- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Introduction
Pigmented lesions of the oral cavity can be attributed to benign physiological changes, systemic diseases and malignancy.1
Lesions within the oral mucosa can be described as either being macular (flat) or papular (raised).
This article will focus on common causes of pigmented lesions found in the mouth and briefly discuss some rarer entities. Clinical appearance, diagnosis and management of pigmented oral lesions will also be discussed.
Aetiology
There are four main sources of pigment.
Melanin
Melanin is the most common source of pigmented lesions in the oral cavity. It is produced in the basal cells by melanocytes (or nevus cells) and is transferred via membrane-bound organelles called melanosomes.1
Whilst these are typically brown or black in appearance, they can also appear blue (as in ‘blue naevus’) due to the Tyndall effect.2
Melanin can be found in both benign and malignant lesions. An example of a benign lesion includes racial pigmentation, which presents intraorally as darker gingivae in Asian or Black individuals.
Haemosiderin
Haemosiderin is a breakdown product from red blood cells which gives rise to blue/black discolouration.
Chemical/foreign body
A variety of metals, such as lead, bismuth, mercury, silver and gold can cause pigmented lesions.3
These metals may leach directly into the mucosa from amalgam fillings or heavy metals from crowns on removal, resulting in an amalgam tattoo (figure 1). Amalgam tattoos can be identified on a radiograph, which typically reveals radiopaque fragments embedded within the mucosa.
No treatment is required for amalgam tattoos, however, clinical photography may be useful to monitor their appearance.4
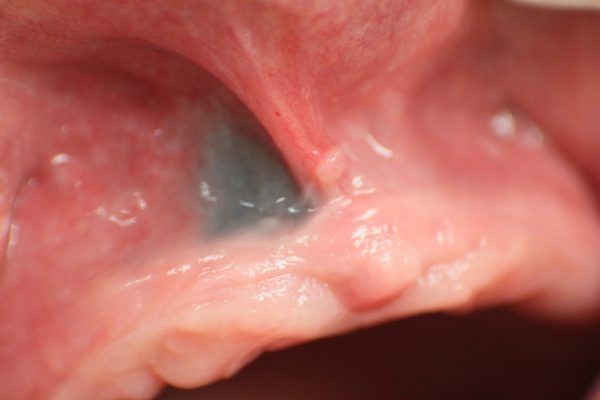
Industries which involve exposure to heavy metals, such as construction work, lead mining and plumbing may also result in the development of pigmented oral lesions via a similar mechanism.
Other sources of discolouration include food and various medications. Examples include chlorhexidine, minocycline, and zidovudine. These drugs can lead to discolouration of the teeth, macular dark areas on the dorsum of the tongue and widespread brown pigmentation respectively.
Chromogenic bacteria
Chromogenic bacteria produce black or brown pigment. Examples include Aspergillus and Actinomyces species.6
The enzymes contained within the bacteria act on saliva to produce the black or brown pigment which causes the condition known as ‘black hairy tongue’ (figure 2). Other causes of black hairy tongue include chlorhexidine, certain foods and smoking. Management includes adequate tongue brushing and excellent oral hygiene to remove food particles and debris. Patients should be advised to avoid the causes listed above.
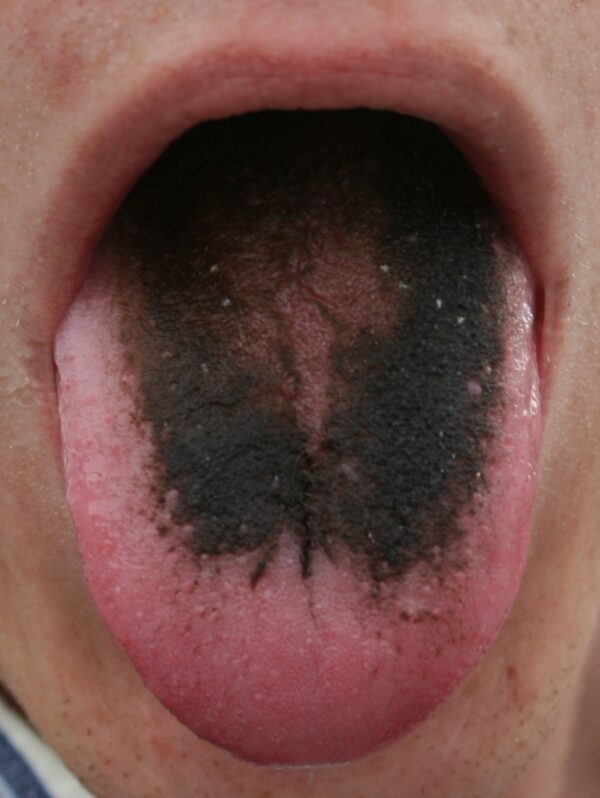
Exogenous pigmentation
Exogenous pigmentation has an external cause or origin.1 Examples, as listed above include graphite and drugs including bismuth subsalicylate (Pepto-Bismol).
