- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Introduction
Hyperlipidaemia refers to raised levels of one or more of total cholesterol (TC), low-density lipoprotein cholesterol (LDL-C) and triglycerides (TG) in the blood.1
Dyslipidaemia is an umbrella term that includes hypercholesterolaemia, hyperlipidaemia and mixed dyslipidaemia. In mixed dyslipidaemia, LDL-C and TG levels are elevated and often accompanied by low levels of high-density lipoprotein cholesterol (HDL-C).2
Approximately 6 in 10 adults in England have serum cholesterol levels above 5 mmol/L.2
Heterozygous familial hypercholesterolaemia (FH) is one of the most common primary hyperlipidaemia with a prevalence of between one in 250 and one in 500 in the UK.
Homozygous FH is rare with an incidence of one in a million.3
Aetiology
The causes of hyperlipidaemia can be divided into primary hyperlipidaemia and secondary hyperlipidaemia.
Primary hyperlipidaemia
Most cases of primary hyperlipidaemia are due to genetic factors interacting with environmental factors. However, single-gene disorders may also be present.
Familial hypercholesterolaemia is usually caused by mutations in the low-density lipoprotein receptor (LDLR) gene which results in an autosomal dominant pattern of inheritance.
Secondary causes of hyperlipidaemia should be excluded before primary hyperlipidaemia may be diagnosed.4
Secondary hyperlipidaemia
The causes of secondary hyperlipidaemia can be further described based on the type of lipid that is elevated in the blood:4
- Secondary hypercholesterolaemia: hypothyroidism, pregnancy, nephrotic syndrome, anorexia nervosa and drugs (e.g. diuretics, glucocorticoids, androgens, antiretroviral agents and ciclosporin)
- Secondary hypertriglyceridaemia: type 2 diabetes mellitus, chronic kidney disease, abdominal obesity, excess alcohol, hepatocellular disease and drugs (e.g. beta-blockers, glucocorticoids, antiretroviral agents and retinoids)
Clinical features
History
Hyperlipidaemia is usually asymptomatic. Patients can present with features of acute pancreatitis such as sudden onset of severe central abdominal pain often radiating to the back, shock, and abdominal skin discolouration due to significantly elevated levels of TG.
Important areas to cover in the history include:5
- Personal history of cardiovascular diseases and secondary causes of hyperlipidaemia
- Family history of cardiovascular diseases, particularly at a young age (<50 years old)
- Smoking
- Excess alcohol consumption
- Obesity
Clinical examination
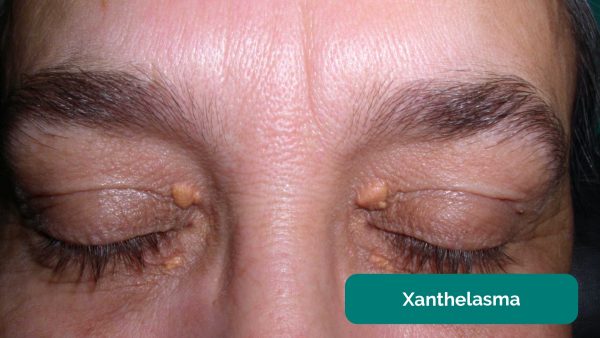
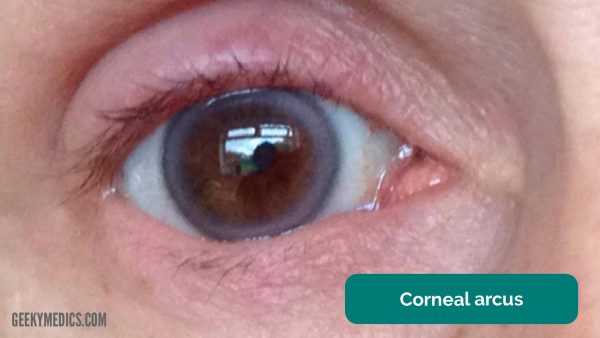
Some patients with hyperlipidaemia may develop signs including tendon xanthomata, xanthelasma and premature corneal arcus.
