- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Introduction
Bronchiolitis is characterised by narrowing of the lower respiratory tract due to inflammation of the bronchioles and build-up of mucus. It is a common respiratory condition in infancy. Around a third of infants develop bronchiolitis before the age of 1, with a peak incidence around 3 to 6 months of age.1
The incidence of bronchiolitis is linked with the winter period. Typically, children present during this time with episodes of bronchiolitis lasting for 7-10 days.2,3
Aetiology
Bronchiolitis is usually caused by a viral infection. About 80% of cases are caused by the respiratory syncytial virus (RSV). The other less common viral causes of bronchiolitis include:
- Parainfluenza virus
- Rhinovirus
- Adenovirus
- Influenza
- Human metapneumovirus
Risk factors
Risk factors for admission to hospital with a severe episode of bronchiolitis include:
- Chronic lung disease
- Congenital heart disease
- Younger than 3 months old
- Prematurity
- Down’s syndrome
- Cystic fibrosis
- Neuromuscular disease2,4
Clinical features
History
Typical symptoms of bronchiolitis include:
- Persistent cough
- Wheeze
- Shortness of breath
- A prodrome of upper respiratory tract features – fever, runny nose, cold
- Symptoms typically worsen during the 2nd or 3rd night of illness
Other symptoms can include:
- Apnoea – in infants younger than 6 weeks of age, also typically seen with RSV
- Poor feeding – young children are obligate nasal breathers, making it difficult to feed and breathe at the same time during bronchiolitis
- Symptoms of dehydration in severe disease – reduced urine output or fewer wet nappies
Other important areas to cover in the history include:
- Past medical history including birth history – ask about known risk factors for severe bronchiolitis, as listed above
- Medications/allergies – this information may be useful if there are other possible differentials
- Family history – ask if anyone in the family has been unwell, this may point towards other differentials. It is also essential to ask about any family history of atopic conditions
- Social history – ask about parental smoking, as this will exacerbate symptoms of bronchiolitis. Also ask about the child’s situation at home (e.g. where they live, who is at home with them, the involvement of social services), as difficult social circumstances will reduce the threshold for admission.
Clinical examination
Typical clinical findings in bronchiolitis include:
- Bilateral polyphonic expiratory wheeze
- Tachypnoea
- Tachycardia
- Low-grade fever (<39o)
- Irritability
Other clinical findings can include:
- Prolonged capillary refill time (>2 seconds)
- Cyanosis
- Signs of dehydration – dry mucous membranes, sunken fontanelle in young babies5
- Reduced conscious level6
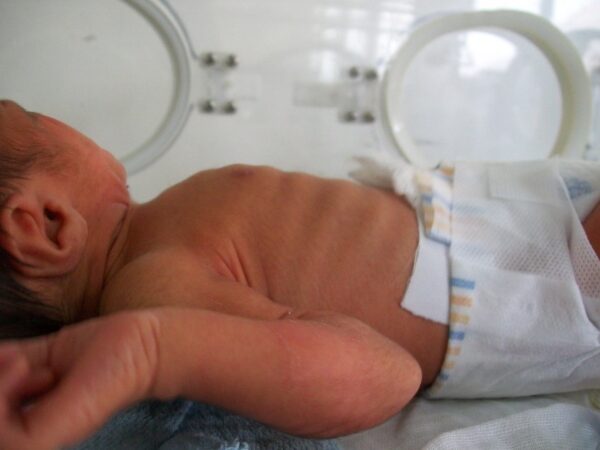
- Recessions (intercostal, subcostal or sternal) – this is a result of children having a compliant rib cage, which makes an increased work of breathing clearly visible externally.
Differential diagnoses
Table 1. Differential diagnoses of bronchiolitis
| Differential diagnosis | Features differentiating from bronchiolitis |
| Pneumonia |
|
| Viral-induced wheeze |
|
| Early-onset asthma |
|
| Bordetella pertussis or whooping cough |
|
| Gastro-oesophageal reflux |
|
| Foreign body aspiration |
|
| Chronic heart disease or failure |
|
Investigations
Children are diagnosed clinically with bronchiolitis if they present with coryzal symptoms lasting up to 3 days, followed by:
- Persistent cough and
- Tachypnoea or chest recession and
- Wheeze or crackles on chest auscultation.4
Investigations do not influence the treatment of bronchiolitis.
