- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
This guide aims to provide a structured approach to performing a newborn baby assessment (NIPE) in an OSCE setting.
Background
The Newborn Infant Physical Examination (NIPE) must be performed within 72 hours of birth by a qualified practitioner.¹
The purpose of the examination of the newborn is: ²
- To screen for congenital abnormalities that will benefit from early intervention
- To make referrals for further tests or treatment as appropriate
- To provide reassurance to the parents
A second examination is performed at 6-8 weeks of age, usually by GP, to identify abnormalities that develop or become apparent later.
Where to perform the NIPE
The NIPE exam should be undertaken in a private area which provides confidentiality for parents when personal information is being discussed.
The room should be warm and well lit (preferably natural light, especially if jaundice is to be assessed).² Visual inspection, however, cannot reliably assess the level of jaundice so if this is suspected a bilirubin level needs to be checked. ³
You’ll ideally require a changing mat to carry out the examination on.
Always make sure that the parents are present for the newborn check as this is an ideal time to answer queries and provide reassurance.
Introduction
Wash your hands and don PPE if appropriate (alcohol gel must dry completely before handling the newborn).
Introduce yourself to the parents including your name and role.
Confirm the infant’s name and date of birth.
Briefly explain what the examination will involve using patient-friendly language: “Today I need to carry out a routine head to toe examination of your child.”
Gain consent to proceed with the examination:
- Parents should have received the National Screening Committee leaflet ‘Screening tests for you and your baby’ in the antenatal period.
- If the parents have not read the information booklet they must be given a copy to read before to the examination.
- The aims and limitations of the examination should be fully explained.
Adequately expose the child for the assessment: ask the parents to undress the child down to their nappy.
Encourage the parents to ask questions during the check and to participate where appropriate.
The optimal way to perform the newborn check is by examining from head to toe sequentially. In reality, it’s an opportunistic examination – if the baby is settled listen to their heart first, if they open their eyes check the fundal reflexes and if they’re crying look at the palate!
Questions to ask the parents
Below are some key points you would ideally cover in a full assessment of a newborn baby. It should be noted that in the context of an OSCE you are unlikely to be expected to cover all these history points due to time constraints.
Maternal history:
- Pregnancy details: date/time and type of delivery/complications/high-risk antenatal screening results
- Breech presentation: if breech at 36 weeks gestation or delivery (if earlier), the baby will need to have an ultrasound scan of their hips as there is an increased risk of developmental dysplasia of the hip.
- Risk factors for neonatal infection
- Abnormalities noted on antenatal scans
- Family history: first-degree relatives with…hearing problems/hip dislocation/childhood heart problems/congenital cataracts/renal problems
Newborn history:
- Feeding pattern
- Urination
- Passing of meconium
- Parental concerns
Weight
Ensure that the infant’s weight is recorded and check on a weight chart whether the baby is:
- Small for gestational age (<10th centile)
- Appropriate weight for gestational age (10th-90th centile)
- Large for gestational age (>90th centile)
If a baby is small, you should also plot head circumference and length to determine whether this is symmetrical (small in all measurements) or asymmetrical (weight disproportionately low, head circumference preserved).
Asymmetrical growth restriction is commonly due to placental insufficiency, whilst symmetrical growth restriction is more commonly due to fetal factors such as genetic abnormalities or intrauterine infection.
General inspection
Inspect the colour of the infant:
- Pallor: a pale colour of the skin that can suggest underlying anaemia (e.g. haemorrhage) or poor perfusion (e.g. congestive cardiac failure).
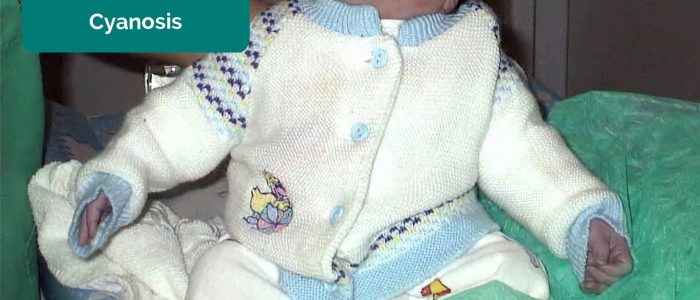
- Cyanosis: a bluish discolouration of the skin due to poor circulation (e.g. peripheral vasoconstriction secondary to hypovolaemia) or inadequate oxygenation of the blood (e.g. right-to-left cardiac shunting).
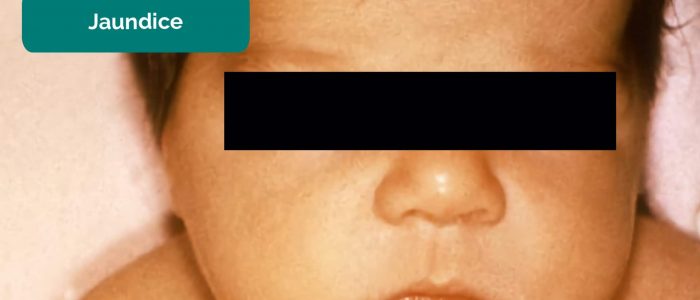
- Jaundice: a yellowish or greenish pigmentation of the skin and whites of the eyes due to high bilirubin levels (e.g. newborn jaundice).
