- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Hearing assessment and otoscopy frequently appears in OSCEs and you’ll be expected to identify relevant signs using your clinical examination skills. This guide provides a step-by-step approach to performing hearing assessment and otoscopy in an OSCE setting, with an included video demonstration.
Introduction
Wash your hands and don PPE if appropriate.
Introduce yourself to the patient including your name and role.
Confirm the patient’s name and date of birth.
Briefly explain what the examination will involve using patient-friendly language: “Today I’d like to examine your ears, this will involve me having a look inside your ears using a special piece of equipment known as an otoscope. I’d also like to assess your hearing.”
Gain consent to proceed with the examination.
Ask the patient to sit on a chair.
Ask the patient if they have any pain before proceeding with the clinical examination.
General inspection
Objects and equipment
Look for objects or equipment on or around the patient that may provide useful insights into their medical history and current clinical status:
- Hearing aids: note if the patient is wearing a hearing aid and ask the patient to remove this when performing otoscopy.
- Mobility aids: items such as wheelchairs and walking aids give an indication of the patient’s current mobility status. The patient may have vestibulocochlear nerve pathology causing both hearing and balance issues.
Gross hearing assessment
Preparation
Ask the patient if they have noticed any change in their hearing recently.
Explain that you’re going to say 3 words or 3 numbers and you’d like the patient to repeat them back to you (choose two-syllable words or bi-digit numbers).
Assessment
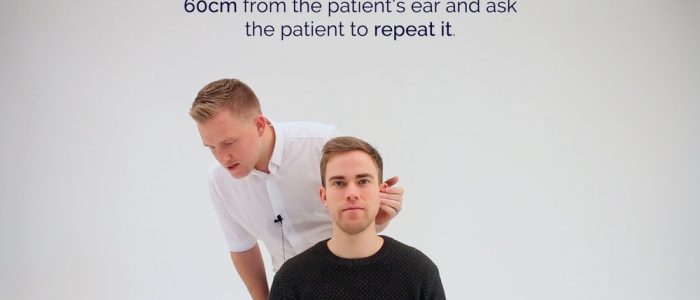
1. Position yourself approximately 60cm from the patient’s ear and then whisper a number or word.
2. Mask the ear not being tested by rubbing the tragus. Do not place your arm across the face of the patient when rubbing the tragus, it is far nicer to occlude the ear from behind the head. If possible shield the patient’s eyes to prevent any visual stimulus.
3. Ask the patient to repeat the number or word back to you. If they get two-thirds or more correct then their hearing level is 12db or better. If there is no response use a conversational voice (48db or worse) or loud voice (76db or worse).
4. If there is no response you can move closer and repeat the test at 15cm. Here the thresholds are 34db for a whisper and 56db for a conversational voice.
5. Assess the other ear in the same way.
Weber’s test
Explain to the patient that you are going to test their hearing using a tuning fork.
1. Tap a 512Hz tuning fork and place in the midline of the forehead. The tuning fork should be set in motion by striking it on your knee (not the patient’s knee or a table).
2. Ask the patient “Where do you hear the sound?”
These results should be assessed in context with the results of Rinne’s test before any diagnostic assumptions are made:
- Normal: sound is heard equally in both ears.
- Sensorineural deafness: sound is heard louder on the side of the intact ear.
- Conductive deafness: sound is heard louder on the side of the affected ear.
A 512Hz tuning fork is used as it gives the best balance between time of decay and tactile vibration. Ideally, you want a tuning fork that has a long period of decay and cannot be detected by vibration sensation.
Rinne’s test
1. Place a vibrating 512 Hz tuning fork firmly on the mastoid process (apply pressure to the opposite side of the head to make sure the contact is firm). This tests bone conduction.
2. Confirm the patient can hear the sound of the tuning fork and then ask them to tell you when they can no longer hear it.
3. When the patient can no longer hear the sound, move the tuning fork in front of the external auditory meatus to test air conduction.
4. Ask the patient if they can now hear the sound again. If they can hear the sound, it suggests air conduction is better than bone conduction, which is what would be expected in a healthy individual (this is often confusingly referred to as a “Rinne’s positive” result).
