- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Introduction
Cushing’s syndrome occurs because of prolonged exposure to elevated levels of either endogenous or exogenous glucocorticoids.
The condition is associated with significant morbidity and mortality, therefore rapid diagnosis, and management is essential.1
Aetiology
Pathophysiology
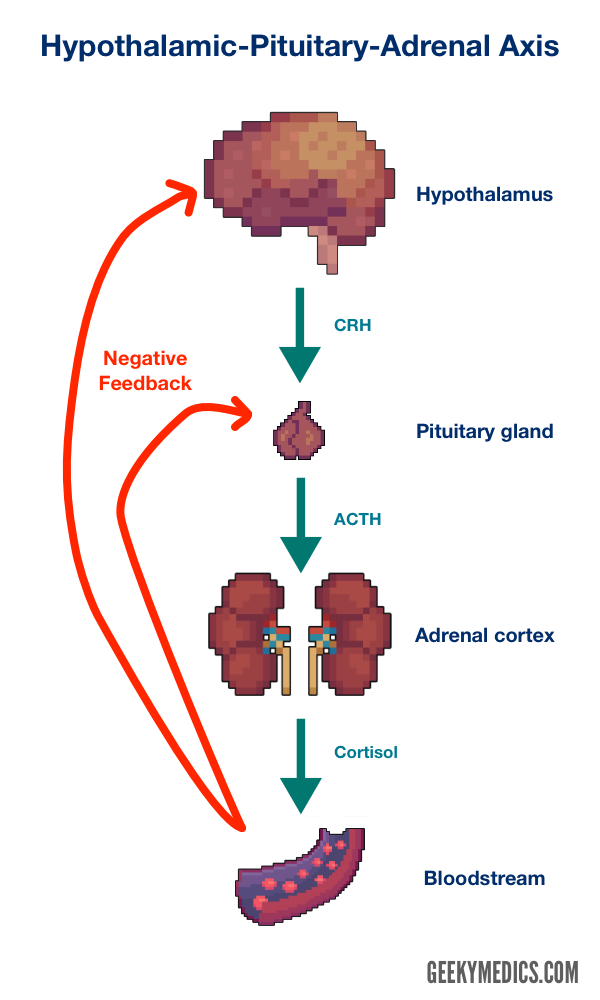
Glucocorticoid production is regulated by the hypothalamic-pituitary-adrenal axis (Figure 1):
- Corticotropin-releasing hormone (CRH) is secreted from the hypothalamus. This release is influenced by stress levels, time of day and serum cortisol levels.
- CRH travels in the blood and binds to specific receptors in the pituitary gland. This binding causes increased production of adrenocorticotropic hormone (ACTH).
- ACTH is released into the bloodstream and travels to the adrenal glands, where it binds to specific receptors on the adrenal cortex.
- This binding of ACTH to the receptors stimulates the adrenal cortex to release cortisol into the bloodstream, where it has a wide range of effects (see below).
- Increased serum cortisol levels inhibit the production of CRH and ACTH via negative feedback, preventing the overproduction of cortisol.
The functions of cortisol include:
- The synthesis of glucose from non-carbohydrate sources (known as gluconeogenesis), resulting in increased levels of glucose in the blood.
- Promoting the breakdown of proteins, which can result in muscle wasting in chronic states of cortisol elevation.
- An initial surge in cortisol levels triggers lipolysis, however, chronically elevated cortisol promotes lipogenesis.
- Inhibition of the production of several inflammatory cytokines causing downregulation of the immune response.
- Reduction in bone formation (chronically elevated levels of cortisol can result in osteoporosis).
In high concentrations, cortisol exhibits mineralocorticoid effects, increasing sodium and water retention whilst increasing potassium excretion.
Causes of Cushing’s syndrome
Exogenous
The most common cause of Cushing’s syndrome is the use of exogenous glucocorticoids (e.g. prednisolone, hydrocortisone).
Endogenous
Endogenous Cushing’s syndrome can be further sub-categorised as either corticotropin-dependent or corticotropin-independent.
Corticotropin-dependent Cushing’s syndrome accounts for 80-85% of cases.2
Pituitary adenomas account for 80% of corticotropin-dependent Cushing’s syndrome (known as Cushing’s disease).
