- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Being able to assess the hydration status of a patient is an important skill that you’ll regularly use in clinical practice. It involves assessment of whether a patient is hypovolaemic (dehydrated), euvolaemic or hypervolaemic (fluid overloaded) to inform ongoing clinical management.
This hydration status assessment OSCE guide provides a clear step-by-step approach to assessing a patient’s hydration status in an OSCE setting.
Background
Hypovolaemia vs hypervolaemia
Hypovolaemia refers to an overall deficit of fluid in the body. Causes include poor fluid intake, excessive fluid loss (e.g. vomiting, diarrhoea, haemorrhage, excessive diuretic therapy) and third space loss of fluid (where fluid remains within the body but has shifted from the intravascular space to another compartment within the body).
Hypervolaemia refers to an excess of fluid in the body. Colloquially it is often referred to as fluid overload. Hypervolaemia is common in the elderly and those with renal or cardiac failure. It can be caused by excessive fluid intake or inappropriate fluid retention (e.g. heart failure, renal failure).
The quest to euvolaemia can be a difficult road to tread. Searching for the perfect fluid balance involves assessing an array of clinical symptoms, signs and biochemical indicators. No single parameter or ‘gold standard’ confirms a state of adequate hydration, and the clinician must contemplate a range of factors to fully appreciate whether the patient is hypovolaemic, euvolaemic or hypervolaemic.
Patient factors to consider that may alter fluid homeostasis
Patient age: elderly/very young patients are more prone to dehydration and elderly patients are generally more likely to have cardiac failure and/or chronic renal disease.
Reasons for admission that can increase fluid requirements:
- Trauma
- Febrile illness and sepsis
- Burns
- Surgical patients may need additional volume secondary to bleeding, drainage and third-space fluid losses.
- Gastrointestinal losses (e.g. vomiting, diarrhoea)
- Polyuria
Medical conditions that can affect fluid balance (e.g. renal disease, congestive cardiac failure).
Medications (e.g. diuretics can increase fluid losses)
Pertinent details in the patient’s history:
- Bleeding from any source
- Vomiting: frequency, volume, presence of blood
- Stools: frequency, volume, presence of blood
- Fever and diaphoresis
- Urine output: colour and volume
- Pre-syncope/syncope
- Presence of thirst
- Eating and drinking status (e.g. oral fluids, nil by mouth, receiving IV fluid therapy)
- Symptoms of fluid overload (e.g. shortness of breath, orthopnoea, paroxysmal nocturnal dyspnoea, leg swelling)
- Is the patient on a fluid restriction for another medical condition (e.g. heart failure)?
Introduction
Wash your hands and don PPE if appropriate.
Introduce yourself to the patient including your name and role.
Confirm the patient’s name and date of birth.
Briefly explain what the examination will involve using patient-friendly language.
Gain consent to proceed with the examination.
Adjust the head of the bed to a 45° angle and position the patient lying down.
Adequately expose the patient’s chest for the examination (offer a blanket to allow exposure only when required and if appropriate, inform patients they do not need to remove their bra). Exposure of the patient’s lower legs is also helpful to assess for peripheral oedema.
Ask the patient if they have any pain before proceeding with the clinical examination.
General inspection
Clinical signs
Inspect the patient from the end of the bed whilst at rest, looking for clinical signs suggestive of underlying pathology:
- Cyanosis: bluish discolouration of the skin due to poor circulation (e.g. peripheral vasoconstriction secondary to hypovolaemia) or inadequate oxygenation of the blood (e.g. right-to-left cardiac shunting).
- Shortness of breath: may indicate pulmonary oedema secondary to fluid overload.
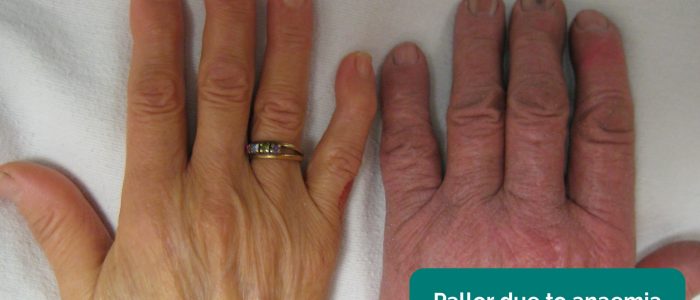
- Pallor: a pale colour of the skin that can suggest underlying anaemia (e.g. haemorrhage, chronic disease) or poor perfusion (e.g. hypovolaemia).
