- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Introduction
Benign paroxysmal positional vertigo (BPPV) is an inner ear disorder characterised by recurrent brief attacks of positional vertigo.1 BPPV is the commonest cause of vertigo.2
The use of the word ‘benign’ reflects the good prognosis of BPPV, as its cause is likely peripheral rather than central.5 However, undiagnosed and untreated cases of BPPV may significantly affect patients with increased risk of falls and reduced quality of life.6
‘Paroxysmal’ refers to the sudden and rapid onset of vertigo with certain head movements.3
Vertigo is an illusory sensation of motion of either oneself or the surroundings in the absence of true motion.3 Positional vertigo is the provoking of a spinning sensation by changes in head position in relation to gravity (e.g. rolling over in bed, bending over and looking upward).4
Aetiology
Anatomy of the inner ear
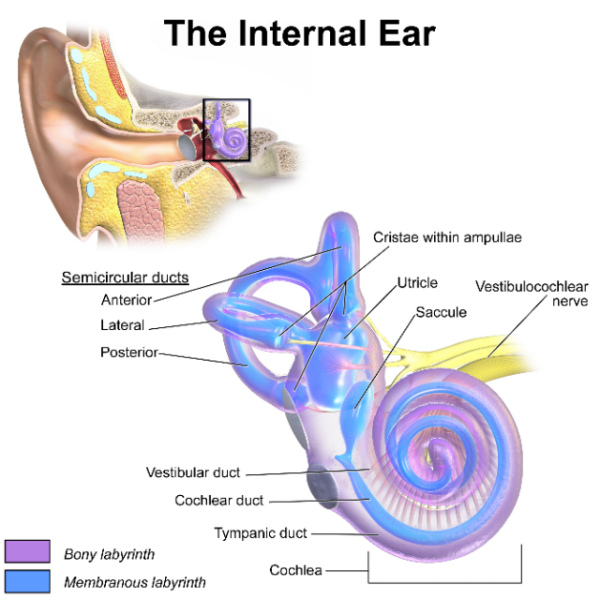
The inner ear consists of two parts, the bony labyrinth and the membranous labyrinth (Figure 1):
- The bony labyrinth comprises cavities in the petrosal part of the temporal bone. It holds the cochlea, vestibule and semi-circular canals.
- The membranous labyrinth sits inside the bony labyrinth. It consists of the cochlear duct, semi-circular ducts, utricle and saccule.
The cochlea is regarded as the spiral organ for hearing. The semi-circular ducts, saccule and utricle form the vestibular apparatus, which assists with balance.
The semi-circular ducts, within the semi-circular canals, have three individual parts that connect at the utricle (located anteriorly to the saccule in the vestibule). The three components are named in regards to their anatomical position – anterior, lateral and posterior semi-circular ducts.
The planes of these semi-circular canals form obtuse angles to one another. These ducts are filled with a fluid called endolymph. They also have enlarged ends when they reach the utricle, called ampullae. The ampulla contains sensory receptors which detect changes in the flow of endolymph with head movements. This sends signals to the brain for balance control.8,9
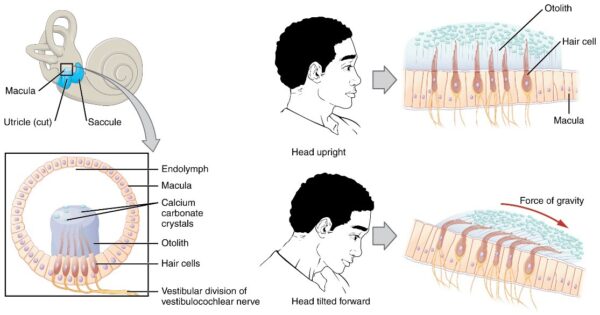
Another important component of the vestibular system is the otoconia. These are bio-crystals present in the utricle and saccule (Figure 2).
They are located above the hair cells (kinocilia and stereocilia) in the macula (sensory epithelium), which is found in the utricle and saccule. The otoconia are displaced with head movements, leading to the depolarisation of sensory hair cells. This further generates electrical signals relayed to the CNS by the vestibular nerve. In turn, this stimulates the CNS to respond with appropriate responses and ensures the maintenance of balance.10
Pathophysiology
The posterior canal is most commonly affected in BPPV. However, the lateral, anterior or multiple canals can be affected.
One of the most understood and accepted theories for the posterior semi-circular canal is canalolithiasis. This describes the displacement of free-floating otoconia particles from the macula that then become trapped in the posterior canal.