Summary of Rinne’s test results
These results should be assessed in context with the results of Weber’s test before any diagnostic assumptions are made:
- Normal result: air conduction > bone conduction (Rinne’s positive)
- Sensorineural deafness: air conduction > bone conduction (Rinne’s positive) – due to both air and bone conduction being reduced equally
- Conductive deafness: bone conduction > air conduction (Rinne’s negative)
Conductive vs sensorineural hearing loss
Conductive hearing loss occurs when sound is unable to effectively transfer at any point between the outer ear, external auditory canal, tympanic membrane and middle ear (ossicles). Causes of conductive hearing loss include excessive ear wax, otitis externa, otitis media, perforated tympanic membrane and otosclerosis.
Sensorineural hearing loss occurs due to dysfunction of the cochlea and/or vestibulocochlear nerve. Causes of sensorineural hearing loss include increasing age (presbycusis), excessive noise exposure, genetic mutations, viral infections (e.g. cytomegalovirus) and ototoxic agents (e.g. gentamicin).
External ear
Inspection
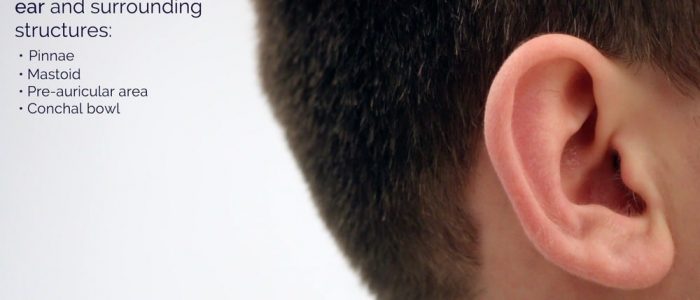
Pinnae
Inspect the pinnae for:
- Asymmetry: by comparing the pinnae you may identify subtle unilateral pathology.
- Deformity of the pinnae: this may be acquired (e.g. cauliflower ear) or congenital (e.g. anotia, microtia, low-set ears).
- Ear piercings: can be a potential source of infection, an allergen and a cause of trauma.
- Erythema and oedema: typically associated with otitis externa.
- Scars: indicative of previous surgery.
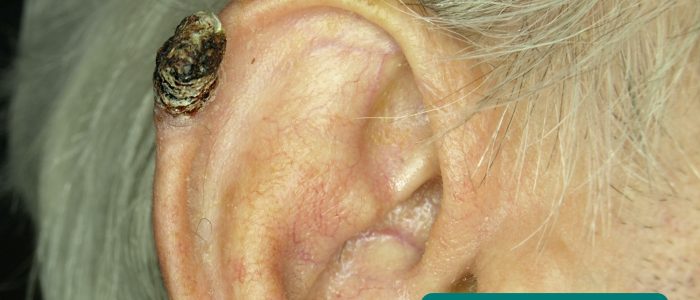
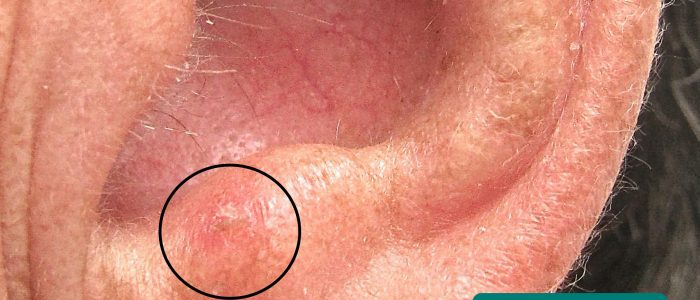
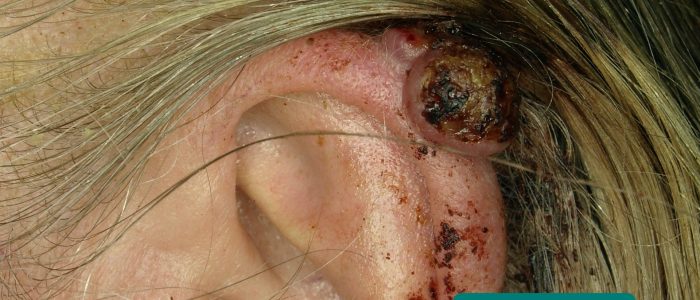
- Skin lesions: look for evidence of pre-malignant (actinic keratoses) and malignant (e.g. basal cell carcinoma, squamous cell carcinoma) skin changes.
