- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Obstetric abdominal examination frequently appears in OSCEs and you’ll be expected to pick up the relevant clinical signs using your examination skills. This obstetric abdominal examination OSCE guide provides a clear step-by-step approach to examining the pregnant abdomen, with an included video demonstration.
Gather equipment
Gather relevant equipment including:
- Measuring tape
- Pinard stethoscope
Introduction
Wash your hands and don PPE if appropriate.
Introduce yourself to the patient including your name and role.
Confirm the patient’s name and date of birth.
Briefly explain what the examination will involve using patient-friendly language: “Today I need to examine your tummy as part of the assessment of your pregnancy. This will involve me looking and feeling the tummy, in addition to performing some measurements. Although it may be a little uncomfortable, it shouldn’t be painful. If at any point you’d like me to stop then please just let me know.”
Offer a chaperone.
Gain consent to proceed with the examination: “Do you understand everything I’ve said? Are you happy for me to carry out the examination?”
Position the patient on the clinical examination couch with the head of the bed at a 30-45° angle for the initial assessment.
Adequately expose the patient’s abdomen for the examination from the pubic symphysis to the xiphisternum (offer a blanket to allow exposure only when required).
Provide the patient with the opportunity to pass urine before the examination.
Ask the patient if they have any pain before proceeding with the clinical examination.
General inspection
Clinical signs
Inspect the patient from the end of the bed whilst at rest, looking for clinical signs suggestive of underlying pathology:
- Pain: if the patient appears uncomfortable, ask where the pain is and whether they are still happy for you to examine them.
- Obvious scars: may provide clues regarding previous abdominal surgery (e.g. caesarian section).
- Pallor: a pale colour of the skin that can suggest underlying anaemia. It should be noted that healthy individuals may have a pale complexion that mimics pallor.
- Jaundice: a yellowish or greenish pigmentation of the skin and whites of the eyes due to high bilirubin levels (e.g. obstetric cholestasis).
- Oedema: a small amount of oedema is normal in the later stages of pregnancy however if there is widespread oedema affecting the arms, legs and face consider the possibility of pre-eclampsia.
Objects and equipment
Look for objects or equipment on or around the patient that may provide useful insights into their medical history and current clinical status:
- Mobility aids: items such as wheelchairs and walking aids give an indication of the patient’s current mobility status.
- Vital signs: charts on which vital signs are recorded will give an indication of the patient’s current clinical status and how their physiological parameters have changed over time (e.g. blood pressure).
- Fluid balance: fluid balance charts will give an indication of the patient’s current fluid status which may be relevant if a patient appears fluid overloaded or dehydrated.
- Prescriptions: prescribing charts or personal prescriptions can provide useful information about the patient’s recent medications.
Obstetric cholestasis
Obstetric cholestasis is a multifactorial condition that is characterised by abnormal liver function tests, jaundice and intense pruritis (typically affecting the palms and soles of the feet). The disease usually presents in the third trimester and is associated with an increased risk of intrauterine death and premature delivery.
Hands
The hands can provide lots of clinically relevant information and therefore a focused, structured assessment is essential.
Inspect the hands for relevant clinical signs:
- Colour: pale hands suggest poor peripheral perfusion (e.g. hypovolaemic shock, aortocaval compression) and cyanosis may suggest underlying hypoxaemia.
- Peripheral oedema: may be a normal finding in late pregnancy, but if widespread consider pre-eclampsia. If pre-eclampsia is suspected, you should check the patient’s blood pressure and perform urinalysis (looking for proteinuria).
- Palmar erythema: a redness involving the heel of the palm that is a normal finding in pregnancy.
Temperature
Place the dorsal aspect of your hand onto the patient’s to assess temperature:
- In healthy individuals, the hands should be symmetrically warm, suggesting adequate perfusion.
- Cool hands may suggest poor peripheral perfusion (e.g. hypovolaemic shock, aortocaval compression).
Capillary refill time (CRT)
Measuring capillary refill time (CRT) in the hands is a useful way of assessing peripheral perfusion:
- Apply five seconds of pressure to the distal phalanx of one of a patient’s fingers and then release.
- In healthy individuals, the initial pallor of the area you compressed should return to its normal colour in less than two seconds.
- A CRT that is greater than two seconds suggests poor peripheral perfusion (e.g. antepartum haemorrhage, aortocaval compression) and the need to assess central capillary refill time.
