- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
This guide provides a step-by-step approach to examining a pigmented skin lesion in an OSCE setting.
You may also be interested in our guide to examining rashes and non-pigmented skin lesions and our guide to dermatological history taking.
Introduction
Wash your hands and don PPE if appropriate.
Introduce yourself to the patient including your name and role.
Confirm the patient’s name and date of birth.
Briefly explain what the examination will involve using patient-friendly language.
Explain the need for a chaperone if the skin lesion is located in an intimate area: “One of the ward staff members will be present throughout the examination, acting as a chaperone, would that be ok?”
Gain consent to proceed with the examination.
Adequately expose the skin lesion and position the patient so that you can clearly visualise it.
Ask the patient if they have any pain before proceeding with the clinical examination.
General inspection
Skin lesions
Note the number, location and distribution of the patient’s skin lesions from the end of the bed.
Number of lesions
Lesion assessment typically involves the examination of a single lesion, however, there may be multiple lesions on a patient.
If there is a single lesion, state this. If there are multiple, it is good practice to verbalise you have noticed the surrounding skin and picked out the relevant lesion for further examination or comment.
- “I can see this patient has numerous pigmented lesions on their back, but the lesion on the mid-upper back stands out for further inspection.”
Location
Make a mental note of exactly where the lesion(s) is/are to describe the/their location accurately when presenting your findings. This can be practised by describing a location to a friend and seeing if they locate it correctly on a basic outline of a person.
Distribution
Note the distribution of the lesion(s):
- Acral distribution: distal areas including the hands and feet (e.g. hand, foot and mouth disease)
- Central distribution: over chest and back (photo-protected)
- Peripheral distribution: over arms and legs (more sun-exposed)
- Sun-exposed (photo) distribution: areas of high sun exposure will have a higher incidence of lesions caused by chronic sun damage (face, ears, nose, arms, lower legs). These areas are more likely to present with worrying pigmented lesions later in life. Young people are more likely to have new, worrying pigmented lesions in minimally photo-damaged areas.
Objects and equipment
Look for objects or equipment on or around the patient that may provide useful insights into their medical history and current clinical status:
- Medical equipment: may include bandages/dressings, oral medications and topical medications.
- Mobility aids: items such as wheelchairs and walking aids give an indication of the patient’s current mobility status.
- Prescriptions: prescribing charts or personal prescriptions can provide useful information about the patient’s recent medications.
Close inspection of lesion(s) – ABCDE assessment
ABCDE of pigmented lesions
When assessing a pigmented (melanocytic) lesion, it is important to assess the risk of the lesions through the ABCDE criteria and communicate this to the examiner in your summary.
Asymmetry
Asymmetry of a lesion typically refers to networks, patterns, markings, colours or features that are not regularly distributed through the entire lesion.
An example would be a pepperoni pizza with pepperoni on only one quarter.
Border
Benign lesions typically have a smooth and regular border.
If an irregular border is present (e.g. streaks, wavy edge) this increases the likelihood of malignancy.
Colour
Benign lesions typically demonstrate uniform colour throughout.
The presence of more than 2 colours increases the likelihood of malignancy.
The types of colours too are notable – describe the colours as you see them and keep it simple (e.g. light brown, mid-brown, dark brown).
Colours within pigmented lesions such as pinks, blues, greys, whites or deep blacks increase the likelihood of malignancy.
Diameter
A lesion with a diameter of 6mm or more increases the likelihood of malignancy.
Evolution
A history of abnormal evolution of the lesion is one of the most concerning risk factors for potential malignancy.
Lesions that are growing quickly and/or changing in appearance over a short time period are highly concerning for malignancy.
Clues to this may be within the vignette (e.g. “Please examine this patient with a new lesion, first noticed 6 weeks ago on the right upper back.”).
Elevation of a pigmented lesion
Elevation within a pigmented lesion is not a hard sign of malignancy and can confuse matters. Most melanomas are flat or macular (i.e. superficial spreading malignant melanomas) and only lesions that are nodular, or later stage, are elevated. Most pigmented lesions are papules or nodules and are usually benign melanocytic naevi (moles).
Lesions which should not be confused with melanoma
When assessing a pigmented lesion, it is always useful to understand if the lesion is truly pigmented (melanocytic) or just darker/thickened skin.