- Malar flush: a plum-red discolouration of the cheeks associated with mitral stenosis.
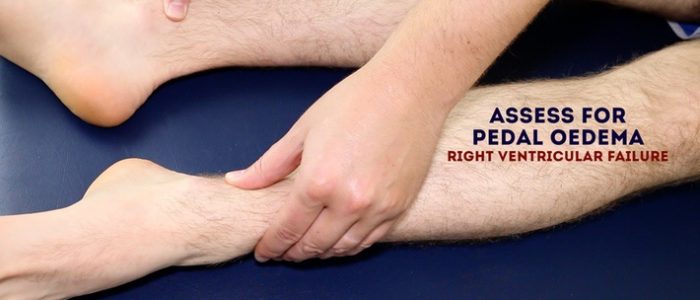
- Oedema: typically presents with swelling of the limbs (e.g. pedal oedema) or abdomen (i.e. ascites).
Objects and equipment
Look for objects or equipment on or around the patient that may provide useful insights into their medical history and current clinical status:
- Medical equipment: such as an oxygen delivery device, intravenous fluid, medication, stoma bag, surgical drain and/or a urinary catheter (note the volume/colour of urine).
- Mobility aids: items such as wheelchairs and walking aids give an indication of the patient’s current mobility status.
- Pillows: patients with congestive heart failure typically suffer from orthopnoea, preventing them from being able to lie flat. As a result, they often use multiple pillows to prop themselves up.
- Vital signs: charts on which vital signs are recorded will give an indication of the patient’s current clinical status and how their physiological parameters have changed over time.
- Fluid balance: fluid balance charts will give an indication of the patient’s current fluid status which may be relevant if a patient appears fluid overloaded or dehydrated. Average urine output should be approximately 0.5mL/kg/hour.
- Daily weight chart: provides an overview of the patient’s weight allowing trends to be identified.
- Stool chart: note the frequency and type of bowel motions (frequent diarrhoea results in significant fluid losses).
- Medication chart: note any medications which may impact fluid balance (e.g. furosemide will cause increased fluid loss).
- Fluid prescription chart: note if the patient has received any intravenous fluids and if so, take note of the volume and type of fluid administered.
- Surgical documentation (if the patient is post-op): check the estimated blood loss in the operating theatre and if any blood or fluid was administered intraoperatively.
Hands
The hands can provide lots of clinically relevant information and therefore a focused, structured assessment is essential.
Inspection
General observations
Inspect the hands and note your findings:
- Colour: pallor suggests poor peripheral perfusion (e.g. congestive heart failure, hypovolaemia) and cyanosis may indicate underlying hypoxaemia.
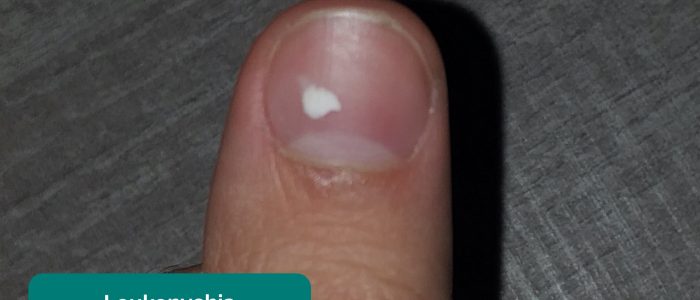
- Leukonychia: whitening of the nail bed, associated with hypoalbuminaemia (e.g. end-stage liver disease, protein-losing enteropathy). Hypoalbuminaemia can result in significant third space fluid loss.
Palpation
Temperature
Place the dorsal aspect of your hand onto the patient’s to assess temperature:
- In healthy individuals, the hands should be symmetrically warm, suggesting adequate perfusion.