The detached otoconial debris, in addition to the endolymph, may continue to stimulate hair cells even after head movements have ceased. This leads to an abnormal sensation of vertigo and nystagmus when the head moves in the plane of the affected semi-circular canal.1,2,3,12
Causes of BPPV
Most cases of BPPV are idiopathic.
Other known causes of BPPV include:
- Head injury
- Vestibular neuronitis (post-viral illness)
- Labyrinthitis (due to age-related degeneration of the labyrinth)
- Complications of mastoid/stapes surgery
Risk factors
Risk factors for the development of BPPV include:
- Older age (onset common between 40 to 60 years old).
- Female sex (women are twice as likely to have BPPV compared to men)
- Meniere’s disease (usually diagnosed alongside BPPV in 30% of cases)
- Patients with migraines and/or anxiety disorders2
Clinical features
History
Typical symptoms of BPPV include:
- Brief episodes of vertigo usually lasting 30 seconds to 1 minute
- Symptoms provoked by head movements such as rolling over in bed, gazing upwards (e.g. when placing an object on a shelf), bending forward (e.g. when tying shoe laces, sitting down)
Less common symptoms include:
- Nausea
- Light-headedness, imbalance (as a result, patients may present with a fall – hence, it is crucial to consider vestibular dysfunction; see the Geeky Medics guide to the assessment of falls)
Clinical examination
Typical clinical findings of BPPV include:
- Dix-Hallpike test positive: leading to rotational vertigo and nystagmus
Investigations
Currently, there are no investigations that can identify the location and movement of otoconia.
Dix-Hallpike test
The current gold-standard test to elicit BPPV is the Dix-Hallpike test (DHT). A positive DHT will confirm posterior semi-circular canal BPPV, with its 82% sensitivity and 71% specificity.13
If the test is positive, there will be:
- Latency period: the onset of nystagmus after 5 to 20 seconds
- Vertigo
- Rotatory and vertical nystagmus (up-beating and towards the affected ear)
These symptoms will begin gradually with the latency period, then increase intensely and decline gradually due to fatigability.
Once the patient returns to sitting, there is prolonged vertigo and reversal of the nystagmus. If any of these features are absent (no latency, no vertigo and persisting nystagmus), investigate for a central cause of vertigo.
In addition, BPPV is generally unilateral. Therefore positive movements will often be in one eye. If the test is bilaterally positive, this could suggest a lateral semi-circular canal BPPV, vestibular neuritis, or a central cause.2
Contraindications to DHT include:
- Patients with neck- or back-related pathology (i.e. severe rheumatoid arthritis, cervical stenosis, spinal cord injury, vertebral artery disease or carotid stenosis).2
Differential diagnoses
It is important to identify any negative symptoms as these may point towards other conditions. Crucial negatives to be established are:
- Persistent vertigo: indicative of Meniere’s disease
- Tinnitus, hearing loss or aural fullness: indicative of Meniere’s disease, labyrinthitis
- Long and gradual onset, viral prodrome: indicative of vestibular neuronitis, labyrinthitis
- Visual, speech, motor or sensory loss: indicative of a CNS lesion
- Vertical/down-beating nystagmus: indicative of a CNS lesion
Further differentiating features between common otologic, neurological and other diseases can be found in Table 1.
Table 1. Differential diagnoses of BPPV
| Differential diagnoses of BPPV | Characteristic differentiating symptoms |
| Otologic diseases | |
| Meniere’s disease | Sustained vertigo, fluctuating loss of hearing, aural fullness, and tinnitus in the affected ear |
| Vestibular neuronitis | Follows a viral prodrome, potential tinnitus; gradual onset |
| Labyrinthitis | Follows a viral prodrome, hearing loss, tinnitus may occur; gradual onset |
| Neurological diseases | |
| Vestibular migraine | Symptoms may last from 5 mins to 72 hours, current history of migraines (with other features – e.g. headache, photophobia, visual aura etc) |
| Brainstem/cerebellar stroke (or transient ischaemic attack) | Very sudden onset, other neurological symptoms – dysarthria, dysphagia, sensory/motor loss |
| Other diseases | |
| Cervical vertigo | History of degenerative cervical spine disease |
| Medication-induced | Carbamazepine, phenytoin, and antihypertensives may produce side effects of vertigo and/or dizziness |
Management
Conservative management
BPPV is often a self-limiting condition, and symptoms may subside within 6 months of onset.3 Patients should be advised to:
- Avoid positions that may provoke vertigo symptoms
- Counsel that symptoms may re-occur. One study identified a 36% symptom recurrence rate within 48 months of onset.14
Medical management
If symptoms persist, vestibular rehabilitation should be performed. This can be done with either:
Repositioning techniques
One of the recommended techniques for posterior canal BPPV is the Epley manoeuvre. The aim is to reposition the displaced otoconial particles back into the utricle from the posterior canal.