Bedside investigations
- Pulse oximetry: children should be admitted if oxygen saturation is <92% 4
Laboratory investigations
- Blood tests (including arterial blood gases): these are not routinely performed
Imaging
- Chest X-ray: not routinely performed, but if there is an area of the lung with reduced air entry or focal crackles, this can be used to rule out pneumonia or pneumothorax.2
Management
Bronchiolitis is typically self-limiting. Not all children with bronchiolitis will require admission to hospital. If a child does not require admission, it is important to provide safety netting to the parents or guardians to return if symptoms get worse.
The criteria for admission to secondary care depends on several factors including:
- Apnoea
- Reduced oxygen saturation: <92%
- Reduced oral intake: <50-75% of normal
- Persistent respiratory distress: significant chest recessions, grunting
- Presence of risk factors for severe disease, as mentioned earlier
- Difficult social factors: living very far from the hospital, lack of parental confidence4
The management of bronchiolitis is supportive:
- Oxygen supplementation if saturations are persistently <92%.
- Positive pressure such as high flow oxygen or CPAP may be required for respiratory distress. If these fail to work, intubation and ventilation may be required.
- Nutritional and fluid supplementation – oral, nasogastric (NG) tube or intravenous (IV). Depending on the severity of the bronchiolitis, a stepwise approach may be considered:
- Small and frequent oral feeds,
- NG tube placement with small and frequent NG bolus feeds,
- Continuous NG feeds,
- IV fluids
- Support parents/guardians with smoking cessation.
Important points to note:
- Bronchodilators are not effective as respiratory tract narrowing is due to increased secretions, not bronchoconstriction.
- Antibiotics are also not effective due to the viral aetiology of bronchiolitis. 4,5
Complications
If bronchiolitis is not diagnosed and treated, complications can include:
- Clinical dehydration
- Syndrome of inappropriate antidiuretic hormone (SIADH) and subsequent hyponatraemia. Because of the risk of SIADH, some guidelines will advocate for 2/3 maintenance NG/IV fluids, please refer to local guidelines.
- Apnoea and respiratory failure requiring intubation and ventilation.6
Key points
- Bronchiolitis is characterised by narrowing of the lower respiratory tract due to inflammation of the bronchioles and build-up of mucus.
- Bronchiolitis is usually caused by a viral infection. About 80% of cases are caused by the respiratory syncytial virus (RSV).
- The diagnosis is clinical, with investigations rarely indicated.
- Bronchiolitis is typically self-limiting. Not all children with bronchiolitis will require admission to hospital.
- Management is supportive: oxygen supplementation, high flow oxygen and treatment of dehydration.
- Complications can include dehydration, SIADH, apnoea and respiratory failure.
References
- Patient. Bronchiolitis. Published in 2018. Available from: [LINK].
- Goldstein H. Published in 2013. Available from: [LINK].
- Spottingthesickchild. Symptoms: Difficulty in Breathing. Published in 2020. Available from: [LINK].
- NICE Guidelines. Bronchiolitis in children: diagnosis and management. Published in 2015. Available from: [LINK].
- Bronchiolitis (and RSV) in infants and children (Beyond the Basics). Published in 2019. Available from: [LINK].
- West Sussex Children & Young People’s Urgent Care Network. Bronchiolitis Pathway and Assessment in Acute Settings for Children 0-2 years. Published in 2011. Available from: [LINK].
- Wikimedia Commons. Intercostal recessions in a newborn with breathing difficulties. License: [CC BY-SA]. Available from: [LINK].
- Bronchiolitis in Infants and Children: Clinical Features and Diagnosis. Published in 2020. Available from: [LINK].
Reviewer
Dr Hannah Murch
Paediatric Emergency Medicine Consultant
Editor
Arunachalam Soma




