- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Introduction
Osteoarthritis is a progressive, degenerative joint disorder. The most common joints affected by osteoarthritis are the knees followed by the hips and hands.
In the United Kingdom, 33% of people aged 45 years and over are treated for osteoarthritis.1
Aetiology
Osteoarthritis is often referred to as a dysfunctional ‘wear and repair’ process within the joint. An initial imbalance in cartilage homeostasis leads to cartilage degradation, remodelling of bone and associated inflammation of the joint.
Chondrocytes are responsible for maintaining the homeostasis between synthesis and degradation of the extracellular matrix within articular cartilage. Over time, continuous ‘wear’ or trauma to the joint causes local inflammation and stimulation of chondrocytes to release degradative enzymes. These enzymes break down collagen and proteoglycan and ultimately destroy the articular cartilage.
Over time, the cartilage thins leading to exposure of the underlying subchondral bone. This causes subchondral sclerosis and the continuous remodelling of subchondral bone forms subchondral cysts and osteophytes. This eventually leads to a progressive loss of joint space.2
Risk factors
There is no single cause for osteoarthritis, however, the following risk factors are associated with an increased likelihood of developing the condition:
- Increasing age
- Female sex
- Obesity
- Less commonly, articular congenital deformities or trauma to the joint
Clinical features
History
Typical symptoms of osteoarthritis include:
- Joint pain
- Stiffness: typically, worse after activity and at the end of the day
- Limitation in day-to-day activities
In some cases, patients will experience referred pain. For example, in a patient complaining of pain in their lower spine or knee, the pain could be arising from the hip.
Inflammatory arthropathies vs non-inflammatory arthropathies
The symptom of joint stiffness can be used to differentiate non-inflammatory arthropathies such as osteoarthritis from inflammatory arthropathies such as rheumatoid arthritis.
In inflammatory arthropathies, joint stiffness improves with activity and stiffness typically lasts longer than 30 minutes in the morning.
Clinical examination
All patients presenting with joint pain should have a thorough examination of the relevant joint bilaterally, as well as the joints above and below (e.g. a person complaining of pain in their right hip should have the contralateral hip, ipsilateral knee and spine examined).
For more information, see the Geeky Medics guides to musculoskeletal examinations.
Typical clinical findings in osteoarthritis include:
- Reduced active and passive range of movement (secondary to pain)
- Tenderness over the joint lines
- Crepitus on movement
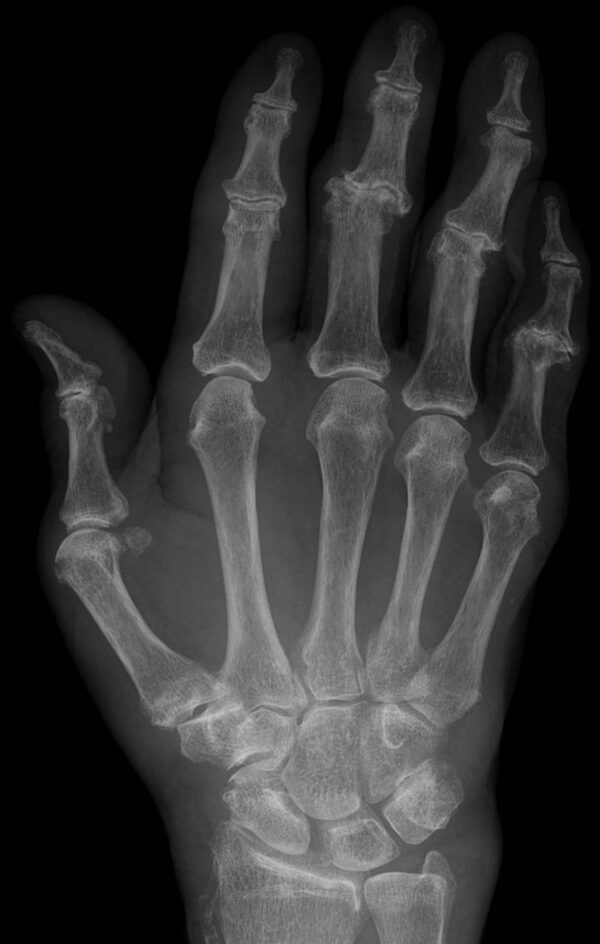
Osteoarthritis of the hands
Osteoarthritis affecting the hands typically presents with more signs than osteoarthritis affecting the larger joints as such as the hip or knee.
Typical clinical findings in the hands include:
- Sparing of the metacarpophalangeal joints
- Bony enlargement of the proximal interphalangeal joints known as Bouchard’s nodes
- Bony enlargement of the distal interphalangeal joints known as Heberden’s nodes
- Squaring of the first carpometacarpal joint (or the base of the thumb)
- Reduced functional movement (e.g. reduced grip strength)
Differential diagnoses
The possible differential diagnoses considered for osteoarthritis depend on the joint affected, but may include:
- Any joint: fracture, inflammatory arthropathies (such as rheumatoid arthritis), crystal arthropathies (such as gout), septic arthritis or malignancy
- Knee: meniscal or ligamentous tears
- Hip: bursitis, avascular necrosis
- Hand: De Quervain’s tenosynovitis
Investigations
Osteoarthritis is primarily a clinical diagnosis. The following are relevant investigations in the context of osteoarthritis.
Bedside investigations
Relevant bedside investigations include:
- Bodyweight and body mass index: obesity is a risk factor for lower limb osteoarthritis and may also aid the development of a management plan
Laboratory investigations
Relevant laboratory investigations include:
- Serum CRP/ESR: if an inflammatory arthropathy is suspected, inflammatory markers should be requested. CRP and ESR are typically normal in osteoarthritis.
