- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
A 52 year old man presents to the GP with worsening headaches. Work through the case to reach a diagnosis.
UK Medical Licensing Assessment (UKMLA)
This clinical case maps to the following UKMLA presentations:
History
Presenting complaint
“Doctor, I’m really getting fed up of these headaches, I’ve been trying my best to deal with them but they’ve been going on for months and I’m really struggling!”
History of presenting complaint
Site
- Unilateral (e.g. migraine)
- Frontal bilateral (e.g. tension headache)
Onset
- Was the onset acute or gradual? (e.g. sudden onset “thunderclap” headache is suggestive of subarachnoid haemorrhage)
- If the headache is chronic, in a month of 30 days, for how many of those days would the patient have a headache? How many days out of the month would the headache be severe?
Character (e.g. aching, throbbing, pounding, pulsating, pressure, pins and needles)
Radiation
- Neck (e.g. meningitis)
- Face (e.g. trigeminal neuralgia)
- Eye (e.g. acute closed-angle glaucoma)
Associated symptoms
- Nausea/vomiting (e.g. migraine, raised intracranial pressure (ICP))
- Visual disturbance (e.g. aura, space-occupying lesion, haemorrhagic stroke)
- Photophobia (raised ICP, meningitis)
- Neck stiffness (e.g. meningitis)
- Fever (e.g. encephalitis, cerebral abscess, meningitis)
- Rash (e.g. non-blanching purpuric rash may indicate meningococcal sepsis)
- Weight loss (potentially suggestive of malignancy, consider cerebral metastases)
- Sleep disturbance (headaches causing sleep disturbance are a red flag, consider raised ICP)
- Temporal region tenderness (consider temporal arteritis)
- Neurological deficits (e.g. weakness, sensory disturbance, impaired co-ordination, cognitive deficits – consider space-occupying lesion, encephalitis, meningitis and intracranial bleeding)
Timing
- Duration of headache
- Frequency
- Pattern (e.g. worse in the mornings – suggestive of raised ICP)
Exacerbating and/or relieving factors
- Are there any obvious triggers for the symptom? (e.g. caffeine, codeine, stress, postural change)
- Does anything appear to improve the symptoms? (e.g. improvement upon lying flat suggestive of reduced ICP)
Severity
- How bad is the pain on a scale of 0-10?
- Is the pain getting worse?
- How is it impacting their daily life?
For more information, see our guide to headache history taking.
Other areas of the history
- Past medical history (e.g. hypertension, malignancy, migraines)
- Drug history (several medications can cause headaches e.g. codeine overuse)
- Surgical history (e.g. previous neurosurgery)
- Family history (e.g. migraines, malignancy)
- Social history (e.g. occupation, alcohol history, smoking history, recreational drug use)
Patient’s answer
“My headaches started around 3 months ago, at which point they were around 3 out of 10 in severity. They have gradually worsened over time and now I’d rate them at about 6/10. The headaches do tend to be worse in the morning and feel like a dull ache behind my eyes. They tend to last a few hours at a time and nothing makes them particularly worse or better.”
“I’ve not had problems with feeling or being sick. I’ve not noticed any fevers, rash or neck stiffness. I haven’t got any weakness or numbness anywhere and I haven’t lost consciousness at any point. I have noticed that recently I’ve been bumping into door frames, but I haven’t noticed any obvious problems with my balance or vision.”
“I don’t have any other medical problems, I take no medication and I have no family history of any diseases. I work as a computer programmer and I don’t drink alcohol or smoke. I’ve never used any recreational drugs.”
Clinical examination
- Upper and lower limb neurological examination
- Cranial nerve examination including visual assessment
- Cardiovascular examination
Clinical findings
Cranial nerve examination:
- No deficits noted
Cardiovascular examination:
- Blood pressure 123/75 mmHg
- Unremarkable examination
Neurological assessment of the limbs:
- No focal motor or sensory deficit in the upper or lower limbs.
Visual assessment:
- Pupils are equal and reactive
- Visual acuity and eye movement are normal
- Visual field testing reveals bitemporal hemianopia
- Colour vision is normal
Differential diagnoses
- Pituitary lesion
- Other space-occupying lesions (e.g. metastases, meningioma, craniopharyngioma)
- Stroke
- Cerebral aneurysm (e.g. anterior communicating artery aneurysm)
Investigations
Blood tests
- Full blood count
- U&Es
- CRP
- Coagulation
- Pituitary hormone profile:
- Serum IGF1 – correlates with the amount of growth hormone secreted over the last 24hrs
- Thyroid-stimulating hormone (TSH)
- Adrenocorticotropic hormone (ACTH)
- Prolactin
- Luteinizing hormone (LH)
- Follicle-stimulating hormone (FSH)
- Antidiuretic hormone (ADH)
Imaging
CT head (+/- contrast):
- Useful for identifying space-occupying lesions and/or intracranial bleeding
MRI head:
- Provides higher resolution imaging than CT
- Sensitive at picking up pituitary fossa lesions
Cerebral angiogram:
- Allows the vasculature of the cerebrum to be assessed in detail
- Useful if considering cerebral aneurysm
Investigation results
Blood tests
- FBC, U&Es, Coagulation and CRP are all normal.
