- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Introduction
Leg ulcers are common in clinical practice and OSCEs and can occur in various forms. It is important to be able to clinically differentiate different types of ulcers, as this guides investigations and subsequent management.
This article provides an overview of the pathophysiology, clinical features, investigations, and management of different types of ulcers.
Assessment of leg ulcers
When assessing ulcers in clinical practice or an OSCE scenario, key steps include:1,2
- Asking about the symptoms experienced (onset, progression, and severity)
- Identifying risk factors, such as immobility and a history of deep vein thrombosis
- Examining the wound (site, edge, size, depth, wound bed, and look for signs of infection)
- Examining both legs (for oedema, varicose veins, venous skin changes, peripheral neuropathy and reduced ankle mobility)
- Assessing for other causes of ulceration and/or delayed wound healing
- Measuring the ankle-brachial pressure index in both legs to exclude arterial insufficiency
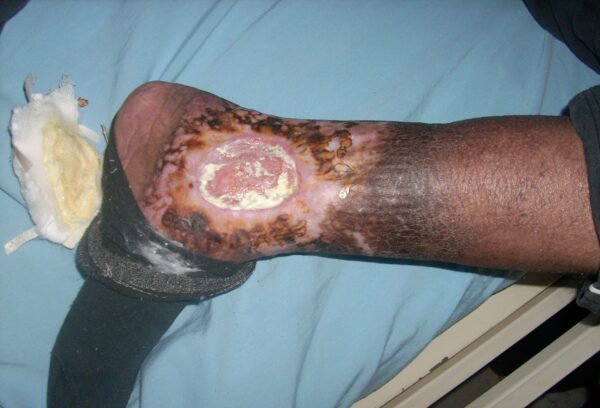
Arterial ulcers
Arterial ulcers, also known as ischemic or arterial insufficiency ulcers, stem from inadequate blood supply to the extremities.
The primary culprit is atherosclerosis, leading to arterial narrowing and compromised blood flow. This diminished perfusion deprives tissues of oxygen and nutrients, resulting in tissue damage and ulceration.1,3
Clinical features
Location: Arterial ulcers predominantly occur on the lower extremities near end-arteries, particularly the toes, heels, and lateral malleolus.
Pain: Patients frequently endure severe, resting pain due to ischemia. Painful, especially at night, and worse when legs are elevated.
Appearance and features:
- Arterial ulcers often appear pale, dry, and gangrenous, with cool surrounding skin
- These ulcers are sharply defined and have a deep ‘punched-out’ appearance
- Loss of hair on surrounding skin (shiny appearance)
Pulses: Diminished or absent pulses, especially in the affected limb, are a hallmark sign.
Investigations
Relevant investigations for arterial ulcers include:
- Doppler ultrasound: this non-invasive test assesses blood flow and identifies arterial stenosis.
- Ankle-Brachial Pressure Index (ABPI): measures the ratio of systolic blood pressure at the ankle to that in the arm. An ABPI <0.8 indicates arterial insufficiency.
- Angiography: invasive angiography may be necessary to visualize arterial anatomy and plan interventions.1
Management
The management of arterial ulcers comprises wound care and lifestyle modification to address the relevant risk factors contributing to arterial insufficiency and subsequent ulcer development in an individual.
Good analgesia to control ischaemic pain and lifestyle promotion, including encouraging smoking cessation, exercise, and control of comorbidities, are important first steps. Reducing blood lipid and sugar levels reduces the risk of further ulcer development.
Proper wound management of any existing ulcers is important, and dressings should maintain a moist wound environment. This may require input from tissue viability teams.
Caution
Compression bandaging and anti-embolism stockings are contraindicated if arterial ulcers are present, as this could further reduce distal blood flow.
Vascular reconstruction via surgical bypass or angioplasty procedures can restore blood flow and nutrient supply to the tissue to aid wound healing.
