- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Introduction
Mastoiditis involves inflammation of the mastoid air cells within the petrous temporal bone.
Acute mastoiditis is a complication of acute otitis media (AOM) with the infection spreading from the middle ear into the mastoid air cells. This can result in abscess formation and several life-threatening sequelae.
Mastoiditis is most common in children, with the highest incidence in children <2 years old, with a median age of 12 months.1 There is an increased incidence in children with learning difficulties, and it is twice as common in children with autism spectrum disorder.2,3
Risk factors
Risk factors for mastoiditis include:5,6
- Recurrent AOM (risk factors for AOM include parental smoking, atopy, formula-fed, nursery/day-care, socio-economic deprivation and family history)
- Age
- Learning difficulties
- Immunocompromise
- Anatomical abnormalities: incomplete pneumatisation of the mastoid process, cholesteatoma
Aetiology
Acute mastoiditis is usually secondary to bacterial infection. The most common causative pathogen is Streptococcus pneumoniae.
Other common organisms include Staphylococcus aureus, Streptococcus pyogenes and Haemophilus influenzae.6
Pathophysiology
The mastoid is part of the petrous temporal bone and is located posterior to the middle ear.
Mastoiditis is associated with the progression of AOM with infection spreading from the middle ear into the mastoid air cell system via the mastoid antrum, causing osteitis of mastoid bone.
Initially, there is hyperaemia and oedema of the mastoid air cell mucosa. Mucositis and swelling of the aditus ad antrum block effective drainage of the mastoid air cell system. Serous then purulent exudate collects in the air cells.
Increased pressure within the air cell system results in bone necrosis of the thin bony septae. Pus coalesces and an abscess cavity forms.7
Clinical features
The initial diagnosis of acute mastoiditis is clinical, supported with cross-sectional imaging.
No consensus exists on exact diagnostic criteria for acute mastoiditis. The most used criteria are a recent episode of acute otitis media plus at least two of the following:8,9
- Proptosed auricle
- Post-auricular swelling
- Post-auricular erythema
- Post-auricular tenderness
History
Typical symptoms of mastoiditis in children (<2) include:
- Ear pulling
- Ear pain
- Non-specific symptoms of systemic upset: irritability, fever, lethargy, reduced oral intake, diarrhoea
- Persistent fever despite appropriate oral antibiotics
Typical symptoms of mastoiditis in adults include:
- Severe otalgia
- Otorrhoea
- Headache
- Hearing loss
- Persistent fever despite appropriate oral antibiotics
- Vertigo
Clinical examination
Typical clinical findings on external examination may include:
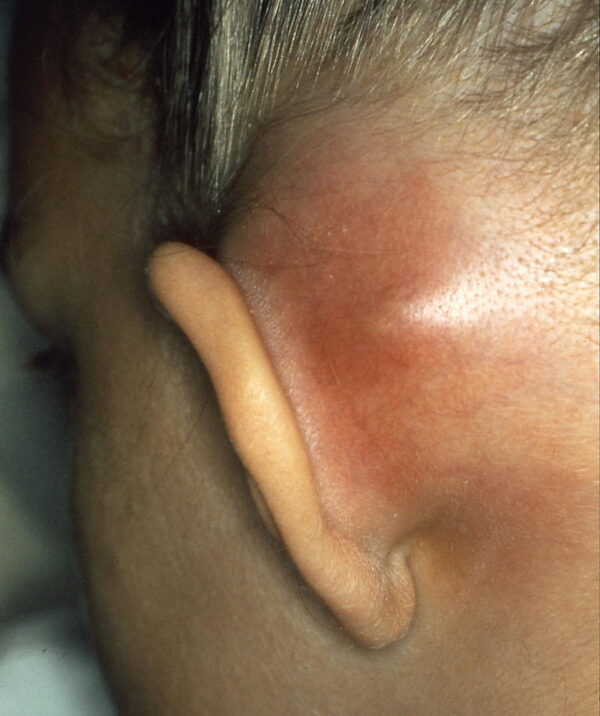
- Post-auricular erythema, tenderness, swelling, fluctuance (Figure 1)
- Proptosed auricle
- Loss of post-auricular sulcus
- Evidence of sepsis
Patients may have clinical findings suggestive of complications of acute mastoiditis. These may include a reduced level of consciousness, facial nerve (CN VII) palsy, abducens nerve (CNVI) palsy (Gradenigo’s syndrome) or fluctuant extra-cranial collections (see complications section).
