- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Dupuytren’s contracture is a benign and progressive disorder of the hand. It involves the development of cords within the palmar fascia leading to contracture and flexion deformity, often localised to the ring finger.1
Epidemiology
Dupuytren’s contracture affects 4% of the UK population, with 20% of those affected being over 65.
The condition predominantly affects middle-aged men, especially those of a Scandinavian and Northern European background.1
Aetiology and risk factors
Although a specific cause has not been established, a number of risk factors have been identified: 1,2
- 70% of patients have a hereditary component
- Excessive alcohol intake
- Manual work – especially involving vibrational machinery3
- Smoking – smokers are 3 times more likely to develop the condition
- Diabetes mellitus – 1 in 5 diabetic patients develop the condition
Pathophysiology
The underlying sequence of events which lead to Dupuytren’s contracture is as follows:
- Myofibroblasts contract producing a thickening of the palmar aponeurosis.
- Clumping of the aponeurosis forms nodules and shortening of the aponeurosis forms pits.
- Fibroblasts then align along lines of tension due to altered collagen matrix, forming cords.
- As the disease progresses, fibrocytes become the dominant cell type, causing the cords to shorten leading and flexion deformities of the digits to develop.2
Clinical features
History
Initially, there is pitting, thickening and puckering of the palmar skin distal to the distal palmar crease.
Following this, a tender nodule can develop at the palmar crease (unlike the base of the finger seen in trigger finger).
The fibres form cords and over time contracture develops causing the fingers to become arched into flexion when the cords shorten.
Since the condition is largely painless, patients often present late once they are struggling with functional impairment.4
Clinical examination
Typical clinical findings include:
- Nodules +/- cords can be felt upon palpation of the palmar fascia.
- The ring finger is most commonly affected, followed by the 5th digit and the 3rd digit.
- Sparing of the index finger and thumb.
- Flexion deformity at the metacarpophalangeal (MCP) and proximal interphalangeal (PIP) joints.
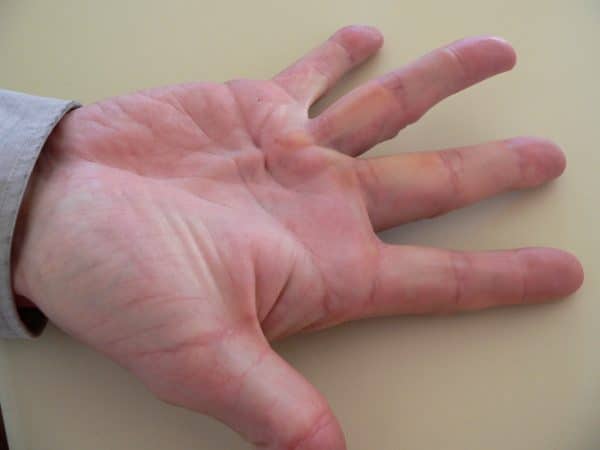
Hueston’s tabletop test:5
- The patient is asked to place their palms down onto a flat surface.
- The test is positive if the patient is unable to do this and there is greater than 30 degrees of flexion at the MCP.
Associated conditions
The following conditions also fall under the fibromatoses category and thus may also be seen in patients with Dupuytren’s disease:
- Plantar fibromatosis (Lederhosen disease) – affecting the sole of the foot
- Peyronie’s disease – affecting the penis
- Garrod disease – affecting knuckle pads
If these are present it indicates ectopic disease and signifies a likelihood that Dupuytren’s will become severe.2
Investigations and diagnosis
Consider checking lipids, LFTs and HbA1c given the association of Dupuytren’s with hyperlipidaemia, alcoholic liver disease and diabetes.4
Dupuytren’s is however primarily a clinical diagnosis.
Management
Conservative management
If a patient feels their Dupuytren’s is not significantly impacting their activities of daily living, reassurance and safety netting is recommended.
Interventions
Referral to a local hand clinic is recommended for patients who are experiencing significant functional impairment and/or if they have a positive tabletop test.4
Non-surgical management
Collagenase is an enzyme therapy that can be injected into palpable cords (outpatient procedure).1
Radiotherapy is also an option limited to the early stages of disease prior to contracture.6
Corticosteroids are not recommended.1
Surgical management
Surgery does not stop the disease process and so contractures are likely to recur.
It is important to warn patients of the risk of recurrence and that pre-morbid levels of functionality are unlikely to be achieved.
Percutaneous needle fasciotomy/aponeurotomy:
- Local anaesthesia is used
- A fine needle is used to break up the cords and nodules
Fasciectomy:
- A general anaesthetic is used
- Limited approach – only segments of the contracture are removed
- Regional approach – the entire cord is removed
- Dermofasciectomy is an extension of the regional approach, where the skin is also removed if there is significant involvement.
- Fasciectomy is usually the best option for recurrent disease.7
- With all surgical options, there is a risk of injuring nerves, vessels and tendons.
- Other risks include infection, pain, inadequate correction, haematoma and stiffness1.
- At five year follow up recurrence was found to affect 75% of those who underwent needle fasciotomy, 47% for collagenase injections and 20% for limited fasciectomy.7
Key points
- Dupuytren’s contracture is a painless but progressive condition where contracture of the palmar fascia causes flexion deformities.
- It typically affects men of Northern European descent over the age of 50.
- It is associated with Garrod’s disease, Peyronie’s disease and plantar fasciitis.
- Referral to a local hand clinic should be considered if, on clinical examination, there is over 30 degrees of flexion at the MCP joint or if the contracture is significantly interfering with the patient’s activities of daily living.
- Management options include reassurance, injection of collagenase, radiotherapy and surgical intervention.
Reviewer
Mr Abhijit Guha
Orthopaedic Surgeon
References
- NICE CKS. Dupuytren’s disease. Published in 2015. Available from: [LINK]
- Townley WA, Baker R, Sherppard N, Grobbelaar AO. Dupuytren’s contracture unfolded. 332, BMJ. Published in 2006.
- Lucas G, Brichet A, Roquelaure Y, Leclerc A, Descatha A. Dupuytren’s disease: Personal factors and occupational exposure. Am J Ind Med. Published in 2008.
- info. Dupuytren’s Contracture. What is Dupuytren’s Contracture?. Published in 2016. Available from: [LINK]
- Hueston JT. The Table Top Test. Published in 1982.
- NICE Guidance. Radiation therapy for early Dupuytren’s disease. Published in 2016. Available from: [LINK]
- Grazina R, Teixeria A, Ramos R, Sousa H, Ferreira A, Lemos R. Dupuytren’s disease: where do we stand? EFFORT Open Reviews. Published in 2019.
- Frank C. Müller. Dupuytren’s contracture photo. Licence: CC BY-SA. Available from: [LINK]




