- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Introduction
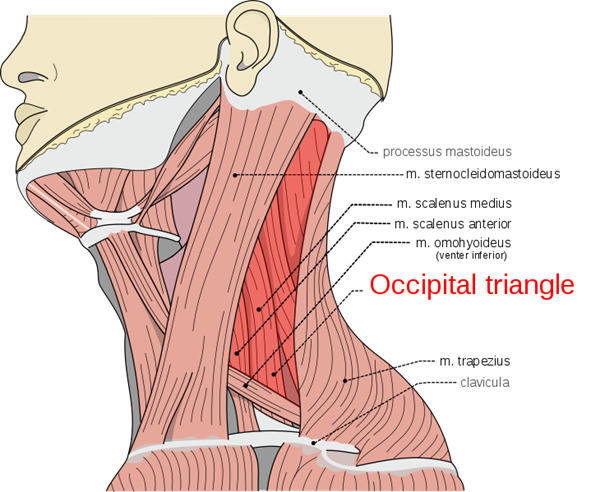
The scalene muscles are located beneath the prevertebral fascia within the floor of the posterior triangle of the neck. They are a set of three muscles (anterior, middle and posterior scalenes) lying deep to the sternocleidomastoid.
The scalene muscles attach among the first and second ribs and the transverse processes of the cervical vertebrae. Their functions include elevating the first and second rib, as well as laterally flexing the neck.
The scalene muscles are active during inspiration and, when the cervical spine is stabilised, the scalenes can elevate the first two ribs to act as accessory muscles of respiration.
This article will cover the scalene muscles individually, to explore their origins and insertions, functions, innervation and blood supply.
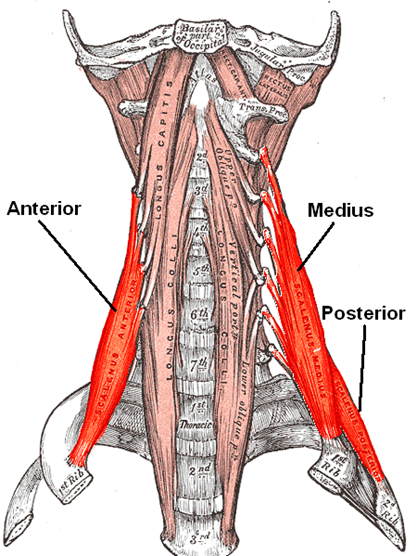
Anterior scalene
Lying posteromedial to the sternocleidomastoid, the anterior scalene has several important structures lying in close proximity:
- Anterior: phrenic nerve
- Posterior: subclavian artery
- Lateral: brachial plexus
Origin
Anterior tubercles of the transverse processes of C3-C6.
Insertion
Scalene tubercle of the first rib.
Function
Flexes the cervical portion of the vertebral column forwards and laterally and rotates it to the contralateral side. The muscle also helps elevate the first rib.
Innervation
Branches of the anterior rami of the cervical spinal nerves (C4-6).
Blood supply
Ascending cervical branch of the inferior thyroid artery.
Middle scalene
The middle scalene is the longest and largest of the scalene muscles. The clavicle and omohyoid muscle cross the middle scalene anteriorly and it is separated from the anterior scalene by the subclavian artery and the ventral rami of the cervical spinal nerves.
The posterior scalene and levator scapulae muscle are situated posterolateral to the middle scalene. The first two roots of the long thoracic nerve and the dorsal scapular nerve pierce the middle scalene and emerge on its lateral surface.
Origin
Posterior tubercles of the transverse processes of C4-C8. It is also attached to the transverse process of the axis and often extends to the transverse process of the atlas.
Insertion
Upper surface of the first rib.
Function
Laterally flexes the cervical portion of the vertebral column to the ipsilateral side and helps elevate the first rib.
Innervation
Branches of the anterior rami of the cervical spinal nerves (C3-8).
Blood supply
Ascending cervical branch of the inferior thyroid artery.
Posterior scalene
The smallest and the most deeply located of the scalene muscles, the posterior scalene is sometimes found to be blended with the middle scalene.
Origin
Posterior tubercles of the transverse processes of C4-C6.
Insertion
Outer surface of the second rib.
Function
Laterally flexes the lower end of the cervical portion of the vertebral column to the ipsilateral side and helps elevate the second rib.
Innervation
Branches of the anterior rami of the cervical spinal nerves (C6-8).
Blood supply
Ascending cervical branch of the inferior thyroid artery. The posterior scalene is also supplied by the superficial cervical artery.