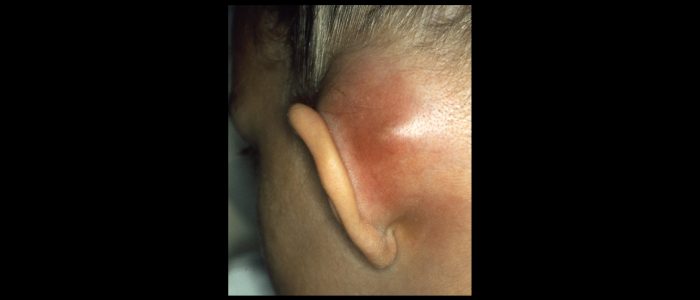
Mastoid
Inspect the mastoid region:
- Erythema and swelling: typically associated with mastoiditis.
- Scars: indicative of previous surgery (e.g. mastoidectomy).
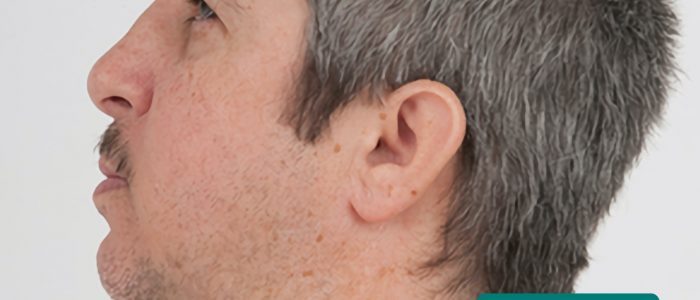
Pre-auricular region
Inspect the pre-auricular region (in front of the ear):
- Pre-auricular sinus/pit: a common congenital deformity that appears as a dimple in the pre-auricular region. These sinuses can sometimes become infected and require surgical drainage.
- Lymphadenopathy: typically associated with an ear infection (e.g. otitis media, otitis externa).
Conchal bowl
Inspect the conchal bowl for signs of active infection such as erythema and purulent discharge.
Palpation
Palpate the tragus for tenderness which is typically associated with otitis externa.
Palpate the regional lymph nodes:
- Pre-auricular lymph nodes
- Post-auricular lymph nodes
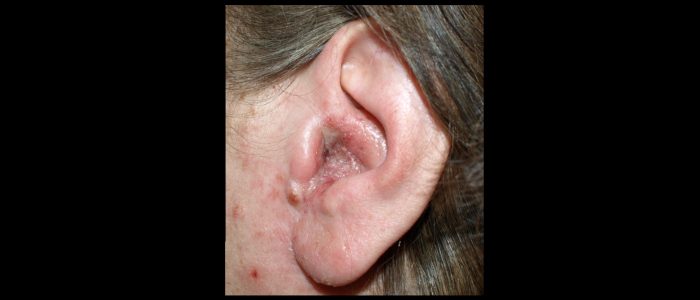
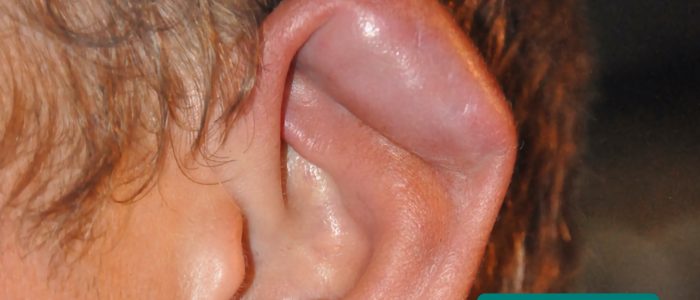
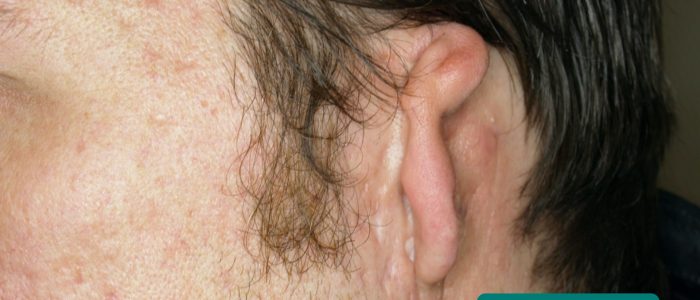
Cauliflower ear
Cauliflower ear is an irreversible condition that develops as a result of repeated blunt ear trauma. Blunt trauma causes bleeding under the perichondrium of the pinna, stripping away the ear’s cartilage. This cartilage normally relies on the perichondrium for its nutrient supply and as a result, once separated it becomes fibrotic, causing distortion of the ear’s architecture.