Other techniques include the Semont manoeuvre, the Brandt-Daroff exercises and the modified Epley manoeuvre (the latter two can be performed at home by the patients once they are taught the steps).
Medications
Medications which may be considered include:
- Anti-emetics: prochlorperazine or cyclizine
- Vestibular sedatives: cinnarizine or betahistine (histamine analogue)
However, the literature suggests that these medications have little effect on controlling symptoms.15
Surgical management
Surgical intervention is usually reserved for patients with intractable symptoms who have failed to respond to repeated repositioning procedures. The two surgical options are:2
- Denervate the posterior semi-circular canal (by singular neurectomy)
- Obliterate the posterior canal (via a trans-mastoid approach)
Patient education
It is important to also counsel on other aspects of a patient’s life:
- Advise the patient not to drive when they feel dizzy or if the driving provokes the episodes.
- Advise the patient to inform their employer where it may pose an occupational hazard (e.g. working with machinery, at heights etc).
Key points
- BPPV is an inner ear disorder characterised by repeated episodes of positional vertigo
- The vertigo is provoked by certain head movements, such as rolling over in bed, looking upward etc…
- It is more common in women (2:1), and patients >40 years old
- Most cases of BPPV are idiopathic; known secondary causes include head injury and vestibular neuronitis/labyrinthitis
- Symptoms include vertigo, provoked by head movements, lasting 30 seconds to 1 minute, with associated nausea, light-headedness and imbalance.
- The main investigation is the Dix-Hallpike test.
- Management is usually supportive. If symptoms persist, patients may be treated with the Epley manoeuvre.
- BPPV is generally self-limiting
Reviewers
Ms Shadaba Ahmed and Dr Elizabeth Cotzias
Consultant ENT Surgeon and ENT Registrar
Editors
Hannah Thomas
Dr Chris Jefferies
References
- GP Notebook. BPPV. Available from: [LINK]
- Benign Paroxysmal Positional Vertigo. Published in 2016. Available from: [LINK]
- Bhattacharyya, N et al. Clinical Practice Guideline: Benign Paroxysmal Positional Vertigo (Update). Published in 2017. Available from: [LINK]
- Joseph Furman and Stephen Cass. Benign Paroxysmal Positional Vertigo. Published in 1999. Available from: [LINK]
- Baloh RW, Honrubia V, Jacobson K. Benign positional vertigo: clinical and oculographic features in 240 cases. Published in 1987. Available from: [LINK]
- Lopez-Escamez JA, Gamiz MJ, Fernandez-Perez A, et al. Long-term outcome and health-related quality of life in benign paroxysmal positional vertigo. Published in 2005. Available from: [LINK]
- Bruce Blaus. Internal Ear Anatomy. [CC BY-SA]
- Ekdale EG. Comparative Anatomy of the Bony Labyrinth (Inner Ear) of Placental Mammals. Published in 2013. Available from: [LINK]
- OpenStax. Hearing and vestibular sensation. Published in 2021. Available from: [LINK]
- Lundberg YW, Xu Y, Theissen KD, Kramer KL. Mechanisms of Otoconia and Otolith Development. Published in 2015. Available from: [LINK]
- OpenStax College. Maculae and Equilibrium. [CC BY-SA]
- Andrew Baldwin, Nina Hjelde, Charlotte Goumalatsou and Gil Myers. Oxford Handbook of Clinical Specialties 10th Ear, Nose and Throat. Published in 2016. Available from: [LINK]
- Lopez-Escamez JA, Lopez-Nevot A, Gamiz MJ, et al. Diagnosis of common causes of vertigo using a structured clinical history. Published in 2000. Available from: [LINK]
- Cochrane Library. The Epley (canalith respositioning) manoeuvre for benign paroxysmal positional vertigo. Published in 2014. Available from: [LINK]
- Cochrane library. Modifications of the Epley (canalith repositioning) manoeuvre for posterior canal benign paroxysmal positional vertigo (BPPV). Published in 2012. Available from: [LINK]




