- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Introduction
Shoulder dystocia is a complication of vaginal cephalic delivery when the anterior fetal shoulder becomes stuck on the maternal pubic symphysis resulting in delayed birth of the baby’s body.
Shoulder dystocia is an obstetric emergency and occurs in about one in 150 vaginal births. If there is a delay to delivery, there is a risk of hypoxic brain injury for the baby.
Aetiology
Shoulder dystocia usually occurs unexpectedly during childbirth and is not predictable.
Pathophysiology
When shoulder dystocia occurs the baby’s head is delivered but the shoulders prevent progression. This happens because the shoulders, at the point of the head being delivered, are only just reaching the pelvic floor therefore they are still negotiating the pelvic outlet (see the Geeky Medics article on the mechanism of labour).
The shoulder compression may cause the umbilical cord to become compressed between the baby’s body and the mother’s pelvis or the baby’s neck may be compressed at an angle that limits blood flow.
Interruption of the oxygen supply may cause hypoxic brain injury potentially resulting in permanent functional change.
The longer the baby is trapped, the greater the risk of hypoxic injury. However, the overall incidence of brain injury remains low in shoulder dystocia as prompt management improves outcomes.
Risk factors
Pre-labour risk factors for shoulder dystocia include:1
- Previous shoulder dystocia
- Macrosomia >4.5kg
- Diabetes mellitus
- Maternal body mass index >30
- Induction of labour
Intrapartum risk factors for shoulder dystocia include:
- Prolonged first stage of labour
- Secondary arrest: no change in cervical dilation over time.
- Prolonged second stage of labour
- Oxytocin augmentation
- Assisted vaginal delivery
Shoulder dystocia is more likely in babies with higher birth weights, but it should be noted that there is no difficulty delivering the shoulders in most babies over 4.5kg.
If a woman has diabetes the risk is significantly higher even with a similar-sized baby. If a woman has pre-existing diabetes or develops diabetes in pregnancy, they will usually be offered early labour induction or a planned caesarean to reduce/eliminate the risk of shoulder dystocia.
Clinical features
History
Shoulder dystocia is an obstetric emergency often with no features or warning signs therefore history is less relevant to this diagnosis.
Clinical examination
Typical clinical findings of shoulder dystocia during delivery include:
- Slower delivery of the head
- Unable to deliver the anterior shoulder after the delivery of the head with the next contraction
- Turtleneck sign: the appearance and retraction of the baby’s head (like a turtle withdrawing into its shell), with a red, puffy face.
Differential diagnoses
Possible differential diagnoses in the context of shoulder dystocia include:
- Congenital abnormality preventing easy delivery of the baby
Investigations
There are no immediate relevant investigations as shoulder dystocia is a time-critical obstetric emergency requiring urgent intervention.
Following delivery, assessment and investigations for shock and haemorrhage need to be performed quickly.
Bedside investigations
Relevant bedside investigations include:
- Vital signs: monitoring for shock
Laboratory investigations
Relevant laboratory investigations include:
- Full blood count
- Crossmatch and group and save: possibility of post-partum haemorrhage as a complication
Management
Initial management
Initial management of shoulder dystocia includes:
- Call for help: obstetric emergency (senior obstetrician, senior midwife and paediatrician will need to be present)
- Advise the mother to stop pushing: can worsen the fetal impaction.
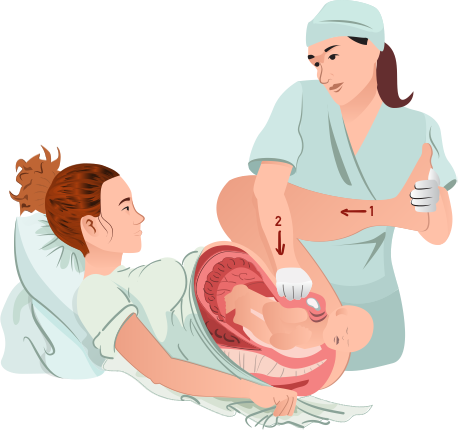
- McRoberts manoeuvres (first line): hyperflex maternal hips (Figure 1 number 1) to widen the pelvic outlet. This alone has a success rate of about 90% which is even higher when combined with suprapubic pressure. Suprapubic pressure is pressure applied behind the anterior shoulder to disimpact it from the maternal symphysis (Figure 1 number 2).
If first-line manoeuvres are not successful, second-line internal manoeuvres include:
- Posterior arm: inserting the hand posteriorly to grasp the posterior fetal arm and deliver
- Internal rotation (‘corkscrew’): simultaneously applying pressure in front of one shoulder and behind the other. The aim is to rotate the baby 180 degrees.
An episiotomy can allow more space to facilitate internal vaginal manoeuvres but will not relieve the bony obstruction of the shoulder. The use of an episiotomy will not decrease the risk of brachial plexus injury.
Always avoid downwards traction on the fetal head as this increases the risk of brachial plexus injury.
Post-delivery management
Post-delivery management includes:
- Active management of the third stage of labour is recommended due to the increased risk of post-partum haemorrhage
- Shoulder dystocia can be a traumatic experience for the mother and birth partner, provide support and debrief the following delivery
- A rectal examination should be performed to exclude a third- or fourth-degree tear
- Paediatric review is recommended before discharge to assess for complications such as brachial plexus injury
Future deliveries
There is a risk of recurrence with any subsequent deliveries. Mothers should be informed of this risk and given options for subsequent deliveries.
Complications
The complications of shoulder dystocia can be divided into maternal and fetal.
Maternal complications of shoulder dystocia include:
- Third- or fourth-degree tears
- Post-partum haemorrhage
- Trauma/post-traumatic stress disorder
Foetal complications of shoulder dystocia include:
- Brachial plexus injury (BPI)
- Fractures: humerus or clavicle
- Hypoxic brain injury.
Brachial plexus injury
Approximately one in ten babies who have shoulder dystocia will have a degree of stretching of the brachial nerve plexus in the neck, called brachial plexus injury.
The most common type of BPI is called Erb’s palsy (Figure 3). It is usually temporary, and movement will return within hours or days. Permanent damage is rare.
If managed appropriately the risk of permanent brachial plexus injury can be almost eliminated. However, it is important to remember that BPI can occur without shoulder dystocia. BPI can also occur in babies born by caesarean section.
Key points
- Shoulder dystocia is an obstetric emergency where the anterior fetal shoulder becomes stuck on the maternal pubic symphysis, delaying the birth of the baby’s body.
- The incidence is around one in 150 vaginal births.
- The most common findings include difficulty in delivering head or chin and the turtleneck sign.
- Pre-labour risk factors include previous dystocia, macrosomia, diabetes mellitus, high maternal BMI and labour induction. However, it is not possible to predict most incidences of shoulder dystocia.
- Emergency management includes calling for help, stopping maternal pushing, first-line McRoberts manoeuvre with suprapubic pressure and second-line internal manoeuvres.
- Maternal complications include third- or fourth-degree tears or PPH
- Fetal complications include humerus or clavicle fracture, brachial plexus injury and hypoxic brain injury.
Reviewer
Dr Rachel Greenwood
Obstetrics & Gynaecology Registrar
Editor
Dr Chris Jefferies
References
- RCOG. Shoulder Dystocia Green-Top Guideline No.42 Edition. Published in March 2012. Available from: [LINK]
- Geraldbaeck. McRoberts Manoeuvre. Licence: [Public domain]
- Donthatemebro. Brachial Plexus Injury. Licence: [CC BY-SA 3.0]
- R. Erbs Palsy. Licence: [CC BY-SA 4.0]