- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Introduction
Chickenpox is a common viral infection, caused by the varicella-zoster virus (VZV).1 Over 75% of children are infected with VZV before age five.2
Aetiology
VZV is a DNA virus of the herpesviridae family.1 Transmission is via droplet spread or direct skin contact with vesicle fluid, with the virus entering the body through the upper respiratory tract.1,3
Clinical features
Chickenpox is an acute disease, characterised by a vesicular rash associated with fever and malaise.3 The incubation period is typically 10-14 days but can be up to 21 days.4
Symptoms are milder in younger children (once past the neonatal stage) and more severe in adults.1
Prodrome
Prodromal symptoms can last up to four days and include the following:1,3
- High fever (38-39°C)
- General malaise
- Myalgia
- Anorexia
- Headache
- Nausea
Rash
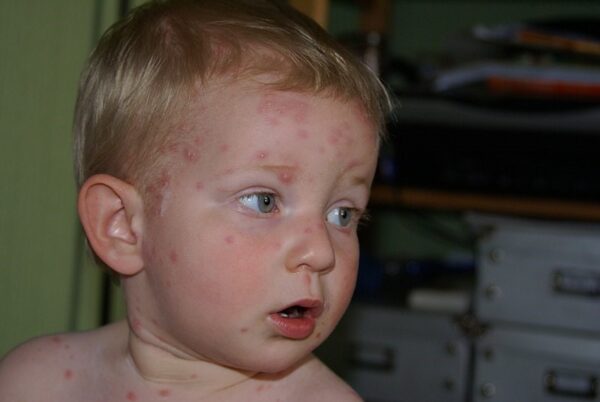
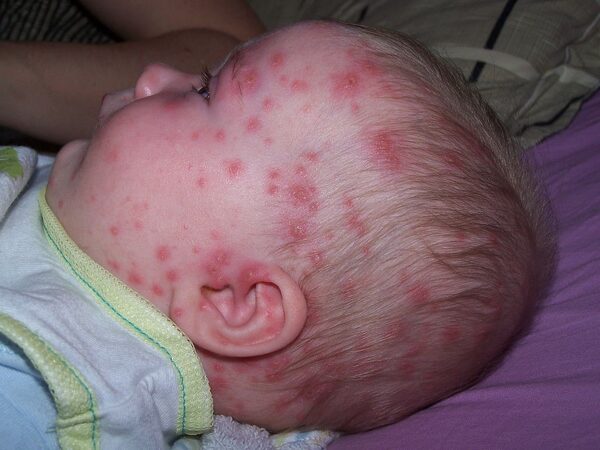
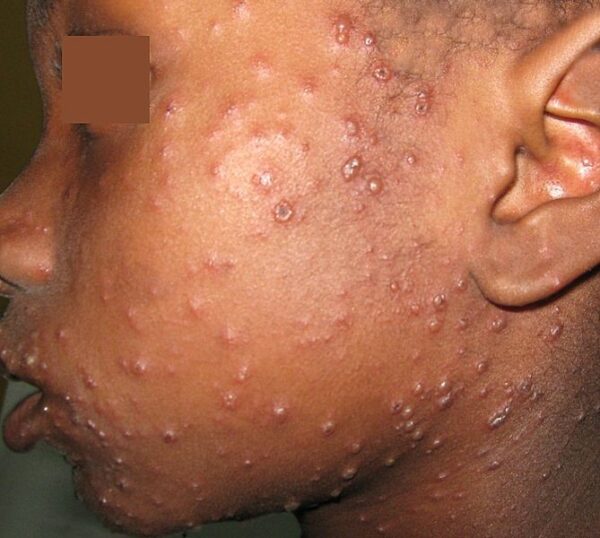
As the prodromal period ends, the characteristic rash (Figures 1-3) develops:3
- It begins as small erythematous macules on the scalp, face, trunk and proximal limbs
- These macules develop into papules, vesicles and pustules which appear in crops
- Vesicles may be found on the palms, soles and mucous membranes, and are especially itchy
- Shallow oral and genital ulcers can also occur, which are painful
- Crusting of the vesicles and pustules usually occurs in five days, at which point new vesicle formation has ceased
Differential diagnoses
There are several differential diagnoses for chickenpox (Table 1).3
Table 1.Differential diagnoses of chickenpox (VZV)
|
|
Differential |
Notes |
|
Vesicular viral rashes |
Herpes simplex (HSV) |
Vesicles are usually more localised i.e. cold sores (except in eczema herpeticum- disseminated HSV) |
|
|
Herpes zoster (VZV) |
Also known as shingles – a reactivation of VZV usually localised to a unilateral dermatome |
|
|
Hand, foot and mouth disease (Coxsackie A virus) |
This rash presents as vesicles localised to the hands and feet, with ulcers in the mouth |
|
Other infections |
Impetigo (usually strep or staph) |
Pustules which develop into golden crusted lesions, usually on the face |
|
|
Scabies (mites) |
Erythematous papular rash usually starting between the fingers |
|
Skin disorders |
Guttate psoriasis, drug eruptions, dermatitis herpetiform, insect bites |
|
Investigations
Chickenpox is a clinical diagnosis, and investigations are not generally required unless there are concerns about complications. If diagnostic confirmation is needed, lesion scrapings can be tested.1
Management
General advice1
General advice to prevent complications and the spread of the virus includes:
- Adequate hydration
- Avoidance of scratching (due to the risk of infection and scarring)
- Avoidance of pregnant women, neonates and immunocompromised individuals
Symptomatic management
Symptomatic management options include:
- Paracetamol for fever and discomfort3
- NSAIDs should be avoided as they increase the risk of necrotising soft tissue infections5
- Sedating antihistamines (chlorphenamine), emollients and calamine lotion for itch1,3
- If an adolescent or adult presents within 24 hours of rash onset (especially if severe or they are at high risk of complications) oral aciclovir can be considered3
Treatment in high-risk groups
Management differs for patients who are immunocompromised (e.g. neonates, pregnant women, breastfeeding women) due to the increased risk of severe disease.