Inspect the posture of the infant: note any gross abnormalities of posture (e.g. hemiparesis/Erb’s palsy).
Tone
Assess tone by gently moving the newborn’s limbs passively and observing the newborn when they’re picked up (your assessment of tone should continue throughout the examination).
Hypotonic infants are often described as feeling like a ‘rag doll’ due to their floppiness. Hypotonic infants often have difficulty feeding, as their mouth muscles cannot maintain a proper suck-swallow pattern or a good breastfeeding latch (hypotonia is common in children with Down’s syndrome).
Head
Size
Measure the infant’s head circumference and record it in the notes.
Head size abnormalities
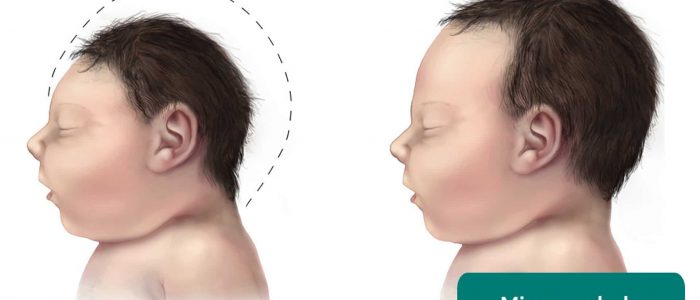
Microcephaly describes a head that is smaller than expected for age and sex. Microcephaly may be associated with reduced brain size or atrophy.
Macrocephaly describes a head that is larger than expected for age and sex. Macrocephaly may be normal but may also be associated with hydrocephalus, cranial vault abnormalities or genetic abnormalities.
Shape
Inspect the shape of the head and note any abnormalities.
Inspect the cranial sutures and note if they are closely applied, widely separated or normal.
Head shape abnormalities
Cranial moulding is common after birth and resolves within a few days.
Caput succedaneum is a diffuse subcutaneous fluid collection with poorly defined margins (often crossing suture lines) caused by pressure on the presenting part of the head during delivery. It does not usually cause complications and resolves over the first few days. 4
Cephalhaematoma is a subperiosteal haemorrhage which occurs in 1-2% of infants and may increase in size after birth. The haemorrhage is bound by the periosteum, therefore, the swelling does not cross suture lines (in contrast to a caput succedaneum). Cephalhaematoma is more common with instrumental delivery and may cause jaundice, therefore, bilirubin should be monitored.
Subgaleal haemorrhages occur between the aponeurosis of the scalp and periosteum and form a large, fluctuant collection which crosses sutures lines. They are rare but may cause life-threatening blood loss.
Craniosynostosis is a condition in which one or more of the fibrous sutures in an infant skull prematurely fuses, changing the growth pattern of the skull which can result in raised intracranial pressure and damage to intracranial structures. Surgical intervention is required with the primary goal being to allow normal cranial vault development to occur. This can be achieved by excision of the prematurely fused suture and correction of the associated skull deformities. 7
Fontanelle
Palpate the anterior fontanelle: note if it feels flat (normal), sunken or bulging (abnormal).
Fontanelle abnormalities
A tense bulging fontanelle may suggest raised intracranial pressure (e.g. hydrocephalus).
A sunken fontanelle may suggest dehydration.
Skin
It is very important to document any birthmarks or bruising/lacerations from birth trauma found on initial examination in case there are any child protection concerns in the future. There are body maps in the red book to help with this.
Colour: inspect the colour of the skin and note any pallor, cyanosis, erythema or jaundice.
Bruising/lacerations: note the location and size of any bruises or lacerations which may have been sustained during childbirth.
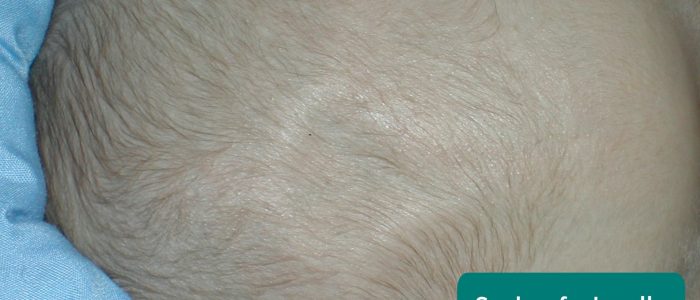
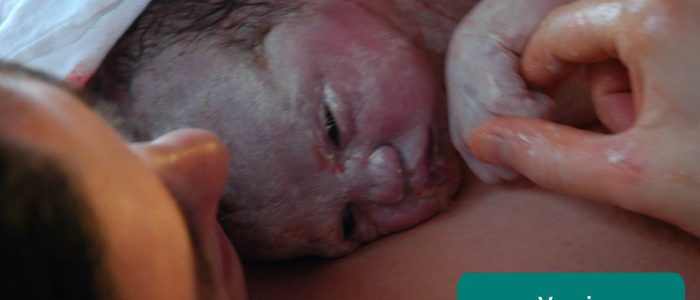
Vernix: a waxy or cheese-like white substance found coating the skin of newborn babies (this is a normal finding).
