragment and healing around the fragment must be reviewed if complications develop; if there are any signs of further pain, infection or failure to heal, the fragment will require removal.
Oro-antral communication and fistula
An oro-antral communication (OAC) is a pathological communication between the oral cavity and maxillary sinus. An OAC, if untreated for 48-72 hours, will progress into an epithelialised tract – an oro-antral fistula (OAF). An OAC should be managed efficiently to prevent OAF formation, sinus infection and potential osteomyelitis.9
Risk factors
Risk factors for the development of an OAC include:
- Extraction of pre-molars/molars with a close relationship to the maxillary sinus
- Pathological lesions (e.g. cyst, tumour)
- A failed sinus lift procedure
- Maxillary tuberosity fracture
- Trauma10
Clinical presentation
History
An OAC may be detected immediately after extraction. If not detected at the time of extraction the patient may present with regurgitation of liquid through the nose, or the inability to suck through straws. They may have unilateral nasal discharge, purulent discharge, and complain of a bad taste. An OAF will present at least 7 days after the extraction and will have a similar history to an OAC. Patients may also present with sinusitis.
Medical conditions such as diabetes, cardiovascular conditions and renal dysfunction can increase complications, such as delayed healing.
Examination
Good clinical examination is essential. Aspiration and lighting are needed to assess if the base of the socket can be seen. Do not probe into the socket.
Findings on examination in the context of an OAC may include:
- If an OAC has been created, you may see an extraction socket with a black hole at the base.
- There may be bubbling of blood around the socket entrance.
- If a mirror/cotton wisp is placed under the socket if may fog/move on exhalation and whistling may be heard on exhalation.10
Investigations
A good pre-op radiograph (PA or DPT) should be available and the relationship of the tooth roots to the maxillary sinus identified. If the roots have a close relationship with the sinus floor or are visibly in the sinus the patient is at high risk of developing an OAC. They should be warned of this during the consent process for the extraction.
A DPT can be taken to assess the size of the bony defect created.9
Management
The patient should be informed of the OAC creation and the treatment options available. Management can be conservative or surgical. The patient should be advised not to blow their nose for the next 2 weeks, and to sneeze with their mouth open to prevent a build-up of pressure. They should maintain good oral hygiene to help prevent infection. Decongestants (e.g. ephedrine) can be used to help improve sinus drainage and antibiotics may be required to prevent or help treat any sinusitis that develops.11
Conservative management
Defects less than 2mm can heal spontaneously following the formation of a blood clot. If the defect is larger, an impression can be taken of the upper arch to allow the creation of an immediate suck down splint that should be worn continuously for 7 days. Place damp gauze over the extraction site and OAC to prevent impression material entering the sinus.
Surgical management
A three-sided buccal advancement flap can be used with or without the buccal fat pad. This allows immediate closure of the OAC. Care should be taken to maintain the buccal sulcus depth in case of future prosthesis creation. A palatal flap can be used if needed.
If an OAF is present this will need a referral to a specialist oral or maxillofacial surgeon. Any epithelialised tract will require surgical removal and either a buccal advancement flap or finger flap will be required to help heal the defect. If the defect is repeatedly non-healing more extensive flaps are often required.9,10
Maxillary tuberosity fracture
The maxillary tuberosity is the weakest area of bone in the maxilla. The maxillary sinus most commonly extends back to the maxillary third molar region, weakening the tuberosity. If posterior molars are to be extracted, they should be planned carefully with all risks including tuberosity fracture explained to the patient if relevant. The pre-operative radiograph should be reviewed, and the size of the sinus noted. If the sinus has a close relationship with the roots of the lone molar to be extracted a cone beam CT scan should be requested and referral to a specialist oral surgeon considered. The incidence of tuberosity fractures is generally low; they occur in every 0.08% – 0.15% of simple extractions.12
Risk factors
Risk factors for maxillary tuberosity fracture include:
- Large maxillary sinus with extension into the maxillary tuberosity
- Lone standing maxillary molar
- Hypercementosis/ankylosis of molar to be extracted
- Chronic periapical infection
- Radicular cyst
- Wide divergent/curved roots
- Abnormal root number
- Iatrogenic – excessive force used12
Clinical presentation
History
Fracture of the tuberosity is most likely to occur during the extraction. The operator may feel a crack and a sudden increase in mobility of the tuberosity region.
Examination
There may be increased bleeding, and a palatal mucosal tear may be visible. There will be increased mobility of the tuberosity region.
