- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
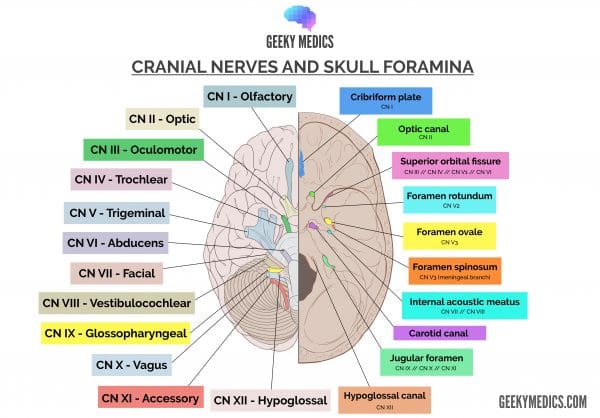
Cranial nerve IX is the glossopharyngeal nerve, important for parasympathetic, motor and sensory innervation of the tongue, pharynx and larynx. Here, we break down the different anatomical structures contributing to the glossopharyngeal nerve and discuss its clinical relevance.
The glossopharyngeal nerve is a combination of several different nuclei throughout the brainstem that supply numerous structures. The following is a general overview of the structures it supplies that we will review several times in this article:
- Motor: stylopharyngeus
- Sensory: carotid body and sinus, dorsal posterior 1/3 of the tongue, oropharynx, middle ear and the Eustachian tube
- Special sensory: taste to the dorsal posterior 1/3 of the tongue
- Parasympathetic: parotid gland
Check out our summary of the cranial nerves here.
You can also check out our cranial nerve anatomy quiz here.
Embryology
The glossopharyngeal nerve is the nerve associated with the third pharyngeal arch. The only muscular structure associated with the third pharyngeal arch is the greater horns of the hyoid. The stylopharyngeus muscle attaches to this structure once ossified. CN IX supplies sensory and parasympathetic innervation to the structures lying around the hyoid cartilage, as we will see later on.
Glossopharyngeal nuclei
The nuclei for the glossopharyngeal nerve all lie in the inferior pontine and medullary regions of the brainstem.
The nuclei that contribute to it include:
- (Rostral) Solitary nucleus: special sense of taste
- Dorsal motor nucleus: secretomotor to the oropharynx
- Inferior salivatory nucleus: parasympathetic parotid gland
- Nucleus ambiguus: motor innervation to stylopharyngeus
- Spinal trigeminal nucleus: pain and temperature from the tongue
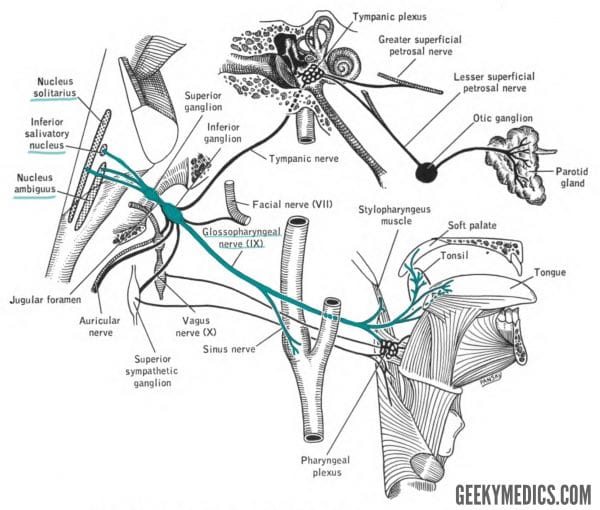
The course of some of these nuclei is shown in Figure 2. The glossopharyngeal nerve is formed by each of these separate regions of the brainstem in order to provide sensory, motor and parasympathetic innervation to structures in and around the mouth.
Intracranial glossopharyngeal nerve
The fibres from these nuclei all converge to form the glossopharyngeal nerve, which exits the medulla oblongata at the post-olivary sulcus (behind the inferior olives). It lies immediately superior to cranial nerves X (vagus) and XI (spinal accessory).
It travels with CNs X and XI inferolaterally in the posterior cranial fossa to reach the internal os of the jugular foramen. Immediately before entering the jugular foramen, the tympanic nerve branches from CN IX, providing sensory fibres to the middle ear and parasympathetic fibres to the parotid gland.
