- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
The coronary arteries provide oxygenated blood to the heart. This article describes the typical course, pattern and distribution of the coronary arteries and some of their respective named branches. Common variations, arterial dominance and coronary artery disease are also discussed.
Right Coronary Artery
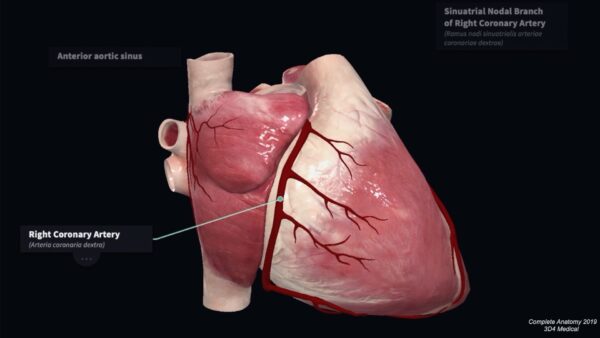
The right coronary artery arises from the anterior aortic sinus at the beginning of the ascending aorta. It passes between the right auricle and the pulmonary trunk in the atrioventricular groove. It gives rise to a number of atrial and ventricular branches within the groove before turning posteriorly to pass onto the diaphragmatic surface of the heart. Here the right coronary artery may anastomose with the left circumflex branch of the left coronary artery shortly after the origin of the posterior interventricular artery.
Branches
Sinoatrial nodal artery
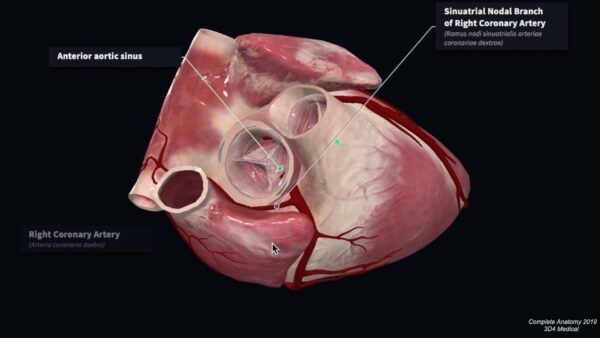
The sinoatrial (SA) nodal artery passes posteriorly between the right auricle and the ascending aorta to form an arterial ring around the termination of the inferior vena cava. It supplies the SA node in approximately 60% of cases. In some, this artery may arise from the left circumflex artery.
Right conus artery
The right conus artery passes upwards and medially on the anterior surface of the pulmonary conus. It often anastomoses with the corresponding branch from the left coronary artery to form an anastomosis around the pulmonary trunk. It supplies the anterior surface of the pulmonary conus and the anterior wall of the right ventricle
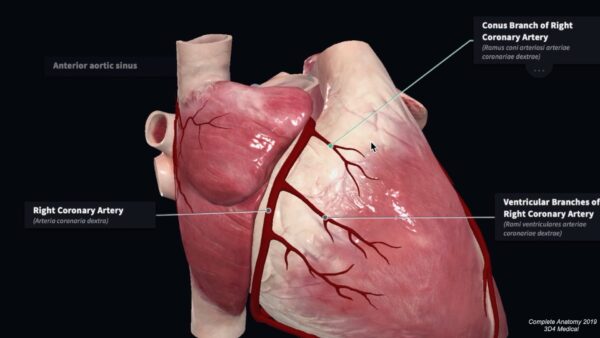
Right marginal artery
The right marginal artery is a large ventricular artery. It arises at the inferior border of the heart and passes along the lower margin of the heart towards the apex. This artery frequently arises higher on the anterior surface of the right ventricle.