Ectopic production of corticotropin (e.g. small cell lung cancer) accounts for around 20% of corticotropin-dependent Cushing’s syndrome. 2
The most common causes of corticotropin-independent Cushing’s syndrome are adrenal adenomas and adrenal carcinomas.2
Clinical features
History
Typical symptoms of Cushing’s syndrome include:
- Weakness
- Facial fullness
- Weight gain
- Low mood
- Decreased libido
- Polydipsia
- Polyuria
- Increased frequency of infections
Clinical examination
Typical clinical findings in Cushing’s syndrome include:
- Truncal obesity
- Buffalo hump
- Supraclavicular fat pads
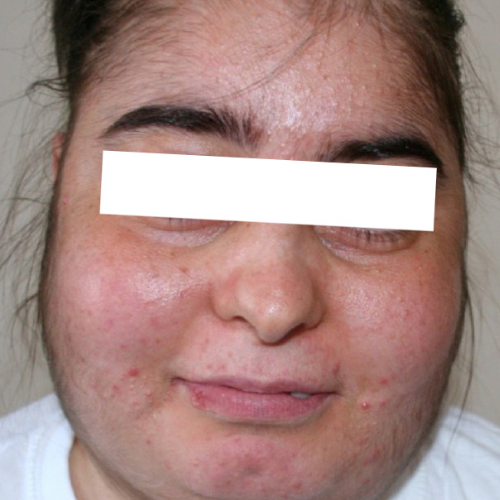
- Moon facies
- Proximal muscle wasting
- Hypertension
- Oedema
- Headaches, visual field defects and galactorrhoea (in Cushing’s disease)
Investigations
Laboratory investigations
Relevant laboratory investigations include:
- Full blood count (white cell count may be raised due to glucocorticoid effects)
- Urea and electrolytes (hypokalemia, hypernatraemia)
Confirming the diagnosis of Cushing’s syndrome
Several investigations are typically required to accurately diagnose a patient with Cushing’s syndrome.
24-hour urinary free cortisol
Cortisol excretion of more than three times the upper limit of normal is strongly suggestive of Cushing’s syndrome.
Low-dose dexamethasone suppression test
This test is particularly useful when screening patients for Cushing’s syndrome, as it is less cumbersome than a 24-hour urinary free cortisol collection.
1mg of dexamethasone is administered at 11pm and then serum cortisol is measured at 8am the following morning.
If a patient has only mild Cushing’s syndrome, it may not be detected using this test alone.
Late-night salivary cortisol measurement
This simple and reliable test relies on the fact that in healthy individuals, the level of cortisol decreases in the evening compared to the morning.4
In the case of Cushing’s syndrome, this normal diurnal variation is absent.
Identifying the underlying cause
Plasma ACTH
Levels of ACTH have a diurnal variation, with the plasma concentration being highest at 8am and lowest at midnight.
An elevated ACTH level alongside a raised serum cortisol level suggests a diagnosis of ACTH-dependent Cushing’s syndrome (see causes above).4
An undetectable ACTH level alongside a raised serum cortisol level suggests a diagnosis of ACTH-independent Cushing’s syndrome (see causes above).5
High-dose dexamethasone suppression test
This test is indicated if ACTH levels are detectable.
The test is useful for differentiating between pituitary and ectopic ACTH production.
A reduction of basal urinary free cortisol of greater than 90% supports a diagnosis of a pituitary adenoma (ectopic ACTH causes less suppression).
Inferior petrosal sinus sampling
Inferior petrosal sinus sampling (IPSS) is an invasive procedure in which ACTH levels are sampled from veins that drain the pituitary gland.
These ACTH levels are compared with peripheral ACTH levels to determine whether a pituitary tumour is responsible for ACTH-dependent Cushing’s syndrome.
This method is used when neuroimaging along with the previous investigations has been insufficient to reach a diagnosis (e.g. no visible lesion on neuroimaging of the pituitary).
Imaging
Relevant imaging investigations include:
- MRI of the pituitary: to confirm the presence of an adenoma
- CT chest and abdomen: to identify suspected adrenal tumours or other sources of ectopic ACTH production
Management
Exogenous Cushing’s syndrome
Management of exogenous Cushing’s syndrome involves reviewing the patient’s current glucocorticoid treatments and reducing doses where possible (often with steroid-sparing immunosuppressive agents).
Endogenous Cushing’s syndrome
Definitive treatment of endogenous Cushing’s syndrome typically involves resection of the causative tumour, however, medical therapies to reduce cortisol production are often used in the interim period to stabilise the patient prior to definitive therapy.6
Medical management
Ketoconazole, metyrapone and mitotane all directly inhibit glucocorticoid synthesis and secretion in the adrenal gland.7
As a result, these medications can be used to temporarily reduce glucocorticoid levels to help prepare the patient for definitive therapy.