Radial pulse
Palpate the patient’s radial pulse, located at the radial side of the wrist, with the tips of your index and middle fingers aligned longitudinally over the course of the artery.
Once you have located the radial pulse, assess the rate and rhythm.
Heart rate
Assessing heart rate:
- You can calculate the heart rate in a number of ways, including measuring for 60 seconds, measuring for 30 seconds and multiplying by 2 or measuring for 15 seconds and multiplying by 4.
- For irregular rhythms, you should measure the pulse for a full 60 seconds to improve accuracy.
- Women typically have a higher baseline heart rate during pregnancy (80-90 beats per minute).
Face
Inspect the patient’s face for relevant clinical signs:
- Jaundice: most evident in the superior portion of the sclera (ask the patient to look downwards as you lift their upper eyelid). In the context of an obstetric abdominal examination, it is most likely secondary to obstetric cholestasis.
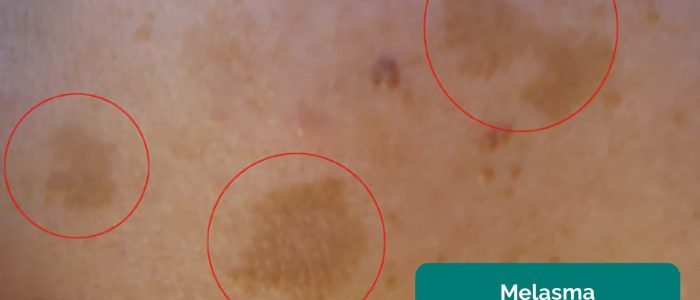
- Melasma: benign dark and irregular hyperpigmented macules which are normal in pregnancy.
- Oedema: may be a normal finding in late pregnancy, but if widespread consider pre-eclampsia.
- Conjunctival pallor: ask the patient to gently pull down their lower eyelid to allow you to inspect the conjunctiva for pallor. Conjunctival pallor is associated with anaemia.
Abdominal inspection
Position the patient
The recommended positioning for a patient during pregnancy varies, depending on the current gestation:
- Early pregnancy: position the patient supine on the couch, with the head end of the bed elevated to 15-30°.
- Late pregnancy: position the patient in the left lateral position (tilted 15° to the horizontal level) to avoid compression of the abdominal aorta and inferior vena cava by the gravid uterus (known as aortocaval compression).
Closely inspect the abdomen
Expose the abdomen appropriately, from the xiphisternum to the pubic symphysis and inspect for relevant clinical signs:
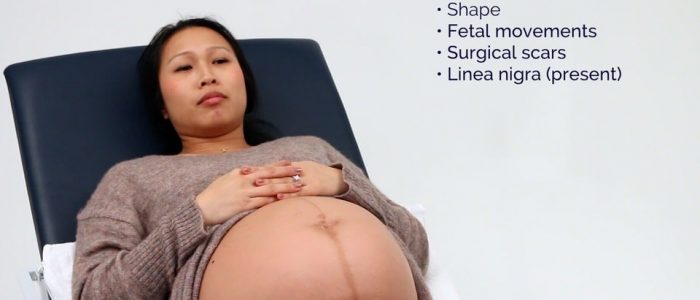
- Abdominal shape: this may give an initial indication of the fetal lie.
- Fetal movements: these are typically visible from 24 weeks gestation.
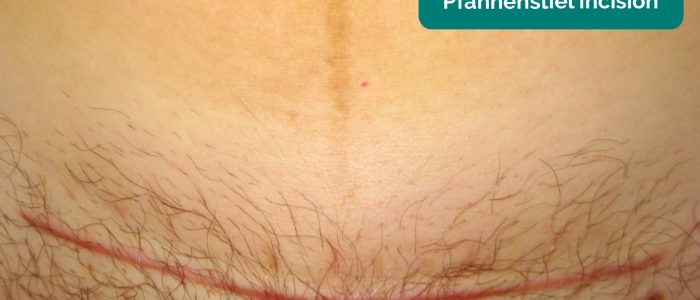
- Surgical scars: may provide clues regarding previous abdominal surgery (e.g. caesarian section).
