- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Introduction
Necrotising fasciitis (NF) is a rare but life-threatening infection involving any layer of the deep soft tissue compartments (i.e. dermis, subcutaneous tissue, fascia or muscle).
Aetiology
Necrotising fasciitis develops when organisms migrate from subcutaneous tissue along fascial planes. Although muscle is typically spared by the organisms themselves, necrosis of muscle tissue can still occur because of compartment syndrome.
A wide range of organisms can cause NF including:
- Group A streptococcus
- Gram-negative organisms such as Vibrio spp and Aeromonas hydrophilia which are typically acquired from seawater contamination of wounds
- Fungal infection (e.g. candida)
In many cases of NF the cause is polymicrobial (i.e. a mixture of aerobic and anaerobic bacteria).
Risk factors
Risk factors for the development of NF include:
- Skin injury (e.g. bites, trauma, wounds)
- Impaired immunity (e.g. malignancy, immunosuppression, chronic alcohol abuse, diabetes, chronic renal disease, chronic liver disease)
- Intravenous drug use
Clinical features
History
Typical symptoms of NF include:
- Pain which is out of proportion to the clinical findings
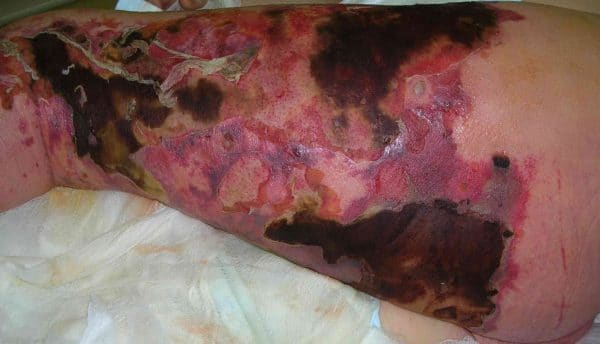
- Skin discolouration
- Skin blistering
- Fever
- Malaise
Clinical examination
Typical findings on clinical examination include:
- Local pain, swelling and erythema
- Poorly defined margins with pain extending beyond the margins of erythema
- Crepitus on palpation of the skin
- Offensive discharge which may have a typical ‘dishwater’ appearance
- Oedema (which may be tense)
- Bullae
Systemic features may include:
- Fever
- Hypotension and tachycardia
Investigations
Laboratory investigations
Relevant laboratory investigations include:
- FBC: white cell count will typically be significantly elevated (unless immunocompromised)
- U&Es: hyponatraemia may be associated with NF
- CRP: typically elevated in the context of NF
- Creatinine kinase: typically elevated in the context of NF secondary to myonecrosis
- Lactate: typically elevated in the context of NF
- Blood cultures: to identify causative organisms which may also be within the circulation.
- Coagulation screen: as part of a pre-operative workup
- Group and save: as part of a pre-operative workup
Microbiology
Relevant microbiological investigations include:
- Blood cultures (mentioned above)
- Wound swabs
- Debrided tissue gram-stain and culture
Imaging
Although imaging can be valuable, it should not delay emergency surgical management.
A CT of the affected area may reveal gas produced by the organisms and help assess the extent of spread.
Bedside finger test
The bedside finger test is sometimes performed by plastic surgeons and involves the following steps:
- A small incision is made down to the fascia under local anaesthetic.
- The tissue is then probed with a sterile gloved finger.
Findings associated with NF include an absence of bleeding, purulent pus and a lack of normal tissue resistance to blunt dissection.
Diagnosis
Necrotising fasciitis is a clinical diagnosis, but investigations can help inform further medical and surgical management.
Management
Medical management
A structured ABCDE assessment should be performed to identify and treat issues such as haemodynamic instability.
Broad-spectrum intravenous antibiotics should be administered as soon as possible according to local guidelines (covering streptococci, staphylococci, gram-negative rods and anaerobes).
Surgical management
Urgent surgical debridement is required to remove the infected tissue in the hope of halting further spread of the infection to surrounding tissue.
After initial debridement, the wound is monitored and may require further debridement until the infection is controlled.
Key points
- Necrotising fasciitis (NF) is a rare but life-threatening infection involving any layer of the deep soft tissue compartments (i.e. dermis, subcutaneous tissue, fascia or muscle).
- A wide range of organisms can cause NF and in most cases the infection is polymicrobial.
- Risk factors for the development of NF include skin injury, impaired immunity and intravenous drug use.
- Typical symptoms of NF include pain which is out of proportion to the clinical findings, skin discolouration, blisters, fever and malaise.
- Typical findings on clinical examination include local pain, swelling and erythema with poorly defined margins. Other findings may include crepitus on palpation, offensive discharge, oedema and bullae.
- Investigations for NF include basic blood tests, blood culture, wound swabs, debrided tissue culture, CT and the bedside finger test.
- NF is a clinical diagnosis but investigations can help inform further medical and surgical management.
- Medical management of NF includes an initial ABCDE assessment and the administration of broad-spectrum IV antibiotics.
- Surgical management involves debridement of the affected tissue with close monitoring post-operatively.
Reviewer
Mr Zakir Shariff
Consultant Plastic Surgeon
References
- Tidy C. Necrotising Fasciitis. Available from: [LINK].
- Hasham S, Matteucci P, Stanley PR, et al; Necrotising fasciitis. BMJ, 2005 Apr 9 330 (7495):830-3.
- Brooks A, Cotton BA, Tai N, Mahoney PF. Emergency Surgery Book. Wiley-Blackwell; 1st ed. 2010 Apr 13.
- Semer NB. Practical Plastic Surgery for Nonsurgeons. Hanley & Belfus, Inc. Philadelphia. 2001
- Piotr Smuszkiewicz, Iwona Trojanowska and Hanna Tomczak. Necrotising fasciitis. License: [CC-BY]