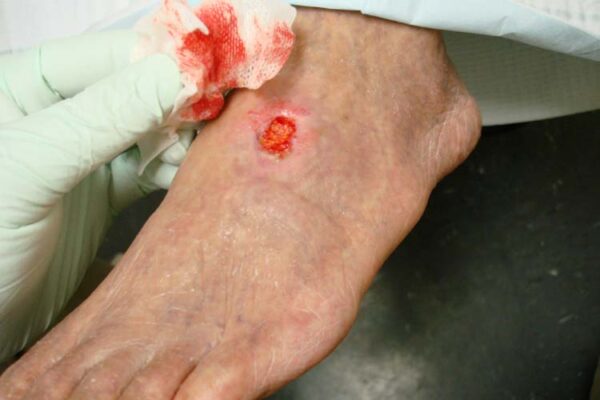
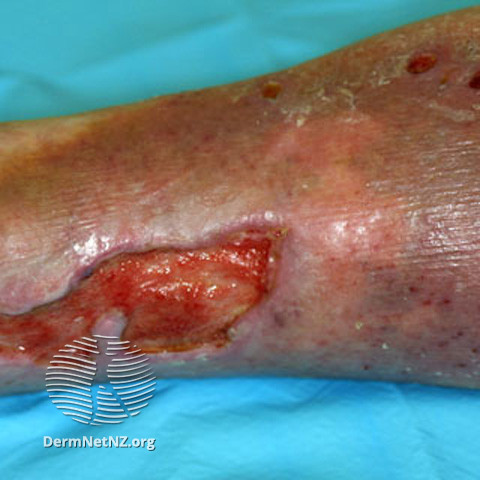
Venous ulcers
Venous ulcers arise from chronic venous insufficiency, resulting in increased venous pressure and impaired tissue oxygenation, triggering inflammation and tissue damage.
Chronic venous insufficiency (CVI) refers to functional changes that may occur in the lower extremities due to persistent elevation of venous pressures. This most commonly results from venous reflux due to faulty valve function developing as a long-term sequelae of deep vein thrombosis or varicose veins.1,3,4
Clinical features
Location: Venous ulcers typically form around the medial or lateral malleolus (more common over medial than lateral).
History of venous disease (e.g. varicose veins, deep vein thrombosis).
Pain: Patients often report aching or heaviness in the affected limb. Pain worsens with prolonged standing and improves with leg elevation.
Appearance and features:1
- Venous ulcers are usually shallow with irregular borders.
- Accompanied by oedema, erythema, and hemosiderin deposition in the surrounding skin (brown pigment).
- Lipodermatosclerosis, and atrophie blanche (white scarring with dilated capillaries)
- Skin is likely to be warm
Pulses: Pulses generally remain normal in venous ulcers.
Investigations
Relevant investigations for venous ulcers include:1
- Doppler ultrasound: to exclude underlying arterial disease and assess venous reflux.
- Venous duplex ultrasound: provides comprehensive information about venous anatomy and reflux.
- Venous pressure measurement: Invasive venous pressure measurement can confirm venous insufficiency, although this is rarely performed clinically
Management
Lifestyle modifications and health promotion are essential in the management of venous ulcers. Weight loss in most cases, regular exercise, and avoidance of prolonged standing or sitting can all help to improve venous sufficiency. Elevation of the legs will also support venous return, so patients should be encouraged to elevate their legs whenever possible.
In contrast to managing arterial ulcers, compression therapy is a mainstay in managing venous ulcers.
However, arterial insufficiency must be excluded before commencing compression bandaging. Compression therapy aids in the reduction of venous hypertension and promotes venous return. This needs to be maintained long-term.
Lastly, wound care for healing ulcers should be prioritised in these patients. Moist dressings facilitate wound healing. Non-viable tissue may necessitate debridement. Frequent use of emollients should be encouraged.2,5
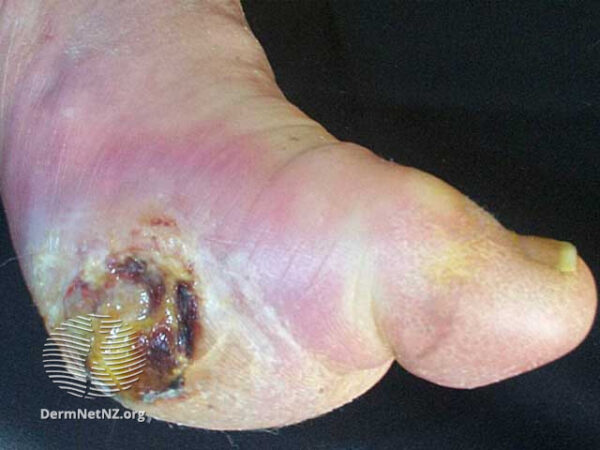
Neuropathic ulcers
Neuropathic ulcers, also referred to as diabetic foot ulcers, develop due to peripheral neuropathy and pressure-related trauma.
Patients with diabetes often experience neuropathy, which leads to reduced sensation in the affected areas. Repetitive pressure and friction can then cause tissue breakdown and ulcer formation.
Clinical features
Location: Neuropathic ulcers frequently appear on weight-bearing foot areas (e.g. plantar surface).
History: Patients usually have a history of diabetes or neurological disease
Pain: These ulcers are often painless due to sensory neuropathy. Patients may not notice the ulcer until it becomes severe.