Examples of facial birthmarks
Examples of facial birthmarks include:
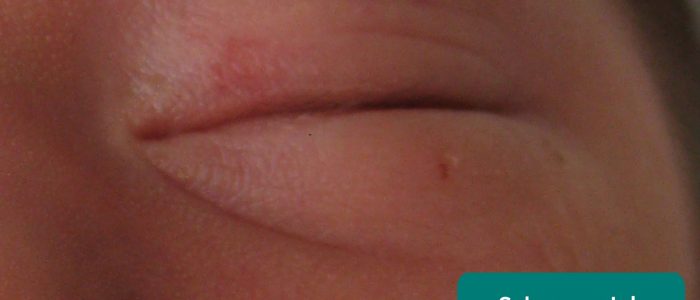
- Salmon patch (also known as a stork mark or nevus simplex): red or pink patches, often on an infant’s eyelids, head or neck caused by congenital capillary malformation. Salmon patches are very common and usually fade by the age of two.
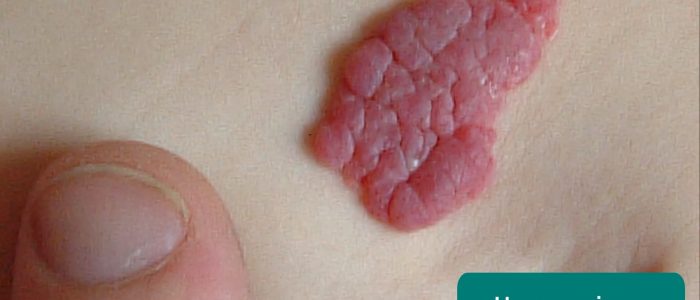
- Haemangiomas (also known as strawberry marks): blood vessels which form a raised red lump on the skin which appears soon after birth. Haemangiomas typically get bigger over the first 6-12 months and then shrink and disappear by the age of 7. They may require treatment if they affect vision, breathing or feeding.
- Port-wine stain (also known as naevus flammeus): red/purple marks on the face and neck which are typically present from birth and do not regress. Port-wine stains can sometimes be associated with Sturge-Weber syndrome and Klippel-Trenaunay syndrome.
Other potential findings
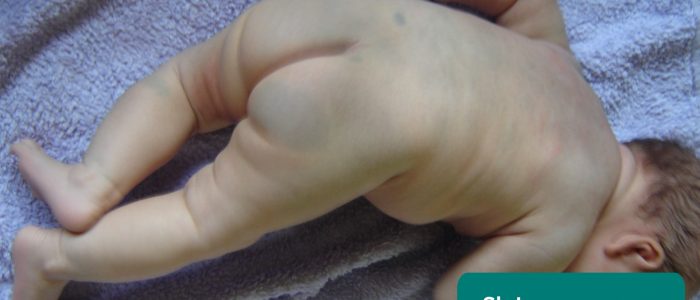
Slate-grey nevus is a benign, flat, congenital birthmark with wavy borders and irregular shape, usually located over the sacrum. It is most commonly blue in colour and can be mistaken for a bruise. They normally disappear within 3-5 years after birth. 5
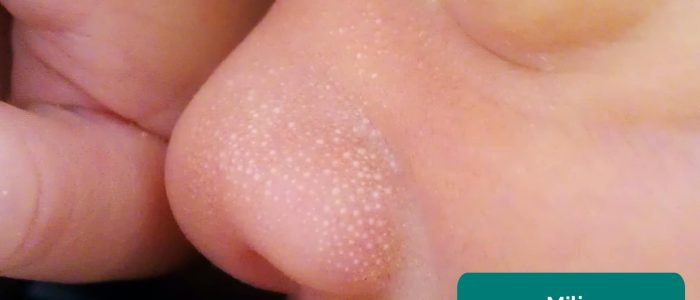
Milia are tiny white cysts containing keratin and sebaceous material. They are very common on the face and most resolve within the first few weeks of life.
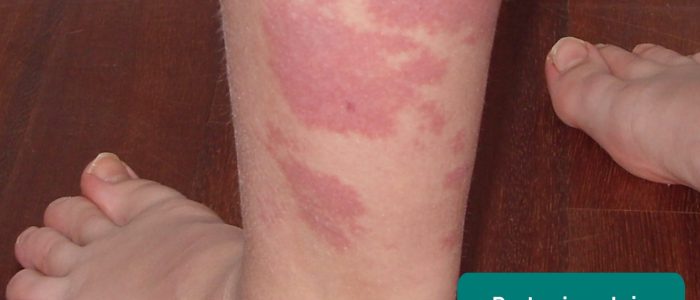
Erythema toxicum is a very common and benign condition seen in newborn infants. It presents with various combinations of erythematous macules, papules, and pustules. Lesions usually appear from 48 hours of age and resolve spontaneously.
Neonatal jaundice can be physiological, appearing at 2-3 days and resolving by day 10. It can also be caused by a wide range of different pathologies including haemolytic disease, infection and Gilbert’s syndrome.
Face
Appearance: note any dysmorphic features of the face (e.g. epicanthic folds in Down’s syndrome).
Asymmetry: note any asymmetry of the face (e.g. facial nerve palsy secondary to instrumental delivery).
Trauma: note any evidence of facial trauma (e.g. bruising, lacerations) likely to have occurred during labour (e.g. instrumental delivery).
Nose: inspect to assess the patency of the nasal passages (infants are obligate nasal breathers and therefore will present with respiratory distress and cyanosis at rest if they have bilateral choanal atresia).