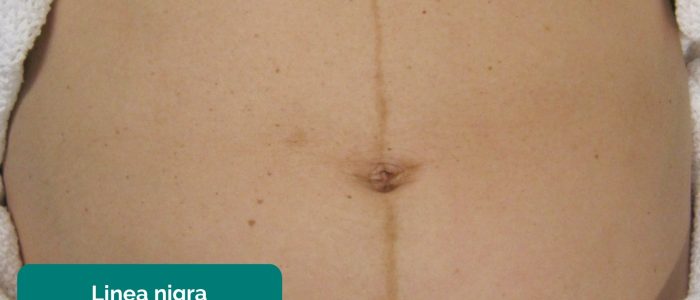
- Linea nigra: a dark line running vertically down the middle of the abdomen (a normal finding in pregnancy).
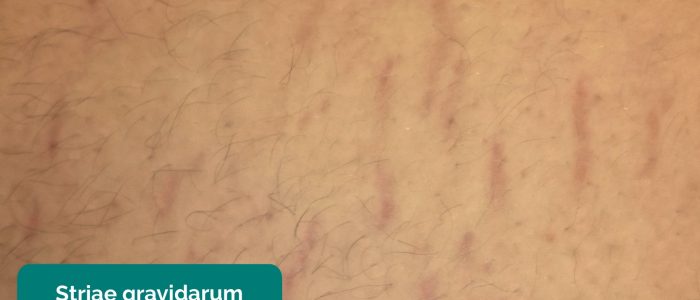
- Striae gravidarum: reddish or purple lesions that develop due to overstretching of the abdominal skin as the gravid uterus expands (commonly referred to as stretch marks).
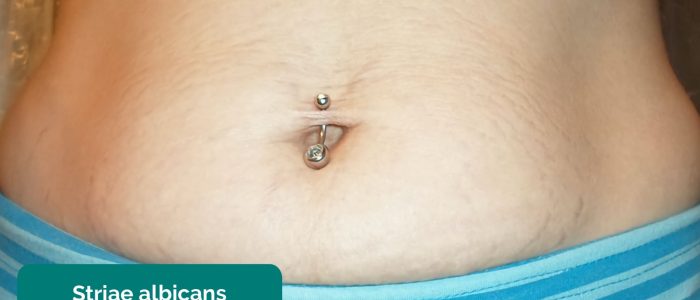
- Striae albicans: mature stretch marks which appear silver-like in colour and are less pronounced.
Aortocaval compression syndrome
Aortocaval compression syndrome occurs due to compression of the abdominal aorta and inferior vena cava by the gravid uterus when a pregnant woman is supine. Aortocaval compression can result in maternal hypotension, loss of consciousness and in rare cases fetal demise. Women in late pregnancy are positioned in the left lateral position when supine to reduce pressure on the aorta and inferior vena cava.
Abdominal palpation
Ask about abdominal tenderness before palpating the abdomen and continue to monitor the patient’s face for signs of discomfort throughout the examination.
Palpate the abdomen
Briefly perform light palpation over each of the nine regions of the abdomen to identify any tenderness or masses that may not relate to the pregnancy (e.g. appendicitis). See the abdominal examination guide for more details.
Palpate the uterus
Palpate the uterus to identify its borders, including the upper and lateral edges.
