- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Cerebellar examination frequently appears in OSCEs and you’ll be expected to identify the relevant clinical signs using your examination skills. This cerebellar examination OSCE guide provides a clear step-by-step approach to examining the cerebellum, with an included video demonstration.
Remembering what to cover
- Dysdiadochokinesia
- Ataxia (gait and posture)
- Nystagmus
- Intention tremor
- Slurred, staccato speech
- Hypotonia/heel-shin test
Introduction
Wash your hands and don PPE if appropriate.
Introduce yourself to the patient including your name and role.
Confirm the patient’s name and date of birth.
Briefly explain what the examination will involve using patient-friendly language.
Gain consent to proceed with the examination.
Ask the patient to sit on a chair, approximately one arm’s length away.
Ask the patient if they have any pain before proceeding with the clinical examination.
General inspection
Clinical signs
Perform a brief general inspection of the patient, looking for clinical signs suggestive of underlying pathology:
- Abnormal posture: may indicate the presence of truncal ataxia.
- Speech abnormalities: slurred staccato speech is typical of cerebellar disease.
- Scars: may indicate previous neurosurgery (often difficult to see because of the patient’s hair).
- Gait: pay attention to the patient’s gait as they enter the room and take a seat, noting any abnormalities (e.g. broad-based gait in cerebellar pathology).
Objects or equipment
Look for objects or equipment on or around the patient that may provide useful insights into their medical history and current clinical status:
- Walking aids: cerebellar disease often causes issues with balance (ataxia), resulting in patients using walking aids to steady themselves.
- Hearing aids: hearing loss can be associated with pathology that may impact the cerebellum (e.g. acoustic neuroma causing local cerebellar compression).
- Prescriptions: prescribing charts or personal prescriptions can provide useful information about the patient’s recent medications.
Ataxia
Ataxia is a neurological sign consisting of involuntary movements with an irregular oscillatory quality which interfere with the normal smooth trajectory of movement. Ataxia can be truncal (affecting the trunk) or appendicular (affecting the limbs):
- Truncal ataxia: affects proximal musculature that is involved in gait stability. This form of ataxia is caused by damage to the cerebellar vermis and associated pathways (i.e. midline cerebellar lesions).
- Appendicular ataxia: affects musculature of the arms and legs involved in the control of limb movement. This form of ataxia is caused by damage to the cerebellar hemispheres (i.e. lateral cerebellar lesions).
Gait
Assess the patient’s gait
Patients with cerebellar disease are at an increased risk of falls so make sure to remain close to the patient during the assessment so that you are able to intervene if required.
Ask the patient to walk to the end of the examination room and then turn and walk back whilst you observe their gait paying attention to:
- Stance: a broad-based ataxic gait is typically associated with midline cerebellar pathology (e.g. a lesion in multiple sclerosis or degeneration of the cerebellar vermis secondary to chronic alcohol excess).
- Stability: a staggering, slow and unsteady gait is typical of cerebellar pathology. In unilateral cerebellar disease, patients will veer towards the side of the lesion.
- Turning: patients with cerebellar disease will find the turning manoeuvre particularly difficult.
Tandem (‘heel-to-toe’) gait
Ask the patient to walk to the end of the examination room and back with their heels to their toes (known as ‘tandem gait’). Heel-to-toe walking exacerbates underlying unsteadiness making it easier to identify more subtle ataxia.
Tandem gait is particularly sensitive at identifying dysfunction of the cerebellar vermis (e.g. alcohol-induced cerebellar degeneration).
Cerebellar degeneration
Cerebellar degeneration involves the progressive loss of Purkinje cells in the cerebellum. It has a wide range of causes including chronic alcohol abuse, nutritional deficiency (typically B12), paraneoplastic disorders and neurological diseases (e.g. multiple sclerosis, spinocerebellar ataxia).