Typical findings on otoscopy may include:
- Bulging tympanic membrane
- Bulging/sagging of postero-superior wall of the external auditory canal
Differential diagnoses
Differential diagnoses to consider include:
- Acute otitis media: clinically differentiated from mastoiditis by the presence of a well-defined post-auricular sulcus and the absence of post-auricular swelling, erythema or tenderness.
- Post-auricular lymphadenopathy: discrete, tender, superficial swelling often preceded by non-specific upper respiratory tract viral illness or minor local trauma. The swelling is palpably distinct from the mastoid process, not specifically associated with otorrhoea and generally not fluctuant.
- Cellulitis/perichondritis: erythema, tenderness and swelling of skin overlying and around the auricle. May be associated with minor trauma (e.g. cat-scratch, ear piercing or severe otitis externa).
Investigations
Laboratory investigations
Relevant laboratory investigations include:
- FBC: white cell count is a reliable marker of infection and inflammation
- U&E: important to establish baseline renal function in case certain antibiotics may be required
- CRP: raised in the context of infection/inflammation
- Lactate: raised lactate is commonly associated with sepsis/severe inflammatory response syndrome
- Blood cultures: may help identify the causative pathogen in severe infection with bacteraemia and inform the choice of antibiotic agent
A lumbar puncture (LP) may be considered if intra-cranial extension is suspected.
Imaging
A CT of the temporal bones can be used to characterise the progression of infection. Indications for CT imaging include:
- Persistent high fever despite 48 hours of medical management (intravenous antibiotics)
- Any suspicion of complicated acute mastoiditis
Radiological findings on CT may include:1
- Mastoid air cell and middle ear opacification due to fluid collection and inflammatory mucosal swelling
- Loss of distinctive air cell wall due to atrophy/necrosis of bony septa
- Haziness or distortion of the mastoid outline, possibly with visible defects of the tegmen or mastoid cortex
- Enhancement of areas of abscess formation
An MR venogram may be performed if lateral sinus thrombosis suspected.
Management
Immediate management
Immediate management of patients with mastoiditis includes:
- Resuscitation following an ABCDE approach (as per ALS/APLS guidelines)
- Initiation of sepsis 6 including administration of broad-spectrum intravenous antibiotics as per local guidelines
- Nil-by-mouth/keep fasted in case emergency surgical intervention required
- Senior paediatric, ear nose and throat and neurosurgical input (if indicated)
- Analgesia
- Consider cross-sectional imaging (particularly if suspicion of complications)
- Consider lumbar puncture (if concern regarding intracranial extension of infection)
Medical management
Broad-spectrum intravenous antibiotics as per local microbiology guidelines. For example, intravenous piperacillin & tazobactam (tazocin), or metronidazole and ciprofloxacin if penicillin-allergic.
Surgical management
Surgical management of mastoiditis may include:
- Tympanocentesis
- Myringotomy +/- grommet/ventilation/tympanostomy tube insertion
- Cortical mastoidectomy
Purulent middle ear fluid should be sent to microbiology for microscopy, culture and sensitivity.
Follow-up
Outpatient follow-up is usually arranged after one to two weeks for a wound review if surgical management is performed.
Patients should undergo pure-tone audiometry once recovered to exclude persistent, conductive hearing loss.
Complications
Complications of mastoiditis are classified by the direction of spread of infection (deeper into the temporal bone, intracranial and extracranial).