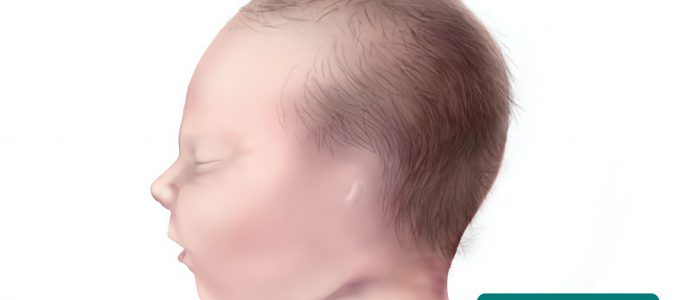
Congenital deformity of the ears
There are several types of congenital ear deformity including:
- Anotia: a complete absence of the pinna.
- Microtia: underdevelopment of the pinna.
- Low-set ears: the ears are positioned lower on the head than usual. Low-set ears are a feature of several genetic syndromes including Down’s syndrome and Turner’s syndrome.
Otoscopy
To help decide which ear to examine first:
- Check if the patient has any ear discomfort and if so examine the non-painful side first.
- Ask the patient which is their “better” ear and examine this one first (this can be useful for comparison).
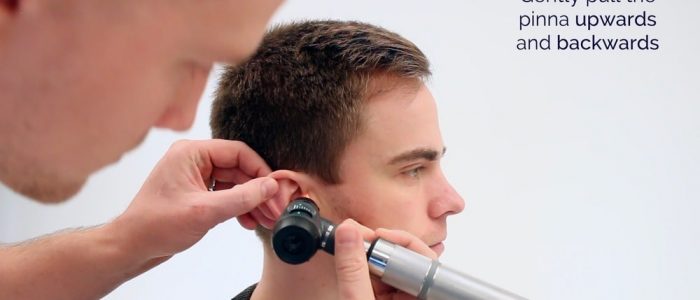
Inserting the otoscope
1. Ensure the light is working on the otoscope and apply a sterile speculum (the largest that will comfortably fit in the external auditory meatus).
2. Pull the pinna upwards and backwards with your other hand to straighten the external auditory canal.
3. Position the otoscope at the external auditory meatus:
- The otoscope should be held in your right hand for the patient’s right ear and vice versa for the left ear.
- Hold the otoscope like a pencil and rest your hand against the patient’s cheek for stability. This will prevent damage to the ear if there is sudden movement.
4. Advance the otoscope under direct vision. Be gentle with the otoscope and ensure movements are slow and considered otherwise you will cause discomfort.
External auditory canal assessment
5. Inspect the external auditory canal for:
- Excessive ear wax: the most common cause of conductive hearing loss.
- Erythema and oedema: typically associated with otitis externa.
- Discharge: may suggest otitis externa or otitis media with associated tympanic membrane perforation.
- Foreign bodies: these may include cotton buds, insects and other small objects.
Tympanic membrane assessment
6. Systematically inspect the four quadrants of the tympanic membrane (TM) to avoid missing pathology.
Colour
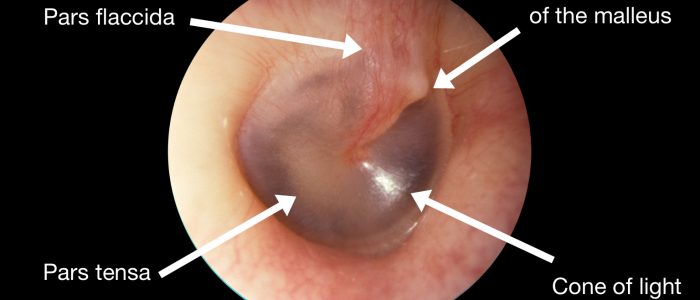
A healthy TM should appear pearly grey and translucent.
Erythema suggests inflammation of the TM which can occur in conditions such as acute otitis media.
