- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Introduction
Mumps is an acute, generalised viral infection characterised by bilateral parotid swelling.1
Prior to the introduction of the measles, mumps, and rubella (MMR) vaccine in 1987, it was common in children, but outbreaks are now more common among young adults at university, especially those who did not receive the MMR vaccine.1
There were over 5000 cases of mumps in England in 2019, more than in any year since 2009.2
Aetiology
Mumps is a viral infection caused by a paramyxovirus, usually affecting children or young adults.1
Although it can infect any organ, the salivary glands are most commonly affected. Less often affected are the testes, ovaries, pancreas, and brain.1
Mumps virus is highly infectious and is spread by respiratory droplets and saliva.3
It has an incubation period of 16 to 18 days, and transmission rates are highest one to two days prior to the onset of symptoms. Almost all of those infected subsequently develop life-long immunity.3
Clinical features
15-20% of those infected with the mumps virus are asymptomatic.3
There is usually a prodrome of non-specific, flu-like symptoms which include fever, headache, malaise, myalgia and anorexia.3
Parotitis (swelling of the parotid glands) then develops in 95% of symptomatic cases and usually lasts three to four days, although can last up to ten.3,1
Mumps is also associated with orchitis and meningitis/encephalitis (see complications section).
Mumps parotitis
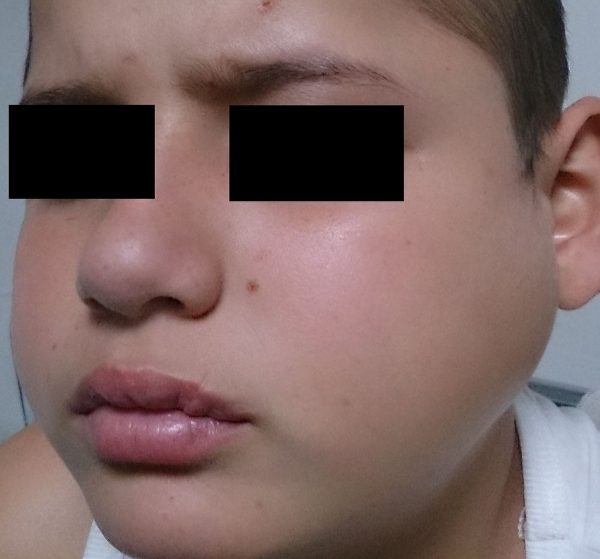
Mumps parotitis is generally bilateral. It causes distortion of the face and neck, giving the distinctive ‘hamster face’ appearance (Figure 2).2
The skin can be hot and flushed, but there is no rash. Parotitis is also commonly associated with pain near the angle of the jaw, dry mouth, and reduced opening of the mouth.
Differential diagnoses
High fever with associated neck pain and swelling can be caused by other infections including pharyngitis, tonsillitis, infectious mononucleosis and HIV.1
Parotid stones can also cause pain and swelling but are usually unilateral and occur in older patients. In this case, chewing causes pain as saliva is produced.1
Unilateral testicular swelling and pain can be caused by testicular torsion (although here there are no preceding systemic symptoms, and the testicle has a horizontal lie).1 Bilateral testicular swelling should prompt consideration of epididymo-orchitis caused by sexually transmitted infections.
Meningitis and encephalitis can be caused by other infectious (viral, bacterial, fungal) and non-infectious (neoplastic) agents.6 For more information, see the Geeky Medics guide to meningitis.
Investigations
Mumps is usually a clinical diagnosis, but confirmation (via a salivary sample) is required as it is a notifiable disease.1
Further investigations are also required if patients present with meningitis/encephalitis or orchitis to look for other causes.
Management
Mumps is a self-limiting condition, and most children recover within one to two weeks.1,3
Supportive management may include simple analgesia (paracetamol and ibuprofen), advice regarding fluid intake and rest.
Admission to hospital is required if there are concerns about complications (e.g. meningitis or encephalitis).3
Children should not attend school for five days following the development of parotitis.3
Vaccination
The MMR (measles, mumps and rubella) vaccination is part of the national immunisation programme. The efficacy of the MMR vaccine (both doses) against mumps is 88%.7
If a person is exposed to mumps and has not been fully immunised, MMR should be offered (in the absence of contraindications).3
For more information, see the Geeky Medics guides to childhood immunisations and childhood immunisation counselling.
Complications
Orchitis (or epididymo-orchitis)
Mumps orchitis often occurs without parotitis, but if both are present, orchitis generally develops four or five days after the parotitis onset.1
Orchitis is found in 25% of post-pubertal males with mumps and is bilateral in 15-30% of cases.1,3
It is associated with severe testicular pain and tenderness. Significant scrotal oedema may make the testes impalpable. Bilateral orchitis may lead to subfertility.1
Meningitis and encephalitis
Mumps meningitis and encephalitis also usually occur without parotitis.1
In patients infected with the mumps virus, 15% develop meningism.8 Although mumps meningitis is usually mild and self-limiting, mumps encephalitis has a mortality rate of 1.5%.1,9
Mumps encephalitis is rare, and may present as part of the initial infection, or later in the disease course.1
Other complications
Other complications include oophoritis, deafness (usually unilateral and transient) and pancreatitis.1
Key points
- Mumps is an acute viral infection caused by a paramyxovirus, which generally affects children and young adults.
- The clinical presentation is of flu-like symptoms followed by bilateral parotitis. However, 15-20% of those infected with the mumps virus are asymptomatic.
- Mumps is usually a clinical diagnosis, but confirmation (via a salivary sample) is required as it is a notifiable disease.
- Mumps is a self-limiting condition, and most children recover within one to two weeks.
- If a person is exposed to mumps and has not been fully immunised, MMR vaccination should be offered (in the absence of contraindications).
- Complications of mumps include orchitis, meningitis and encephalitis.
Reviewer
Dr Jennifer Mackintosh
Paediatric registrar
Editor
Dr Chris Jefferies
References
- Patient.info. Mumps. Last edited September 2020. Available from: [LINK]
- GOV.UK. Mumps outbreaks across England. Published February 2020. Available from: [LINK]
- NICE CKS. Mumps. Last revised December 2018. Available from: [LINK]
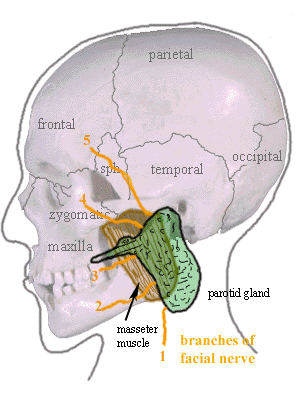
- Memorial University Newfoundland. Parotid gland. License: [CC BY-SA]
- Afrodriguezg. Parotiditis (Parotitis; Mumps). License: [CC BY-SA]
- Geeky Medics. Meningitis. Last updated October 2020. Available from: [LINK]
- Harling et al. The effectiveness of the mumps component of the MMR vaccine: a case control study. Published July 2005. Available from: [LINK]
- Balbi et al. Mumps: Resurgence of a once-dormant disease. Published May 2018. Available from: [LINK]
- Orlíková et al. Protective effect of vaccination against mumps complications, Czech Republic, 2007-2012. Published April 2016. Available from: [LINK]