- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Thyroid function tests (TFTs) are a commonly requested investigation in clinical practice. This guide aims to provide you with the knowledge needed to interpret TFTs and consider underlying pathology.
Thyroid hormonal axis
The ability to interpret thyroid function tests (TFTs) first requires an understanding of the thyroid hormonal axis. Each of the thyroid function tests assesses a different aspect of this axis and understanding the relationship between the results is key to being able to reach a diagnosis.
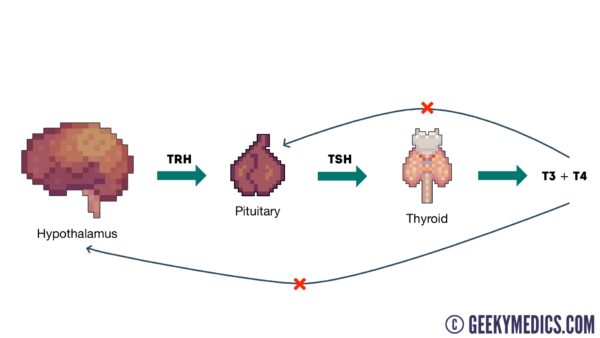
Thyroid hormonal axis overview
1. The paraventricular nuclei in the hypothalamus release thyroid-releasing hormone (TRH).
2. This causes thyrotrope cells in the anterior pituitary to release thyroid-stimulating hormone (TSH).
3. The thyroid responds to the TSH by releasing T4 and T3.
4. T4 inhibits the pituitary and hypothalamus in a negative feedback loop. This is the ‘brake system’ which aims to maintain a state of homeostasis.
Thyroid function tests (TFTs)
The term ‘thyroid function tests‘ refers to the following investigations:
- TSH (0.4 – 4 mU/L)
- Free T4 (9 – 25 pmol/L)
- Free T3 (3.5 – 7.8 nmol/L)
There are separate reference ranges for children and pregnant women.
Reference ranges for TFTs often vary between labs, so always refer to your local guidelines.
Important points
Whilst free T3 (fT3) is measured, it is less relevant than free T4 (ft4). This is because the thyroid releases T4 and T3 at a ratio of about 20:1 respectively, with T3 mainly being produced by peripheral conversion of T4. As a result, T4 is a much better marker of thyroid function.
Free T4 (fT4) is roughly 1% of the total T4, with the rest being bound to thyroid-binding globulin.
T4 has a half-life of about one week, therefore, to monitor the impact of an intervention (e.g. increasing a patient’s levothyroxine dose) you need to wait several weeks before repeating TFTs.

Hypothyroidism
Primary hypothyroidism
Primary hypothyroidism involves reduced secretion of thyroid hormone from the thyroid gland itself.
Pathology which decreases the thyroid’s ability to release T4 and T3 or respond to TSH can, therefore, cause primary hypothyroidism.
Primary hypothyroidism is the most common cause of hypothyroidism, accounting for 99% of all cases.
Pathophysiology
1. Less T4 and T3 are produced due to the thyroid’s reduced capacity to produce hormone or respond to TSH.
2. As a result, there is reduced negative feedback on the pituitary and hypothalamus.
3. The reduction in negative feedback results in increased production of TRH (which we don’t typically measure) and TSH.
4. The end result is low T4 and T3 and a raised TSH.
Diagnosis
The typical findings that would indicate a diagnosis of primary hypothyroidism are as follows:
- Raised TSH: due to the absence of negative feedback.
- Low T4: due to the thyroid’s inability to produce enough T4.
A normal T4 in the context of a raised TSH may suggest subclinical hypothyroidism (most commonly caused by underlying autoimmune disease).
Aetiology
Causes of primary hypothyroidism include:
- Autoimmune thyroiditis (50%)
- Iodine deficiency or excess
- Thyroidectomy
- Therapy with radioactive iodine – a treatment for hyperthyroidism
- External radiotherapy
- Drugs
- Thyroid agenesis or dysgenesis
Secondary hypothyroidism
Secondary hypothyroidism involves a reduction in the hormones that stimulate the thyroid to produce thyroxine.
Pathology which affects the pituitary and hypothalamic glands can result in decreased production of TRH and TSH, causing secondary hypothyroidism.
Secondary hypothyroidism is a rare cause of hypothyroidism, accounting for 1% of all cases.
Pathophysiology
1. Decreased production or secretion of TRH and TSH results in decreased stimulation of the thyroid gland.
2. The thyroid gland, therefore, produces less T3 and T4.
3. The low T3 and T4 would normally stimulate the pituitary and hypothalamic glands to increase TRH and TSH production, however, they are unable to increase production.
