- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Introduction
A peritonsillar abscess (also known as quinsy) is a complication of acute tonsillitis in which pus collects in the peritonsillar space.
If untreated it may lead to deep neck space infection.
Quinsy affects around 12 per 100,000 people in England.1
Aetiology
Peritonsillar abscesses are a complication of acute tonsillitis.
The palatine tonsils are bilateral lymphatic tissue in the oropharynx that make up part of Waldeyer’s ring along with the adenoids, bilateral tubal tonsils and lingual tonsil.
A peritonsillar abscess collects lateral to the palatine tonsils in the peritonsillar space. This is a potential space between the palatine tonsil and pharyngeal mucosa.
While most cases of tonsillitis are caused by a viral infection (e.g. Epstein-Barr virus), the most common bacterial pathogen is group A beta-haemolytic streptococcus.2
Risk factors
The main risk factor for developing a peritonsillar abscess is recurrent tonsillitis.
Other risk factors include:
- Age: teenagers/young adults are more likely to develop a peritonsillar abscess
- Male sex
- Smoking
Clinical features
History
Typical symptoms of a peritonsillar abscess include:
- Sore throat: particularly on swallowing (odynophagia), typically worse on one side (may have referred pain to the ear – a.k.a. otalgia)
- Change in voice: commonly described as ‘hot potato voice’, but not hoarseness
- An inability to swallow: this may be limited to saliva or small sips of liquid
Clinical examination
Typical clinical findings in the context of peritonsillar abscess include:1
- Trismus: inability or difficulty in opening the mouth fully (defined as opening <3cm)
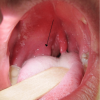
- Bulging palatine arch on the affected side: with uvula deviation away from the affected side (Figure 1)
- Signs of sepsis: altered mental state, fever, tachypnoea, tachycardia and hypotension
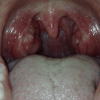
A unilaterally swollen palatine tonsil, or bilateral swollen tonsils (Figure 2), does not indicate a peritonsillar abscess. This is a common misdiagnosis. A peritonsillar abscess will result in a bulging palatine arch anterolateral to the palatine tonsils (Figure 1).
Differential diagnoses
Differential diagnoses to consider include:
- Acute tonsillitis
- Epiglottitis: severe throat pain, fever, hoarse voice and/or stridor
- Para- or retro-pharyngeal abscess: can be similar in presentation to epiglottitis, may have aphagia or severe dysphagia and sudden voice change. Patients often have stiffness or reduced range of motion of the neck.
- Dental pathology
Investigations
Peritonsillar abscess is a clinical diagnosis, however, the following investigations may be considered.
Bedside investigations
Relevant bedside investigations include:
- Flexible nasendoscopy (FNE): to look for other pathology in the pharynx and larynx
Laboratory investigations
Relevant laboratory investigations include:
- FBC: white cells are typically raised in acute infection. It is also important to establish a baseline haemoglobin and platelet count if the patient requires a surgical procedure.
- CRP: likely to be raised in acute infection
- LFTs: important to have a baseline if commencing on intravenous antibiotics. Acute derangement is often associated with infectious mononucleosis (glandular fever)
- U&Es: often patients are dehydrated as a result of reduced oral intake
- EBV/monospot/glandular fever screen: EBV can cause infectious mononucleosis (glandular fever), a viral cause of tonsillitis
- Blood cultures: should be taken if there is a suspicion of sepsis to guide future antimicrobial decisions
Imaging investigations
Relevant imaging investigations include:
- CT neck: may be considered if a patient is not improving to look for other sources of cervical sepsis (e.g. deep neck space infection)
- Orthopantomogram: if dental pathology is suspected
Diagnosis
The Liverpool Peritonsillar Abscess (LPS) score is a decision aid for patients with suspected peritonsillar abscesses.1
The LPS has since been adjusted during the COVID-19 pandemic to remove the need for an oral examination. The criteria are as follows:
- Unilateral sore throat – 3 points
- Trismus – 2 points
- Male gender – 1 point
- Hot potato voice – 1 point
A score of three or less means a peritonsillar abscess is unlikely, with a negative predictive value of 98%.
A score of four or more means a peritonsillar abscess is more likely.