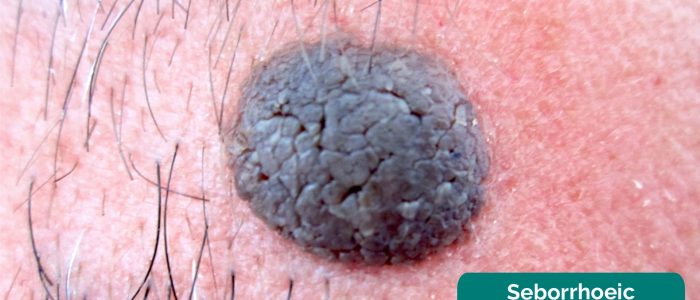
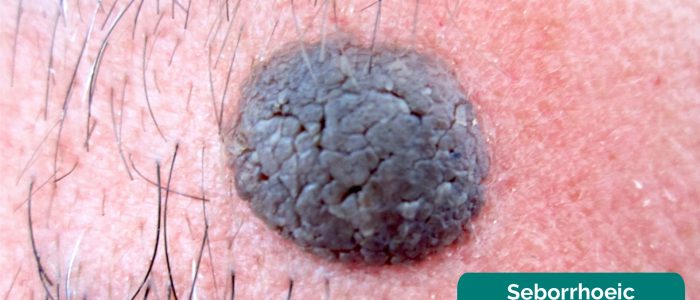
A common and wholly benign class of lesion that can score highly on the ABCDE criteria are seborrhoeic keratoses (a.k.a seborrhoeic warts). These have very specific findings which will reassure you when present, and increase your index of suspicion for malignancy if absent. These include:
- Stuck-on appearance: seborrhoeic keratoses look like they have been stuck to the top of the skin. These would be described as a stuck-on papule, nodule, or plaque.
- Cerebriform pattern: cerebriform, or brain-like, describes the gyri and sulci of the stuck-on plaque or nodule. It can also be described as a fingerprint pattern.
- Pseudo-comedones: these are blackhead-like structures within the keratosis. They are not true comedones but resemble them.
- Keratin pearls: these go hand in hand with pseudo-comedones and are small, pale, round structures that dot a keratosis.
- Shiny or wart-like: seborrhoeic means “greasy”. This refers to the smoother, more shiny keratoses. They are exactly the same underlying pathology as the more wart-like lesions which are dull and have a rough, warty or verruciform structure.
Types of pigmented lesions
These are the main types of pigmented lesions and their malignant potential:
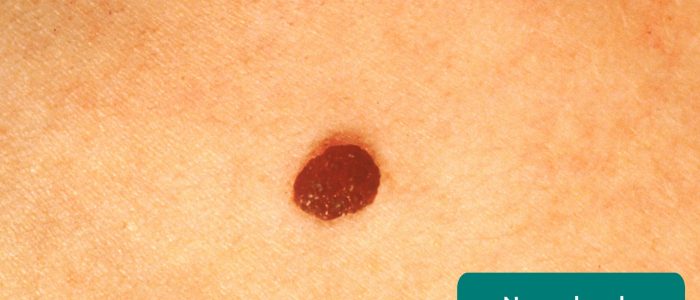
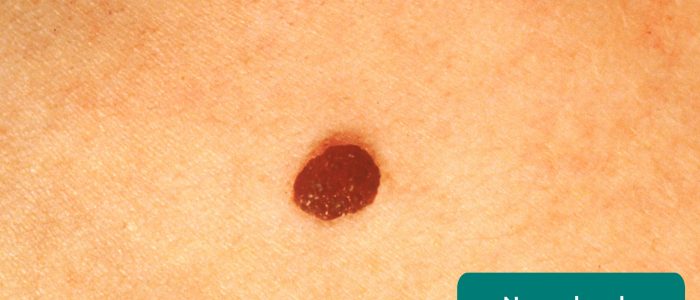
- Melanocytic naevus (“mole”): benign – a collection of a high number of melanocytes along the dermo-epidermal junction. Early lesions are usually flat, macular lesions.
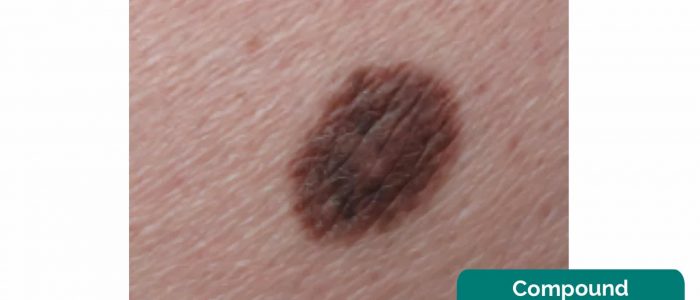
- Compound melanocytic naevus: benign – raised melanocytic naevus which is palpable and soft. Many flat naevi mature into raised, compound naevi over time.