4. The end result is low T4 and T3 and a normal/low TSH.
Diagnosis
The typical findings that would indicate a diagnosis of secondary hypothyroidism are as follows:
- Normal/low TSH: due to a lack of production.
- Low T4: due to the absence of any positive feedback from TSH.
Aetiology
Causes of secondary hypothyroidism can be either pituitary or hypothalamic in origin.
Pituitary causes:
- Pituitary adenoma: the most common cause.
- Pituitary surgery or radiotherapy which damages the pituitary tissue.
Hypothalamic causes:
- Hypothalamic or suprasellar tumour.
- Surgery or radiotherapy which damages the hypothalamic tissue.
TRH is not measured as part of thyroid function tests, as it is only released locally between the hypothalamus and pituitary (so it is not present in representative quantities within the peripheral circulation). Both structures are commonly grouped together into ‘secondary’ because an issue with TRH gives the same blood test results as an issue with TSH, however, some literature may refer to the hypothalamus as a ‘tertiary’ cause.
Hyperthyroidism
Primary hyperthyroidism
Primary hyperthyroidism involves an excessive production of T3 and T4 by the thyroid gland as a result of pathology within the thyroid gland itself.
Pathophysiology
1. The thyroid produces excessive amounts of T4 and T3.
2. The excessive T4 and T3 cause negative feedback on the pituitary and hypothalamus, resulting in decreased production of TRH and TSH.
3. The end result is a raised T3 and T4 and a low TSH.
Diagnosis
The typical findings that would indicate a diagnosis of primary hyperthyroidism are as follows:
- Raised T3/T4: due to excessive production.
- Low TSH: due to negative feedback on the pituitary/hypothalamus.
Aetiology
Causes of primary hyperthyroidism include:
- Graves’ disease (75% of all cases)
- Toxic multinodular goitre
- Toxic adenoma
- Iodine-induced (rare)
- Trophoblastic tumour (very rare)
Secondary hyperthyroidism
Secondary hyperthyroidism involves stimulation of the thyroid gland by excessive thyroid-stimulating hormone (TSH).
Pathophysiology
1. TSH production is increased by either the pituitary/hypothalamus or another source (known as ectopic production).
2. The excess TSH causes overstimulation of the thyroid gland, resulting in high levels of T3 and T4 production.
3. Normally a raised T3 and T4 level would cause negative feedback, decreasing TSH production, however, in this instance, the TSH production is not responsive to any negative feedback, resulting in continued excess production.
Diagnosis
The typical findings that would indicate a diagnosis of secondary hyperthyroidism are as follows:
- Raised T3/T4: due to excess production that is driven by a raised TSH level.
- Raised TSH: due to excess production.
Aetiology
Causes of secondary hyperthyroidism include:
- TSH-secreting tumour
- Chorionic-gonadotropin secreting tumours (hCG secreting)
- Thyroid hormone resistance (usually euthyroid): TSH is resistant to T3/T4 negative feedback.
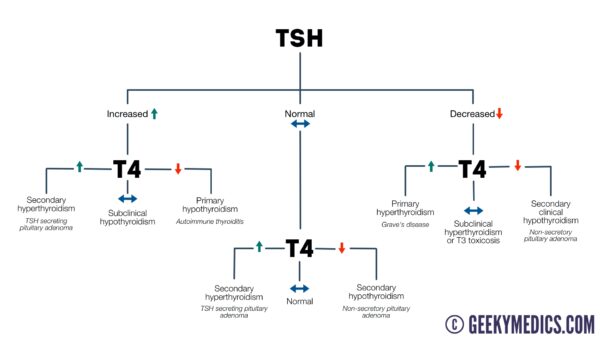
Summary
Below is a flowchart that summarises the key points discussed in this article.
Reviewer
Professor Levy
Consultant Endocrinologist
References
- The endocrine system at a glance, 3rd edition; B.Greenstein D.Wood; Wiley-Blackwell; ISBN 978-1-4443-3215-5; 2011
- Comprehensive Clinical Endocrinology 3rd ed., G.Besser, M. Thorner; 2002; 0-7234-3185-X; Elsevier science limited
- Willims Textbook of Endocrinology 10th ed.; Larsen, Kronenberg, Melmed, Polonsky; 0-7216-9184-6; 2003
- De Leo, Lee, Braverman; Hyperthyroidism; Lancet. 2016 Aug 27; 388(10047): 906–918; available from: [LINK].
- Kostoglou-Athanassiou, Ntalles; Hypothyroidism – new aspects of an old disease; Hippokratia, 2010 Apr-Jun; 14(2): 82-87
- Dr Lousie Newson; Thyroid Function Tests. Patient.info. Published in 2015. Available from: [LINK].