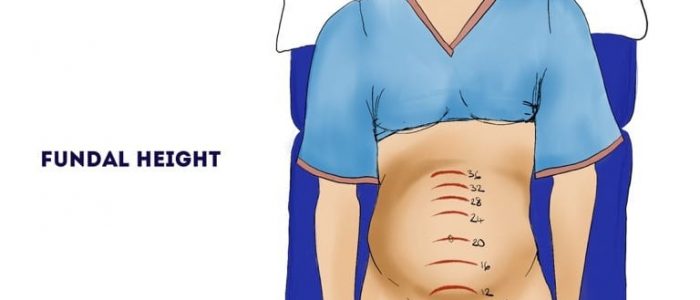
The uterine fundus can be found at different locations during pregnancy, depending on the patient’s current gestation:
- 12 weeks gestation: pubic symphysis
- 20 weeks gestation: umbilicus
- 36 weeks gestation: the xiphoid process of the sternum
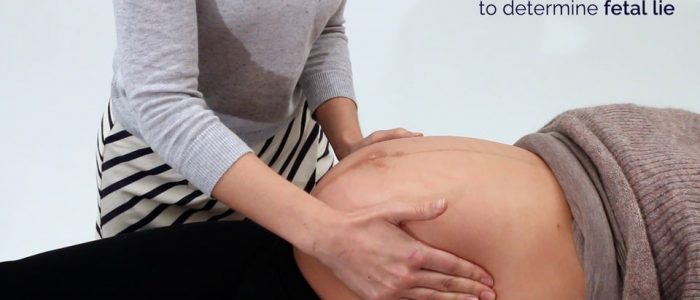
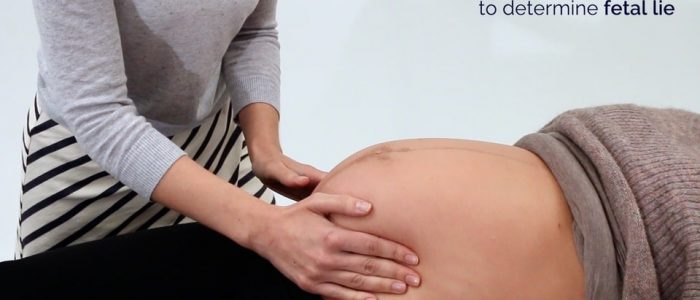
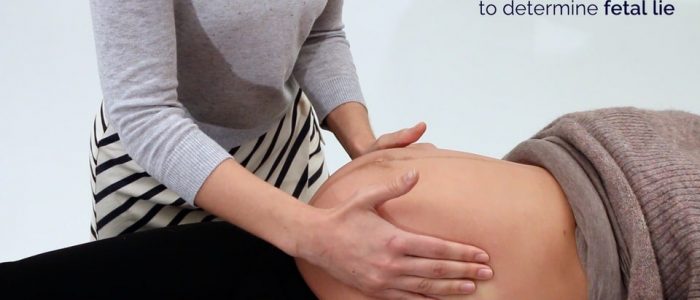
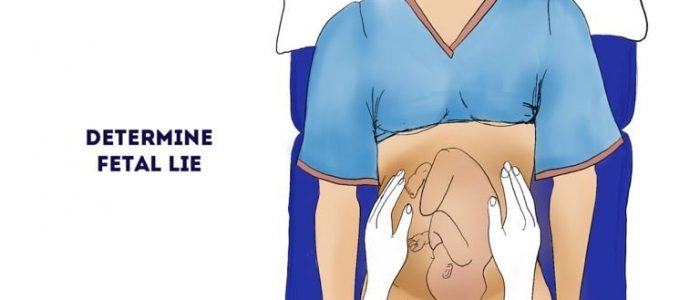
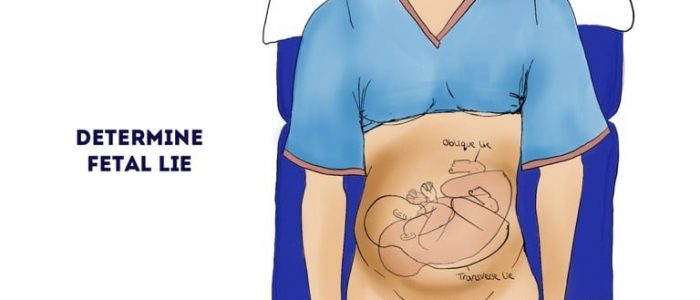
Fetal lie
Fetal lie refers to the relationship between the long axis of the fetus with respect to the long axis of the mother.
Assess the gravid uterus to determine the fetal lie:
1. Place your hands on either side of the patient’s uterus (ensuring you are facing the patient).
2. Gently palpate each side of the uterus:
- One side of the uterus should feel full in nature (due to the presence of the fetal back).
- On the other side of the uterus, you may be able to feel the fetus’s limbs.
Types of fetal lie
There are three main types of fetal lie which include:
- Longitudinal lie: the head and buttocks are palpable at each end of the uterus.
- Oblique lie: the head and buttocks are palpable in one of the iliac fossae.
- Transverse lie: the fetus is lying directly across the uterus.
