- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Everyone loves the term ‘supraventricular tachycardia’. It describes any fast heart rate that you aren’t sure what it is and usually triggers an immediate cardiology referral after a certain amount of panic. However, with a bit of thought (and possibly some adenosine), the underlying diagnosis can be revealed and appropriate treatment can be started.
Firstly, a statement…SUPRAVENTRICULAR TACHYCARDIA IS NOT A DIAGNOSIS
A ‘supraventricular tachycardia’ is a rapid heart rate that originates from above or within the atrioventricular (AV) node. It is a blanket term that includes a lot of different rhythms and is simply a starting point on the road to diagnosis. To divide up this myriad of possibilities, a bit of basic electrophysiology terminology needs to be applied.
Focal Tachycardias
The tachycardia originates from a single point (or points) in the atrium or AV node. Also knows as ‘enhanced automaticity’ – the sinus node is meant to be the most autonomic part of the heart and as such takes charge. If another part of the heart becomes MORE autonomic (or the sinus node becomes LESS autonomic), it takes over and a focal tachycardia results. This means there will be an organised atrial contraction and a wave similar to a P wave will appear before the QRS complex.
Sinus tachycardia
- Yes, this is a focal tachycardia
- The ‘focus’ is the sinoatrial node!
- Usually regular
Atrial tachycardia
- A different focus in the atrium takes over from the sinoatrial node resulting in ABNORMAL P waves preceding QRS complexes
- Often seen in patients with chronic lung disease
- Normally > 100 bpm and regular
- ‘Normal’ P waves should LOOK like a regular P wave and should be POSITIVE in the inferior leads (as they originate from the top of the atrium and propagate towards the inferior lead)
- Atrial tachycardia is common amongst patients with concomitant lung disease (e.g. COPD)
Multifocal atrial tachycardia
- The name says it all!
- The P waves will have different morphologies as the atrial focus changes from beat to beat.
- Similar to atrial tachycardia in all other respects.
Junctional rhythms
- The atrioventricular node is the next most autonomic piece of tissue in the heart after the sino-atrial node. If the sinoatrial node is not functioning (e.g. high vagal tone, sick sinus syndrome), the AV node takes over.
- The impulse originates from the AV node and propagates to the atrium and the ventricles simultaneously.
- P waves are often hidden in the QRS complex.
Management
- INAPPROPRIATE sinus tachycardia can be slowed using beta-blockers or ivabradine (selective sinus node blocker), however it is usually best left alone.
- APPROPRIATE sinus tachycardia (due to concurrent sepsis/anaemia/thyrotoxicosis/pain) should be left alone and the underlying trigger treated.
- Atrial tachycardias can usually be rate controlled with beta-blockers or calcium channel blockers.
Re-entry tachycardias
These account for more than 75% of all tachyarrhythmias, both atrial and ventricular.
Atrial flutter
- Well known for its sawtooth baseline (see below), atrial flutter is a MACRO-RE-ENTRANT tachycardia.
- This means there is a single large re-entry circuit around the atrium which stimulates the AV node every time it passes.
- TYPICAL atrial flutter runs anti-clockwise around the right atrium and across the cavotricuspid valve isthmus.
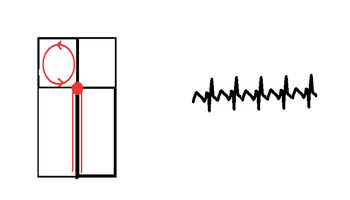
- ATYPICAL flutter can be clockwise in the right atrium, in the left atrium or around sites of previous surgery and can be difficult to identify as they lack the typical sawtooth appearance. However, flutter should be suspected in ANY regular tachycardia at or around 150bpm.
- The sawtooth appearance is best seen in the inferior leads and is caused by the circuit alternately heading towards the inferior leads and away as it speeds around the atrium.
- As the circuit is fixed, the rate of atrial contraction is constant (depending on the size of the atria – in a normal-sized chamber, flutter waves are around 300bpm but patients with dilated atria can have much slower circuits).
The ventricular rate then depends on the degree of AV block:
- 2:1 = 150bpm
- 3: 1 = 100bpm
- Variable – can produce an irregularly irregular rhythm
Atrial fibrillation
- The mechanism of AF is complex and not entirely clear. The easiest way to think of it is as a MICRO-RE-ENTRANT tachycardia with lots of tiny circuits contributing to the chaotic and random fibrillation of the atrium.
- As such, you can sometimes see the very rapid F (fibrillation) waves on the baseline and the absence of P waves.