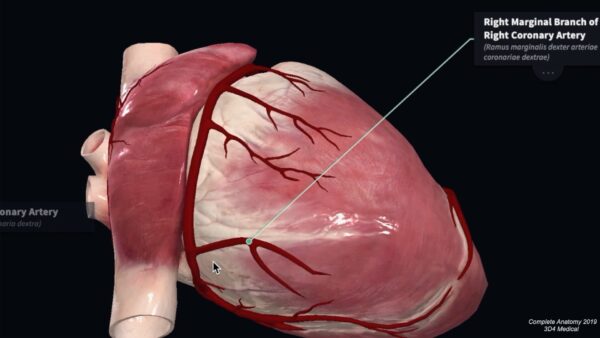
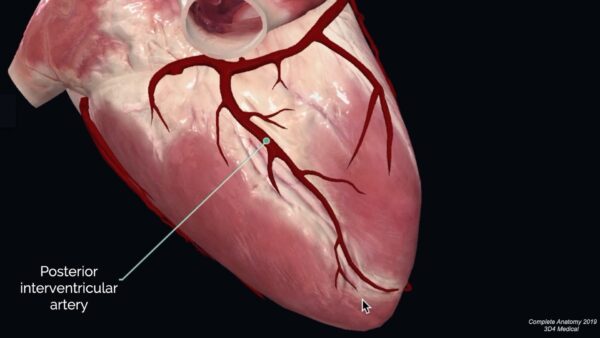
Posterior interventricular artery
The posterior interventricular branch arises on the diaphragmatic surface of the heart. It passes between the right and left ventricles within the interventricular groove. It supplies branches to the left and right ventricles, as well as the posterior portion of the interventricular septum. A large branch supplies the atrioventricular node. At the heart’s apex, it may anastomose with the anterior interventricular artery. In 10% of people, this branch may arise from the left circumflex artery.
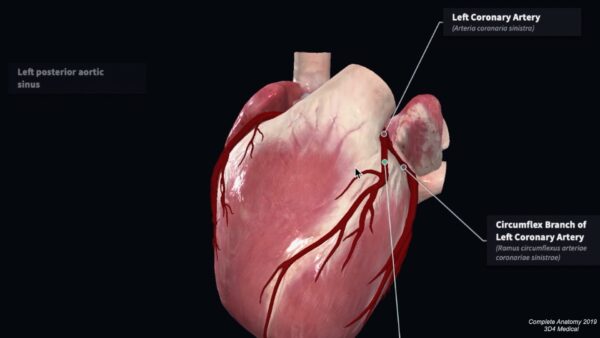
Left Coronary Artery
The left coronary artery arises from the left posterior aortic sinus. It passes behind the pulmonary trunk and emerges between the left auricle and the infundibulum of the right ventricle. The left coronary is the larger of the coronary arteries. It soon divides into two terminal branches: the circumflex and anterior interventricular branches.
Branches
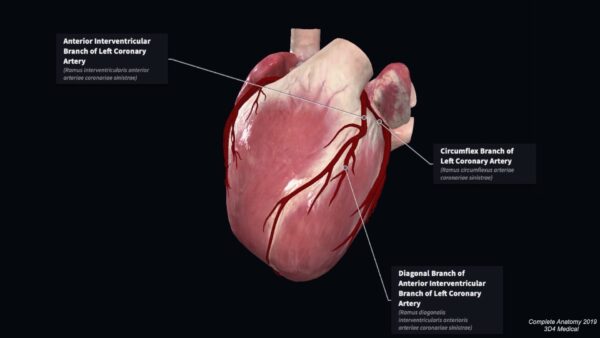
Anterior interventricular artery (left anterior descending artery)
This artery passes between the left and right ventricle within the interventricular groove towards the apex of the heart. Here it will often pass around the apex of the heart to anastomose with the posterior interventricular artery. In approximately one-third of individuals, it will terminate at the apex of the heart. It supplies the left and right ventricles, as well as the anterior portion of the interventricular septum.
Left conus artery
The left conus artery arises close to origin to supply the pulmonary conus. It may anastomose with the corresponding branch from the right coronary artery.
Ventricular branches
A number of left and right ventricular branches arise from the anterior interventricular artery. In 50% of individuals, a large diagonal artery passes along the anterior surface of the left ventricle. The diagonal branch may also arise directly from the trunk of the left coronary artery.
Circumflex branch
This terminal branch continues towards the diaphragmatic surface of the heart within the atrioventricular groove. It will give off a number of atrial and ventricular branches and often anastomoses with the right coronary artery on the diaphragmatic surface.
Left marginal artery
The left marginal artery passes along the left border of the heart towards the apex to supply the left border of the left ventricle.