The pigmented lesions may appear brown, black, green, or grey. It is vital to take a thorough history to allow identification of exogenous causes including occupational history, previous dental work, medication history and dietary details.
General management of exogenous pigmentation involves removing the precipitant where possible.
Smoker’s melanosis
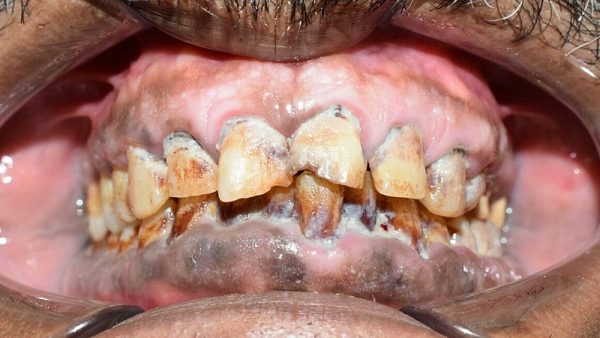
Smoker’s melanosis is a brownish discolouration of the oral mucosa (figure 3). The process often affects the anterior facial gingivae of both jaws, but with a higher incidence in the mandible.
Pipe smokers more frequently display pigmentation of the commissures (corners of the mouth) and buccal mucosae. Treatment is not required, however, smoking cessation may inhibit further progression.
Endogenous pigmentation
Endogenous pigmentation has a wide variety of causes.1 Pigmentation may be a benign physiological variant, such as that seen in Asian or Afro-Caribbean ethnicities. Others, however, may be pathological.
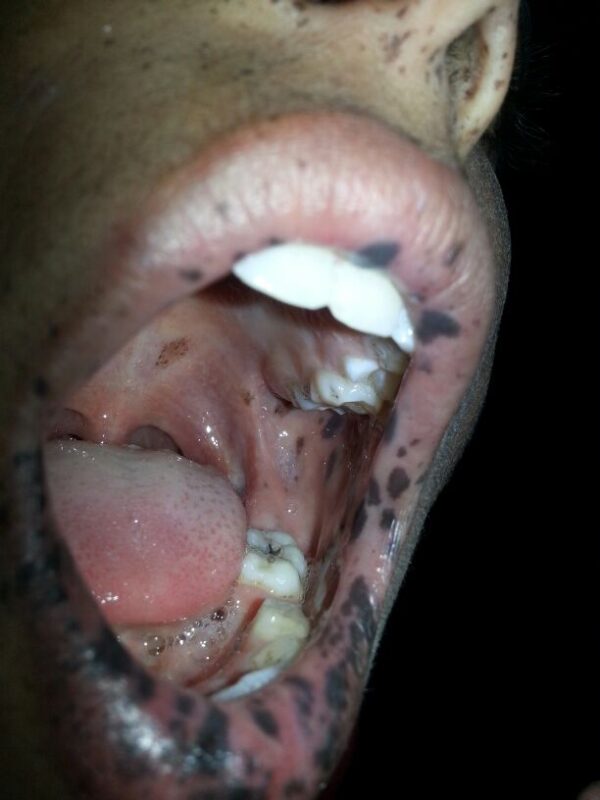
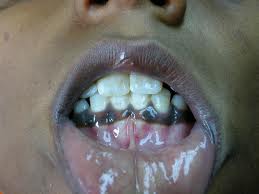
Peutz-Jegher’s syndrome
Peutz-Jegher’s syndrome is a rare, inherited condition characterised by hyperpigmentation around the mouth and on the lips, as well as the fingers and toes.1 Patients are more susceptible to polyps in the digestive tract, as well as cancers in the breast, colon, rectum, pancreas, and stomach.
Pigmented naevia
Pigmented naevi (<6mm diameter) are occasionally found in the mouth and are either flat pigmented lesions (macules) or slightly raised (papules).4 The palate is most affected. Usually, no active treatment is required, but monitoring to ensure no change in size, shape, consistency or associated symptoms is necessary.
Addison’s disease
Addison’s disease is another cause of endogenous pigmented lesions of the oral mucosa. Addison’s disease involves an inability of the adrenal glands to produce enough steroid hormones, most commonly due to autoimmune destruction. Oral pigmentation in Addison’s disease may be a precursor to more generalised skin hyperpigmentation.
Addison’s disease is life-threatening if left untreated, therefore urgent onwards referral to an endocrinologist is essential to allow commencement of appropriate glucocorticoid replacement therapy.10
Oral melanomas
Oral mucosal melanoma is extremely rare, accounting for only 0.5 % of oral neoplasms and 1–2 % of all melanomas. They occur more commonly in males than females, between the 4th and 7th decade, and can be non-pigmented (amelanotic). The hard palate is most commonly affected (40%) followed by the gingivae.