- AF is irregularly irregular because of this disorganised activity – the rate, again, depends on the degree of AV block
AVNRT (atrio-ventricular node re-entrant tachycardia)
This is the rhythm that always gets labelled as an ‘SVT’.
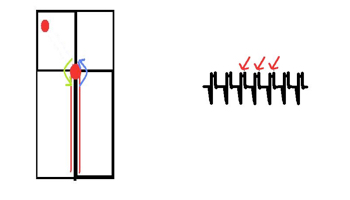
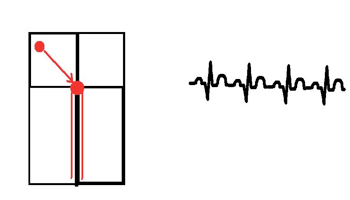
Because it is technically WITHIN the node, the resulting circuit activates both the ventricles and atria almost simultaneously. Two anatomical pathways next to the AV node (the slow and fast pathways) form a circuit with very rapid conduction that produces a rapid regular tachycardia. This is seen as a ‘pseudo R wave’ (see the RED arrows) which is actually the retrograde P wave superimposed on the QRS complex. Treatment involves inducing complete transient AV node blockade.
AVRT (atrio-ventricular re-entrant tachycardia)
This requires two pathways – the normal AV conduction system and an accessory pathway (AP).
Accessory pathways can conduct:
- ANTEGRADE (atria to ventricles) which is shown as pre-excitation on the resting ECG (the mythical DELTA wave)
- RETROGRADE (ventricle to atria) which is not seen on a resting ECG
Not all AP’s can form AVRT circuits – this is because they have a long ‘refractory period’ which is the time it takes the pathway to become active again after it has conducted an impulse. Therefore the impulse has travelled the rest of the circuit BEFORE the AP is ready to receive it again and the circuit is terminated. These are ‘safe’ pathways and do not need treatment.
Types of AVRT’s
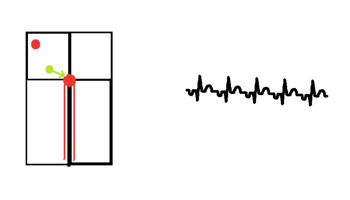
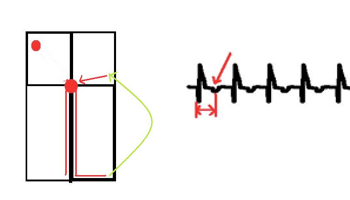
ORTHODROMIC – down the AV node and up the accessory pathway (in green)
- As the impulse goes down the normal conduction pathway, the QRS complex is narrow.
- The impulse then propagates slowly across the ventricular myocardium before reaching the accessory pathway and heading back to the atrium resulting in a delay in atrial activation. This results in a LONG RP interval (marked on the above diagram) before the P wave (arrow) which marks the atrial contraction.
- COMPARE this to the AVNRT section above where the P wave is almost superimposed on the QRS complex (a pathognomonic feature).
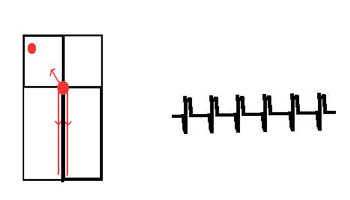
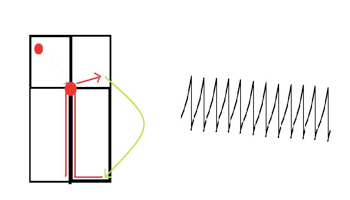
ANTIDROMIC – down the accessory pathway and up the normal AV conduction
- As the impulse goes down the AP, the ventricular contraction starts in an abnormal way (pre-excitation).
- Therefore, the ECG will have a broad QRS complex caused by the presence of delta waves.
- DO NOT USE AV NODAL BLOCKING AGENTS. This promotes transmission down the accessory pathway and if there is AF, the fibrillation waves can be transmitted to the ventricles……….causing VF.
Management of AVRT’s
- The safest way to deal with AVRT’s is to electrically cardiovert the patient back to sinus rhythm and worry about medical therapy later!
- Flecainide can be used to prevent AVRT’s but ablation is usually the mainstay of treatment given the risk of VF and sudden death.
Treating re-entrant ‘SVT’s’
As you can see, the varying mechanisms of the different SVT’s mean that the treatment of each arrhythmia will vary.
IF THE PATIENT IS HAEMODYNAMICALLY UNSTABLE DUE TO THE UNDERLYING RHYTHM, DC CARDIOVERSION IS THE TREATMENT OF CHOICE (as per ALS algorithms).