- Pituitary hormone profile demonstrates a low TSH, but nil else.
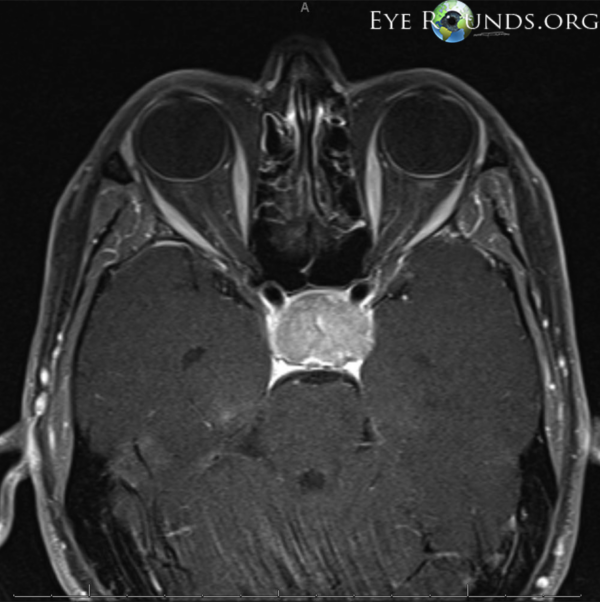
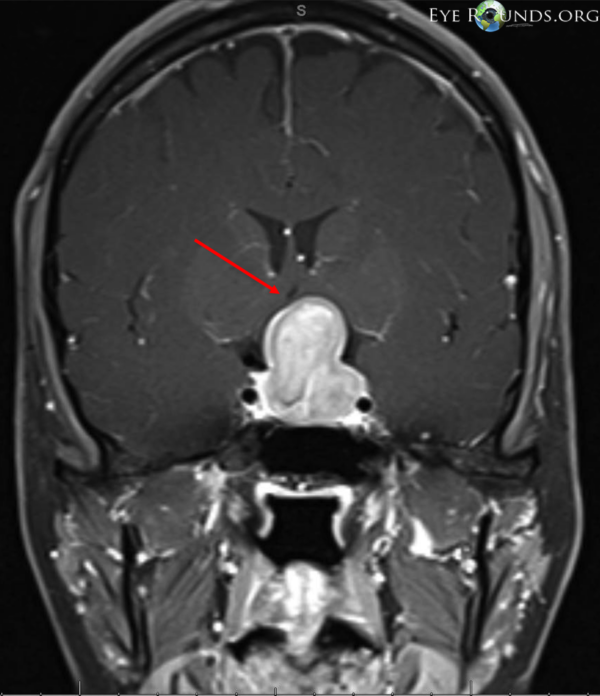
MRI head
The MRI reveals a pituitary lesion with elevation and compression of the optic chiasm. The ventricles are normal size, and no other abnormalities are noted.
Diagnosis
Non-functioning pituitary adenoma
- Prolactinoma
- Growth hormone-secreting adenoma
- Adreno-corticotrophic secreting adenoma
- Biopsy – histology of the lesion is required to confirm the diagnosis
Management
Conservative
Watchful waiting, with regular imaging to monitor the growth rate and identify compression of local structures. In this case, the patient is symptomatic with clinical and radiological evidence of optic chiasmal compression, therefore surgical intervention to excise and decompress the pituitary fossa is indicated.
Surgical
Trans-sphenoidal excision of the adenoma:
- Minimally invasive approach
- Allows reduction in the mass effect of the lesion
Radiotherapy
Radiotherapy can be used if surgical excision is incomplete, or if recurrence of the pituitary lesion occurs.
Following the operation
The patient recovers well after surgery; however, at three days post-op, the patient complains of feeling nauseated and generally unwell.
Blood tests are taken:
- Sodium – 152 mmol/L (133-146)
- Potassium – 3.8 mmol/L (3.5–5.3)
- Creatinine – 78 μmol/ L (59–104)
- Serum osmolality- 328 mmol/kg (275 – 295)
- Random urine osmolality – 38 mOsm/kg (50-1400)
Post-operative diabetes insipidus:
- Not uncommon after pituitary surgery.
- ADH is normally released from the posterior pituitary.
- Surgery can damage this area and as a result, cause reduced ADH secretion.
- Lack of ADH results in the body being unable to retain water effectively.
- As a result, the kidneys produce inappropriately large volumes of dilute urine.
- The patient, therefore, becomes dehydrated, leading to a rise in serum sodium concentration.
- The underlying issue in this patient is a lack of endogenous ADH, resulting in inappropriate water loss via the kidneys.
- The patient, therefore, requires an ADH analogue such as desmopressin (the endocrine team would lead management).
- A strict fluid balance and regular monitoring of U&Es would also be essential.
- Often post-operative diabetes insipidus is transient and will resolve a few days post-op. However, desmopressin is often required in the short term until the patient remains consistently normonatraemic.