Typical clinical features include:
- Broad-based ataxic gait
- Truncal ataxia
- Dysmetria (incoordination)
- Nystagmus (abnormal eye movements)
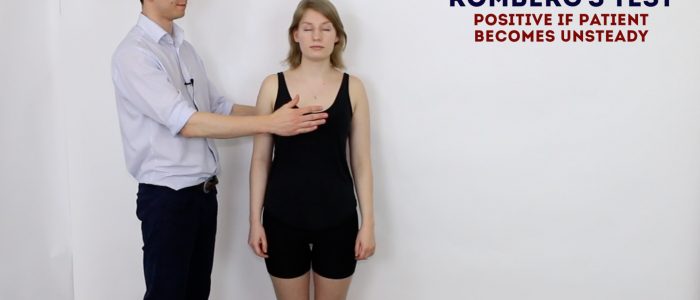
Romberg’s test
Romberg’s test is used to assess for loss of proprioceptive or vestibular function (known as sensory ataxia). The test does not assess cerebellar function and instead is used to quickly screen for evidence of sensory ataxia (i.e. non-cerebellar causes of balance issues).
Romberg’s test is based on the premise that a patient requires at least two of the following three senses to maintain balance whilst standing:
- Proprioception: the awareness of one’s body position in space.
- Vestibular function: the ability to know one’s head position in space.
- Vision: the ability to see one’s position in space.
Romberg’s test involves removing the sense of vision by asking the patient to close their eyes. As a result, if the patient has a deficit in proprioception or vestibular function they will struggle to remain standing without visual input.
Assessment
1. Position yourself within arms reach of the patient to allow you to intervene should they begin to fall.
2. Ask the patient to put their feet together and keep their arms by their sides (be aware that patients with truncal ataxia may struggle to do this, however, this type of unsteadiness is not the same as a positive Romberg’s sign).
3. Ask the patient to close their eyes.
Interpretation
Falling without correction is abnormal and referred to as a positive Romberg’s sign. This indicates unsteadiness is due to sensory ataxia (i.e. a deficit of proprioceptive or vestibular function, rather than cerebellar function). Causes of proprioceptive dysfunction include joint hypermobility (e.g. Ehlers-Danlos syndrome), B12 deficiency, Parkinson’s disease and ageing (known as presbypropria). Causes of vestibular dysfunction include vestibular neuronitis and Ménière’s disease.
Swaying with correction is not a positive result and often occurs in cerebellar disease due to truncal ataxia.
Speech
Assess speech by asking the patient to repeat the following phrases:
- “British constitution”
- “Baby hippopotamus”
Cerebellar lesions can cause ataxic dysarthria which can present in a number of ways:
- Scanning speech (also known as staccato speech): words are broken down into separate syllables, often separated by pauses and spoken with varying volume.
- Slurred speech: patients are often mistaken for being intoxicated as a result.
Scanning and slurred speech often occur in combination (often referred to as “slurred staccato speech”).
Eyes
Nystagmus
Nystagmus involves repetitive, involuntary oscillation of the eyes and can be either physiological (i.e. benign) or associated with cerebellar pathology.
Assessment
When assessing for nystagmus, begin by asking the patient to report any double vision (diplopia) if they experience it during the assessment. Diplopia may suggest the presence of strabismus which can be associated with some cerebellar syndromes (e.g. vestibulocerebellar syndrome).
1. Ask the patient to look straight ahead and examine the eyes in the primary position. Look for any abnormal movement such as nystagmus.
2. Ask the patient to keep their head still and follow your finger (or another visual target) with their eyes.
3. Move your finger throughout the various axes of vision in a ‘H’ pattern.
4. Look for multiple beats of nystagmus (a few beats at the extremes of gaze can be a normal variant and is termed physiological nystagmus).
Describing nystagmus
Detecting the presence or absence of nystagmus will be sufficient in an OSCE examination, however, nystagmus can be characterised further by assessing the following:
- Direction of nystagmus: most nystagmus has a fast phase and a slow phase (termed “jerk” nystagmus). By convention, the direction of the nystagmus is defined by the direction of the fast phase. In cerebellar lesions, the direction is towards the side of the lesion.
- Direction of gaze: note if nystagmus is present on horizontal or vertical gaze.
- Plane of nystagmus: note if nystagmus beats in a horizontal or vertical plane.
