- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Introduction
Necrotising enterocolitis (NEC) is the most common surgical emergency in neonates.1
NEC is an acute inflammatory disease, predominantly affecting preterm infants. It can lead to bowel necrosis, multi-system organ failure and is life-threatening. Prompt recognition of NEC and appropriate treatment is vital.2
NEC occurs in around 12% of low birth weight infants (< 1500g). Due to the advancement of neonatal intensive care, more at-risk infants are surviving long enough for the disease to develop and so the incidence of NEC is increasing.3
Aetiology
NEC is a multifactorial condition and the exact cause is unknown. Damage to the intestinal mucosa can occur due to vascular insults, toxin exposure, infection and genetic factors.
This damage allows pathogenic colonisation of normal commensal bacteria. However, some outbreaks of NEC have been isolated to a pathogenic organism, such as Escherichia coil.3
Risk factors
85% of NEC cases occur in infants who are premature (especially <32 weeks), or with low birth weight.3
Other risk factors include:
- Abnormal dopplers (measuring blood flow from the placenta to baby)
- Antibiotic treatment lasting longer than 10 days or multiple courses of antibiotics
- Enteral feeding
- Use of cow’s milk formula (breastfeeding is protective against NEC)
- Congenital heart disease
Clinical features
History
NEC usually presents at a corrected gestational age of 30 – 33 weeks (i.e., in weeks 3 – 4 of life in a baby born at 28 weeks).
Typical symptoms of NEC include:4
- A new feed intolerance
- Vomiting (which may be bilious) or increasing volume of NG aspirate
- Distended abdomen, which becomes tender and tense
- Haematochezia (fresh blood in the stools)
Other important areas to cover in the history include:
- Feeding history: infants with NEC often have a new onset feed intolerance. Ask about rate of feeding, volume taken, vomiting after food, any changes in food (e.g. from breast to bottle and changes in formula).3
- Bowel movements: ask about normal bowel habits. Has meconium been passed? How often do they open their bowels? This can be quantified by the number of dirty nappies in a day.
- Past medical history: especially respiratory/cardiac history and history of previous infections.
- Pregnancy history: it is important to take a thorough pregnancy history from the parent/carer.
- Family history: ask about a family history of illness in the newborn period. Many neonatal conditions, including NEC, have a genetic predisposition.
Pregnancy history
Key areas to cover in the pregnancy history include:
- Was the mother under hospital-led maternity care (and if so, why)?
- Was this a high-risk pregnancy?
- Did the mother or baby develop any problems during the pregnancy?
- Were any antenatal scans abnormal?
- Pregnancy gestation?
- Method of birth?
- Any complications with the birth (both mother and infant)?
Clinical examination
All unwell infants require a thorough clinical examination. See the Geeky Medics OSCE guide to performing a newborn baby assessment.
Typical clinical findings in NEC include:3
- Abdominal distension, tender to palpation and can feel tense or “wooden”
- Reduced bowel sounds
- Palpable abdominal mass
- Visible intestinal loops
- Signs of sepsis (e.g. lethargy, temperature instability, haemodynamic instability)
Differential diagnoses
The clinical presentation of NEC can appear similar to several other conditions.
Table 1. Differential diagnoses of NEC.
| Condition | Clinical features |
| Sepsis |
Can develop as a complication of NEC. Bacteria can translocate through the inflamed bowel, into the systemic circulation causing sepsis. Other common causes of neonatal sepsis include group B strep infection, premature or prolonged rupture of membranes, chorioamnionitis and maternal septicaemia.6 |
| Intussusception | Intussusception occurs in infants aged between 3 months and 3 years; it is rare in infants. NEC tends to occur corrected gestational age of 30 – 33 weeks. |
| Volvulus | An important differential for the acute abdomen in infancy.3 |
| Hirschsprung’s disease | Hirschsprung’s can cause failure to pass meconium in the first 48 hours of life, NEC does not cause this.8 |
Investigations
Laboratory investigations
Relevant laboratory investigations include:
- Baseline blood tests (FBC, CRP): CRP may be raised and there may be thrombocytopenia and neutropenia.
- Blood cultures: non-specific in NEC and are commonly reported as negative. However, if a bacterial, viral or fungal agent is isolated this can be useful for guiding treatment.9
- Blood gas: may show a raised lactate or acidosis.
Imaging
Relevant imaging investigations include:
- Abdominal ultrasound: ultrasound is a safe first choice of imaging due to the lack of exposure to ionising radiation. Signs that are indicative of NEC include air in the portal system, ascites and perforation.