A score of six or more means a peritonsillar abscess is very likely, with a positive predictive value of 80%.1
Management
In patients with a suspected peritonsillar abscess, an ABCDE approach should be adopted during the initial assessment.
Airway problems are rare in patients with quinsy, however, those with large abscesses may develop stertor. If there is concern regarding airway compromise, a senior ENT surgeon should be involved.
Stridor is very unlikely and would usually indicate laryngeal pathology.
Stertor vs. stridor
Stertor is caused by a partial upper airway obstruction above the level of the larynx. It is due to vibration of nasopharynx, oropharynx or soft palate, and sounds like heavy snoring or gasping.
Stridor, on the other hand, is a high-pitched sound that can be inspiratory, expiratory or both (biphasic) and is caused by partial airway obstruction at the level of the larynx, or lower down the respiratory tract.
Medical management
Medical management of a peritonsillar abscess includes:2,5
- Analgesia: non-steroidal anti-inflammatories (NSAIDs) are recommended
- Intravenous fluids: to re-hydrate patients who may have had reduced oral intake due to difficulty swallowing
- Intravenous antibiotics: usually a combination of benzylpenicillin and metronidazole (or in penicillin-allergic patients, clindamycin/clarithromycin monotherapy). Local guidelines should be followed.
- Corticosteroids: a single dose of corticosteroids (e.g. dexamethasone) may reduce inflammation and relieve trismus, however, there is limited evidence for this treatment
Surgical management
The definitive of surgical management of a peritonsillar abscess involves aspiration of the abscess.
Aspiration is typically performed on a ward or in a treatment room with the patient awake, using a local anaesthetic spray.
Aspiration of the abscess often provides rapid symptomatic relief. Occasionally incision and drainage may be required for a persistent collection.
The pus obtained should be sent for culture and sensitivity to guide antimicrobial therapy.
Complications
Complications of quinsy include:
- Retro- and parapharyngeal abscess: deep neck space infections are an airway emergency and can develop from untreated quinsy. Senior members of the ENT team should be involved immediately. Deep neck space infections often need drainage of the collection under general anaesthetic. If not managed promptly, it can lead to airway obstruction, which may require intubation or tracheostomy and critical care input.
- Mediastinitis: if left untreated deep neck space infections, as described above, can subsequently track down into the mediastinum. This is a life-threatening complication which will require input from the cardiothoracic surgeons.
Recurrent episodes of peritonsillar abscess (two or more) is an indication for tonsillectomy.2
Key points
- A peritonsillar abscess is a complication of acute tonsillitis involving the collection of pus in the peritonsillar space.
- The most common bacterial cause is group A beta-haemolytic streptococcus.
- Clinical features include a unilateral sore throat, difficulty swallowing, trismus and hot potato voice.
- On examination, a unilateral swelling is visible often with uvula deviation away from the affected side.
- Peritonsillar abscess is a clinical diagnosis, but laboratory tests (including FBC, U&Es, CRP, microbial cultures) and flexible nasendoscopy are important investigations.
- Management includes analgesia, intravenous fluids, antibiotics, steroids and aspiration (or incision and drainage) of the abscess.
- If left untreated, a peritonsillar abscess can develop into a deep neck space infection and potentially cause airway obstruction.
- If a patient has recurrent episodes of peritonsillar abscess (two or more) tonsillectomy would be indicated.
Reviewer
Mr Andrew Williamson
BSc MBChB MRCS & MRCS ENT
ST5 Otolaryngology
Editor
Dr Chris Jefferies
References
- Lau AS, Selwyn DM, Yang D, et al. The Liverpool Peritonsillar abscess Score: Development of a predictive score through a prospective multicentre observational study. Clin Otolaryngol. 2019; 44:293-298.
- Scottish Intercollegiate Guidelines Network. Management of sore throat and indications for tonsillectomy: A national clinical guideline. SIGN; 2010 (SIGN 117). Available from: [LINK]
- James Heilman, MD (Own work). A right sided peritonsillar abscess. Licence: [CC BY-SA]. Available from: [LINK]
- Madonella (Own Work). akute bilaterare Tonsillitis. Licence: [CC BY-SA]. Available from: [LINK]
- National Institute for Health and Care Excellence. Sore throat (acute): antimicrobial prescribing (Clinical Guideline[NG84]). Available from: [LINK]