- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Cranial nerve V is known as the trigeminal nerve. It is the largest (in diameter) of the cranial nerves and contains sensory fibres for the face, as well as a motor segment important for mastication (chewing).
Understanding the embryology can assist in appreciating the course and innervation of cranial nerves V and VII, the facial nerve. This article explores the embryological and anatomical structure of the trigeminal nerve complex before focussing on its clinically relevant aspects.
A note on nomenclature:
- A nucleus refers to a density of neuronal somas (cell bodies) that lie within the central nervous system.
- A ganglion refers to a density of neuronal somas that lie outside the central nervous system.
Check out our summary of the cranial nerves here.
You can also check out our cranial nerve anatomy quiz here.
Embryology
The name trigeminal is derived from the Latin “tri-” meaning three, and “-geminal” meaning a group attached to a common point. There are ‘three’ major branches of the trigeminal nerve, coming from four distinct nuclei in the brainstem.
The trigeminal nerve complex begins growing in the brainstem from four distinct paired nuclei, as discussed below.
Sensory nuclei:
- Mesencephalic trigeminal nucleus: mainly in the midbrain (mesencephalon)
- Principal/chief/main trigeminal nucleus: mainly in the pons
- Spinal trigeminal nucleus: mainly in the medulla oblongata and upper cervical cord
Motor nuclei:
- Trigeminal motor nucleus: in the pons
These nuclei form early during neural development and send sensory fibres to a common point of exit in the brainstem at the ventral mid-pons, at roughly the same level as the principal trigeminal nucleus.
The trigeminal motor nucleus “hitch-hikes” with this common sensory afferent. Together, these structures go to supply the mesodermal structures associated with the first pharyngeal arch (sometimes called the first branchial arch).
Structures of the first pharyngeal arch
The structures of the first pharyngeal arch are shown below.
Bones
- Maxilla (maxillary prominence)
- Zygomatic bone (maxillary prominence)
- Vomer (maxillary prominence)
- Palatine bone (maxillary prominence)
- Mandible (mandibular prominence)
- Squamous part of the temporal bone
- Malleus
- Incus
Skin
- Overlying the bony structures above
Muscles
- Tensor veli tympani
- Tensor veli palatini