Eyes
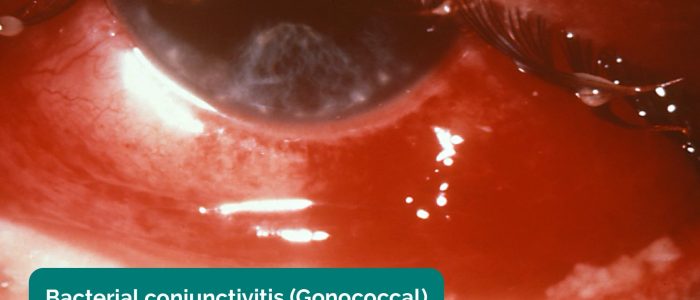
Inspect the eyes for evidence of erythema or discharge (e.g. conjunctivitis).
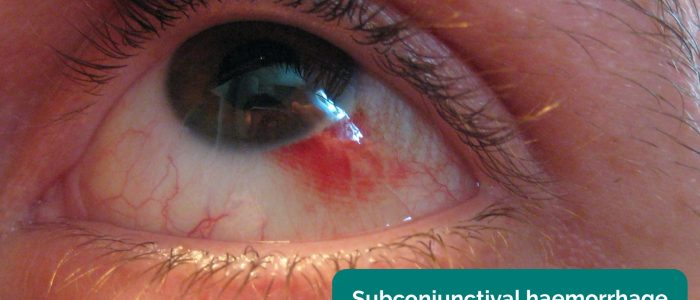
Inspect the sclera by gently retracting the lower eyelid noting any discolouration (e.g. jaundice, subconjunctival haemorrhages). Subconjunctival haemorrhages often look dramatic but are fairly common after delivery and benign, you should, however, document their presence.
Inspect the position and shape of the eyes: look for evidence of ptosis or the presence of epicanthic folds (e.g. Down’s syndrome).
Fundal reflex
Correct terminology
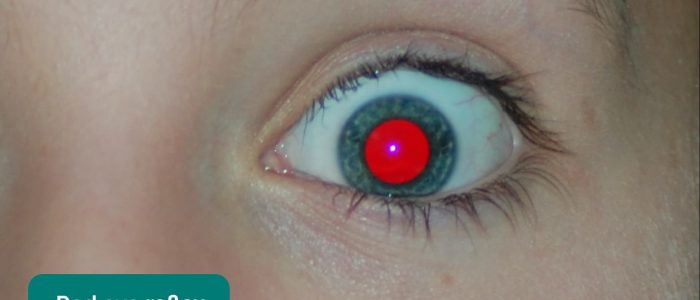
The term fundal reflex is preferred over red reflex as the colour of the healthy reflex varies depending on a patient’s skin colour.
In patient’s with lighter skin, the reflex typically appears orange-red in colour, whereas in those with darker skin, the reflex can be yellow-white or even blue in colour.
Assess for the fundal reflex in each eye:
1. Look through the ophthalmoscope, shining the light towards the patient’s eye at a distance of approximately one arm’s length.
2. Observe for a reddish/orange reflection in each pupil, caused by light reflecting back from the vascularised retina.
Causes of an absent fundal reflex
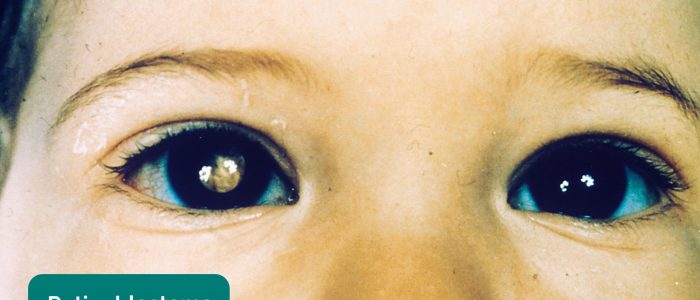
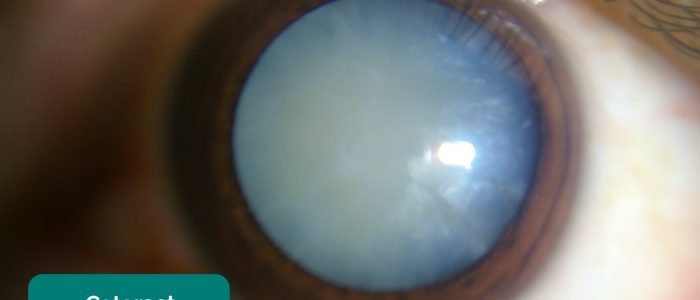
Absence of the fundal reflex in children can be due to congenital cataracts, retinal detachment, vitreous haemorrhage and retinoblastoma.
An absent fundal reflex or the presence of a white reflex requires immediate ophthalmology referral.
Ears
Inspect the pinna: note any asymmetry, skin tags, pits or the presence of accessory auricles.
All infants should undergo a hearing screening test prior to being discharged from hospital.