A few days later…
The patient is given desmopressin on the advice of the endocrine team, and over the next four days, the patient’s sodium levels normalise, with no more desmopressin required.
However, at seven days post-op, the patient feels unwell again, so further blood tests are performed:
- Sodium – 121 mmol/L (133-146)
- Potassium – 4.1 mmol/L (3.5–5.3)
- Creatinine – 85 μmol/ L (59–104)
- Serum osmolality – 240 mmol/kg (275 – 295)
- Urine osmolality – 600 mOsm/kg (50-1400)
Syndrome of inappropriate antidiuretic hormone secretion (SIADH)
- Despite the patient initially presenting with hypernatraemia, they are now significantly hyponatraemic.
- The patient is hyponatraemic with a low serum osmolality, however, despite this, they are still excreting inappropriately high amounts of sodium into the urine.
- This type of picture is seen in SIADH, where there is an excess of ADH in the circulation.
- This is the opposite of the earlier presentation (where a lack of ADH was causing hypernatraemia).
For more information, see our guide to SIADH.
- SIADH is a state of normovolaemic dilutional hyponatraemia.
- Often the first line of management for this condition is fluid restriction.
- This management strategy attempts to avoid further dilution and increase sodium concentration.
As a result, the patient is fluid restricted to 1.5 litres daily, with a strict fluid balance.
A few more days later…
The patient is fluid-restricted. However, four days later, the patient develops dysphagia and dysarthria. Blood tests are repeated:
- Sodium – 163 mmol/L (133-146)
- Potassium – 4.8 mmol/L (3.5–5.3)
- Creatinine – 88 μmol/L (59–104)
- Serum osmolality – 347 mmol/kg (275 – 295)
- Urine osmolality – 38 mOsm/kg (50-1400)
Triphasic response
The triphasic response is a well recognised post-operative complication of pituitary surgery and involves three stages.
Stage 1 – Transient diabetes insipidus:
- There is a lack of ADH within the circulation, due to local trauma to neurons responsible for producing ADH.
- This results in large volumes of dilute urine and secondary hypernatraemia.
- This phase typically begins 24-48 hours post-op and lasts 5-7 days.
Stage 2 – SIADH:
- SIADH occurs due to the uncontrolled release of ADH from the degenerating posterior pituitary tissue damaged during surgery.
- As a result, the kidneys retain excessive volumes of water, causing dilutional hyponatraemia.
- The duration of this phase is highly variable and can last between 2-14 days.
Stage 3 – Chronic diabetes insipidus:
- Once all stores of ADH released from the degenerating pituitary tissue are depleted, there is no source of further production of ADH, leading to a sudden drop in circulating ADH levels.
- As a result, the kidneys begin to lose high volumes of water, leading to a sharp rise in sodium concentration.
- This rise in sodium can be further exacerbated if the patient is still being treated for hyponatraemia during the second SIADH phase (NaCl 0.9% IV fluid, NaCl tablets, fluid restriction).
- This sudden fluctuation in sodium levels can lead to catastrophic irreversible complications such as central pontine myelinolysis.
- Once the third stage of the triphasic response is reached, the patient will likely continue to have diabetes insipidus long term, which will require ongoing specialist endocrine input.
Central pontine myelinolysis
- A disease characterised by severe damage to the myelin sheath in the area of the pons.
- It is caused by rapid changes in serum osmolarity – most often due to rapid correction of hyponatraemia.
- This occurs because brain cells adjust to hyponatraemic state by absorbing free fluid to increase the osmolarity of the surrounding fluid. If the serum osmolarity then increases suddenly, it leads to a rapid movement of free fluid out of the cells into the surrounding fluid, which causes cell damage and subsequent demyelination.
- Common symptoms include dysphagia, dysarthria and paralysis.
- To avoid this complication, sodium levels should be monitored frequently and correction should be no faster than 10 mmol/L/24hr.
Learning points
- Patients with headaches need a thorough history and examination to narrow the differential diagnosis and guide further investigations.
- Pituitary tumours are not always hormone-producing (functional), therefore a normal pituitary hormone profile does not rule out the presence of a pituitary lesion.
- Pituitary tumours can be managed conservatively if small and not causing significant compression of surrounding structures.
- Post-operative electrolyte imbalances are common in pituitary surgery.
- Frequent monitoring of electrolytes is essential to recognise issues early and prevent complications.
- The triphasic response should always be considered in patients with sodium imbalances post-pituitary surgery.
- Specialist endocrine opinion should be sought before commencing sodium replacement in this patient group.
- Rapid correction of hyponatraemia is dangerous and can result in catastrophic complications.
References
- Weed MC, Longmuir RA, Thurtell MJ. Pituitary Adenoma Causing Compression of the Optic Chiasm: 49-year-old white female with painless progressive vision loss. EyeRounds.org. September 9, 2013; available from: [LINK]
- Patient.info. Hyponatraemia. Last updated in 2022. Available here: [LINK]
- Patient.info. Pituitary tumours. Last updated in 2023. Available here: [LINK]