- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Cranial nerve XI is the accessory nerve, supplying somatic motor fibres to two large muscles: the sternocleidomastoid and trapezius. In this article, we look in more detail at the structure, function and clinical relevance of the accessory nerve.
Check out our summary of the cranial nerves.
You can also check out our cranial nerve anatomy quiz.
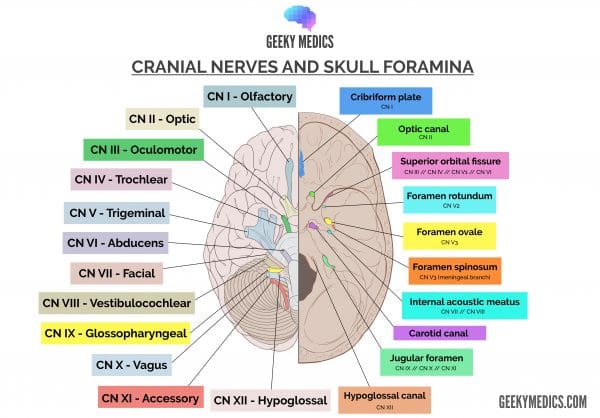
Accessory nuclei
The accessory nerve is traditionally described as arising from two nuclei (cranial and spinal):
- Cranial nucleus: joins the vagus nerve; based on function, this is not a true part of the accessory nerve, and will not be discussed further.
- Spinal nucleus: lower motor neurons clustered in the lateral aspect of the ventral horn of the superior cervical cord (C1-C6). This lateral aspect of the ventral horn appears continuous with the nucleus ambiguus of the medulla oblongata.
Accessory nerve
Fibres exiting this nucleus from these spinal levels exit the superior cervical cord and lower medulla at the post-olivary sulcus. As some roots begin arising below the skull, CN XI is the only cranial nerve that enters the skull passing through the foramen magnum.
It then courses inferolaterally with CNs IX and X to reach the jugular foramen. Here, it transiently interacts with the cranial portion of the accessory nuclear complex. It then passes through the jugular foramen.
Extracranial accessory nerve
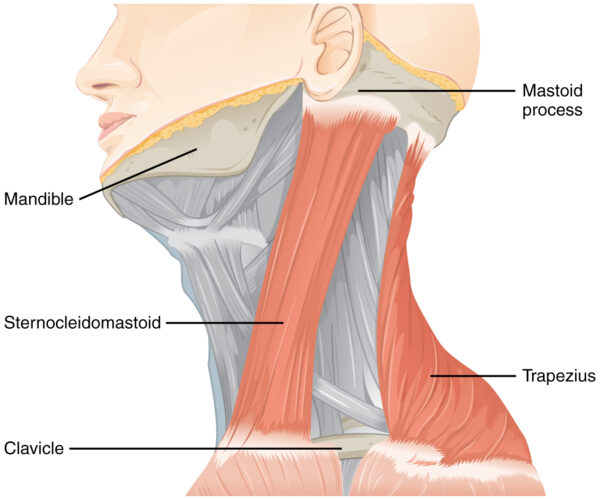
Upon passing through the jugular foramen, the spinal accessory nerve travels inferiorly with the internal carotid artery to reach and supply the sternocleidomastoid muscle. It continues travelling through the posterior triangle of the neck to supply motor fibres to the trapezius.
Clinical relevance: assessing the accessory nerve
Examination of the accessory nerve involves assessing two muscles: the trapezius and sternocleidomastoid.
When assessing the trapezius, ask the patient to shrug their shoulders, then apply resistance. Accessory nerve weakness will present with weak or no resistance to your downward force.
When assessing the sternocleidomastoid, ask the patient to turn their head as far to the left as they can. With your left hand bracing their left shoulder, pull their chin forward. Weakness or no resistance to your pull suggests accessory nerve weakness.
The accessory nerve travels between the prevertebral and investing fascial layers of the neck. This superficial location predisposes it to injury.
Clinical relevance: tension headaches
The motor innervation of the trapezius and sternocleidomastoid has been discussed in some detail, but what about the sensory innervation?
The sternocleidomastoid derives sensory supply from the dorsal rami of spinal nerves C2 and C3. The trapezius derives sensory supply from the dorsal rami of C3 and C4.
Chronic contraction in these muscles can lead to increased tension and local inflammatory mediators such as substance P and prostaglandins. These inflammatory mediators may stimulate the C2-C4 nerve roots and cause a referred pain in the distribution of C2 to C4 – the head and neck.
Stretching and massage of the sternocleidomastoid and trapezius muscles may help to alleviate this pain.
Key points
- CN XI is the accessory nerve
- It originates in the medulla oblongata and superior cervical cord region
- It provides general somatic efferent fibres to the trapezius and sternocleidomastoid
- It exits the spinal cord in the neck and enters the skull through the foramen magnum
- It then leaves the skull by the jugular foramen with CNs IX and X
References
Reference texts
- Sinnatamby, C. S. (2011). Last’s Anatomy, International Edition: Regional and Applied. Elsevier Health Sciences.
- Moore, K. L., Dalley, A. F., & Agur, A. M. (2013). Clinically oriented anatomy. Lippincott Williams & Wilkins.
- Nolte, J. (2002). The human brain: an introduction to its functional anatomy.
- Snell, R. S. (2010). Clinical neuroanatomy. Lippincott Williams & Wilkins.
Reference images