- Cool hands may suggest poor peripheral perfusion (e.g. congestive cardiac failure, hypovolaemia).
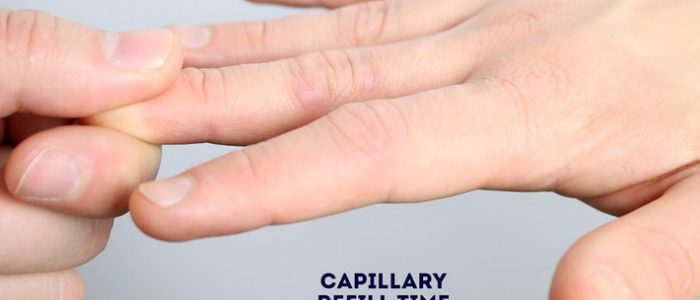
Capillary refill time (CRT)
Measuring capillary refill time (CRT) in the hands is a useful way of assessing peripheral perfusion:
- Apply five seconds of pressure to the distal phalanx of one of a patient’s fingers and then release.
- In healthy individuals, the initial pallor of the area you compressed should return to its normal colour in less than two seconds.
- A CRT that is greater than two seconds suggests poor peripheral perfusion (e.g. hypovolaemia, congestive heart failure) and the need to assess central capillary refill time.
Skin turgor
Assess skin turgor by gently pinching a fold of skin (this can be done on the back of the hand), holding for a few seconds and then releasing the skin. Well hydrated skin should spring back to its previous position immediately, whereas dehydrated skin will slowly return to normal (this is known as decreased skin turgor).
Pulses and blood pressure
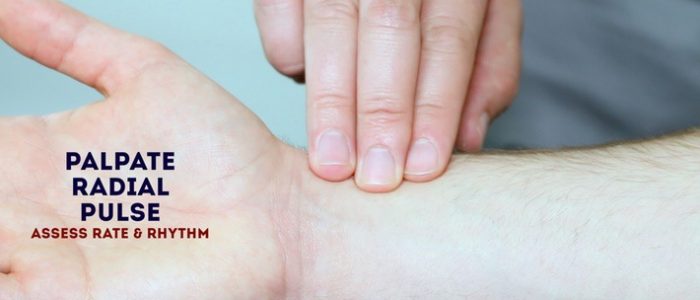
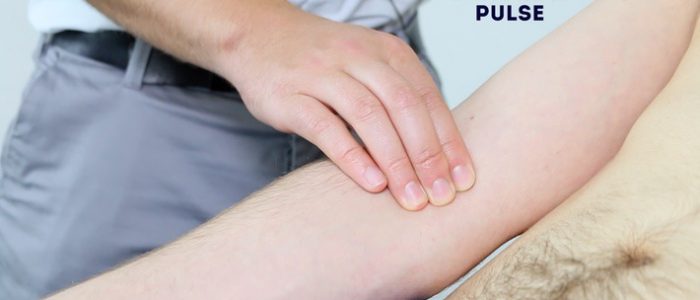
Radial pulse
Palpate the patient’s radial pulse, located at the radial side of the wrist, with the tips of your index and middle fingers aligned longitudinally over the course of the artery.
Once you have located the radial pulse, assess the rate and rhythm.
Calculating heart rate
You can calculate the heart rate in a number of ways, including measuring for 60 seconds, measuring for 30 seconds and multiplying by 2 or measuring for 15 seconds and multiplying by 4. For irregular rhythms, you should measure the pulse for a full 60 seconds to improve accuracy.
Normal and abnormal heart rates
- In healthy adults, the pulse should be between 60-100 bpm.
- A pulse <60 bpm is known as bradycardia and has a wide range of aetiologies (e.g. healthy athletic individuals, atrioventricular block, medications, sick sinus syndrome).
- A pulse of >100 bpm is known as tachycardia and also has a wide range of aetiologies (e.g. anxiety, supraventricular tachycardia, hypovolaemia, hyperthyroidism).
- An irregular rhythm is most commonly caused by atrial fibrillation, but other causes include ectopic beats in healthy individuals and atrioventricular blocks.