Mouth and palate
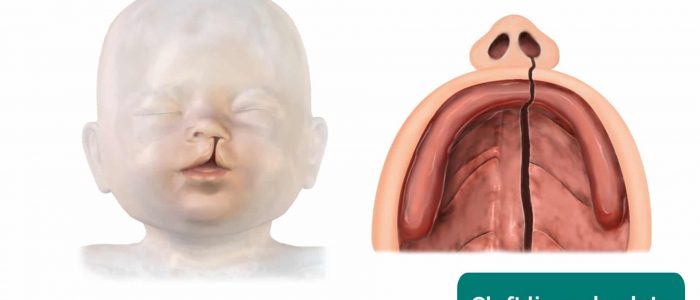
Look for clefts of the hard or soft palate: the full palate should be examined by visual inspection. You will need to use a tongue depressor and a torch, and ask a parent to help keep the baby’s head still. You must visualise the whole palate, and see the central uvula to ensure it is intact. You cannot rely on palpation to exclude a cleft.
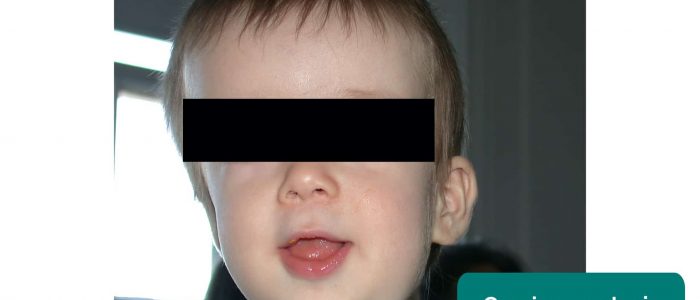
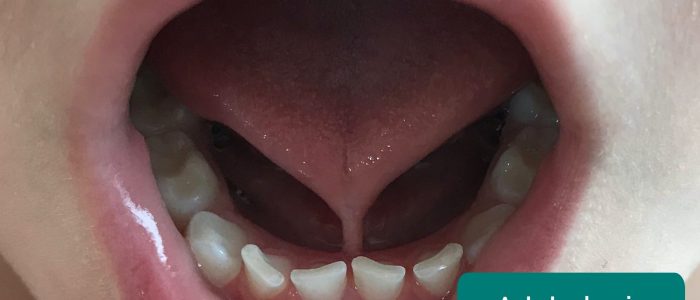
Inspect the tongue and gums: look for evidence of tongue-tie (ankyloglossia).
Neck and clavicles
Inspect the length of the neck and note any abnormalities such as webbing: a shortened webbed neck is typically associated with Turner’s syndrome.
Inspect for neck lumps: a lump in the left posterior triangle of the neck may represent a cystic hygroma.
Look for evidence of a clavicular fracture: signs may include bruising, discontinuity of the clavicle and an abnormal position of the arm (fractures most commonly occur in the context of shoulder dystocia).
Cystic hygroma
A cystic hygroma is a congenital lymphatic lesion which is typically identified prenatally or at birth. A cystic hygroma can arise anywhere but typically develops in the left posterior triangle of the neck. Cystic hygromas are benign but can be disfiguring and typically require surgical treatment including drainage and use of sclerosing agents to prevent reaccumulation of lymphatic fluid.
Upper limbs
Assess the symmetry of the upper limbs: they should appear equal in size and length.
Inspect the fingers: count the fingers and note any abnormal morphology (e.g. polydactyly).
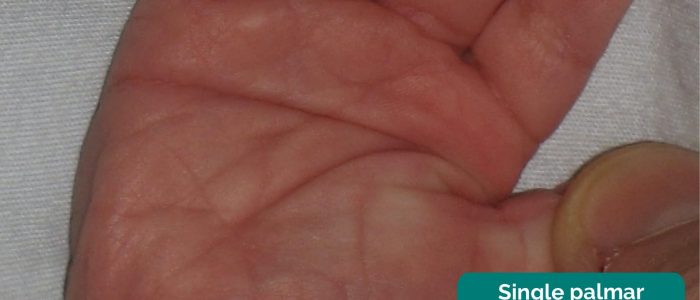
Inspect the palms: check if the child has two palmar creases (normal).
Palpate the brachial pulse on each upper limb: note any asymmetry suggestive of an underlying vascular abnormality (e.g. coarctation of the aorta).
Abnormalities of the hand
Polydactyly is a congenital abnormality where there are supernumerary fingers or toes.
A single palmar crease is associated with Down’s syndrome.
Chest
Inspection
Observe the chest, paying particular attention to the respiratory rate and work of breathing.
Respiratory rate
Count the respiratory rate whilst observing the child. The normal respiratory rate of a newborn is 40-60 breaths per minute.
Work of breathing
Assess for signs of increased work of breathing:
- Difficulty feeding
- Expiratory grunting
- Tracheal tug
- Supraclavicular recession
- Intercostal recession
- Subcostal recession
- Nasal flaring
- Abdominal breathing
- Head bobbing (secondary to sternocleidomastoid contractions)
Other clinical signs
Inspect the chest for other relevant clinical signs:
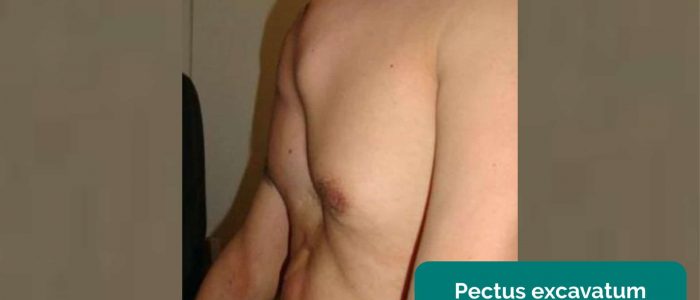
- Pectus excavatum: a caved-in or sunken appearance of the chest.