- Anterior belly of the digastricus
- Mylohyoid muscle
- Muscles of mastication: masseter, temporalis, lateral and medial pterygoid muscles
As you progress through the information below, you will see a link between the trigeminal innervation of muscles and the bones they attach to.
The trigeminal nuclei
In order to understand the somatosensory function of the trigeminal nerve, we must first appreciate the different trigeminal nuclei and the role they play.
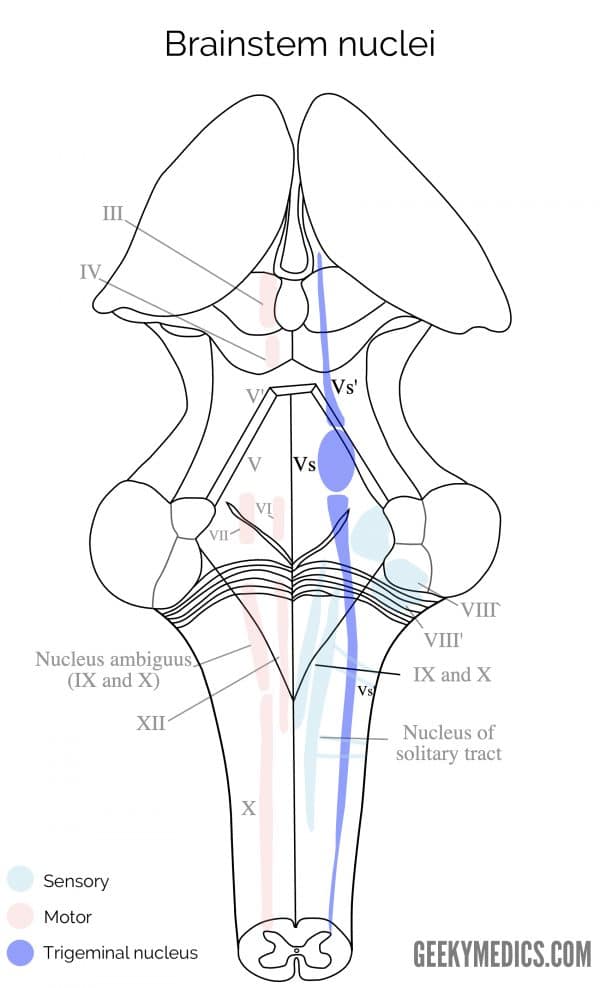
Mesencephalic trigeminal nucleus:
- Proprioceptive information from the face
- Superior-most Vs’ (Figure 2)
Principal trigeminal nucleus:
- Light touch and discriminative information from the face
- Middle, round Vs (Figure 2)
Spinal trigeminal nucleus:
- Pain and temperature information from the face
- Inferior-most Vs’ (Figure 2)
Trigeminal motor nucleus:
- Motor efferent fibres for somatic control of mastication
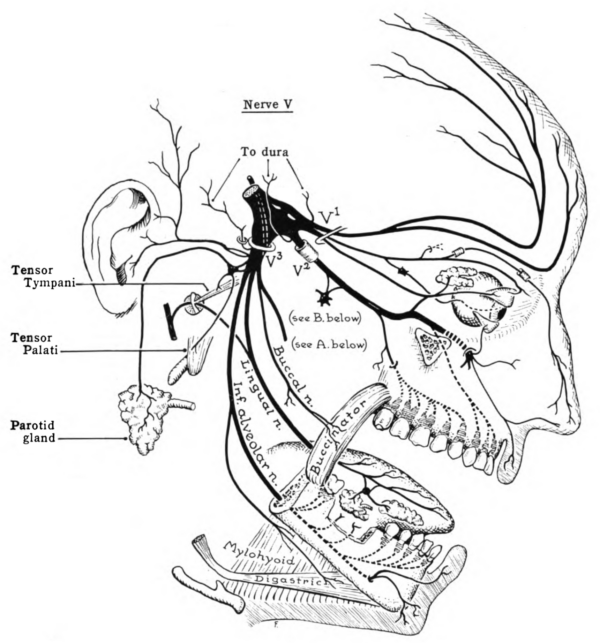
The trigeminal nerve roots
Both motor and sensory components of the trigeminal nerve complex exit the ventral mid-pons as distinct nerves.
The larger, more medial nerve is the trigeminal sensory root; and a smaller, more lateral nerve is the trigeminal motor root named portio minor (the minor portion of the trigeminal nerve; the fourth branch). These two nerve roots come together to form a common trigeminal nerve complex.
The trigeminal nerve complex
The trigeminal nerve complex travels anteriorly in the middle cranial fossa before reaching the trigeminal ganglion, which lies immediately posterolateral to the cavernous sinus, in a depression called the trigeminal cave.
Each of the fibres from the three nuclei mixes here so that part of the mesencephalic, principal and spinal trigeminal nuclei all send fibres to the three divisions of the trigeminal nerve complex:
- Ophthalmic (sensory only)
- Maxillary (sensory only)
- Mandibular (the only branch to contain sensory and motor fibres)
The course of these three divisions will be considered before discussing each branch separately.
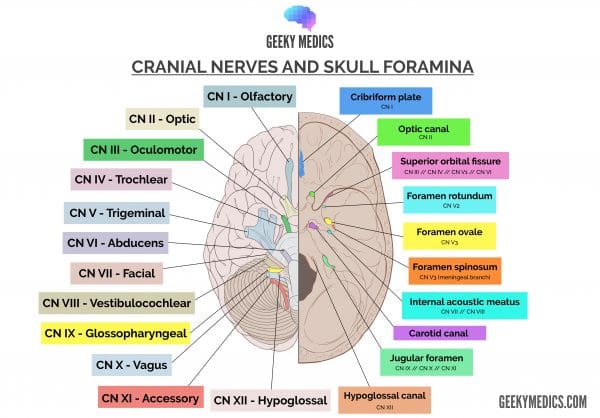
Cranial foramen of the trigeminal branches
The ophthalmic branch of cranial nerve V (V1) is the most superior of the three divisions. After leaving the trigeminal ganglion, it pierces a layer of dura mater, travels in the lateral wall of the cavernous sinus and continues through the superior orbital fissure.