- Dysplastic naevus: benign but with histologically concerning features – usually presents clinically with a suspicious naevus which scores on the ABCDE criteria. Some abnormal melanocytes but in a normal naevus pattern.
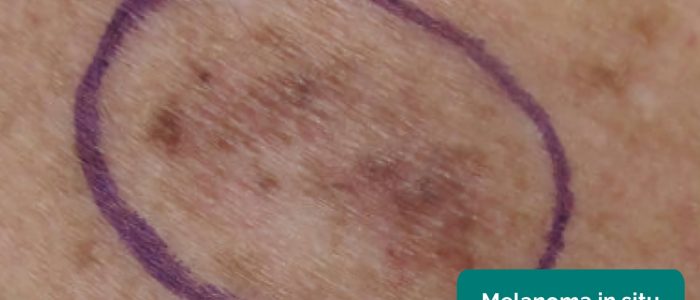
- Melanoma in situ: malignant (in situ) – malignant melanocytic cells but none that have crossed the basement membrane.
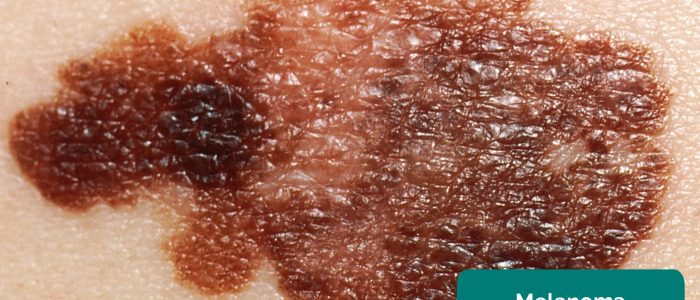
- Superficial spreading malignant melanoma: malignant – abnormal and malignant nests of melanocytes that have crossed the basement membrane and are in a horizontal growth phase
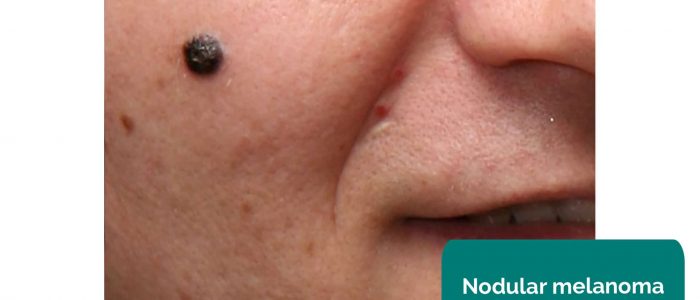
- Nodular melanoma: malignant (aggressive) – abnormal and malignant nests of melanocytes with high growth rate, with vertical growth.
- (Solar) Lentigo: benign – a macular “sunspot” – higher number of benign melanocytes on a sun-exposed or photo-damaged area.
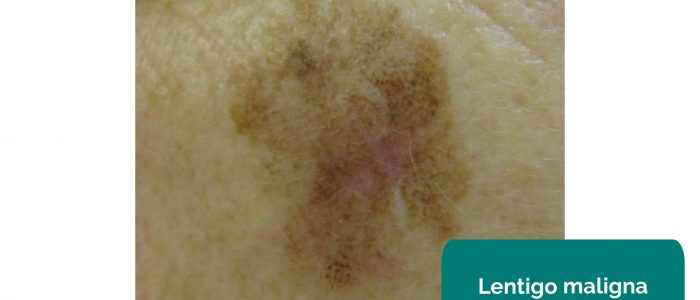
- Lentigo maligna: malignant (in situ) – an area of melanoma in situ within a lentigo.