- Pectus carinatum: protrusion of the sternum and ribs.
- Asymmetrical chest wall expansion: asymmetry may be noted unilateral lung pathology (e.g. pneumonia).
Auscultation
Lungs
Auscultate each side of the chest in a symmetrical pattern, comparing side to side:
- Pay attention to the inspiratory and expiratory sounds at each placement.
- Note the quality and volume of the breath sounds.
- Note any additional sounds (e.g. wheeze, coarse crackles).
- Repeat auscultation on the posterior aspect of the chest.
Heart
Auscultate ‘upwards’ through the valve areas using the diaphragm of a paediatric stethoscope:
- Mitral valve: 5th intercostal space – midclavicular line (apex beat)
- Tricuspid valve: 4th or 5th intercostal space – lower left sternal edge
- Pulmonary valve: 2nd intercostal space – left sternal edge
- Aortic valve: 2nd intercostal space – right sternal edge
Listen over each area with both the bell (for low pitched sounds – gallops and split S2) and the diaphragm (high pitched sounds – pericardial rubs, S1/S2 and most murmurs).
The normal heart rate of a newborn is approximately 120-150 bpm.
If a murmur is noted, try to determine where it is heard loudest and if it radiates anywhere.
Pulse oximetry
Some centres recommend checking preductal and postductal oxygen saturations to improve detection of critical congenital heart disease in newborn infants. Both readings should both be ≥95% and within 3% of each other.
Abdomen
Inspection
Inspect for evidence of abdominal distension: causes include bowel obstruction, organomegaly and ascites.
Inspect the umbilicus: note any swelling (e.g. umbilical hernia) or erythema and discharge (e.g. umbilical cord stump infection).
Inspect for evidence of an inguinal hernia in the groin: if present, arrange a paediatric surgical review.
Palpation
Palpate the abdomen to assess for organomegaly:
- Liver: should be palpable no more than 2cm below the costal margin (if palpable lower in the abdomen consider hepatomegaly).
- Spleen: may be palpable at the left costal margin in healthy infants (if easily palpable, consider splenomegaly).
- Kidneys: normally only palpable using deep bimanual palpation (if easily palpable consider polycystic kidney disease).
- Bladder: should not be palpable in healthy infants (if easily palpable, considering urinary tract obstruction).
Genitalia
Note any ambiguity of genitalia: typically associated with congenital adrenal hyperplasia (CAH) in girls (boys with CAH have normal genitalia).
Males
Assessment of male genitalia:
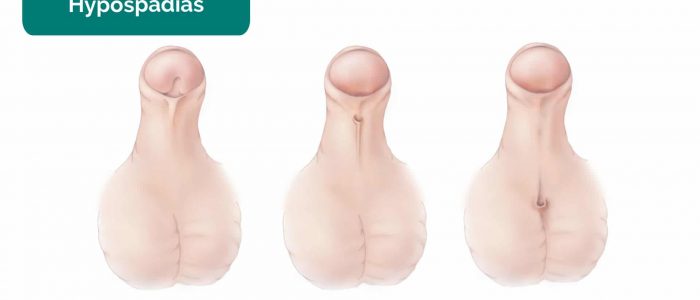
- Note the position of the urethral meatus: an abnormal position may be noted in hypospadias or epispadias.
- Note the size of the penis: it should be at least 2cm.
- Assess for evidence of testicular swelling indicative of hydrocele: a collection of fluid around the testicle (the swelling will transilluminate when a light source is placed nearby).
- Palpate the scrotum to ensure both testes are present: a unilateral undescended testis is common and should be followed up over time; bilateral absence is considered a disorder of sexual development and should be investigated.
Females
Assessment of female genitalia:
- Inspect the labia: to check they are not fused.
- Inspect the clitoris: to ensure it is a normal size.
- Note any vaginal discharge: white discharge is a normal finding, caused by exposure to maternal oestrogens.
Lower limbs
Inspect the lower limbs for abnormalities:
- Asymmetry: the lower limbs should appear equal in size and length.
- Oedema: may indicate hypoalbuminaemia or congestive cardiac failure.
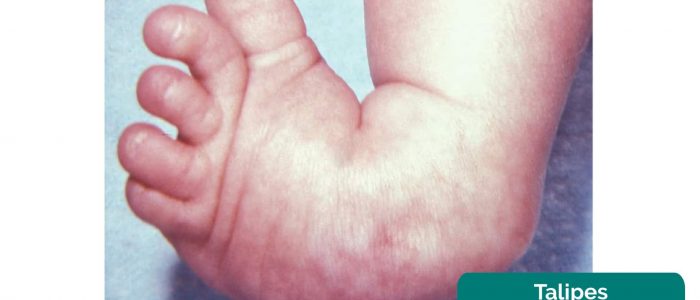
- Ankle deformities: talipes (club foot) is a common ankle deformity causing the foot to be turned inward.
- Missing digits: ensure the correct number of digits are present on each foot.