Sinoatrial nodal artery
The sinoatrial (SA) nodal branch arises from the circumflex artery in approximately 40% of the population. If present, the SA nodal artery passes behind the ascending aorta towards the right atrium.
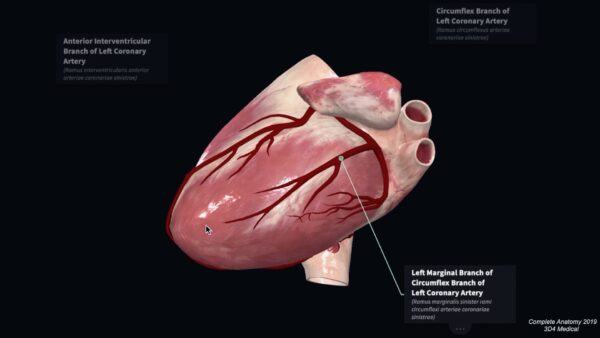
Coronary artery dominance
The coronary artery giving off the posterior interventricular artery determines coronary artery dominance. The posterior interventricular artery is most commonly a branch of the right coronary artery, but arises from the left circumflex branch in 10% of cases. Equal dominance occurs when branches from the right and left coronary arteries run within the posterior interventricular groove.
Coronary artery disease
The coronary arteries are essentially functional end arteries, though some anastomoses exist at the arteriolar level. Anastamoses can potentially occur between the arteries within the atrioventricular groove, the interventricular and conus branches. In slow occlusion, arterioles may develop between the branches described. However, these anastomoses are usually only sufficient in cases of slow, progressive coronary artery disease. Sudden occlusion of one of the larger branches of either coronary artery usually leads to myocardial death. Most cases of occlusion occur secondary to acute coronary artery thrombosis on a background of chronic atherosclerotic narrowing of the lumen.
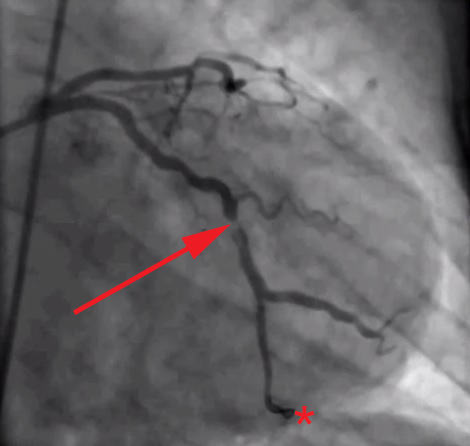
Sites of coronary artery occlusion
Table 1 lists the sites of coronary artery occlusion, in order of frequency. Sites 1-3 account for up to 85% of all occlusions. Coronary bypass surgery involves harvesting a vessel from an alternative site within the body. The vessel is either connected to the aorta or proximal coronary artery and then to the artery distal to the occlusion. Common candidates for vessel harvesting include the great saphenous vein and the radial artery.
| Order of frequency | Coronary artery |
| 1 | Proximal anterior interventricular branch |
| 2 | Proximal right coronary artery |
| 3 | Proximal left circumflex branch |
| 4 | Left coronary artery |
| 5 | Proximal posterior interventricular |
| 6 | Right coronary artery (diaphragmatic surface) |
Table 1: Coronary artery occlusion in order of frequency
You can purchase a licence for the Complete Anatomy software we use in our videos here (we also get a percentage of your purchase fee if you use this link).
References
Software
The images and video included in this article were produced using Complete Anatomy 2019 by 3D4 Medical. You can learn more about Complete Anatomy 2019 here.
Other resources
1. Moore, K., Dalley, A., & Agur, A. (2018). Clinically Oriented Anatomy. Philadelphia, PA: Wolters Kluwer.
2. Todt T, Maret E, Alfredsson J, Janzon M, Engvall J, Swahn E – Todt T, Maret E, Alfredsson J, Janzon M, Engvall J, Swahn E (2012). “Relationship between treatment delay and final infarct size in STEMI patients treated with abciximab and primary PCI”. BMC Cardiovascular Disorders. doi:10.1186/1471-2261-12-9. PMID 22361039. PMC 3359186.