Extracranial glossopharyngeal nerve
As CN IX leaves the jugular foramen, it meets the superior and inferior ganglia (no other special name!), which contain the neuronal cell bodies of the sensory components of CN IX. These ganglia appear to be small bulges in the glossopharyngeal nerve next to the jugular foramen.
The glossopharyngeal nerve accompanies the internal carotid artery, which lies posteromedial to the nerve. As the nerve passes the inferior border of the stylopharyngeus muscle, it supplies it with motor fibres. At this point, the glossopharyngeal nerve sends sensory fibres to the carotid sinus via the nerve to the carotid sinus.
Continuing down the neck, the glossopharyngeal nerve then enters the pharynx as it passes through the superior and middle pharyngeal constrictor muscles. It then branches into several small branches that supply the tongue (lingual branch), tonsils (tonsillar branch) and pharynx.
Glossopharyngeal nerve branches
Here is a short summary of the branches of the glossopharyngeal nerve and their functions:
- Tympanic: sensory innervation to the mucosa of the middle ear, turning into the lesser petrosal nerve to supply parasympathetic fibres to the parotid gland*
- Stylopharyngeus: motor innervation to the stylopharyngeus
- Tonsillar: sensory and parasympathetic innervation to the tonsils and oropharynx
- Nerve to carotid sinus: sensory innervation to the carotid sinus
- Nerve to dorsal posterior 1/3 of the tongue: special sense of taste from the dorsal posterior 1/3 of the tongue
- Lingual branch: sensory information from the dorsal posterior 1/3 of the tongue
- Vagal communicating branch: parasympathetic communicating branches with the vagus nerve
This also happens to be the rough order of the branches as they leave the glossopharyngeal nerve. There are several mnemonics for this, one such is, “Tom Says To Never Never Leave Vegas.”
* The tympanic nerve takes fibres from the inferior salivatory nucleus and communicates these fibres from the middle ear as the lesser petrosal nerve. The lesser petrosal nerve synapses at the otic ganglion, where the parasympathetic fibres then travel with the auriculotemporal nerve to the parotid gland.
Clinical relevance: examination of the glossopharyngeal nerve
When examining CN IX, it is important to test the glossopharyngeal nerve. One of the more accessible terminal branches of this nerve is the tonsillar branch, which supplies sensory innervation to the oropharynx.
When a foreign object, such as a long cotton tip, touches the mucosal surface of the oropharynx the gag reflex is initiated.
The afferent limb of the gag reflex is the glossopharyngeal nerve, and the efferent limb is the vagus nerve.
When assessing the gag reflex, you are really assessing two cranial nerves in one test!
Clinical relevance: the interface of neurophysiology and medicine
Interestingly, an absent gag reflex may not be pathological. Up to 20% of patients suggest they have no gag reflex. A reflex arc, much like an action potential, needs adequate stimulation to begin. We know that action potentials require either spatial summation (lots of stimuli at once) or temporal summation (rapid and repetitive stimuli) to elicit a signal. Reflex arcs are much the same – a stimulus on the oropharyngeal mucosa that is large enough or present for long enough will begin to elicit a gag reflex, even in those who say they don’t have a gag reflex!
Key points
- CN IX is the glossopharyngeal nerve
- It originates in the medulla oblongata
- It draws fibres from the solitary nucleus (taste) and nucleus ambiguus (motor)
- It draws more fibres from the inferior salivatory nucleus (parotid gland) and dorsal motor nucleus (DMX; pharyngeal sensation)
- It passes through the jugular foramen
- It provides many fibre types, which are shown in the table below
| General somatic afferent | Special visceral afferent | General visceral efferent | Special visceral efferent |
| Sensation from the posterior 1/3 of the tongue, pharynx | Taste to posterior 1/3 of the tongue | Parasympathetic to parotid glands | Motor to stylopharyngeus |
References
Reference texts
- Sinnatamby, C. S. (2011). Last’s Anatomy, International Edition: Regional and Applied. Elsevier Health Sciences.
- Moore, K. L., Dalley, A. F., & Agur, A. M. (2013). Clinically oriented anatomy. Lippincott Williams & Wilkins.
- Nolte, J. (2002). The human brain: an introduction to its functional anatomy.
- Snell, R. S. (2010). Clinical neuroanatomy. Lippincott Williams & Wilkins.
Reference images
- Patrick J. Lynch. License: [CC BY]. Modified by Dr Lewis Potter.
- House, Earl Lawrence. Pansky, Ben. License: [Public domain]