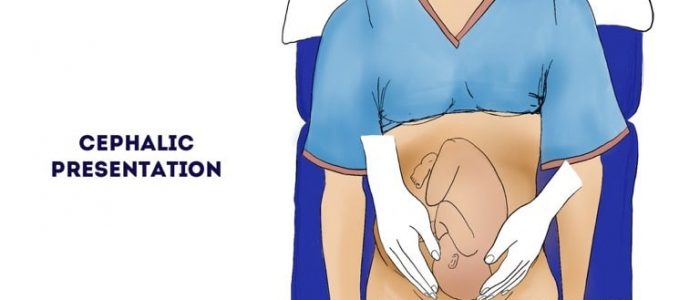
Fetal presentation
Fetal presentation refers to which anatomical part of the fetus is closest to the pelvic inlet.
Assess the gravid uterus to determine fetal presentation:
1. Ensure you are facing the patient to observe for signs of discomfort and warn the patient this may feel a little uncomfortable.
2. Place your hands either side of the lower pole of the uterus, just above the pubic symphysis.
3. Apply firm pressure to the uterus angled medially, palpating for the presenting part:
- A hard round presenting part is suggestive of a cephalic presentation (normal).
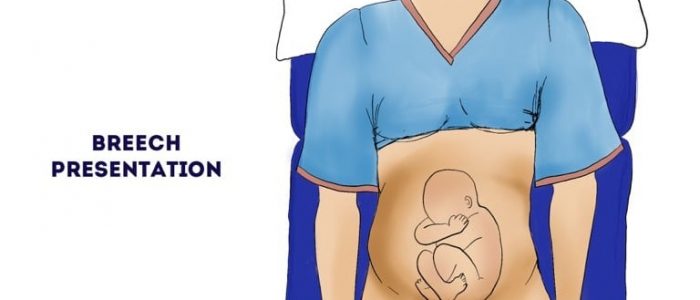
- A broader, softer, less defined presenting part (i.e. the fetal bottom or legs) is suggestive of a breech presentation (abnormal).
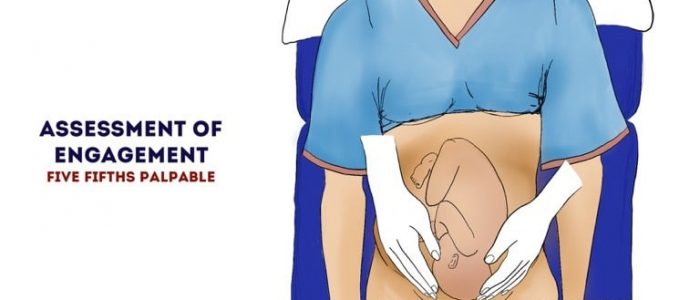
Fetal engagement
In late pregnancy, the level of fetal engagement should be assessed. A fetus is considered ‘engaged’ when more than 50% of the presenting part (usually the head) has descended into the pelvis.
The fetal head is divided into fifths when assessing engagement:
- If you are able to feel the entire head in the abdomen, it is five fifths palpable (i.e. not engaged).
- If you are not able to feel the head at all abdominally, it is zero fifths palpable (i.e. fully engaged).
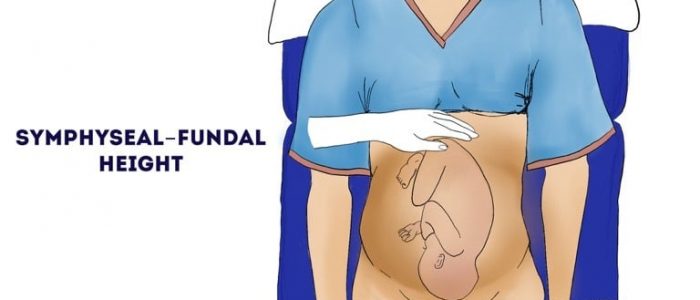
Symphyseal-fundal height
Symphyseal-fundal height is the distance between the fundus and the upper border of the pubic symphysis. After 20 weeks gestation, the symphyseal-fundal height should correlate with the gestational age of the fetus in weeks (+/- 2cm).