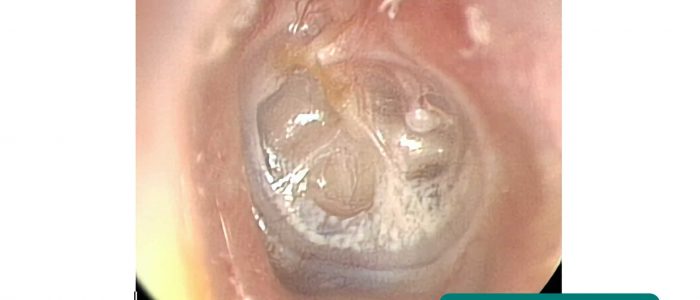
Shape
A healthy TM should appear relatively flat.
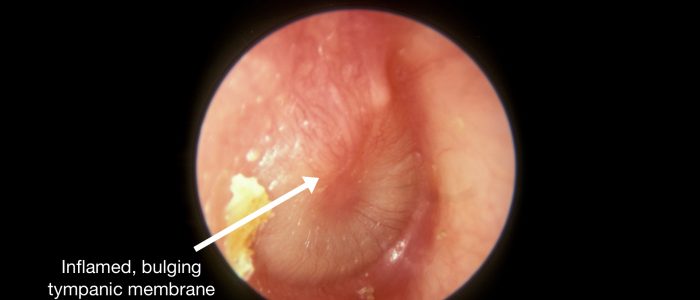
Bulging of the TM suggests increased middle ear pressure, which is commonly caused by acute otitis media with effusion (there is often an associated visible fluid level).
Retraction of the TM suggests reduced middle ear pressure, which is commonly caused by pharyngotympanic tube dysfunction secondary to upper respiratory tract infections and allergies.
Light reflex
The light reflex (also known as the “cone of light”) is visible when a light is shone onto the TM.
If a TM is healthy, the cone-shaped reflection of light should appear in the anterior inferior quadrant.
In the left ear, the light reflex should be positioned at approximately 7 o’clock to 8 o’clock.
In the right ear, the light reflex should be positioned at approximately 4 o’clock to 5 o’clock.
Absence or distortion of the light reflex is associated with otitis media (due to bulging of the TM).
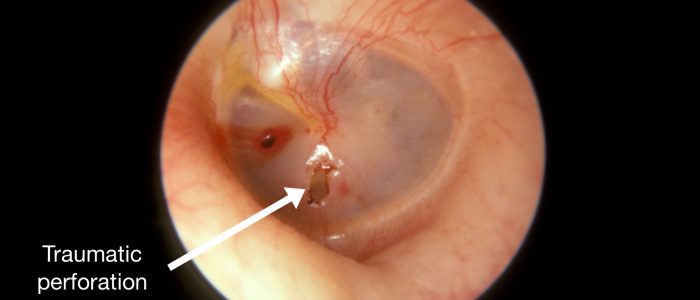
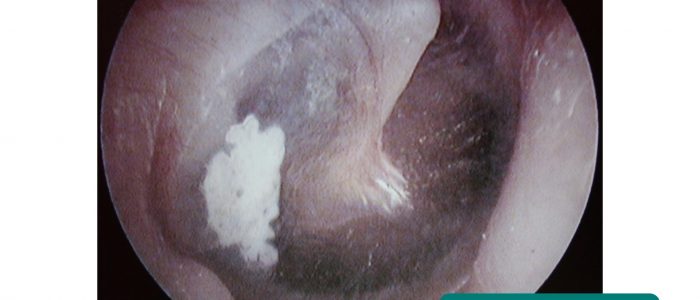
Perforation
Note the size and the position of any perforations of the TM.
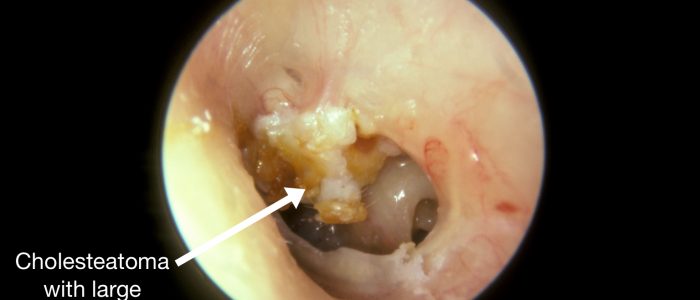
Causes of TM perforation include infection (e.g. otitis media with effusion), trauma (e.g. diving-related), cholesteatoma and insertion of tympanostomy tubes (also known as grommets).