Tendon xanthomata are hard, painless nodules commonly found on the knuckles of the hands and in the Achilles tendons and rarely on the extensor hallucis longus and triceps tendons. The presence of tendon xanthomata, particularly over the Achilles tendon, is pathognomonic of FH.
Xanthelasma (Figure 1) are lipid-laden nodules on the eyelids whereas premature corneal arcus (Figure 2) are bluish rims surrounding the irises of the eyes.5
Investigations
Lipid profile
A lipid profile is a blood test that shows the serum levels of TC, non-HDL cholesterol, LDL-C, HDL-C and TG.
The TC/HDL ratio provides the best estimate of cardiovascular risk in a patient and is specifically used in the QRISK2 score to calculate the 10-year risk of developing myocardial infarction or stroke in a patient.
Current NICE guidelines do not recommend a fasting sample to test for lipid profile.6
Other investigations
Common secondary causes of hyperlipidaemia should be ruled out by ordering specific investigations as shown in the table below.7
Table 1. Investigations for secondary hyperlipidaemia.
|
Secondary cause of hyperlipidaemia |
Investigations |
|
Excess alcohol |
Liver function test to look for raised GGT |
|
Uncontrolled diabetes |
Fasting blood glucose, HbA1c both of which would be elevated |
|
Hypothyroidism |
Thyroid function test to look for raised TSH and low T4 and T3 |
|
Liver disease |
Liver function test to look for raised serum AST, ALT, ALP and bilirubin |
|
Nephrotic syndrome |
Urine dipstick to look for proteinuria Liver function test to look for hypoalbuminaemia |
|
Chronic kidney disease |
Renal function test to look for raised serum urea and creatinine |
Diagnosis
NICE recommends that a diagnosis of hyperlipidaemia be made based on clinical findings, lipid profile and family history rather than the use of strict lipid cut‑off values alone.
Familial hypercholesterolaemia should be diagnosed based on the Simon Broome diagnostic criteria or the Dutch Lipid Clinical Network (DLCN) criteria/score.8
Management
The management of hyperlipidaemia can be divided into conservative, medical and surgical and aims to reduce the risk of cardiovascular diseases due to long-term uncontrolled hyperlipidaemia.
Conservative management
All patients with hyperlipidaemia should be encouraged to adopt several lifestyle modifications:6
- Consume a diet low in saturated fats and cholesterol and high in fruits, vegetables, mono-and polyunsaturated fats
- Exercise for at least 150 minutes per week with at least 30 minutes per day
- Reduce alcohol intake to <14 units per week for both men and women and avoid binge drinking
- Stop smoking by enrolling on a smoking cessation programme
Medical management
Hyperlipidaemia due to secondary causes usually resolves following treatment of the underlying condition.
Lipid-lowering drugs play a key role in treating primary lipid disorders and for primary and secondary prevention of cardiovascular diseases.
Table 2. Examples of lipid-lowering drugs and their mechanism of action are shown in the table below.9
|
Lipid-lowering drugs |
Examples |
Mechanism of action |
Indication |
|
HMG-CoA reductase inhibitors (statins) |
Atorvastatin, simvastatin |
Inhibit conversion of HMG-CoA to mevalonic acid, a cholesterol precursor |
First-line for hyperlipidaemia, primary and secondary prevention of cardiovascular diseases |
|
Bile acid sequestrants |
Cholestyramine |
Prevents intestinal absorption of bile acids |
Considered if statins and ezetimibe are contraindicated |
|
Ezetimibe |
– |
Prevents intestinal absorption of cholesterol |
Second-line if statins are contraindicated or as an addition to initial statin therapy for poorly-controlled hyperlipidaemia |
|
Fibrates |
Gemfibrozil, fenofibrate |
Activates PPAR-𝛂 to increase triglyceride clearance and increase HDL-C synthesis |
Considered if statins and ezetimibe are contraindicated |
|
Niacin |
– |
Inhibits lipolysis |
Considered if statins and ezetimibe are contraindicated |
|
PCSK9 inhibitors |
Alirocumab, evolocumab |
Inactivation of LDL-receptor degradation, hence increases LDL clearance from the blood |
For poorly controlled hyperlipidaemia despite maximal tolerated lipid-lowering therapy |
For patients with FH or uncontrolled hyperlipidaemia despite the maximum amount of drug treatment and lifestyle modifications, LDL apheresis can be considered. This is a type of dialysis treatment that removes LDL-C from the blood.8
Surgical management
Liver transplantation can be considered for patients with homozygous FH with no significant improvement following treatment with lipid-modifying therapy and LDL apheresis.8
Complications
If hyperlipidaemia is not diagnosed and treated early, major atherosclerotic complications can occur including:5
- Ischaemic heart disease
- Acute coronary syndrome
- Peripheral vascular disease
- Stroke
- Erectile dysfunction
- Mesenteric ischaemia
Complications of lipid-lowering drugs
Complications may also occur due to adverse drug reaction (ADR) of lipid-lowering drugs, particularly statins and fibrates.
