- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Introduction
Chiari malformations are a group of conditions characterised by abnormal displacement of the hindbrain (cerebellum, medulla oblongata, pons) into the spinal canal through a defect in the skull.1
Chiari malformations are estimated to occur in 1 in 1000 births and with a slight female predominance (3:1 ratio of females to males).
Aetiology
There are four types of Chiari malformations.2
Type 1 Chiari malformation
Type 1 Chiari malformation is the most common and mildest form of the disease.
Patients with type 1 malformations tend to present during late childhood or adulthood.
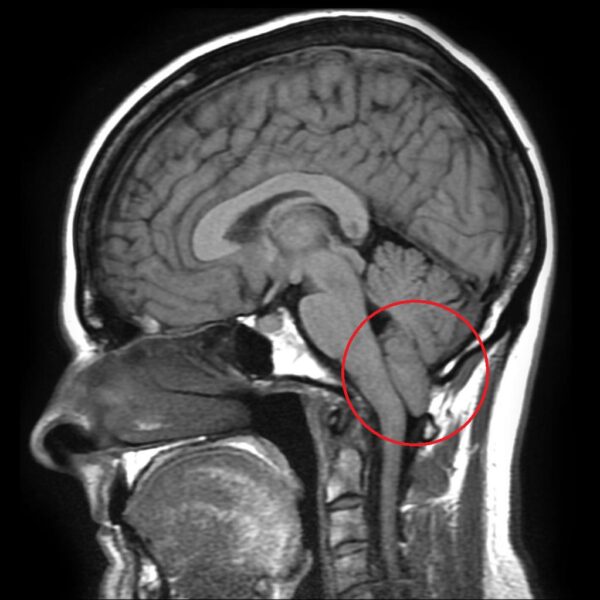
Type 1 Chiari malformation is characterised by a downward displacement of the cerebellar tonsils, of more than 5mm, through the foramen magnum.
This type of malformation can occur due to congenital or acquired (e.g. previous neurosurgery) structural defects in the skull base.
The defect in the skull base reduces the space available in the posterior fossa for the cerebellum, resulting in the cerebellar tonsils protruding through the foramen magnum. As a result, nearby neurological structures can become compressed, which then causes neurological symptoms and signs.
Type 2 Chiari malformation
Type 2 Chiari malformation (also known as Arnold-Chiari malformation) involves a greater range of brain tissue and a more shallow posterior fossa than is seen in type 1.
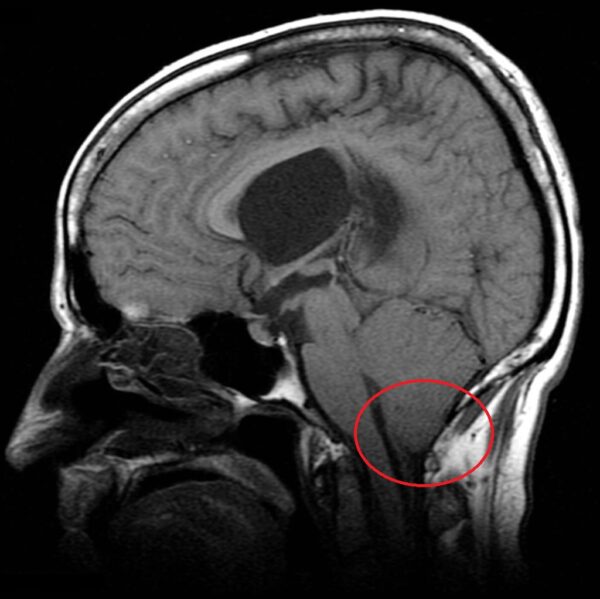
There is downward displacement of the cerebellar tonsils, as well as the fourth ventricle, brainstem and inferior vermis. Because there is more brain matter involved with this type of malformation, the clinical presentation tends to be more severe than type 1.
People with this type of malformation present earlier, typically during early childhood or even infancy.
Type 2 Chiari malformation is also often associated with myelomeningocele as a result of the vertebrae and spinal canal not closing properly before birth (i.e. spina bifida).
Type 3 Chiari malformation
Type 3 Chiari malformation is much rarer than type 1 and 2. In type 3, there is herniation of the posterior fossa’s contents through a posterior encephalocele.
This is a rare congenital type of neural tube defect in which a portion of the skull has not formed properly, which enables parts of the brain and meninges to protrude through it. It is usually associated with a poor prognosis.