Brachial pulse
Palpate the brachial pulse
Palpate the brachial pulse in their right arm, assessing volume and character:
1. Support the patient’s right forearm with your left hand.
2. Position the patient so that their upper arm is abducted, their elbow is partially flexed and their forearm is externally rotated.
3. With your right hand, palpate medial to the biceps brachii tendon and lateral to the medial epicondyle of the humerus. Deeper palpation is required (compared to radial pulse palpation) due to the location of the brachial artery.
Types of pulse character
- Normal
- Slow-rising (associated with aortic stenosis)
- Bounding (associated with aortic regurgitation and also CO2 retention)
- Thready (associated with intravascular hypovolaemia in conditions such as sepsis)
Blood pressure
Measure the blood pressure
Measure the patient’s blood pressure in both arms (see our blood pressure guide for more details).
A comprehensive blood pressure assessment should also include lying and standing blood pressure.
Blood pressure abnormalities
Blood pressure abnormalities may include:
- Hypertension: blood pressure of greater than or equal to 140/90 mmHg if under 80 years old or greater than or equal to 150/90 mmHg if you’re over 80 years old. Causes include essential hypertension, hypervolaemia and renal artery stenosis.
- Hypotension: blood pressure of less than 90/60 mmHg. Causes include hypovolaemia, sepsis and antihypertensives.
- Narrow pulse pressure: less than 25 mmHg of difference between the systolic and diastolic blood pressure. Causes include aortic stenosis, congestive heart failure and cardiac tamponade.
- Wide pulse pressure: more than 100 mmHg of difference between systolic and diastolic blood pressure. Causes include aortic regurgitation and aortic dissection.
- Difference between arms: more than 20mmHg difference in blood pressure between each arm is abnormal and may suggest aortic dissection.
- Postural drop: more than a 20mmHg decrease in systolic blood pressure when moving from sitting to standing. Causes include hypovolaemia, autonomic dysfunction and antihypertensives.
Jugular venous pressure (JVP)
Jugular venous pressure (JVP) provides an indirect measure of central venous pressure. This is possible because the internal jugular vein (IJV) connects to the right atrium without any intervening valves, resulting in a continuous column of blood. The presence of this continuous column of blood means that changes in right atrial pressure are reflected in the IJV (e.g. raised right atrial pressure results in distension of the IJV).
The IJV runs between the medial end of the clavicle and the ear lobe, under the medial aspect of the sternocleidomastoid, making it difficult to visualise (its double waveform pulsation is, however, sometimes visible due to transmission through the sternocleidomastoid muscle).
Because of the inability to easily visualise the IJV, it’s tempting to use the external jugular vein (EJV) as a proxy for assessment of central venous pressure during clinical assessment. However, because the EJV typically branches at a right angle from the subclavian vein (unlike the IJV which sits in a straight line above the right atrium) it is a less reliable indicator of central venous pressure.
See our guide to jugular venous pressure (JVP) for more details.
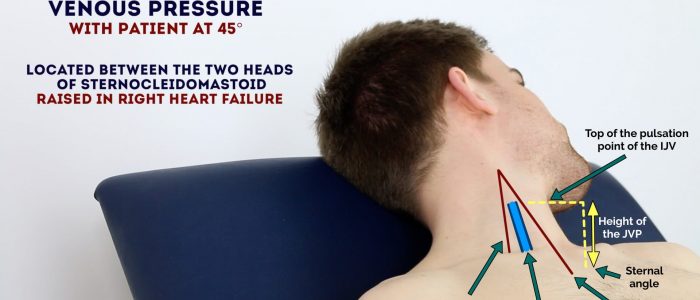
Measure the JVP
1. Position the patient in a semi-recumbent position (at 45°).
2. Ask the patient to turn their head slightly to the left.
3. Inspect for evidence of the IJV, running between the medial end of the clavicle and the ear lobe, under the medial aspect of the sternocleidomastoid (it may be visible between just above the clavicle between the sternal and clavicular heads of the sternocleidomastoid. The IJV has a double waveform pulsation, which helps to differentiate it from the pulsation of the external carotid artery.