The maxillary branch of cranial nerve V (V2) is the middle of the three divisions. After leaving the trigeminal ganglion, it pierces the dura mater inferior to V1 and travels through the lateral wall of the cavernous sinus, before exiting the skull via the foramen rotundum.
The mandibular branch of cranial nerve V (V3) is the most inferior of the three divisions. After leaving the trigeminal ganglion, it immediately dives inferiorly and laterally to reach the foramen ovale. It does not pass through the cavernous sinus.
Trigeminal nerve branches
There are several branches in each of the divisions of the trigeminal nerve.
Ophthalmic division
Branches of the ophthalmic division include:
- Frontal: the skin of the forehead, frontal sinus and medial superior eyelid
- Lacrimal: lacrimal gland, conjunctiva and lateral superior eyelid
- Nasociliary: mucosal epithelium of the ethmoidal air cells, upper eyelids, nasal bridge, conjunctiva, lacrimal sac and caruncle
- Long ciliary nerve: contributes to scleral innervation (contains some sympathetic fibres from the internal carotid plexus)
- Parasympathetic: the pterygopalatine ganglion of the facial nerve contributes some fibres to V2, which then pass into the lacrimal nerve for secretomotor action at the lacrimal gland.
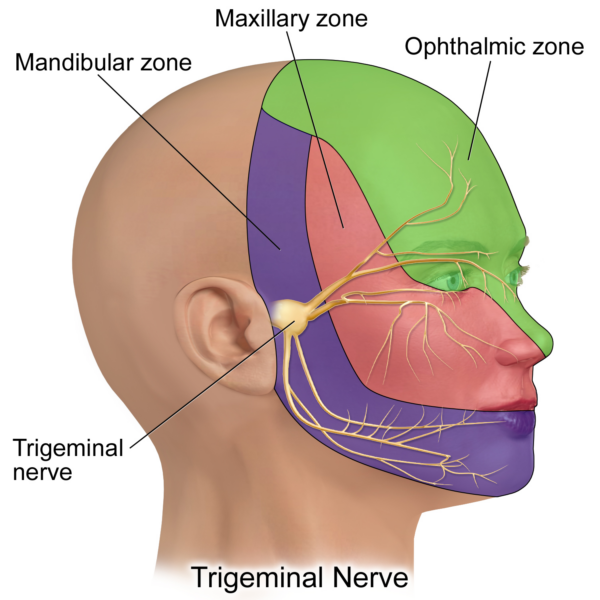
The ophthalmic division supplies sensory innervation from the crown of the head down to the upper eyelid at the lateral canthus of the eye, including the cornea.
Maxillary division
Branches of the maxillary division include:
- Middle meningeal: supplies the meninges
- Nasopalatine: mucosa of the nasal septum, palate around the anterior teeth
- Greater and lesser palatine: sensation and parasympathetic innervation to the gingiva and mucosa near the hard palate
- Zygomatic: skin over the zygomatic and temporal bones
- Infraorbital: lower eyelid and upper lip
The maxillary division supplies sensory innervation from the lower eyelid at the lateral canthus to the upper lip at the lateral angle of the mouth.
Mandibular division
Branches of the main trunk (before splitting into anterior and posterior division) of the mandibular division include:
- Meningeal: meninges
- Branch to medial pterygoid, tensor tympani and tensor veli palatini
Branches of the anterior division include:
- Masseteric: to masseter muscle
- Lateral pterygoid: to lateral pterygoid muscle
- Deep temporal: to temporalis muscle
- Buccal: sensory to buccal muscle
Branches of the posterior division include:
- Auriculotemporal: sensory to the ear and temporal skin
- Lingual: sensory to anterior 2/3 of the tongue
- Inferior alveolar: sensory to teeth, motor branch to the mylohyoid and anterior belly of the digastric muscle
The mandibular division supplies sensory innervation from the lower lip at the lateral angle of the mouth to the lower border of the mandible and motor innervation to the muscles of mastication.