The most severe form is rhabdomyolysis, a condition in which there is a breakdown of myocytes causing a release of myoglobin and creatinine kinase into the bloodstream. If not treated early, this can lead to renal and multiorgan failure and eventually, death.
Patients with rhabdomyolysis typically present with muscle pain and dark urine. A raised serum creatinine kinase at least 5 times the upper limit of normal is diagnostic.10
Key points
- Hyperlipidaemia is a condition involving elevated levels of one or more of TC, LDL-C and TG in the blood.
- FH is the most common primary hyperlipidaemia and can be diagnosed based on the Simon Broome diagnostic criteria or the Dutch Lipid Clinical Network (DLCN) criteria/score.
- Key clinical features of hyperlipidaemia include tendon xanthomata, particularly in FH, xanthelasma and corneal arcus.
- A non-fasting lipid profile is the main investigation to diagnose hyperlipidaemia.
- Secondary and reversible causes of hyperlipidaemia must be ruled out and treated before making a diagnosis of and managing primary hyperlipidaemia.
- Lipid-lowering therapy is the mainstay treatment for hyperlipidaemia. LDL apheresis and liver transplantation can be considered in patients with no significant improvement following lipid-lowering therapy.
- Complications of untreated hyperlipidaemia include major atherosclerotic and cardiovascular complications.
- Rhabdomyolysis is a severe adverse drug reaction of statins and fibrates which can lead to renal failure and death if not treated early.
Reviewer
Dr Sarah Lontac Nufable
BSBio, MD, DPCGGI, FPCGM, PGCMedEd(UK), FHEA(UK)
Associate Professor, Assistant Dean of Academic Affairs (MBBS), Newcastle University Medicine Malaysia
Editor
Dr Chris Jefferies
References
- Dr Rajeer Srivastava. Synopsis of causation: Hyperlipidaemia. Published in September 2008. Available from: [LINK]
- National Institute for Care and Excellence (NICE). Draft scope for the appraisal of evolocumab for treating primary hypercholesterolaemia and mixed dyslipidaemia. Published in May 2015. Available from: [LINK]
- National Institute for Care and Excellence Clinical Knowledge Summaries (NICE CKS). Hypercholesterolaemia – familial. Published on September 2020. Available from: [LINK]
- Ralston, S. H., Penman, I. D., Strachan, M. W. J., & Hobson, R. Davidson’s principles and practice of medicine (23rd edition). Published in 2018.
- BMJ Best Practice. Hypercholesterolaemia. Published in April 2021.
- National Institute for Care and Excellence (NICE). Cardiovascular disease: risk assessment and reduction, including lipid modification. Published on 18 July 2014. Available from: [LINK]
- Dr Colin Tidy. Published on 11 June 2021. Available from: [LINK]
- National Institute for Care and Excellence (NICE). Familial hypercholesterolaemia: identification and management. Published on 27 August 2008. Available from: [LINK]
- Dale, M. M., Rang, H. P. and Dale, M. M. Rang and Dale’s pharmacology (9th edition). Published in 2020.
- BMJ Best Practice. Rhabdomyolysis. Published in November 2019.