4. Measure the JVP by assessing the vertical distance between the sternal angle and the top of the pulsation point of the IJV (in healthy individuals, this should be no greater than 3 cm).
Causes of a raised JVP
A raised JVP indicates the presence of venous hypertension/hypervolaemia. Cardiac causes of a raised JVP include:
- Right-sided heart failure: commonly caused by left-sided heart failure. Pulmonary hypertension is another cause of right-sided heart failure, often occurring due to chronic obstructive pulmonary disease or interstitial lung disease.
- Tricuspid regurgitation: causes include infective endocarditis and rheumatic heart disease.
- Constrictive pericarditis: often idiopathic, but rheumatoid arthritis and tuberculosis are also possible underlying causes.
Face
Eyes
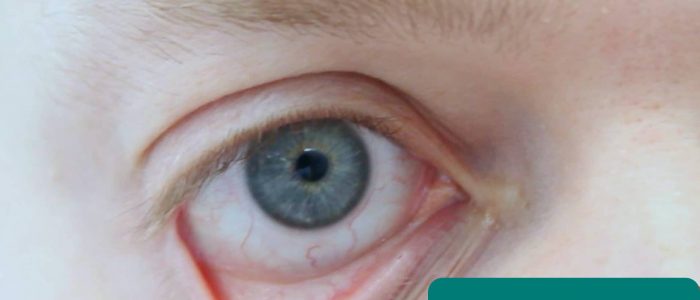
Inspect the eyes for signs relevant to the patient’s fluid status:
- Sunken appearance: associated with hypovolaemia.
- Conjunctival pallor: suggestive of underlying anaemia. Ask the patient to gently pull down their lower eyelid to allow you to inspect the conjunctiva.
Mouth
Inspect the mouth for signs relevant to the patient’s fluid status:
- Dry mucous membranes: associated with hypovolaemia.
Chest
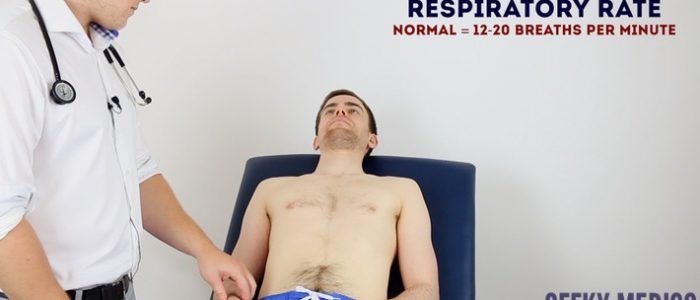
Respiratory rate
Assess the patient’s respiratory rate for 30 seconds and then multiply by 2 to calculate the number of breaths per minute. An increased respiratory rate (tachypnoea) may indicate pulmonary oedema secondary to hypervolaemia.
Central capillary refill time
If capillary refill time was prolonged on peripheral assessment, repeat again over the sternum.
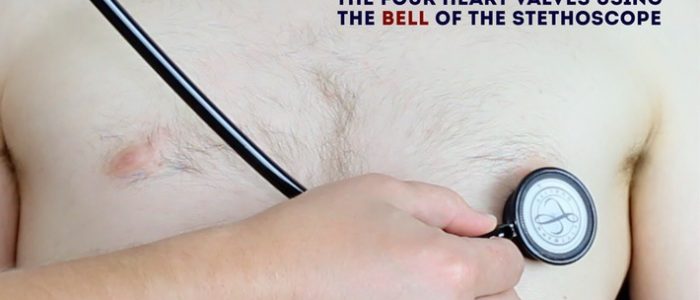
Auscultate heart sounds
A systematic routine will ensure you remember all the steps whilst giving you several chances to listen to each valve area. Your routine should avoid excess repetition whilst each step should ‘build’ upon the information gathered by the previous steps. Ask the patient to lift their breast to allow auscultation of the appropriate area if relevant.