Table 1. The complications of mastoiditis.
| Intra-temporal spread | Extra-temporal/intracranial spread | Extracranial spread |
|
Subperiosteal abscess |
Otogenic meningitis |
Bezold abscess (along sternocleidomastoid) |
|
Facial nerve palsy |
Temporal lobe/cerebellar abscess |
Citelli abscess (overlying posterior belly of digastric) |
|
Bacterial labyrinthitis |
Epidural/subdural abscess |
Luc abscess (deep to temporalis muscle) |
|
Gradenigo’s syndrome/apical petrositis |
Venous sinus thrombosis |
|
|
|
Otitic hydrocephalus |
|
Prognosis
Mastoiditis has a good prognosis in uncomplicated disease with no intracranial extension. Facial nerve palsies are usually transient.
Conductive hearing loss usually resolves with the infection unless significant destruction of middle ear structures has occurred.
Key points
- Mastoiditis is an uncommon complication of acute otitis media and can have life-threatening sequelae if not recognised and managed in a timely fashion.
- The most common bacterial cause is Streptococcus pneumoniae.
- Mastoiditis most commonly affects children under the age of two. It is more common in children with learning difficulties.
- The most used diagnostic criteria are a recent episode of acute otitis media plus two of the following: post-auricular tenderness/erythema/swelling or proptosed auricle. Diagnosis can be supported with cross-sectional imaging.
- Management includes analgesia, broad-spectrum intravenous antibiotics, and surgical intervention if complicated or fails to respond to conservative management.
- Surgical options include tympanocentesis, myringotomy +/- ventilation tube insertion and cortical mastoidectomy.
- There is a good prognosis with early diagnosis and management. However, mastoiditis can be life-threatening if complications develop.
Reviewer
Mr Niall Woodley
Specialty Registrar in ENT
Royal Hospital for Children, Glasgow
Editor
Dr Chris Jefferies
References
- Devan P. Mastoiditis Workup: Approach Considerations, Imaging Studies [Internet]. Medscape. 2020. Available from: [LINK]
- Freeman BA, Parkins C. The Prevalence of Middle Ear Disease among Learning Impaired Children: Does a Higher Prevalence Indicate an Association? Clin Pediatr (Phila) [Internet]. 1979;18(4):205–12. Available from: [LINK]
- Adams DJ, Susi A, Erdie-Lalena CR, Gorman G, Hisle-Gorman E, Rajnik M, et al. Otitis Media and Related Complications Among Children with Autism Spectrum Disorders. J Autism Dev Disord [Internet]. 2016 May 1;46(5):1636–42. Available from: [LINK]
- Zhang Y, Xu M, Zhang J, Zeng L, Wang Y, Zheng QY. Risk factors for chronic and recurrent otitis media-A meta-analysis. PLoS One [Internet]. 2014 Jan 23;9(1):86397. Available from: [LINK]
- Ardc C, Yavuz E. Effect of breastfeeding on common pediatric infections: A 5-year prospective cohort study. Arch Argent Pediatr [Internet]. 2018 Apr 1;116(2):126–32. Available from: [LINK]
- Mansour T, Yehudai N, Tobia A, Shihada R, Brodsky A, Khnifies R, et al. Acute mastoiditis: 20 years of experience with a uniform management protocol. Int J Pediatr Otorhinolaryngol [Internet]. 2019 Oct 1;125:187–91. Available from: [LINK]
- Klein JO. Otitis Externa, Otitis Media, and Mastoiditis. In: Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases [Internet]. Elsevier Inc.; 2014. p. 767-773.e1. Available from: [LINK]
- Laulajainen-Hongisto A, Aarnisalo AA, Jero J. Differentiating Acute Otitis Media and Acute Mastoiditis in Hospitalized Children. Vol. 16, Current Allergy and Asthma Reports. Current Medicine Group LLC 1; 2016.
- Van Den Aardweg MTA, Rovers MM, De Ru JA, Albers FWJ, Schilder AGM. A systematic review of diagnostic criteria for acute mastoiditis in children [Internet]. Vol. 29, Otology and Neurotology. Otol Neurotol; 2008. p. 751–7. Available from: [LINK]
Image references
Figure 1. B. Welleschik. Mastoiditis mit Subperiostalabszess. License: [CC-BY-SA]