Clinical relevance: testing the trigeminal nuclei and nerves
When assessing the trigeminal nerve, it is also important to consider which specific nucleus is being assessed:
- Pin-prick: assesses pain in each of the three sensory distributions of the face, and also assesses the function of the spinal trigeminal sensory nucleus
- Cotton wool: assesses light tough in each of the three sensory distributions of the face, and also assesses the function of the principal trigeminal nucleus
- Jaw-jerk reflex: assess the proprioceptive reflex circuit of the masseter and temporalis muscles, and also the activity of the mesencephalic trigeminal nucleus
- Muscles of mastication (temporalis and masseter): assesses the activity of the muscles of mastication, and also the activity of the trigeminal motor nucleus
This can help to narrow the differential diagnosis to either a central or peripheral lesion.
Clinical relevance: the corneal reflex
The corneal reflex is an important step in the assessment of cranial nerves and is a way to link the examination of the fifth and seventh cranial nerves.
The sensory innervation of the cornea is received by V1, which sends this information to the spinal trigeminal nucleus, which interacts with both facial motor nuclei of cranial VII. On synapsing at this nucleus, an activating constrictor signal is sent bilaterally to the orbicularis oculi, causing eye closure.
Embryology and innervation
It is easy to confuse the muscles of the face with their innervation by either the trigeminal or facial nerves. While the trigeminal nerve is the nerve for the first pharyngeal arch, the facial nerve is the nerve of the second pharyngeal arch.
Now that we understand what each branch of the trigeminal nerve innervates, we can deduce which muscular structures are innervated by the trigeminal nerve and which are innervated by the facial nerve.
The muscles attached to the mandible are innervated by the motor root of the trigeminal nerve, portio minor, as it travels with V3. This includes the muscles of mastication, mylohyoid and anterior belly of the digastric muscle.
The posterior belly of the digastric muscle is attached between the hyoid bone and the mastoid notch of the temporal bone – two structures derived from the second pharyngeal arch. Thus, it is innervated by the facial nerve. The styloid process is another structure that is derived from the second pharyngeal arch, and the stylohyoid is appropriately supplied by the facial nerve. The final example is the stapes of the ear, derived from the second pharyngeal arch, which is supplied by the facial nerve.
Key points
- CN V is the trigeminal nerve.
- It has three nuclei: mesencephalic (proprioception), principal (light touch and discrimination) and spinal (pain, temperature, crude touch)
- It emerges from the pons
- It is the afferent limb of the corneal reflex; CN VII is the bilateral efferent limb
- CN V has three divisions, shown in the table below
Table 1. The three divisions of the trigeminal nerve.
| Division | Modality | Sensory function | Motor function | Foramen |
|
Ophthalmic V1 |
General somatic afferent | Above the lower eyelid | X | Superior orbital fissure |
|
Maxillary V2 |
General somatic afferent | Lower eyelid to the upper lip | X | Foramen rotundum |
|
Mandibular V3 |
General somatic afferent Special visceral efferent |
Below upper lip | Muscles of mastication | Foramen ovale |
References
Reference texts
- Sinnatamby, C. S. (2011). Last’s Anatomy, International Edition: Regional and Applied. Elsevier Health Sciences.
- Moore, K. L., Dalley, A. F., & Agur, A. M. (2013). Clinically oriented anatomy. Lippincott Williams & Wilkins.
- Nolte, J. (2002). The human brain: an introduction to its functional anatomy.
- Snell, R. S. (2010). Clinical neuroanatomy. Lippincott Williams & Wilkins.
Reference images
- Patrick J. Lynch, medical illustrator. License: [CC BY]. Modified by Dr Lewis Potter.
- CFCF. License: [CC BY-SA]
- BruceBlaus. License: [CC BY-SA]