1. Palpate the carotid pulse to determine the first heart sound.
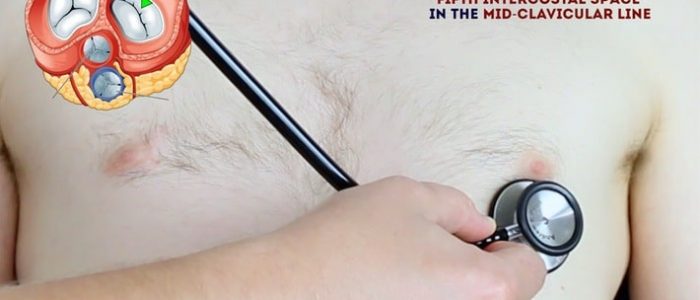
2. Auscultate ‘upwards’ through the valve areas using the diaphragm of the stethoscope whilst continuing to palpate the carotid pulse:
- Mitral valve: 5th intercostal space in the midclavicular line.
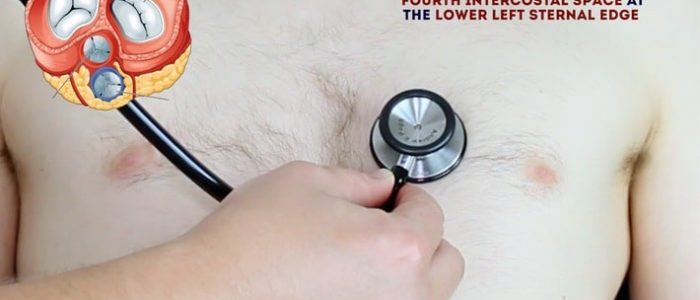
- Tricuspid valve: 4th or 5th intercostal space at the lower left sternal edge.
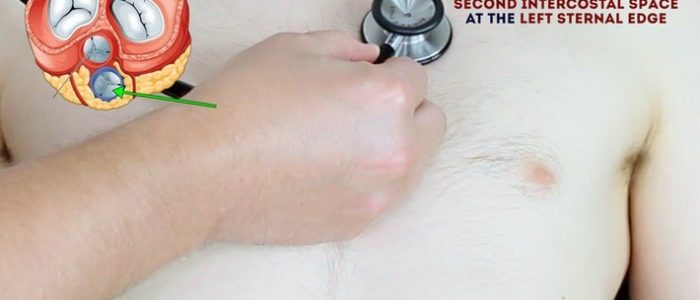
- Pulmonary valve: 2nd intercostal space at the left sternal edge.
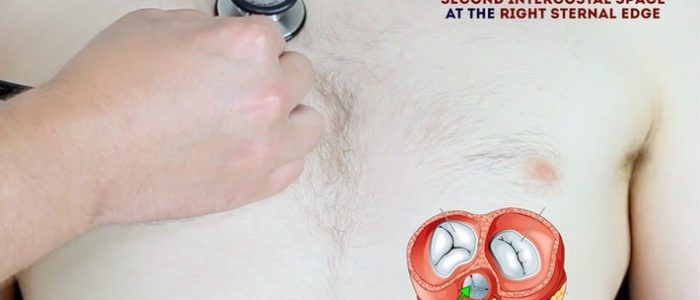
- Aortic valve: 2nd intercostal space at the right sternal edge.
3. Repeat auscultation across the four valves with the bell of the stethoscope.
Abnormal heart sounds in hypervolaemia
A gallop rhythm (i.e. a third heart sound occurring after the normal ‘lub’ ‘dub’ heart sounds) may be noted in hypervolaemia due to elevated atrial and ventricular filling pressures. A gallop rhythm is typically associated with heart failure although it can also be present in healthy athletic individuals.
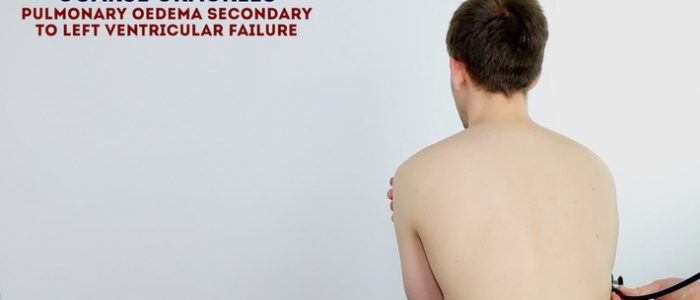
Auscultate the lungs
Auscultate the lung fields posteriorly:
- Coarse crackles are suggestive of pulmonary oedema.