Clinical relevance: thoracic outlet syndrome
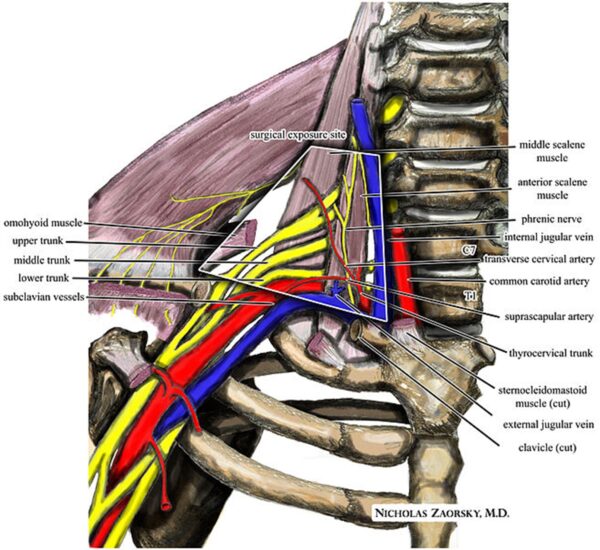
The brachial plexus and/or the subclavian vessels can become compressed as they go from the neck to the axilla. Thoracic outlet syndrome describes the range of symptoms that arise from this compression.
Although the specific mechanism of compression in any person is challenging to ascertain, several predisposing factors exist including:
- Fibrous bands that spread from the transverse process of C7 to the first rib called cervical ribs
- Differences in the insertion of the anterior scalene muscle
- Nerves and vasculature following an atypical course
- A cervical fracture causing deformity
- Anterior scalene hypertrophy from weightlifting
There are three symptom complexes:
- Neurogenic (majority of cases): the compression typically happens in the scalene triangle (formed by the anterior scalene, middle scalene and first rib). The lower trunk of the brachial plexus is most often involved. Features include chronic neck pain and paraesthesia following the distribution of the ulnar nerve.
- Venous: the subclavian vein becomes compressed in the costoclavicular space where it passes the first rib. Features include arm swelling, pain and cyanosis.
- Arterial: a subclavian artery aneurysm or a post-stenotic area of dilation can cause compression. Subclavian artery aneurysms can be accompanied by a mural thrombus. Thromboemboli can then form causing symptoms such as hand pain, pallor, coldness and paraesthesia due to ischaemia of the digits.
The treatment of neurogenic thoracic outlet syndrome is often conservative with physiotherapy. Surgery may be considered for progressive neurological deficits or refractory symptoms; it is typically performed to manage vascular features.
Clinical relevance: interscalene block
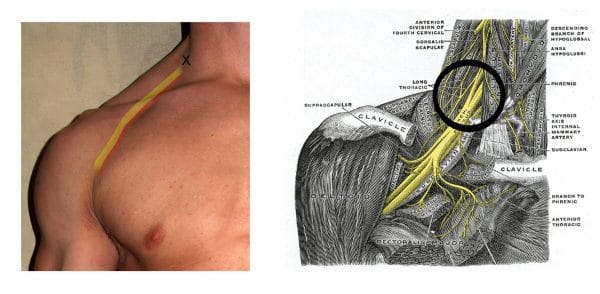
An interscalene block is used to provide regional anaesthesia by anaesthetising the nerve roots of the cervical plexus and the upper and middle trunks of the brachial plexus.
This type of brachial plexus block is often used in the context of shoulder/upper limb surgery, often to provide effective post-op analgesia. The interscalene groove between the anterior scalene and middle scalene is identified and local anaesthetic is injected over the roots of the brachial plexus at the level of the groove (Figure 4).
Key points
- The scalene muscles are a set of three muscles: the anterior scalene, the middle scalene and the posterior scalene. They are located in the posterior triangle of the neck.
- The scalene muscles originate from the transverse processes of cervical vertebrae and insert along the first and second ribs.
- Their functions include elevating the first and second rib, laterally flexing the neck and acting as accessory muscles of respiration.
- They are innervated by cervical spinal nerves and receive arterial supply from the inferior thyroid artery.
Editor
Dr Chris Jefferies
References
- Susan Standring. Gray’s Anatomy. 42nd Elsevier. Published in 2020.
- John T. Hansen. Netter’s Clinical Anatomy. 4th Elsevier. Published in 2018.
- Donald A. Neumann. Kinesiology of the Musculoskeletal System. 3rd Elsevier. Published in 2016.
- Peter A Brennan, Susan Standring, Sam M Wiseman. Gray’s Surgical Anatomy. 1st Elsevier. Published in 2020.
Image references
- Remesz, Olek (2007). Scheme of muscles of neck (left side, platysma muscle dissected). License: [CC BY]
- Häggström, Mikael (2007). Scalenus muscles. License: [Public domain]
- Zaorsky, Nicholas, M.D. (2010). An illustration of the relevant neurovascular anatomy in anterior supraclavicular neurosurgical approach to the brachial plexus and subclavian vessels for thoracic outlet syndrome. License: [CC BY-SA]
- Shankbone, David (Foto) (2008), Grey’s anatomy. Interscalene block. License: [CC BY-SA]