Urgent specialist advice should be sought and further management options may include:
- Antiviral medication such as aciclovir
- Intravenous immunoglobulin (typically for individuals who have not previously been exposed to varicella-zoster virus)
Treatment of complications
Secondary bacterial skin infection and pneumonia require antibiotics.1 Hospital admission is likely to be necessary for those with severe disease or complications.
Public health requirements
Chickenpox is a notifiable disease in Scotland and Northern Ireland, but not in England or Wales.1 Children should not return to school until all lesions are crusted over, due to the highly infectious nature of the virus.6 A vaccine is available in the UK, but there is no mass vaccination programme.1
Complications
In healthy children, chickenpox is usually self-limiting.3 However, complications occur more frequently in the following high-risk groups:1
- Immunocompromised patients (e.g. cancer patients on chemotherapy)
- Very young (neonates) or older patients
- Pregnant women: causes both more severe maternal disease and fetal complications (discussed below)
Complications may include:
- Dehydration3
- Secondary bacterial infection of lesions1
- Scarring1
- Viral pneumonia: this is more common in older children and adults and can be life-threatening1
- Encephalitis: the associated mortality is 5-10%1
- Reye’s syndrome: a very rare condition seen in children and young adults recovering from viral illnesses. It is thought to be related to the use of aspirin, which should be avoided in children7
Once a person has had chickenpox they are usually immune if immunocompetent, with second episodes thought to be rare.1
Shingles
The VZV virus remains dormant in the sensory nerve ganglia of the dorsal root and can reactivate as herpes zoster (shingles) many years later.3
High-risk populations
Chickenpox in pregnancy
If chickenpox is contracted before 20 weeks gestation there is a <2% risk of congenital varicella syndrome.8 This is characterised by:1
- Intrauterine growth restriction
- Microcephaly
- Limb hypoplasia
- Ophthalmological defects
- Cutaneous scarring
After 20 weeks gestation, maternal chickenpox infection can cause neonatal herpes zoster (shingles) or preterm labour.1 Maternal chickenpox can also be severe, with a high risk of pneumonia for the mother.1
Chickenpox in neonates
There is a risk of neonatal chickenpox if the maternal rash appears seven days before, to two days after delivery (as there is transplacental transmission of the virus but not the initial IgM antibodies).1 Neonatal chickenpox has a 30% mortality, usually from severe pneumonia or fulminant hepatitis.1 Treatment is with aciclovir and immunoglobulin.1
Chickenpox in immunocompromised individuals
There is a greater risk of severe disseminated chickenpox, varicella pneumonia, encephalitis, hepatitis, and haemorrhagic complications amongst immunocompromised individuals.3
Key points
- Chickenpox is a very common and highly infectious viral infection.
- The characteristic rash begins as macules and progresses to papules, vesicles and pustules before crusting over. Crops of different stages are found at different sites.
- Chickenpox is generally self-limiting in the immunocompetent and only symptomatic treatment is required.
- Aciclovir can be used in high risk or severe cases.
- Complications include pneumonia, encephalitis and secondary bacterial infection.
- Pregnant women are at risk of congenital varicella syndrome, preterm labour or neonatal chickenpox.
- VZV can re-emerge as shingles later in life.
References
- Patient.info. Chickenpox. Updated November 2016. Available from: [LINK]
- Manikkavasagan G, Dezateux C, Wade A, Bedford H. The epidemiology of chickenpox in UK 5-year olds: an analysis to inform vaccine policy. Published November 2010. Available from: [LINK]
- NICE CKS. Updated August 2018. Available from: [LINK]
- Heininger U, Seward JF. Published February 2007. Available from: [LINK]
- Mikaeloff Y, Kezouh A, Suissa S. Nonsteroidal anti-inflammatory drug use and the risk of severe skin and soft tissue complications in patients with varicella or zoster disease. Published February 2008. Available from: [LINK]
- HSC Public Health Agency. Guidance on infection control in schools and other childcare settings. Published March 2017. Available from: [LINK]
- NHS.uk. Reye’s Syndrome. Updated November 2019. Available from: [LINK]
- Royal College of Obstetricians and Gynaecologists. Chickenpox in Pregnancy. Published January 2015. Available from: [LINK]
- Phyllis Buchanan. Oh no – chicken pox! Licence: [CC BY-SA 2.0] Available from: [LINK]
- ILJR. Varicelle enfant. Licence: [CC BY-SA 3.0] Available from: [LINK]
- Grook da Oger. Varicelle importante chickenpox. Licence: [CC BY-SA 4.0] Available from: [LINK]
Reviewer
Dr Jennifer Mackintosh
Paediatrics ST8
Editor
Hannah Thomas