- Absent air entry and stony dullness on percussion are suggestive of an underlying pleural effusion.
Abdomen
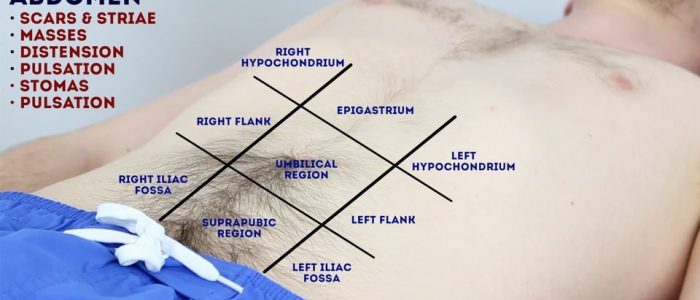
Inspection
Position the patient lying flat on the bed, with their arms by their sides and legs uncrossed for abdominal inspection.
Inspect the patient’s abdomen for signs suggestive of hypervolaemia:
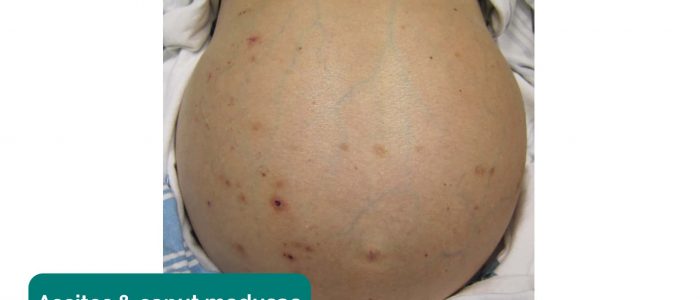
- Abdominal distension: can be caused by a wide range of pathology, but in the context of a hydration status assessment, consider ascites.
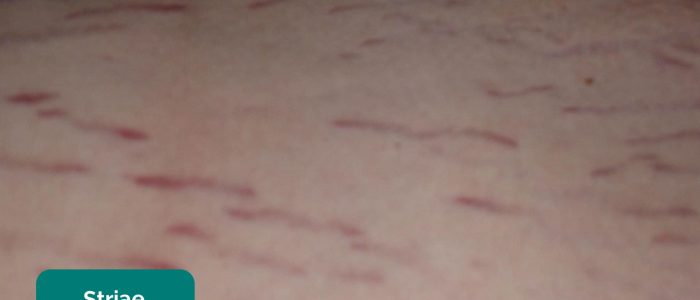
- Striae (stretch marks): caused by tearing during the rapid growth or overstretching of skin (e.g. ascites, intrabdominal malignancy, Cushing’s syndrome, obesity, pregnancy).
Assess shifting dullness
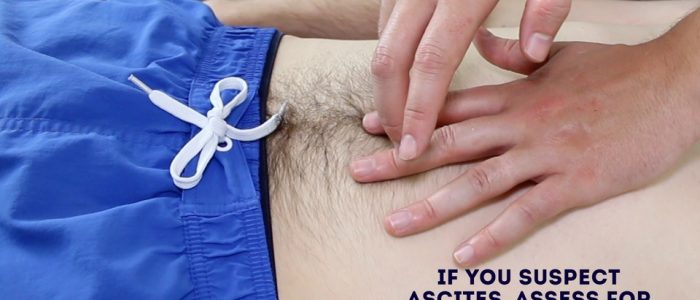
Percussion can also be used to assess for the presence of ascites by identifying shifting dullness:
1. Percuss from the umbilical region to the patient’s left flank. If dullness is noted, this may suggest the presence of ascitic fluid in the flank.