Cholesteatoma typically causes perforation in the superior part of the TM and there may be visible granulation tissue and discharge in this region.
Scarring
Scarring of the TM is known as tympanosclerosis and can result in significant conductive hearing loss if it is extensive.
Tympanosclerosis often develops secondary to otitis media or after the insertion of a tympanostomy tube.
Final steps
7. Withdraw the otoscope carefully.
8. Repeat your assessment on the other ear, comparing your findings. If the patient has an infection in one ear, you should change the speculum on the otoscope before examining the other ear.
9. Discard the otoscope speculum into a clinical waste bin.
Otitis media and otitis externa
Acute otitis media is an inflammatory condition of the middle ear that can be caused by viruses and bacteria. Typical findings on otoscopy include a bulging red, yellow or cloudy tympanic membrane with an associated air-fluid level behind the membrane. There may also be discharge in the auditory canal if the tympanic membrane has perforated.
Otitis externa is an inflammatory condition of the outer ear that can affect the auricle, external auditory canal and external surface of the tympanic membrane. The condition is usually caused by a bacterial infection. Typical findings on examination include erythema of the auricle and external auditory canal with associated pain. Other findings may include oedema of the auditory canal causing narrowing, regional lymphadenopathy and discharge in the ear canal.
To complete the examination…
Explain to the patient that the examination is now finished.
Thank the patient for their time.
Dispose of PPE appropriately and wash your hands.
Summarise your findings.
Example summary
“Today I examined Mr Smith, a 25-year-old male. On general inspection, the patient appeared comfortable at rest and there were no abnormalities noted on inspection of the external ear.”
“Otoscopy revealed normal tympanic membranes and auditory canals. There was no evidence of hearing loss on assessment.”
“In summary, these findings are consistent with a normal examination of the ears.”
“For completeness, I would like to perform the following further assessments and investigations.”
Further assessments and investigations
- Cranial nerve examination: to identify evidence of facial nerve pathology.
- Audiometry and tympanometry: to screen for hearing loss.
Reviewers
Mr Krishan Ramdoo
ENT Registrar
Mr Ben Cosway
ENT Registrar
References
- CNX OpenStax. Adapted by Geeky Medics. Otitis externa. Licence: [CC BY 4.0].
- B. Welleschik. Adapted by Geeky Medics. Mastoiditis. Licence: CC BY-SA.
- Klaus D. Peter, Gummersbach, Germany. Adapted by Geeky Medics. Basal cell carcinoma. Licence: CC BY 3.0 DE.
- Future FamDoc. Adapted by Geeky Medics. Actinic keratosis. Licence: CC BY-SA.
- Klaus D. Peter, Gummersbach, Germany. Adapted by Geeky Medics. Melanoma. Licence: CC BY 3.0 DE.
- MartialArtsNomad.com. Adapted by Geeky Medics. Cauliflower ear. Licence: CC BY.
- Lisa Leathwood, Maureen Risch. Adapted by Geeky Medics. Low-set ears. Licence: CC0.
- Klaus D. Peter, Gummersbach, Germany. Adapted by Geeky Medics. Microtia. Licence: CC BY 3.0 DE.
- Centers for Disease Control and Prevention, National Center on Birth Defects and Developmental Disabilities. Adapted by Geeky Medics. Anotia.
- By Michael Hawke MD. Adapted by Geeky Medics. Normal tympanic membrane. Licence: [CC BY 4.0].
- By Michael Hawke MD. Adapted by Geeky Medics. Tympanic membrane perforation. Licence: [CC BY 4.0].
- By Michael Hawke MD. Adapted by Geeky Medics. Cholesteatoma. Licence: [CC BY 4.0].
- By Michael Hawke MD. Adapted by Geeky Medics. Acute otitis media. Licence: [CC BY 4.0].
- Didier Descouens. Adapted by Geeky Medics. Tympanosclerosis. Licence: CC BY-SA.
- Adrian L James. Adapted by Geeky Medics. Tympanic membrane retraction. Licence: CC BY-SA.