Appearance and features:
- Variable size and depth. Surrounding skin may be warm, dry, and calloused.
- Typically occur in numb skin
Pulses: Pulses are usually present and normal in neuropathic ulcers, although they can be absent if there is concomitant arterial insufficiency.
Investigations
The diagnosis is primarily clinical, considering the patient’s history and physical examination findings. A neurological examination can assess sensory loss to confirm neuropathy.1
X-rays may be used to exclude osteomyelitis in chronic or non-healing ulcers.1
Management
Wound care is crucial to maintain a moist wound environment with appropriate dressings. Tissue viability nurses can support with dressing choice, and these patients may also be seen in a dedicated foot clinic.
Debridement may be necessary for callused tissue. In this patient population, offloading the legs or feet with specialised footwear or total contact casting is crucial to prevent further trauma and relieve pressure on the wound.
Glycaemic control and optimisation of diabetes management should be reviewed in these patients to slow the progression of neuropathy.1,3,8,9
Vasculitic ulcers
Vasculitic ulcers, often purpuric and punched out, stem from inflammation and damage to blood vessel walls.
Clinical features
Appearance: Purpuric, punched-out lesions. Biopsy shows vasculitis of medium-sized vessels.
Pain: Very painful and fast-evolving
Patients may have systemic signs of vasculitis, such as fever and joint pain.8
Infected ulcers
Infected ulcers occur when bacteria invade the wound, causing purulent discharge and potential systemic infection.
Clinical features
Patients may show signs of systemic infection (e.g. fever and malaise). 8
The ulcer may exhibit purulent discharge, erythema, warmth, and swelling. It is also accompanied by new onset or worsening pain.
Monitoring for infection
In any ulcer, it is important to monitor for infection and treat it promptly. Antibiotic courses may need to be prolonged to 10-14 days, and different types of dressings may be used in case of a wet ulcer.
Malignant ulcers
Malignant transformation can occur in long-standing non-healing ulcers, such as the development of squamous cell carcinoma.
Clinical features
Clinical features of malignant transformation include irregular border, rapid growth, friable, and contact bleeding.
A tissue biopsy is essential to confirm malignancy.8
Summary
In clinical practice, ulcers can exhibit a mixture of arterial, venous, and neuropathic components, making accurate diagnosis and management challenging.
ABPI results can aid in distinguishing these ulcers:
- Arterial ulcers typically have an ABPI <0.8, indicating arterial insufficiency
- Venous ulcers generally have an ABPI >0.8, reflecting normal arterial perfusion
- Neuropathic ulcers are typically associated with normal ABPI values
For vasculitic ulcers, infected ulcers, and malignant ulcers, ABPI results may vary, but the focus should be on clinical assessment, tissue biopsy (if malignancy is suspected), and appropriate investigations for vasculitis or infection.
|
|
Arterial ulcer | Venous ulcer | Neuropathic ulcer |
|
Aetiology |
Develop as a result of inadequate blood supply to the extremities |
Result from chronic venous insufficiency due to persistent elevation of venous pressures |
Develop due to peripheral neuropathy and pressure-related trauma. |
|
Clinical features |
|
|
|
|
ABPI/ investigations |
|
|
|
Reviewer
Dr Shabana Habib
Dermatology registrar
Editor
Dr Chris Jefferies
References
- British Association of Dermatologists (2020) Dermatology: a handbook for medical students & junior doctors. Available from: [LINK]
- NICE (2023) Venous Leg Ulcers. Available from: [LINK]
- DermNet NZ (2004b) Leg ulcer, DermNet. Available at: [LINK]
- BMJ Best Practice (2023) Chronic venous insufficiency – Symptoms, diagnosis and treatment| BMJ Best Practice. Available at: [LINK]
- DermNet NZ (2004) Compression therapy, DermNet. Available from: [LINK]
- Skinsight (2023) Stasis ulcer (venous ulcer): Causes, symptoms, & treatment, Skinsight. Available from: [LINK]
- DermNet NZ (2007) Leg ulcer images, DermNet. Available from: [LINK]
- DermNet NZ (2016) Differential diagnosis of Leg Ulcer, DermNet. Available from: [LINK]
- NICE (2015) Diabetic foot problems: Prevention and management: Guidance. Available from: [LINK]
Image references
- Figure 1. Jonathan Moore. Arterial ulcer peripheral vascular disease. License: [CC BY]
- Figure 2. Dermnet. Venous ulcer. License: [CC BY-NC-ND]
- Figure 3. Ashashyou. Chronic venous insufficiency & Venous ulcer. License: [CC BY-SA]
- Figure 4. Dermnet. Diabetic foot ulcer. License: [CC BY-NC-ND]