- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
A 66 year old man is brought to his GP by his daughter, who is concerned he “just isn’t himself”. She feels he is confused and has slept most of the past two days. Work through the case to reach a diagnosis.
UK Medical Licensing Assessment (UKMLA)
This clinical case maps to the following UKMLA presentations:
- Confusion
History
Screen for confusion
Use the abbreviated mental test score (AMTS) or other tools (e.g. six-item cognitive impairment test) to assess the patient for evidence of confusion:
- Age
- Time (nearest hour)
- Address for recall at the end of the test (get the patient to repeat back to you, to ensure it has been heard correctly e.g. “42 West Street”).
- Year
- Name of this place
- Identification of two people (e.g. doctor/nurse)
- Date of birth
- The year that World War 1 occurred
- The name of the present monarch
- Count backwards from 20 to 1
Address from question 3 recalled correctly?
Patient’s response
- He remembers his name but struggles with his date of birth.
- He believes the year is 1978 and he is at home.
- His overall score is 5/10
History of presenting complaint
Insight:
- Ask the patient if they are aware of any periods in which they felt confused (sometimes patients are aware of their confusion if it has been intermittent).
Mood:
- Depression can present with symptoms similar to those this patient is presenting with.
Appetite and weight:
- If the patient’s weight has changed, clarify if this was intentional.
- Try to get an idea of the amount of weight loss and the time period this occurred over (e.g. 3kg of unintentional weight loss over 2 months).
Recent trauma:
- Ask about recent falls or other trauma (particularly head injuries).
Headaches:
- Location
- Duration
- Timing (e.g. worse in the morning)
- Frequency
- Exacerbating factors (e.g. worse when lying flat)
- Relieving factors (e.g. improved on standing)
Nausea and/or vomiting:
- Duration
- Frequency
- Onset
- Triggers
Pain elsewhere:
- Site
- Onset
- Character
- Radiation
- Associated symptoms
- Timing
- Exacerbating/relieving factors
- Severity
Recent infections:
- Clarify the type of infection
- Duration
- Clarify if symptoms have fully resolved
- Ask about specific infection symptoms (e.g. productive cough, fever, dysuria, sore throat, abdominal pain)
Past medical history
- Pre-existing medical conditions
- Surgical procedures
- Allergies
Medication history
Regular medications:
- Anticoagulants and antiplatelets – relevant if considering haemorrhage
- Analgesia (e.g. opiates or other analgesics can cause confusion)
Over-the-counter medications:
- May cause drowsiness (e.g. antihistamines)
- May interfere with drug metabolism (e.g. St John’s Wart decreases the effect of warfarin)
Social history
Living situation:
- Accommodation (e.g. important when considering falls risk)
- Clarify if the patient lives with anyone else
- Ask if the patient is coping with their activities of daily living
Alcohol history:
- Amount of alcohol consumed each day/week
- Frequency of drinking
Smoking history:
- Duration of smoking
- Number of cigarettes smoked each day on average
Recreational drug use:
- It is important to rule this out when patients present with confusion.
Answer
The patient denies any headache but appears rather blank as you continue to ask further questions, failing to provide meaningful answers.
When presented with a confused patient, a collateral history from a friend or relative is particularly valuable. In this scenario, it would make sense to ask the patient’s daughter questions to gain further insight into the patient’s baseline versus how they are currently presenting.
- When your father is well, what is his baseline level of function?
- Has your father ever been confused in the past?
- Do you feel your father is coping at home at the moment?
- Are you aware of your father recently experiencing any falls or other trauma?
- Do you know if your father has any medical conditions and if he has previously undergone any surgical procedures?
- Do you know if your father takes any regular medications or anything over the counter?
- Have your father’s medications been changed recently?
- Does your father drink alcohol, smoke or take recreational drugs?
Daughter’s response
His daughter states that he is normally “fully with it” and hasn’t been confused in the past, remaining fully independent at home. She isn’t aware of any recent trauma but has noticed he has become increasingly unsteady on his feet over the last 6 months. She knows her father is on some blood pressure tablets and also on warfarin for “a funny heart rhythm”. She last took him to have a blood test to “check his warfarin is working ok” about 4 weeks ago. She denies any knowledge of her father taking recreational drugs and he doesn’t drink alcohol or smoke.
Clinical examination
On examination, the patient appears confused but alert. He can obey commands, and his eyes open spontaneously.
On general inspection, you notice some abrasions to his left shoulder and left ear, with mild bruising on his head just posterior to the left ear.
14
For more information on calculating GCS, see our guide to the Glasgow Coma Scale.
