- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Blind spot assessment occasionally features in OSCEs. This guide provides a step-by-step approach to assessing a patient’s blind spot. It also includes a video demonstration.
Background
A physiological blind spot exists in all healthy individuals due to the lack of photoreceptor cells in the area where the optic nerve emerges through to the retinal plane (optic nerve head / optic disc). In day-to-day life, the brain does an excellent job of reducing our awareness of the blind spot by using information from other areas of the retina and the other eye to mask the defect.
Introduction
Wash your hands and don PPE if appropriate.
Introduce yourself to the patient including your name and role.
Confirm the patient’s name and date of birth.
Briefly explain what the examination will involve using patient-friendly language.
Gain consent to proceed with the examination.
Position the patient sitting on a chair.
Ask if the patient has any pain before proceeding.
Blind spot assessment
1. Sit directly opposite the patient, at a distance of around 1 metre.
2. Ask the patient to cover one eye with their hand.
3. If the patient covers their right eye, you should cover your left eye (mirroring the patient).
4. Ask the patient to focus on part of your face (e.g. nose) and not move their head or eyes during the assessment. You should do the same and focus your gaze on the patient’s face.
5. Using a red hatpin (or alternatively, a cotton bud stained with fluorescein/pen with a red base) start by identifying and assessing the patient’s blind spot in comparison to the size of your own. The red hatpin needs to be positioned at an equal distance between you and the patient for this to work.
6. Ask the patient to say when the red part of the hatpin disappears, whilst continuing to focus on the same point on your face.
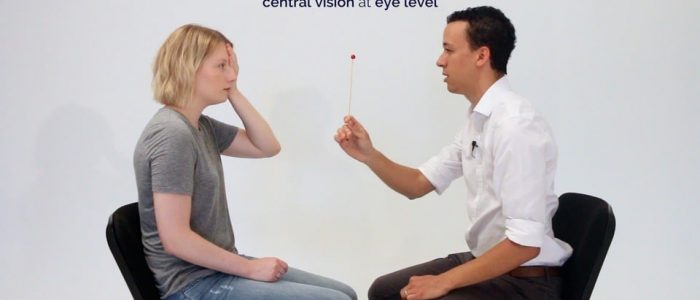
7. With the red hatpin positioned equidistant between you and the patient, slowly move it laterally until the patient reports the disappearance of the top of the hatpin. The blind spot is normally found just temporal (lateral) to central vision at eye level. The disappearance of the hatpin should occur at a similar point for you and the patient.
8. After the hatpin has disappeared for the patient, continue to move it laterally and ask the patient to let you know when they can see it again. The point at which the patient reports the hatpin re-appearing should be similar to the point at which it re-appears for you (presuming the patient and you have a normal blind spot).
9. You can further assess the superior and inferior borders of the blind spot using the same process.
Causes of an enlarged blind spot
An enlarged blind spot is typically associated with a swollen optic nerve head.
Papilloedema is a bilaterally swollen optic nerve head secondary to raised intracranial pressure (e.g. brain tumour, hypertensive crisis, intracranial haemorrhage). Other causes of optic nerve head swelling (papillitis) must be excluded before making this diagnosis.
To complete the examination…
Explain to the patient that the examination is now finished.
Thank the patient for their time.
If mydriatic drops were instilled, remind the patient they cannot drive for the next 3-4 hours until their vision has returned to normal.
Dispose of PPE appropriately and wash your hands.
Summarise your findings
Suggest further assessment and investigations
All of the following further assessments and investigations are dependent on the patient’s presenting complaint and in most cases, none of them would need to be performed:
- Examination of the eyes and vision: to assess for other causes of an enlarged blind spot
- Cranial nerve examination: to further assess for evidence of cranial nerve pathology. It is especially important to rule out an abducens nerve palsy as this may be present in individuals with raised intracranial pressure.
- Retinal photography: to better visualise any abnormalities noted on fundoscopy.
- Optical Coherence Tomography (OCT): measures the thickness of the retinal nerve fibre layer in microns. Used for baseline assessment and monitoring of optic nerve head swelling.