To measure the symphyseal-fundal height:
1. Begin palpation of the abdomen just inferior to the xiphisternum using the ulnar border of your left hand.
2. Locate the fundus of the uterus (a firm feeling edge at the upper border of the bump).
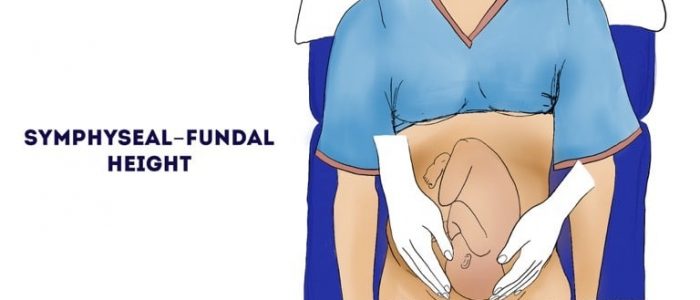
3. Once the fundus has been identified, locate the upper border of the pubic symphysis.
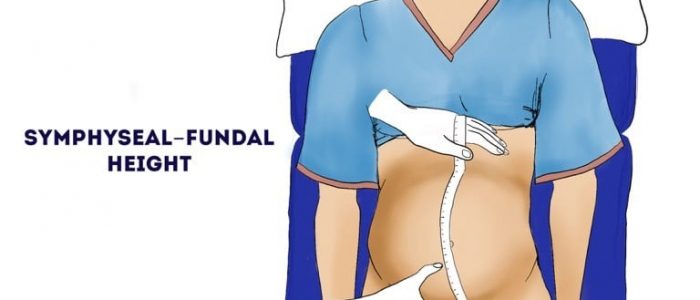
4. Measure the distance between the upper uterine border and the pubic symphysis in centimetres using a tape measure. The distance measured should correlate with the gestational age in weeks (+/- 2cm).
To avoid bias, it’s best to place the tape measure facing down and only turn to view the numbers once in position.
Fetal heartbeat
You may be asked to identify the fetal heartbeat using a Pinard stethoscope (or a Doppler ultrasound probe). As a result, it is important to have a basic understanding of how to locate and identify the fetal heartbeat.
1. Based on your assessment of the fetus’s position, you should place the Pinard stethoscope aiming between the fetal shoulders on the fetal back.
2. Palpate the patient’s radial pulse (i.e. maternal pulse).
3. Place your ear to the Pinard and take your hand away (so the Pinard is held against the abdomen using your ear only):
- You should be applying gentle pressure, to ensure a good seal between your ear and the Pinard, as well as between the Pinard and the abdomen.
- Pressing too hard will be uncomfortable for the patient and pressing too softly will make it difficult to hear anything at all.
4. Listen for the fetal heartbeat:
- If the maternal pulse coincides with the pulse you can hear, you are most likely listening to the flow through the uterine vessels, rather than the fetal heartbeat.
To complete the examination…
Explain to the patient that the examination is now finished.
Thank the patient for their time.
Dispose of PPE appropriately and wash your hands.
Summarise your findings.
Example summary
“Today I examined Mrs Smith, a 28-year-old female who is currently at 36 weeks gestation. On general inspection, the patient appeared comfortable at rest. There were no objects or medical equipment around the bed of relevance. There was no evidence of oedema of the face or peripheries on assessment.”
“Symphyseal-fundal height was 36cm, which is in keeping with the patient’s current gestation. The fetus was positioned in a longitudinal lie with a cephalic presentation. The fetal head was three fifths palpable.”
“In summary, these findings are consistent with a normal obstetric abdominal examination.”
“For completeness, I would like to perform the following further assessments and investigations.”
Further assessments and investigations
- Assessment of the fetal heartbeat: using a Pinard stethoscope or Doppler ultrasound.
- Blood pressure measurement: to assess for evidence of hypertension (e.g. pre-eclampsia).
- Urinalysis: to assess for evidence of proteinuria (pre-eclampsia) and urinary tract infection.
- Speculum examination: if there are concerns about vaginal bleeding or premature rupture of membranes.
- Weight and height measurement
- Ultrasound scan: to assess the position and wellbeing of the fetus.
Reviewers
Mr Isaac Magani
Consultant Obstetrician
Mr Gareth Waring
Senior Obstetric Registrar
Illustrator
Aisha Ali
Medical Student and Illustrator
References
- Elord. Adapted by Geeky Medics. Melasma. Licence: CC BY-SA.
- Azoreg. Adapted by Geeky Medics. Caesarian section scar. Licence: CC BY-SA-3.0.
- James Heilman, MD. Adapted by Geeky Medics. Linea nigra. Licence: CC BY-SA.
- FatM1ke. Adapted by Geeky Medics. Striae. Licence: CC BY-SA.
- ParentingPatch. Adapted by Geeky Medics. Striae albicans. Licence: CC BY-SA.