Assess tone in both lower limbs: tone is typically decreased in infants with Down’s syndrome and may be asymmetrically increased secondary to upper motor neuron lesions (e.g. ischaemic stroke, intracranial haemorrhage).
Assess movement in both lower limbs: note any weakness which may indicate an upper or lower motor neuron lesion or joint pathology.
Assess the range of knee joint movement: typically excessive in hypermobility.
Palpate and compare femoral pulses: this can be difficult, particularly in an active baby, and requires practice. Weak, absent or delayed femoral pulses are a sign of coarctation of the aorta.
Hips
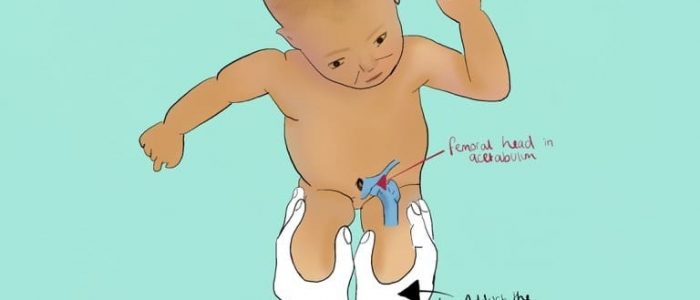
Both Barlow’s and Ortolani’s tests are carried out as part of the routine newborn examination to detect hip joint instability and dislocation. Each hip should be examined individually with all clothing, including the nappy, removed.
Barlow’s test
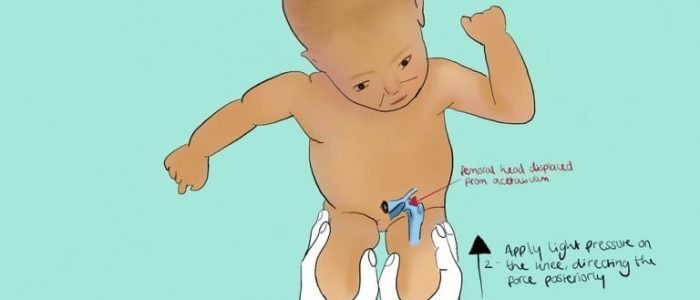
Barlow’s test is performed by adducting the hip (bringing the thigh towards the midline) whilst applying light pressure on the knee with your thumb, directing the force posteriorly. 6
If the hip is unstable, the femoral head will slip over the posterior rim of the acetabulum, producing a palpable sensation of subluxation or dislocation.
If the hip is dislocatable the test is considered positive. The Ortolani manoeuvre is then used to confirm the positive finding (i.e. that the hip actually dislocated).
Ortolani’s test
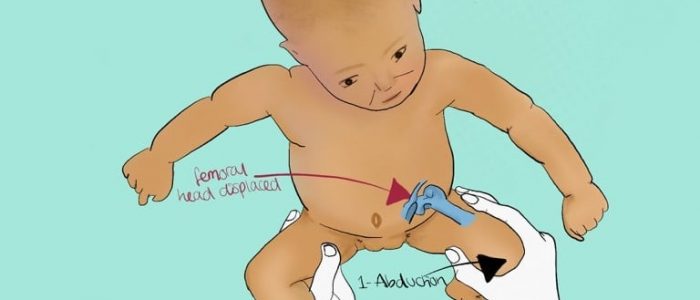
Ortolani’s test is used to confirm posterior dislocation of the hip joint. 7
1. Flex the hips and knees of a supine infant to 90°.
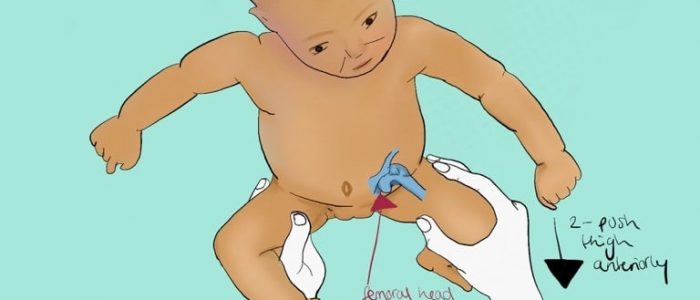
2. With your index fingers placing anterior pressure on the greater trochanters, gently and smoothly abduct the infant’s legs using your thumbs.
A positive sign is a distinctive ‘clunk’ which can be heard and felt as the femoral head relocates anteriorly into the acetabulum.
Back and spine
Inspect the spine for:
- Scoliosis
- Hair tufts
- Naevi
- Birthmarks
- Sacral pits
Hair tufts and sacral pits can be associated with underlying neural tube defects (e.g. spina bifida).
Anus
Inspect the anus for patency: abnormal embryological development of the rectum can result in an imperforate anus.
Meconium should be passed within 24 hours: a delay is suggestive of obstruction or Hirschsprung’s disease.
Reflexes
Assess the newborn’s reflexes
Assess a selection of the following reflexes which should all be present in a healthy newborn. The absence of several reflexes may indicate an underlying neurological abnormality.
Palmar grasp reflex
When an object is placed in the infant’s hand and strokes their palm, the fingers will close and they will grasp it with a palmar grasp.8
Sucking reflex
Causes the child to instinctively suck anything that touches the roof of their mouth, absence of this reflex is most apparent during feeding.