Oral melanomas have an extremely poor prognosis, typically requiring radical surgical excision. The 5-year survival rate is less than 12.3%.12
Clinical features
History
A detailed history of a pigmented lesion is important to formulate a differential diagnosis. The history should include:
- Name, age and occupation of the patient
- History of the lesion: clarify when the lesion was first noticed and how it has progressed since.
- Medical history: ask about conditions associated with oral pigmentation (e.g. Addison’s disease, Peutz-Jegher’s syndrome, haemochromatosis).
- Drug history: take a comprehensive medication history (e.g. tetracycline antibiotics).
- Dental history: clarify when the patient last had a dental review and if they are aware of any dental problems. Also ask about previous dental treatments, including amalgam fillings and crowns.
- Social history: ask about smoking history and alcohol intake.
Clinical examination
- Clinical findings will vary depending on the aetiology as discussed earlier in the article.
- Clinical photography can be useful to monitor lesions.
Management
If there is a clear benign precipitant for the pigmented lesion (e.g. amalgam tattoo), it may be monitored with regular clinical review and photography.
If there is any doubt as to the aetiology of the lesion, referral to a relevant specialist is required (e.g. oral medicine specialist for biopsy or endocrinologist if concerns regarding Addison’s).
Key points
- Oral pigmentation can arise from endogenous and exogenous causes.
- Careful assessment is required to decide whether oral pigmented lesions should be monitored or referred to a specialist for further investigation and treatment. The shape, size, location and colour of such lesions should be carefully documented.
- Clinical photography is essential for accurate monitoring of lesions as well as being invaluable for onward referral. In the case of a more sinister diagnosis, such as melanoma, regular monitoring could be lifesaving.12
- The table below summarises the classification of oral pigmentation.
Table 1. A non-exhaustive summary table of the classification of oral pigmentation.1
| The classification of oral pigmentation | ||
| Exogenous | Endogenous | Syndrome related |
|
Drug-induced Tobacco Heavy metals Amalgam tattoo |
Addison’s disease Diabetes Pregnancy Hyperthyroidism |
Peutz-Jegher’s syndrome McCune-Albright syndrome Haemochromatosis
|
| Infections | Chronic irritation | Reactive |
|
HIV Candidiasis Tuberculosis |
Post-traumatic Post-inflammatory (lichen planus, pemphigus) |
Melanocytic macule |
| Neoplastic | ||
|
Benign (nevus) Malignant (melanoma) |
||
Editor
Dr Chris Jefferies
References
- Sreeja et al. Oral pigmentation: A review. J Pharm Bioallied Sci. 2015 Aug; 7(Suppl 2): S403–S408. doi: 10.4103/0975-7406.163471. Available from: [LINK]
- A, Pavone.M, Blanas.N, Bradley.G. Pigmented Lesions of the Oral Cavity: Review, Differential Diagnosis, and Case Presentations. J Can Dent Assoc 2004; 70(10):682–3 Available from: [LINK]
- O. Gondak et al. Oral pigmented lesions: Clinicopathologic features and review of the literature. Medicina oral, patologia oral y cirugia bucal 17(6) · May 2012 Available from: [LINK]
- Susan Müller, Non-Neoplastic Lesions of the Oral Cavity, Head and Neck Pathology (Third Edition), 2019, Available from: [LINK]
- Bin im Garten. Amalgam tattoo from filling, left on the gums. License: [CC-BY-SA]. Available from: [LINK]
- Faizan Alawi, DDS, Pigmented lesions of the oral cavity: An Update. Dent Clin North Am. 2013 Oct; 57(4): 699–710. Published online 2013 Aug 15. doi: 1016/j.cden.2013.07.00. Available from: [LINK]
- Com4. Black hairy tongue (Lingua Villosa Nigra). License: [Public domain]. Available from: [LINK]
- Shaimaa Abdellatif. Smoker’s melanosis in a patient consuming 2 packs of cigarettes per day. License: [CC-BY-SA]. Available from: [LINK]
- Abdullah Sarhan. Oral presentation of a patient with Peutz- Jegher’s Syndrome. License: [CC-BY-SA]. Available from: [LINK]
- Reshna Roy. Classification of oral pigmented lesions: A review, International Journal of Applied Dental Sciences 2019; 5(2): 397-402 Available from: [LINK]
- FlatOut Dermatology Online Journal. Classic hyperpigmentation of Addison’s disease. License: [Public domain].
- Narayan Sharma Lamichhane, et al. Primary malignant mucosal melanoma of the upper lip: a case report and review of the literature BMC. Res Notes. 2015; 8: 499. Available from: [LINK]