Type 4 Chiari malformation
Type 4 Chiari malformation is very rare and is not compatible with life. It involves the incomplete development of the cerebellum.
Clinical features
This section will focus on the clinical features of type 1 and type 2 Chiari malformations.
Although both type 1 and type 2 Chiari malformations present with similar clinical features, the severity of these features is typically worse in patients with a type 2 malformation.
History
Typical symptoms of type 1 and 2 Chiari malformations include:1-3
- Sub-occipital headaches: often worsened by Valsalva manoeuvres such as coughing, straining or sneezing
- Lhermitte’s sign: an electric shock-type sensation that, upon neck flexion, radiates down the spine and sometimes into the limbs
- Neck pain
- Dizziness and balance problems
- Arm and/or leg weakness
- Numbness/tingling in the arms and/or legs
- Double vision
- Slurred speech
- Swallowing problems
- Hearing loss
- Tinnitus
Clinical examination
All patients require a thorough neurological examination.
Typical clinical findings may include:1-3
- Motor or sensory deficits of the limbs (e.g. weakness, loss of temperature sensation)
- Dysarthria
- Diplopia
- Sensorineural hearing loss
- Cerebellar features such as ataxia and nystagmus
Investigations
Imaging
Relevant imaging investigations include:
- MRI head and spine: can provide high-resolution images of the defect in the skull and the position of the neural structures in the cranium and spinal canal
- Ultrasound: used for prenatal screening and can identify Chiari malformations in utero
Management
Conservative management
A conservative approach is adopted for patients who remain asymptomatic despite their Chiari malformation.
Routine monitoring of the defect and associated structures may be performed to allow early identification of complications.
Surgical management
Surgical management is offered to symptomatic patients with the aim of reducing symptoms and halting the progression of associated complications.
Patients with symptomatic type 2 Chiari malformations are typically offered surgery during early childhood as this can help significantly reduce mortality and morbidity.
Surgical treatments aim to decompress the brainstem and relieve pressure within the skull and spinal canal.
The main surgical options for the management of Chiari malformations include:
- Posterior decompression of the foramen magnum
- Ventriculoperitoneal (VP) shunt: to treat secondary hydrocephalus
- Syringo shunt (to treat some forms of syringomyelia – e.g. syringo-subarachnoid shunt)
Complications
Complications of Chiari malformations may include:
- Hydrocephalus: due to the blockage of normal CSF drainage within the CSF
- Syringomyelia: a CSF-filled tubular cyst, known as a syrinx, forms within the spinal cord’s central canal. The growing syrinx destroys the centre of the spinal cord, resulting in pain, weakness and sensory loss.
Key points
- Chiari malformations are a group of conditions characterised by abnormal displacement of the hindbrain (cerebellum, medulla oblongata, pons) into the spinal canal through a defect in the skull.
- There are four types of Chiari malformations, with type one and type two being the most common.
- Typical symptoms of Chiari malformations can include sub-occipital headaches, Lhermitte’s sign, neck pain, dizziness, balance problems, limb weakness, sensory disturbances, slurred speech, swallowing problems and hearing loss.
- Typical clinical signs of Chiari malformations include motor or sensory deficits of the limbs, dysarthria, diplopia, sensorineural hearing loss and cerebellar signs.
- The most important investigation in the diagnosis of Chiari malformations is an MRI of the head and spine.
- A conservative approach is adopted for patients who remain asymptomatic despite their Chiari malformation.
- Surgical treatments aim to decompress the brainstem and relieve pressure within the skull and spinal canal.
- Complications of Chiari malformations include hydrocephalus and syringomyelia.
Reviewer
Mr Konstantinos Lilimpakis
Neurosurgical Clinical Fellow
Editor
Samantha Strickland
Hull York Medical Student
References
- National Institute of Neurological Disorders and Stroke. Chiari Malformation Fact Sheet. Published in 2018. Available from: [LINK]
- Jones J. Chiari malformations. Published in 2018. Available here: [LINK]
- Khare S, Seth D. Annal of Indian Academy of Neurology. 2015. April; 18(2): 154-156. DOI: 10.4103/0972-2327.150622 Available from: [LINK].
- Neurosurgery Department at Great Ormond Street Hospital for Children. Encephalocele. Available from: [LINK].
- Frank Gaillard (Radiopaedia 2592). Chiari Malformation 1. License: [CC-BY-NC-SA]
- Frank Gaillard (Radiopaedia 16048). Chiari Malformation 2. License: [CC-BY-NC-SA]