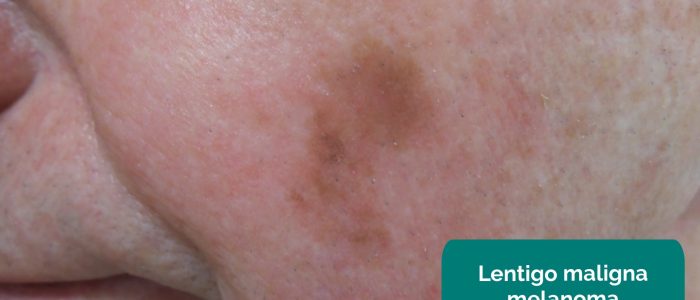
- Lentigo maligna melanoma: malignant – abnormal and malignant nests of melanocytes within a lentigo.
Rare types of malignant melanoma
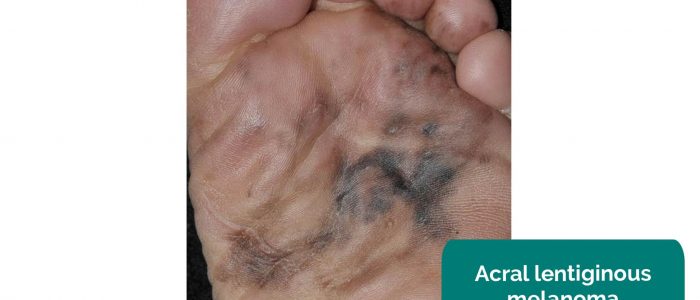
- Acral-lentiginous melanoma: melanoma of the acral skin (hands and feet). These are difficult to categorise as benign or malignant clinically, so it is best practice to inspect further with a dermatoscope.
- Subungual melanoma: a form of acral-lentiginous melanoma starting at the nail fold or nail bed in the fingers or toes. This gives the worrying Hutchinson’s sign (pigmented nail starting at the proximal nail fold and extending to the distal nail or lateral nail fold).
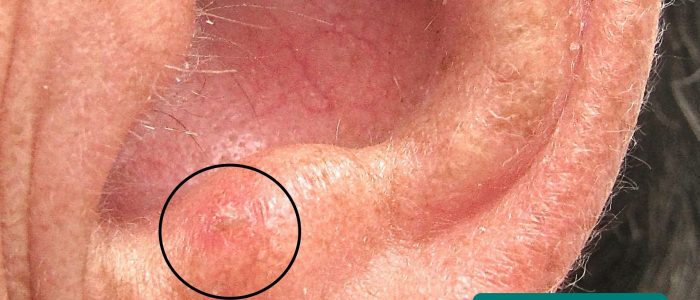
- Amelanotic melanoma: a difficult-to-diagnose subtype of melanoma with few if any signs clinically of pigment. These lesions are aggressive, pink-white in colour and may have been pigmented originally.
Final steps
If you identify a skin lesion that may be malignant you should perform a comprehensive assessment (full skin check) for other suspicious lesions.
Palpation
Don gloves if there is a risk that the skin lesion is infective and/or is likely to expose you to bodily fluids (e.g. blood/pus).
Assess the surface characteristics of the lesion:
- Texture: note if the lesion feels smooth (e.g. benign naevus, seborrhoeic keratosis) or rough (e.g. warty seborrhoeic keratosis or actinic keratosis).
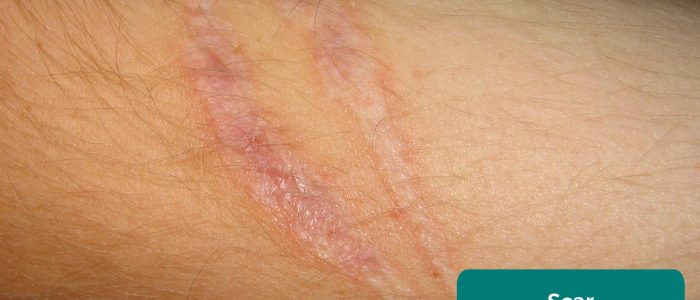
- Elevation: note if the lesion is flat (e.g. ecchymoses), raised (e.g. keratoacanthoma) or depressed (e.g. hypotrophic scar).
- Crust: if present, assess if you can remove the crust and inspect the underlying tissue (e.g. psoriasis).
Examine the regional lymph nodes if a suspicious lesion is identified.
‘Wobble sign’
A ‘soft’ sign of benignity in a lesion, the ‘wobble sign’ is positive if when viewing the lesion with a dermatoscope, the lesion is soft and can wobble from side to side. This usually denotes it being a benign intradermal naevus which is soft and fleshy.
To complete the examination…
Explain to the patient that the examination is now finished and provide them with privacy to get dressed if relevant.