Atrial Fibrillation and Atrial Flutter
RATE control:
- Beta-blockers
- Calcium channel blockers
- Digoxin
RHYTHM control:
- Chemical cardioversion (amiodarone, flecainide)
- Electrical cardioversion (DC shock)
Ablation:
- More likely to succeed in atrial flutter than atrial fibrillation 95% vs 60-80%
- More likely to succeed in paroxysmal AF than persistent AF
- 1 in 3000 risk of death during the procedures
Anticoagulation:
- According to stroke risk vs bleeding risk (CHADS2 VASc score)
Choosing a treatment strategy
Which strategy you adopt depends on the patient and a couple of key facts:
- AF is NOT life-threatening
- A patient with well-controlled AF and normal LV function has the same life expectancy as someone in sinus rhythm.
- Therefore, symptomatic patients with well rate controlled AF will not feel better or live longer by returning them to sinus rhythm!
Patients who should be considered for cardioversion:
- New-onset AF
- Symptomatic AF
- LV dysfunction secondary to AF
- Patients with a reversible cause of AF (e.g. post-surgical, post-infection)
- Patients who have a reasonable chance of maintaining sinus rhythm:
- Previous successful cardioversion – although subsequent cardioversions are often less and less successful in terms of time spent in sinus rhythm
- Minimal dilatation of the left atrium
- No significant mitral valve disease
AVNRT
Induce AV node blockade and the tachycardia is terminated:
- Mechanical (vasovagal manoeuvres, carotid sinus massage)
- Chemical (adenosine, beta-blockers, verapamil)
AVRT
- AVOID AV node blockade as this can promote conduction down the AP and AF can transmit to VF.
- Electrical cardioversion is the best initial option although flecainide can be used to chemically cardiovert.
- Ablation of the pathway is a curative option. Should be considered in all antidromic AVRT’s because of risks of VF and death if AF were to occur, symptomatic retrograde AVRT’s and is MANDATORY in airline pilots and deep-sea divers!
Using Adenosine
Adenosine is a purine nucleoside that, administered intravenously, causes transient complete AV node blockade. It is a useful diagnostic tool as well as a treatment in the setting of a narrow complex tachycardia.
NOTE:
- Adenosine is safe in pregnancy
- It can also usually be used safely in asthmatics unless they have brittle severe asthma
Administering adenosine
1. Place a LARGE (green or grey) cannula in the antecubital fossa.
2. Ensure the patient is connected to 12 lead monitoring which can produce a rhythm strip.
3. Draw up the adenosine in the smallest syringe possible (2-5ml depending on the dose).
4. Draw up a 20ml normal saline flush.
5. Connect the adenosine syringe to the top port of the cannula and the flush to the backport – any delay in flushing the medication will mean that it will not reach the heart in time!
6. Warn the patient that they will about the upcoming ‘sense of impending doom’ that will pass after a few seconds.
7. Start the 12 lead rhythm strip recording.
8. Give the adenosine AS FAST AS POSSIBLE followed IMMEDIATELY by the full saline flush AS FAST AS POSSIBLE.
9. Observe the rhythm strip for AV block.
Effects of adenosine
If you have administered the adenosine correctly, you will see a few seconds of total AV block (a complete pause in ventricular contraction on the rhythm strip). DO NOT PANIC!!!
If you do NOT see AV block, one of two things have occurred:
1. You haven’t given it properly and the adenosine has not reached the heart in time given its very short half-life. Try again with a bigger dose and faster flush.
2. The rhythm is not involving the AV node – it is, therefore, VENTRICULAR TACHYCARDIA.
If you terminate the tachycardia, the rhythm is an AVNRT or an orthodromic AVRT (as you have cut the AV node out of the circuit).
If you pause the tachycardia but it then restarts as the effects wear off, you have demonstrated that the tachycardia is SUPRAVENTRICULAR but you have not terminated it. However, you have proved that the re-entry circuit does NOT involve the AV node (or it would have been terminated) – such as atrial flutter or atrial tachycardia. The short period of AV block will reveal what the atria are up to and give you the diagnosis.
Example of atrial flutter when adenosine is administered
- AV block attained confirming a supraventricular tachycardia.
- The atrial activity is shown to be flutter waves.
- The rhythm continues, demonstrating the circuit does not involve the AV node.

Summary
- Supraventricular tachycardias can be a challenge to diagnose.
- However, by systematically working through the ECG (rhythm, presence of P waves, P wave morphology) and applying a little adenosine if needed, the diagnosis can be made and management put in place.