Imaging
Relevant imaging investigations include:
- X-ray of affected joints: the most common imaging modality to assess the presence and severity of osteoarthritis
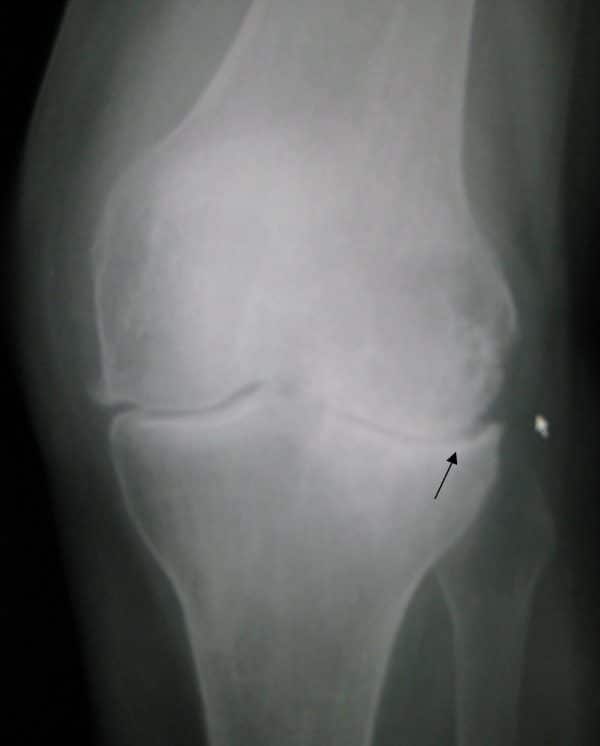
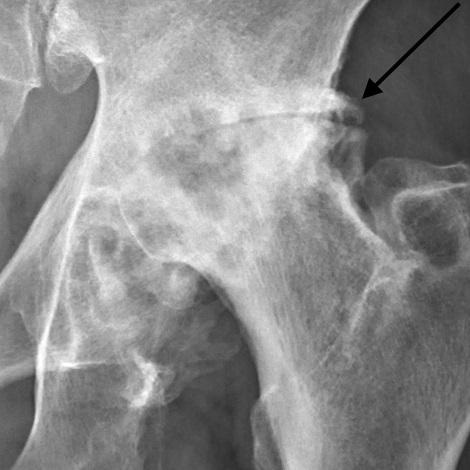
X-ray changes in osteoarthritis
The common changes found on X-ray imaging with osteoarthritis can be memorised using the mnemonic ‘LOSS’:
- Loss of joint space
- Osteophytes
- Subchondral sclerosis
- Subchondral cysts
More details about interpretation and examples of musculoskeletal X-rays can be found in the Geeky Medics guide to musculoskeletal X-ray interpretation.
Diagnosis
Current NICE guidelines advise that osteoarthritis can be diagnosed clinically if a person meets the below criteria:2
- ≥ 45-year-old and
- has activity-related joint pain and
- has either no morning joint-related stiffness or morning stiffness that lasts no longer than 30 minutes
Management
Conservative management
Conservative management is the first-line treatment for osteoarthritis. NICE recommends the following:
- Education and advice about their condition
- Exercise: both muscle strengthening and general aerobic fitness
- Weight loss (if overweight or obese)
Medical management
Medical management involves the prescription of analgesics in a stepwise approach and is commonly used alongside conservative management:2
- First-line: topical non-steroidal anti-inflammatory drugs (NSAIDs)
- Second-line: paracetamol and topical analgesia
- Third-line: NSAID, paracetamol and topical capsaicin
- Fourth-line: opioid, NSAID, paracetamol and topical capsaicin
Intra-articular corticosteroid injection can be offered for acute exacerbation of pain despite regular use of the above analgesia. Typically, these are performed in an outpatient clinic environment. The injection consists of both a steroid and local anaesthetic, the latter providing immediate symptomatic relief to the patient for the first few hours. Patients may experience a worsening of symptoms for the first few days after administration, this is known as the ‘steroid flare’.
Surgical management
If pain persists despite conservative and medical management or severe disability is present, surgical management may be considered. Most commonly, this is in the form of joint replacement (arthroplasty) or fusion of the joint (arthrodesis).
Key points
- Osteoarthritis is a degenerative joint condition, common in the ageing population.
- The most common joint affected by osteoarthritis is the knee.
- Important risk factors to consider with osteoarthritis include age, female sex and obesity.
- The most common symptoms include joint pain, joint stiffness and limitation in day-to-day activities.
- The most common finding on clinical examination is a reduced range of movement.
- Plain X-rays are the primary investigation.
- Conservative management involves patient education on weight loss and exercise.
- Medical management involves analgesia.
- Surgical management involves the replacement or fusion of affected joints.
Reviewer
Miss Charlotte Cross
Trauma and Orthopaedic Consultant
Editor
Dr Chris Jefferies
References
- Versus Arthritis. The state of musculoskeletal health 2019: arthritis and other musculoskeletal conditions in numbers. Published in 2019. Available from: [LINK]
- GS Man, G. (2014). Osteoarthritis pathogenesis – a complex process that involves the entire joint, Journal of Medicine and Life, 7(1), p. 37. Available from: [LINK]
- Hellerhoff. Adapted by Geeky Medics. Hand OA. License: [CC BY-SA]
- James Heilman, MD. Adapted by Geeky Medics. Knee OA. License: [CC BY-SA]
- Mikael Häggström. Adapted by Geeky Medics. Hip OA.License: [Public domain]
- NICE. Recommendations | Osteoarthritis: care and management | Guidance | NICE (2014). Available from: [LINK]