Clinical findings
Neurological examination of the upper and lower limbs:
- Normal tone
- Power MRC grade 4/5 in the right arm
- Power normal in all other limbs
- Brisk right biceps and triceps reflex
- Reflexes normal in all other limbs
- Normal co-ordination
- Normal sensation
- Mild right pronator drift
Cranial nerves:
- No deficits noted
Investigations
Imaging
This man needs hospital admission for a CT head.
Other investigations
- Blood tests (FBC, U&Es, CRP, Bone profile, Magnesium, TFTs) – useful to screen for potential causes of confusion (e.g. electrolyte abnormality, infection, hypothyroidism)
- Urinalysis: urinary tract infections are a common cause of confusion/falls in the elderly
- INR:
- Warfarin is monitored using measurements of a patient’s INR
- A raised INR increases the risk of haemorrhage
Investigation results
- FBC – anaemia
- U&Es, CRP, Bone profile, Magnesium, TFTs – normal
- INR – 7.3
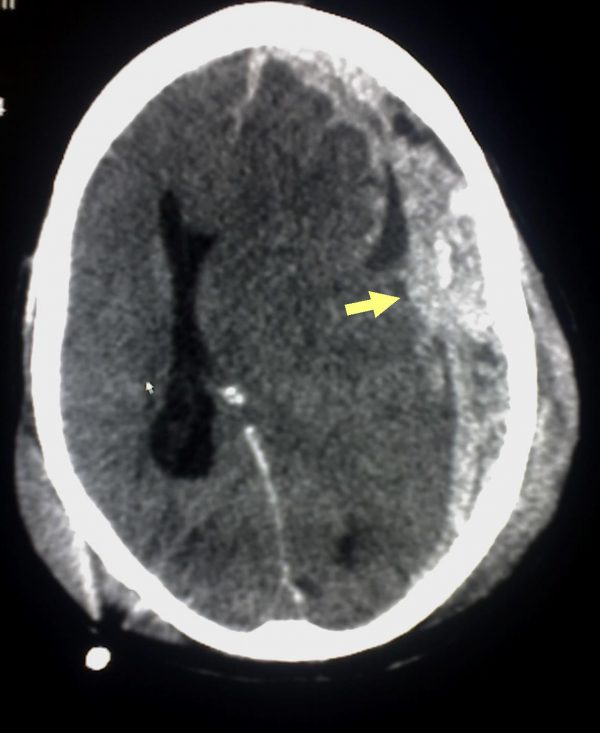
- CT head (shown below)

Diagnosis
Left subdural haematoma (no midline shift), likely secondary to an unwitnessed fall in the context of a raised INR.
Hospital admission
Whilst on the ward, the patient has another fall. Shortly afterwards, his GCS begins to deteriorate.
His eyes are now only opening to pain, he is demonstrating a withdrawal response to pain and making incomprehensible sounds.
8
A potential extension of the subdural haematoma and/or a new acute intracranial bleed causing raised intracranial pressure.
A seizure is also a possible explanation for the sudden drop in GCS. However, there is no mention of other typical seizure symptoms (e.g. jerking).
- An anaesthetist should be asked to urgently review the patient as his current GCS increases the risk of airway compromise.
- A GCS of 8 or below indicates a significant risk of airway obstruction.
- There is an extension of the left subdural haematoma
- Midline shift is now present.
- There is some new extra-axial soft tissue swelling on the left
Management
Burr hole evacuation of the acute subdural haematoma by the neurosurgical team.
You must contact the on-call haematologist for advice on warfarin reversal before surgery.
Vitamin K (not appropriate in this scenario as the onset of action is too slow):
- Warfarin works by inhibiting the recycling of active vitamin K, reducing its availability. This, in turn, decreases the availability of vitamin K dependent clotting factors (II, VII, IX, and X).
- Giving vitamin K replenishes active vitamin K and allows the production of the vitamin K dependent clotting factors.
- Administered orally, it reduces the INR within 24-48 hours.
- Administered intravenously, it reduces INR significantly within 12-14 hours.
- In this situation, active bleeding needs to be managed urgently. As a result, vitamin K would not be a sufficient solution, given it will take at least 12 hours to have an effect.
Octaplex / Beriplex:
- These contain a combination of blood clotting factors II, VII, IX and X, as well as protein C and S. They are highly effective at reversing warfarin’s anticoagulant effects.
- They can rapidly replace clotting factors in emergencies, under the guidance of a haematology specialist.
References
- CT scan image. By Lucien Monfils (Own work). Licence: CC BY-SA 3.0 via Wikimedia Commons. Available here: [LINK]
- Glitzy queen00. Public domain. Available from: [LINK]