- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Introduction
Erythema multiforme (EM) is a type IV hypersensitivity reaction which presents with a skin rash.
It is typically triggered by an infection (most commonly herpes simplex virus) however it can also develop secondary drug reactions. EM typically affects those aged between 20 to 40.1
Erythema multiforme is characterised by target-like lesions which appear on the hands and feet and progress proximally. It is an uncommon skin disorder, affecting less than 1% of the global population annually.2
Aetiology
While the pathophysiology of erythema multiforme is unclear, it is suspected that the immune system triggers an inflammatory cascade when exposed to viral, bacterial, or chemical components.2
Herpes simplex virus
Herpes simplex virus-associated erythema multiforme is caused by virus DNA fragments being deposited on distal skin cells by monocytes, attracting CD4+ T helper cells which release interferon-gamma and trigger the inflammatory cascade.3
HSV-1 is the most likely causative organism, however, HSV-2 and Mycoplasma pneumoniae are other possible causes.4
HLA-DQ3 is an important marker that can be used to differentiate herpes-associated erythema multiforme from other types of EM and cutaneous disorders.3
Medications
In drug-associated erythema multiforme, the inflammation is driven by tumour necrosis factor-alpha, involving CD8+ cells rather than the CD4+ cells associated with herpes simplex virus-associated EM.3
Drugs associated with the development of erythema multiforme include:4
- Anticonvulsants such as barbiturates and phenytoin.
- Non-steroidal anti-inflammatory drugs.
- Antibiotics including amoxicillin, ampicillin, sulphonamides and tetracyclines.
Erythema multiforme major
Erythema multiforme major affects one or more mucous membranes in addition to the skin; most commonly the oral mucosa.1
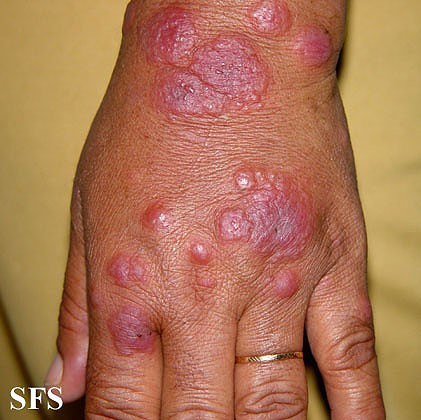
The lesions in this form of erythema multiforme are more likely to blisters which can spontaneously burst.4
It is important to note that while this form of erythema multiforme looks similar to Stevens-Johnson syndrome, they are separate conditions which are differentiated by skin biopsy.
Risk factors
The main risk factors for erythema multiforme include:5
- Previous episodes of EM
- Herpes simplex (1 or 2) infection
- Mycoplasma pneumoniae infection
Other potential risk factors include:
- Exposure to causative medications
- Hepatitis B vaccination
- Syphilis
- Epstein-Barr virus
- Cytomegalovirus
- HIV infection
- Hepatitis B
- Lymphoma
- Tattoos
Clinical features
Erythema multiforme minor
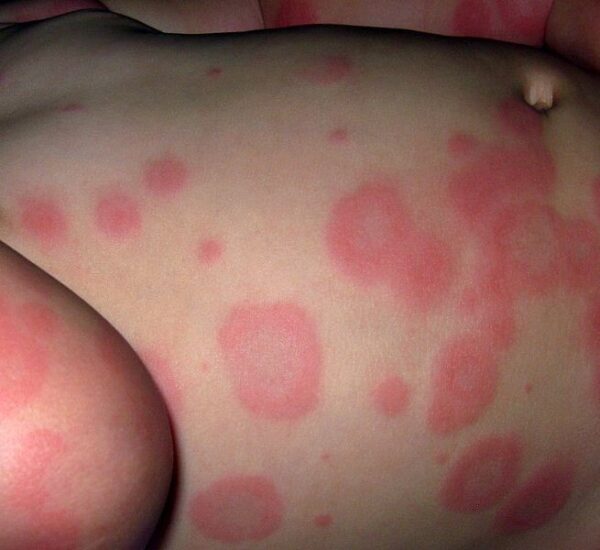
Erythema multiforme minor typically features no prodromal symptoms and classically starts with round erythematous macules.1 These macules then develop into papules which then progress to the target lesions characteristic of erythema multiforme.6
The target lesions have a dark centre with a blister or a crust, surrounded by a pale oedematous ring, which is then surrounded by an outermost darker ring. Atypical lesions can also occur which have only two zones.1
EM minor has a polymorphous pattern due to the different stages of lesion development so a thorough examination may be necessary to identify the target lesions.1 EM minor lesions may also be pruritic, so excoriation marks may be noted.