Rooting reflex
Present at birth and disappears around four months of age, as it gradually comes under voluntary control. A newborn infant will turn its head toward anything that strokes its cheek or mouth to aid breastfeeding. 9
Stepping reflex
When the soles of the infant’s feet touch a flat surface they will appear to walk by placing one foot in front of the other.10
Moro reflex
Support the infant’s upper back with one hand, then drop back once or twice into your other hand. A normal Moro reflex involves the extension of the legs and head whilst the arms jerk upwards with the fingers extended. The arms are then brought together and the hands clench into fists, and the infant cries. Asymmetry may be due to hemiparesis, brachial plexus injury or a fractured clavicle.
To complete the examination…
Explain to the parents that the examination is now finished and offer to dress the baby.
Share the results of the assessment with the parents, explaining the reason for any referrals you feel are required.
Check if the parents have any further questions.
Thank the parents for their time.
Dispose of PPE appropriately and wash your hands.
Summarise your findings
Document your findings and the need for further investigations/referrals: in the UK the NIPE is documented using a national online system (which you would print and place in the baby’s notes).
Reviewer
Dr Rebecca Naples
Paediatric Registrar
Illustrator
Aisha Ali
Medical student and illustrator
References
Text references
- Newborn and Infant Physical Examination Screening Programme Handbook 2016/17. Public Health England. Published April 2016. Retrieved 15 March 2017.
- Newborn Infant Physical Examination. Nottingham Neonatal Service – Clinical Guidelines. Published November 2015. Retrieved 15 March 2017.
- Jaundice in newborn babies under 28 days. NICE guidance. Published May 2010. Retrieved 15 October 2017. Available from: [LINK].
- Slater BJ, Lenton KA, Kwan MD, Gupta DM, Wan DC, Longaker MT (April 2008). “Cranial sutures: a brief review”. Plast. Reconstr. Surg. 121 (4): 170e–8e. doi:10.1097/01.prs.0000304441.99483.97. PMID 18349596.
- Circumscribed dermal melanosis (Mongolian spot) (1981) Kikuchi I, Inoue S. in “Biology and Diseases of Dermal Pigmentation”, University of Tokyo Press, p83
- French LM, Dietz FR (July 1999). “Screening for developmental dysplasia of the hip”. American Family Physician. 60 (1): 177–84, 187–8. PMID 10414637.
- Storer SK, Skaggs DL (October 2006). “Developmental dysplasia of the hip”. American Family Physician. 74 (8): 1310–6. PMID 17087424.
- Jakobovits, AA (2009). “Grasping activity in utero: a significant indicator of fetal behaviour (the role of the grasping reflex in fetal ethology).”. Journal of perinatal medicine. 37 (5): 571–2. doi:10.1515/JPM.2009.094. PMID 19492927.
- Odent M. The early expression of the rooting reflex. Proceedings of the 5th International Congress of Psychosomatic Obstetrics and Gynaecology, Rome 1977. London: Academic Press, 1977: 1117-19.
- Siegler, R.; Deloache, J.; Eisenberg, N. (2006). How Children Develop. New York: Worth Publishers. p. 188. ISBN 978-0-7167-9527-8.
Image references
- Cornelia Csuk. Adapted by Geeky Medics. Cyanosis. Licence: CC BY-SA.
- Brar_j- Flickr. Adapted by Geeky Medics. Microcephaly. Licence: CC BY.
- Michael L. Kaufman. Adapted by Geeky Medics. Craniosynostosis. Licence: CC BY-SA.
- Johann Dréo. Adapted by Geeky Medics. Sunken fontanelle. Licence: CC BY-SA.
- Tonicthebrown. Adapted by Geeky Medics. Salmon patch. Licence: CC BY-SA.
- Dr. Wonko. Adapted by Geeky Medics. Port-wine stain. Licence: CC BY-SA.
- Tom & Katrien. Adapted by Geeky Medics. Vernix. Licence: CC BY-SA.
- GeoWombats. Adapted by Geeky Medics. Slate-grey nevus. Licence: CC BY-SA.
- FiP. Adapted by Geeky Medics. Subconjunctival haemorrhage. Licence: CC BY-SA.
- Imrankabirhossain. Adapted by Geeky Medics. Cataract. Licence: CC BY-SA.
- Klaus D. Peter, Gummersbach, Germany. Adapted by Geeky Medics. Accessory auricle. Licence: CC BY 3.0 DE.
- BruceBlaus. Adapted by Geeky Medics. Cleft palate. Licence: CC BY-SA.
- Gzzz. Adapted by Geeky Medics. Ankyloglossia. Licence: CC BY-SA.
- Vardhan Kothapalli. Adapted by Geeky Medics. Cystic hygroma. Licence: CC BY-SA.
- Bobjgalindo. Adapted by Geeky Medics. Polydactyly. Licence: CC BY-SA.
- Aurora Bakalli, Tefik Bekteshi, Merita Basha, Afrim Gashi, Afërdita Bakalli and Petrit Ademaj. Adapted by Geeky Medics. Pectus excavatum. Licence: CC BY-SA.
- Jprealini. Adapted by Geeky Medics. Pectus carinatum. Licence: CC BY-SA.
- OpenStax College. Adapted by Geeky Medics. Talipes. Licence: CC BY.