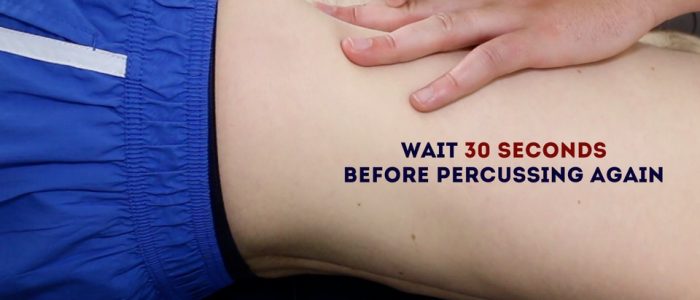
2. Whilst keeping your fingers over the area at which the percussion note became dull, ask the patient to roll onto their right side (towards you for stability).
3. Keep the patient on their right side for 30 seconds and then repeat percussion over the same area.
4. If ascites is present, the area that was previously dull should now be resonant (i.e. the dullness has shifted).
Oedema
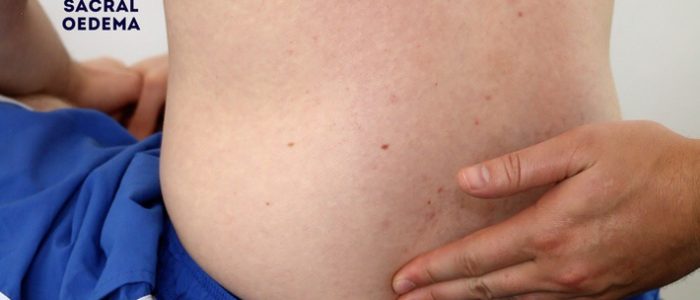
Sacral oedema
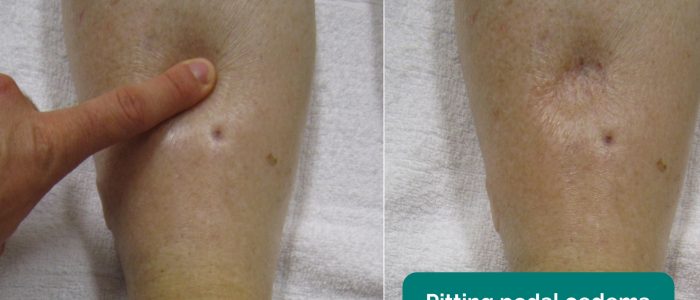
Inspect and palpate the sacrum for evidence of pitting oedema.
Legs
Inspect and palpate the patient’s ankles for evidence of pitting pedal oedema.
To complete the examination…
Explain to the patient that the examination is now finished.
Thank the patient for their time.
Dispose of PPE appropriately and wash your hands.
Summarise your findings.
Further assessments and investigations
Suggest further assessments and investigations to the examiner:
- Measure blood pressure: if not performed already.
- Full blood count: may reveal a raised haematocrit in hypovolaemic patients and a sudden drop in haemoglobin in patients with ongoing haemorrhage.
- Urea and electrolytes: urea/creatinine will be raised in hypovolaemic patients and in those with acute or chronic renal disease. Electrolytes such as sodium may be low in hypervolaemic patients (e.g. dilutional hyponatraemia).
- Further imaging: this could include a chest X-ray to assess for pulmonary oedema, an echocardiogram to assess cardiac function or an abdominal ultrasound to rule out ascites.
- Accurate fluid balance: including daily weights, urine output, fluid intake and stool chart.
- Urine and serum osmolality: if considering syndrome of inappropriate antidiuretic hormone secretion (SIADH) or diabetes insipidus.
References
- Adapted by Geeky Medics. James Heilman, MD. Peripheral pallor. Licence: CC BY-SA.
- Adapted by Geeky Medics. BrotherLongLegs. Leukonychia. Licence: CC BY-SA.
- Adapted by Geeky Medics. James Heilman, MD. Ascites. Licence: CC BY 3.0.
- Adapted by Geeky Medics. PanaromicTiger. Striae. Licence: CC BY-SA.
- Adapted by Geeky Medics. James Heilman, MD. Pedal oedema. Licence: CC BY-SA.