The distribution of lesions typically involves the acral and extensor surfaces of the extremities. These lesions then progress proximally towards the trunk (however the trunk is usually less affected).6
Erythema multiforme major
Erythema multiforme major typically involves prodromal symptoms including weakness, painful joints and fevers that present around one week prior to the cutaneous manifestations of the disease.1,6
EM major also affects at least one mucous membrane resulting in superficial lesions associated with local erythema and oedema.6 The oral mucosa is most often affected; however, other mucosal sites can be involved including genital, gastrointestinal, ocular and respiratory sites.1,6
Differential diagnoses
Differential diagnoses that should be considered include:9
- Urticaria
- Dermatitis herpetiformis
- Vasculitis
- Pemphigus
For those with mucosal involvement, the differentials include:
- Hand, foot and mouth disease
- Aphthous stomatitis
- Herpetic stomatitis
- Steven-Johnson syndrome
Investigations
In most cases, the diagnosis of erythema multiforme is made based on clinical examination findings alone.2
If there is diagnostic uncertainty, a skin biopsy can be performed. Histology typically reveals the following:⁸
- Apoptotic and degenerative keratinocytes at the base of the epidermis
- Spongiosis and blisters in the epidermis
- Small areas of epidermal necrosis (large sheets of epidermal necrosis are often seen in toxic epidermal necrolysis and Stevens-Johnson syndrome)
- Superficial dermal oedema and eosinophilic infiltrates in the dermis
- Perivascular lymphocytic infiltrate along the dermo-epidermal junction
Further investigations can be performed to determine whether herpes simplex or mycoplasma is the cause of erythema multiforme (e.g. swabs, sputum sample, chest X-ray).2
Management
Most cases of erythema multiforme require no treatment as the condition is self-limiting. However, if erythema multiforme develops secondary to an infective cause, this should be treated.
Acyclovir is used to treat herpes simplex infections and doxycycline is used to treat mycoplasma infections.
Other supportive management options include:1
- Oral antihistamines and topical corticosteroids: to reduce pruritis.
- Mouthwashes which have antiseptic and local anaesthetic components: to help with oral pain.
- Ophthalmological input: if there is ocular involvement.
- Oral acyclovir (taken for 6 months): for recurrent erythema multiforme (even if herpes simplex is not an obvious trigger).
- Hospital admission: if there is severe oral involvement. Hospitalisation is to aid with nutrition and fluid balance as well as preventing secondary infection of the lesions.
Complications
Erythema multiforme minor will usually resolve spontaneously over two to three weeks while erythema multiforme major can take up to six weeks to completely resolve. There may be mild skin discolouration following this condition, but scarring is rare.1
Secondary infection may develop at sites of EM.
Eye involvement in erythema multiforme major can result in scarring and reduced visual acuity.1
Key points
- Erythema multiforme has two forms: minor and major. The major form includes mucosal involvement of at least one site (e.g. oral mucosa).
- EM is most commonly caused by herpes simplex infection.
- Target lesions are the defining feature of EM.
- EM is self-limiting, only supportive treatment is required in most cases.
- Complications can include skin discolouration, secondary infection and reduced visual acuity (if there is ocular involvement).
Reviewer
Dr Leah Mapara
Clinical fellow in dermatology
Editor
Dr Chris Jefferies
References
- DermNet NZ. Erythema Multiforme. Published in 2015. Available from: [LINK]
- Plaza, J. Erythema Multiforme. Published in 2020. Available from: [LINK]
- Lamoreux M, Sternbach M, Hsu T. Erythema Multiforme. Published in 2006. Available from: [LINK]
- Stinson A. What To Know About Erythema Multiforme. Published in 2018. Available from: [LINK]
- BMJ Best Practice. Erythema Multiforme. Published in 2018. Available from: [LINK]
- Sokumbi O, Wetter D. Clinical features, diagnosis, and treatment of erythema multiforme: a review for the practicing dermatologist. Published in 2012. Available from: [LINK]
- Figure 1. Grook Da Oger. Erythema Multiforme EM. Licence: [CC-BY-SA]. Available from: [LINK]
- Figure 2. Dermatology Atlas. Erythema multiforme. Available from: [LINK]
- Benedetti J. Erythema Multiforme. Published i2020. Available from: [LINK]
- DermNet NZ. Erythema multiforme: histological features and mechanisms. Published in 2009. Available from: [LINK]