In some cases, these medications can be used long-term for patients who are too unfit to undergo definitive surgical management.
Surgical management
Surgical management differs depending on the site of ectopic cortisol production:
- Adrenal tumours (e.g. adrenal adenoma): laparoscopic excision
- Pituitary tumours: trans-sphenoidal surgery (may also require adjunct radiotherapy)
Complications
Complications of Cushing’s syndrome include:
- Hypertension
- Diabetes
- Obesity
- Metabolic syndrome
- Osteoporosis
Key points
- Cushing’s syndrome occurs because of prolonged exposure to elevated levels of either endogenous or exogenous glucocorticoids.
- The most common cause of Cushing’s syndrome is the use of exogenous glucocorticoids (e.g. prednisolone, hydrocortisone).
- Typical symptoms of Cushing’s syndrome include weakness, facial fullness, weight gain, low mood, decreased libido, polydipsia, polyuria and increased frequency of infections.
- Typical clinical signs of Cushing’s syndrome include truncal obesity, buffalo hump, moon facies, proximal muscle wasting, hypertension and oedema.
- There is a range of investigations that can be used to confirm a diagnosis of Cushing’s syndrome such as the low-dose dexamethasone suppression test. Further investigations can be performed to identify the underlying cause of Cushing’s syndrome (e.g. imaging, serum ACTH, inferior petrosal sinus sampling).
- Management of exogenous Cushing’s syndrome involves reviewing the patient’s current glucocorticoid treatments and reducing doses where possible.
- Definitive treatment of endogenous Cushing’s syndrome typically involves resection of the causative tumour, however medical therapies to reduce cortisol production are often used in the interim period to stabilise the patient prior to definitive therapy.
- Complications of Cushing’s syndrome include hypertension, diabetes, obesity, metabolic syndrome and osteoporosis.
References
- Biller BM, Grossman AB, Stewart PM, et al; Treatment of ACTH-dependent Cushing’s syndrome: a consensus statement. J Clin Endocrinol Metab. 2008 Apr 15. Available from: [LINK]
- Dr Roger Henderson. Patient.info. Cushing’s syndrome. Edited July 2015. Available from: [LINK]
- Boscaro M, Arnaldi G; Approach to the patient with possible Cushing’s syndrome. J Clin Endocrinol Metab. 2009 Sep94(9):3121-31. Available from: [LINK].
- Pecori Giraldi F, Invitti C, Cavagnini F; The corticotropin-releasing hormone test in the diagnosis of ACTH-dependent Cushing’s syndrome: a reappraisal. Clin Endocrinol (Oxf). 2001 May 54(5):601-7. Available from: [LINK]
- Stratakis CA; Cushing syndrome caused by adrenocortical tumours and hyperplasias (corticotropin- independent Cushing syndrome). Endocr Dev. 200813:117-32. doi: 10.1159/000134829. Available from: [LINK]
- Shalet S, Mukherjee A; Pharmacological treatment of hypercortisolism. Curr Opin Endocrinol Diabetes Obes. 2008 Jun15(3):234-8. Available from: [LINK]
- Newell-Price J, Bertagna X, Grossman AB, et al; Cushing’s syndrome. Lancet. 2006 May 13367(9522):1605-17. Available from: [LINK].
Image references
Figure 1. GeekyMedics. Hypothalamic-Pituitary-Adrenal axis diagram.
Figure 2. Moon Facies. Ozlem Celik, Mutlu Niyazoglu, Hikmet Soylu and Pinar Kadioglu. License: [CC BY]. Available from: [LINK]
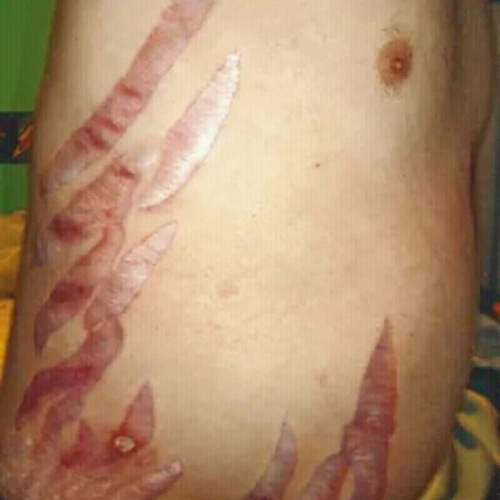
Figure 3. Striae. Masry. License: [CC BY-SA]. Available from: [LINK]