Investigations
A PA should have been taken pre-extraction. If the patient is more at risk of tuberosity fracture a CBCT may be justified. If a fracture is suspected a CBCT scan may be needed to fully visualise the extent of the fracture.12
Management
If a tuberosity fracture is suspected the procedure must be stopped. There are multiple methods of management. Operator experience should be considered when selecting a management strategy and referral to a specialist oral surgeon should be seriously considered.
If a fracture is detected a rigid splint can be placed to stabilise the fracture. This should be left in place for 4-6 weeks to allow bony healing, then the tooth should be removed surgically.
The tooth should not be twisted or removed using forceps, as this can tear the mucous membrane, and potentially the greater palatine artery leading to the possible creation of an OAC and severe blood loss.13
Other complications
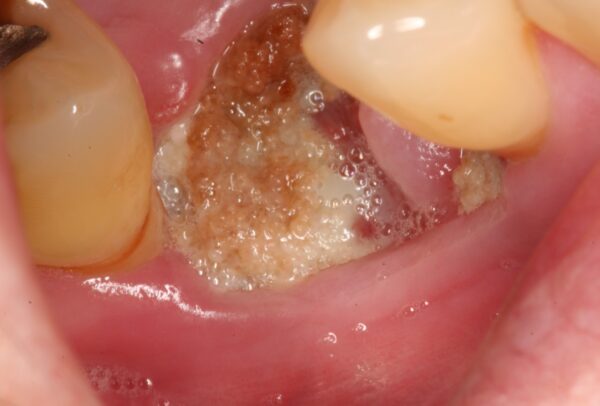
Medication-related osteonecrosis of the jaw (MRONJ) and osteoradionecrosis (ORN) are both serious complications of dental extractions that cause bone destruction and exposure in the maxillofacial region. Clinically they look similar with areas of exposed bone, however, they have different aetiologies.
Risk factors for MRONJ include:
- Treatment with anti-angiogenic (e.g. Sunitinib) and/or anti-resorptive drugs (e.g. bisphosphonates) in the management of cancer
- Use of anti-resorptive drugs and glucocorticoids concurrently
- Radiotherapy to the head and neck region14
If a patient is at risk of either MRONJ or ORN, alternatives to extraction should be seriously considered. If extraction is necessary, referral to a specialist oral surgeon/ oral and maxillofacial surgery department is advised.14
The SDCEP provide further guidance and explanation of MRONJ and ORN.15
References
- Bowe D, Rogers S, Stassen L. The management of dry socket/ alveolar osteitis. 2012. Available from: [LINK]
- Kolokythas A, Olech E, Miloro M. Alveolar osteitis: A comprehensive review of concepts and controversies. 2010. Available from: [LINK]
- Mel11691. Dry socket. Licence: CC Attribution-Share Alike 3.0 Unported. Available from: [LINK]
- Septodont. Alvogyl Patient information leaflet. 2006.
- Mamoun J. Dry Socket Etiology, Diagnosis, and Clinical Treatment Techniques. 2018. Available from: [LINK]
- Cochrane Database. Interventions for treating post-extraction bleeding. 2018. Available from: [LINK]
- Scottish Dental Clinical Effectiveness Programme. Management of dental patients taking anticoagulants or antiplatelet drugs. 2015. Available from: [LINK]
- Nayyar J, Clarke M, O’sullivan M, Stassen L. Fractured root tips during dental extractions and retained root fragments. A clinical dilemma? 2015. Available from: [LINK]
- Parvini P, Obreja K, Begic A, Scwarz F, Becker J, Sader R, Salti L. Decision making in closure of Oro-Antral communication and fistula. 2019. Available from: [LINK]
- Khandelwal P, Hajira N. Management of oro-antral communication and fistula: various surgical options. 2017. Available from: [LINK]
- British National Formulary. Oral bacterial infections. 2020. Available from: [LINK]
- Chrcanovic B, Freire-Maia B. Consideration of maxillary tuberosity fractures during extraction of upper molars: a literature review. 2011. Available from: [LINK]
- Thirumurugan K, Munzanoor R, Prasad G, Sankar K. Maxillary tuberosity fracture and subconjunctival haemorrhage following extraction of maxillary third molar. 2013. Available from: [LINK]
- Chronopoulos A, Zarra T, Ehrenfeld M, Otto S. Osteoradionecrosis of the jaws: definition, epidemiology, staging an clinical and radiological findings. A concise review. 2017. Available from: [LINK]
- Scottish Dental Clinical Effectiveness Programme. Oral health management of patients at risk of medication related osteonecrosis of the jaw. 2017. Available from: [LINK]
- Coronation Dental Speciality Group. MRONJ in the maxilla. Licence: CC Attribution-Share Alike 4.0 international. Available from: [LINK]
Editor
Louise Griffith
General Dental Practitioner and Clinical Research Dentist




