- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Introduction
Impetigo is a common superficial bacterial infection of the skin, often caused by Staphylococcus aureus (most common) or Streptococcus pyogenes.¹
It most often affects children but can present at any age, with an annual incidence of 2.8% in children up to 4 years old and 1.6% in children who are 5-15 years old.²
Impetigo can present in the non-bullous or bullous form. Non-bullous impetigo is the most common and recognisable form and presents as the typical, crusted honey-coloured lesions.
Aetiology
Non-bullous impetigo
Non-bullous impetigo is usually caused by bacteria (Staphylococcus aureus or Streptococcus pyogenes) entering the skin through a site of minor trauma.¹
Bullous impetigo
Bullous impetigo is similar to non-bullous impetigo but is usually caused by staphylococcus bacteria which invade intact skin and damage the superficial epidermis, eventually forming blisters or bullae.¹
Risk factors
Any pre-existing damage to the skin barrier (such as atopic eczema) or trauma to the skin can predispose an individual to developing impetigo.
Clinical features
Non-bullous impetigo
Small fluid-filled vesicles or pustules form at the affected site, these then progress over hours to days into the characteristic honey-coloured crusted lesions.
These commonly appear on the hands or face, particularly around the mouth or chin area.
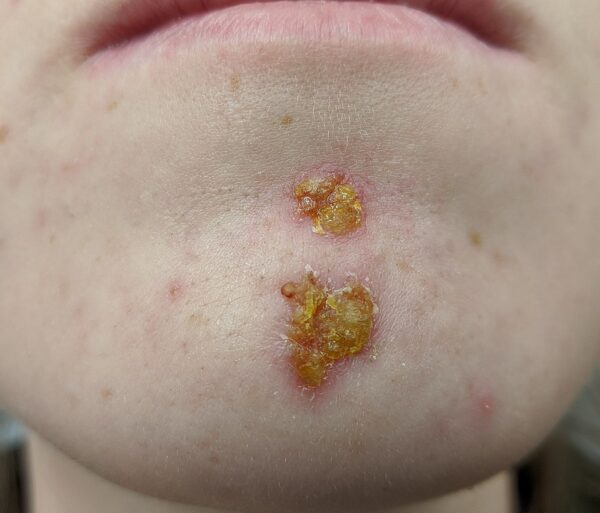
Bullous impetigo
Similarly to non-bullous impetigo, bullous impetigo begins with small fluid-filled vesicles, but these continue to progress into large fluid-filled blisters or bullae which rupture easily.
It is more likely to occur in areas of pre-existing eczematous skin but can occur anywhere on the body. Bullous impetigo can be painful, and patients can feel generally unwell.
Bullous impetigo tends to commonly affect infants, but can occur at any age.²
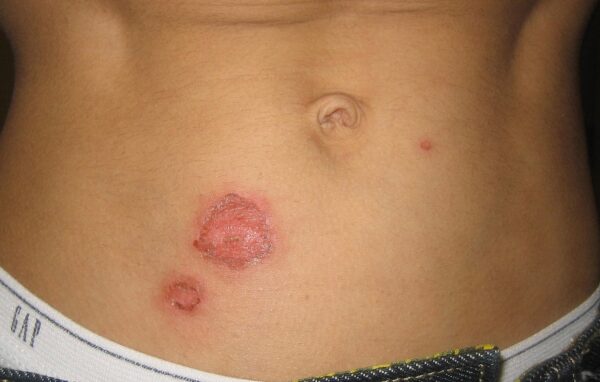
Differential diagnoses
Differential diagnoses to consider in the context of impetigo include:
- Herpes simplex virus: this can present similarly with small crops of vesicles, which erode and are typically painful in nature. These can present around the mouth (type 1) or the genitalia following sexual contact (type 2).
- Chickenpox: caused by the varicella-zoster virus; this most commonly presents in children with general malaise and fever accompanied by crops of vesicles which progress to become pustular before crusting over.
- Cellulitis: often presents with a demarcated area of erythema, swelling and warmth. There are usually no vesicles or pustules present.
- Bullous pemphigoid: this most commonly presents in the elderly with tense, large blisters on the limbs or trunk.
- Steven-Johnson syndrome / toxic epidermal necrolysis: patients may have a flu-like prodrome before a painful rash forms, this typically spreads within hours; the affected skin will then blister before desquamation occurs.
Investigations
Impetigo is usually a clinical diagnosis based on examination findings.
However, swabs of the affected area can be sent for culture. Indications for sending a swab include:
- An extensive area of skin is affected
- The lesions do not respond to treatment
- Methicillin-resistant Staphylococcus aureus (MRSA) infection is suspected
Management
Conservative management
Conservative management for all patients with impetigo includes:
- Hygiene advice such as regular hand washing, avoiding touching the affected area and not sharing towels with other people.
- Advice not to attend school or work until the lesions are dry and crusted over, or have had 48 hours of oral antibiotics.
Medical management
Patients with impetigo should be referred urgently to secondary care if they are presenting with complications of impetigo or are immunocompromised and have widespread impetigo.
Non-bullous impetigo
If localised, offer a 5-day course of hydrogen peroxide 1% cream. If more widespread, a topical antibiotic such as can be used such as fusidic acid 2% or mupirocin 2%.
Oral antibiotics such as flucloxacillin can be used if systemically unwell or at high risk of complications.
Bullous impetigo
Offer all patients with bullous impetigo an oral antibiotic such as flucloxacillin and consider referral to a dermatologist for further assessment.
Complications
Complications of impetigo include:
- Superadded infection of the impetiginous lesions can lead to cellulitis and even sepsis. It is important to assess the patient thoroughly and record basic observations (vital signs).
- In the rare event that impetigo is caused by Group A β-haemolytic streptococcus, this can lead to the development of scarlet fever or glomerulonephritis.
Any patient presenting with complications associated with impetigo requires urgent referral to secondary care.
Key points
- Impetigo is a common superficial skin infection most commonly caused by Staphylococcus aureus.
- The most common form of impetigo is the non-bullous form. Infection occurs via breaks in the skin barrier which allow entry of bacteria, causing the formation of small crops of vesicles which eventually rupture to form the characteristic golden-honey-crusted lesions.
- In bullous impetigo, bacteria invade the intact skin barrier and form bullae which rupture easily.
- Diagnosis is usually made based on clinical examination findings.
- Non-bullous impetigo usually heals quickly and effectively with topical treatment such as hydrogen peroxide or fusidic acid.
- Oral antibiotics should be offered to all patients with bullous impetigo.
- For both forms, strict hygiene measures are required to prevent the spread to other people.
- Complications are rare but will require urgent referral to secondary care should they occur.
Reviewer
Dr Thomas King
Consultant Dermatologist
Editor
Dr Chris Jefferies
References
- DermNet NZ. Impetigo. Last updated 2022.Available from: [LINK]
- NICE CKS. Impetigo. Last updated 2020. Available from: [LINK]
Image references
- Figure 1 James Heilman, MD. Impetigo2020. Licence: [CC BY-SA]
- Figure 2 Littlekidsdoc. Bullous impetigo1. Licence: [CC BY-SA]