Thank the patient for their time.
Dispose of PPE appropriately and wash your hands.
Summarise your findings.
Further assessments and investigations
Suggest further assessments and investigations to the examiner:
- Perform relevant examinations of any systems that may be related to dermatological findings (e.g. local lymph node assessment).
- Swabs/skin scrapings of lesions: for microbiology, virology and fungal culture.
- Dermatoscopy of lesions: to more accurately assess a skin lesion (particularly melanocytic or vascular lesions).
- Photography of lesions: a standard of 3 images to help with care and documentation – locating image (shown on the body the lesion is), macro image (close-up image), and dermoscopic image with cross-polarised light (to show dermoscopic features).
- Perform a biopsy of the skin lesion: for histological analysis – a 2mm peripheral margin with a cuff of fat is needed, with further wide local excision after pathological staging. Never partially excise a concerning melanocytic lesion.
References
Text references
- British Association of Dermatologists. Handbook for Medical Students and Junior Doctors. Published in 2014.
- Dermnet New Zealand. Dermatology terminology. Published in 1997. Revised in 2017.
- NICE Clinical Knowledge Summaries. Melanoma and pigmented lesions. Revised March 2011.
Image references
- Делфина. Adapted by Geeky Medics. Seborrhoeic keratosis. Licence: CC BY-SA.
- Dermanonymous. Adapted by Geeky medics. Compound naevus. Licence: CC BY-SA 4.0
- Dermanonymous. Adapted by Geeky medics. Melanoma in situ. Licence: CC BY-SA 4.0
- Juliana Casagrande Tavoloni Braga, Mariana Petaccia Macedo, Clovis Pinto, João Duprat, MariaDirlei Begnami, Giovanni Pellacani, Gisele Gargantini Rezze. Superficial spreading melanoma. Adapted by Geeky Medics. Licence: CC BY 4.0
- 0x6adb015. Adapted by Geeky Medics. Nodular melanoma. Licence: CC BY-SA 4.0
- Kilbad. Adapted by Geeky Medics. Lentigo maligna. Licence: CC BY 3.0
- Omar Bari, Philip R. Cohen. Adapted by Geeky Medics. Lentigo maligna melanoma. Licence: CC BY 3.0
- Xavier-Júnior, José & Munhoz, Tania & Souza, Vinicius & Campos, Eloísa & Stolf, Hamilton & Marques, Mariângela. Adapted by Geeky Medics. Acral lentiginous melanoma. Licence: CC BY 4.0
- Future FamDoc. Adapted by Geeky Medics. Actinic keratosis. Licence: CC BY-SA.
- Jmarchn. Adapted by Geeky Medics. Keratocanthoma. Licence: CC BY-SA.
- Svdmolen. Adapted by Geeky Medics. Scar. Licence: CC BY-SA.
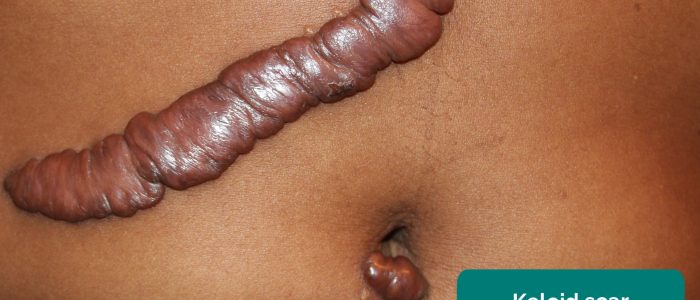
- Htirgan. Adapted by Geeky Medics. Keloid scar. Licence: CC BY-SA.
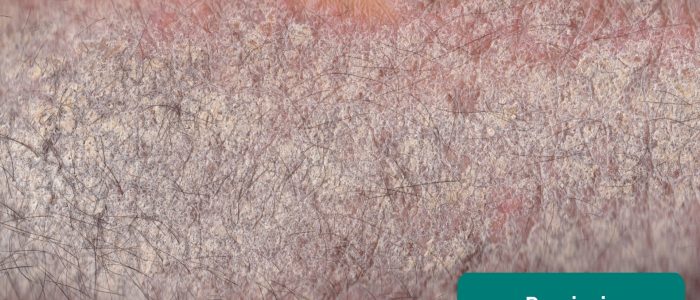
- MediaJet. Adapted by Geeky Medics. Psoriasis. Licence: CC BY-SA.