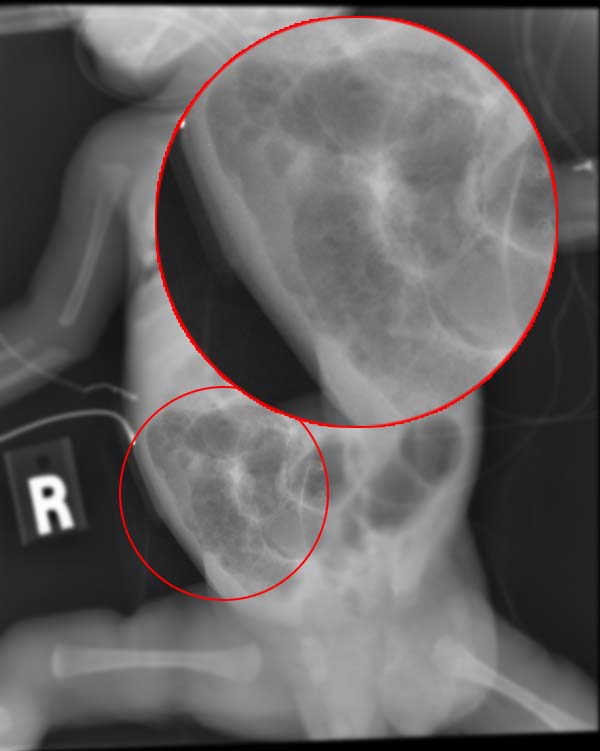
- Abdominal X-ray: first-line imaging when ultrasound is not available (e.g. out of hours). May show thickening of the bowel wall, dilated bowel loops filled with gas, distended bowel and pneumatosis intestinalis (intramural bowel gas, this sign is diagnostic of NEC).10
- If the bowel has perforated, Rigler’s sign may be visible. This occurs when both sides of the bowel wall are visible due to the presence of gas inside the lumen and within the peritoneal cavity.11
Management
Neonates with suspected NEC require urgent review by a paediatric surgeon.
Medical management
Principles of medical management for NEC include:4
- Keep the infant nil by mouth (total parenteral nutrition may be required)
- Consider bowel decompression with a nasogastric tube
- Assess and manage sepsis
- Intravenous fluid resuscitation
- Intravenous antibiotics (broad-spectrum cover is recommended as first-line, such as cefotaxime and metronidazole)
- Circulatory support and ventilation may be required
Surgical management
Surgical management is required in 20-50% of cases.2
According to the modified Bell’s staging criteria, the main indication for surgical intervention is evidence of perforation. A laparotomy is carried out to remove the perforated and necrotic bowel from the abdomen.5
Complications
General complications of NEC include:3
- Bowel perforation
- Disseminated intravascular coagulation
- Sepsis
- Adverse neurodevelopmental outcomes (especially in infants who undergo surgery)
Post-operative complications of NEC include:3
- Short bowel syndrome
- Formation of intestinal strictures
- Enterocolic fistulae
- Abscess formation
In infants who undergo surgery for NEC, a 29% post-surgical mortality rate has been reported at one year.12
Key points
- NEC is the most common surgical emergency in the neonatal period.
- It is most common in underweight, pre-term infants (<32 weeks) fed with cow’s milk formula.
- NEC presents with blood in the stool, problems with feeding and abdominal distension.
- These infants need urgent surgical review and to be made nil by mouth.
- Approximately one in four infants who develop NEC will require surgery
Reviewer
Dr Amanda Gilbert
Paediatric trainee
Editor
Dr Chris Jefferies
References
- Great Ormond Street Hospital for Children. Necrotising Enterocolitis. Published July 2016. Available from: [LINK]
- Shaffner. Roger’s Handbook of Paediatric Intensive Care. Published 2016.
- Patient UK. Necrotising Enterocolitis. Published 2016. Available from: [LINK]
- Barry. Paediatric Intensive Care. Published 2010.
- National Institute for Health and Care Excellence. NG143: Traffic light system for identifying risk of serious illness. Published 2019. Available from: [LINK]
- NICE. Quality Standard 75: Neonatal Infection. Published 2014. Available from: [LINK]
- Patient UK. Intussusception in Children. Published 2016. Available from: [LINK]
- Patient UK. Hirschsprung’s Disease. Published 2018. Available from: [LINK]
- Coggins et al. Infectious Causes of Necrotizing Enterocolitis. Clin Perinatol. Published 2015. Available from: [LINK]
- Lissauer. Illustrated Textbook of Paediatrics. Published 2018.
- Radiopedia. Rigler sign. Published 2020. Available from: [LINK]
- Allin et al. One-year outcomes following surgery for necrotising enterocolitis: a UK-wide cohort study. ADC Fetal & Neonatal Edition. Published 2017. Available from: [LINK]
- Figure 1. WikiRad. X-ray of an infant with necrotizing enterocolitis. License: [CC BY-SA]. Available from: [LINK].