Other gaze disturbances
Other disturbances of gaze that are associated with cerebellar disease include dysmetric saccades and impaired smooth pursuit.
Dysmetric saccades
1. Position your hand approximately 30cm to the side of your head.
2. Ask the patient to look at your hand, then back to your nose. Repeat this assessment on both sides.
The movement of the patient’s eyes should be quick and accurate. In cerebellar lesions, there will often be overshoot (i.e. the eyes will go too far past the target, then correct themselves back to the target). This overshoot and subsequent correction are known as dysmetric saccades.
Impaired smooth pursuit
When the patient is tracking your finger, the eyes should move smoothly (known as ‘smooth pursuit’). In cerebellar lesions, pursuit can be “jerky” or “saccadic”( i.e. made up of lots of small movements).
Upper limbs
Finger-to-nose test
Assessment
The finger-to-nose test is a convenient method of assessing upper limb co-ordination:
1. Position your finger so that the patient has to fully outstretch their arm to reach it.
2. Ask the patient to touch their nose with the tip of their index finger and then touch your fingertip.
3. Ask the patient to continue to do this finger to nose motion as fast as they are able to.
Interpretation
When patients with cerebellar pathology perform this task they may exhibit both dysmetria and intention tremor:
- Dysmetria: refers to a lack of coordination of movement. Clinically this results in the patient missing the target by over/undershooting.
- Intention tremor: a broad, coarse, low-frequency tremor that develops as a limb reaches the endpoint of a deliberate movement. Clinically this results in a tremor that becomes apparent as the patient’s finger approaches yours. Be careful not to mistake an action tremor (which occurs throughout the movement) for an intention tremor.
The presence of dysmetria and intention tremor is suggestive of ipsilateral cerebellar pathology.
Rebound phenomenon
Rebound phenomenon is a reflex that occurs when a patient attempts to move a limb against resistance that has been suddenly removed.
Assessment
1. Ask the patient to close their eyes and position their arms outstretched in front of them.
2. Explain to the patient that you are going to apply some downward resistance on each arm and that they should try to maintain the current position of their arms as you apply that resistance.
3. Push downwards on one of the patient’s forearms and then immediately remove the resistance.
4. Observe the movement of the limb being assessed.
Interpretation
In healthy individuals, when the resistance is removed the limb will usually move a short distance upwards (i.e. the direction the patient was pushing towards to maintain limb position) before antagonist muscles contract and move the limb back to the original position. This is the normal reflex that results in rebound phenomenon.
An exaggerated version of rebound phenomenon is suggestive of spasticity (e.g. stroke affecting the cerebrum).
A complete absence of the phenomenon, caused by a failure of the antagonist muscles to contract, is suggestive of cerebellar disease.
Tone
Assessment
Assess tone in the muscle groups of the shoulder, elbow and wrist on each arm, comparing each side as you go:
1. Support the patient’s arm by holding their hand and elbow.
2. Ask the patient to relax and allow you to fully control the movement of their arm.
3. Move the muscle groups of the shoulder (circumduction), elbow (flexion/extension) and wrist (circumduction) through their full range of movements.
4. Feel for abnormalities of tone as you assess each joint (e.g. hypotonia).
Interpretation
Hypotonia can be caused by an ipsilateral cerebellar lesion. However, the ability to detect reduced muscle tone is highly subjective and in many cases, tone can feel ‘normal’ in cerebellar disease. As a result, it is advisable not to put too much weight on this sign or the lack of it.
Dysdiadochokinesia
Dysdiadochokinesia is a term that describes the inability to perform rapid, alternating movements, which is a feature of ipsilateral cerebellar pathology.
Assessment
1. Ask the patient to place their left palm on top of their right palm.
2. Then ask them to turn over their left hand and touch the back of it onto their right palm.
3. Now ask them to return their left hand to the original position (left palm on right palm).
4. Ask the patient to now repeat this sequence of movements as fast as they are able until you tell them to stop. It is often useful to demonstrate the sequence of movements to the patient to aid understanding.
5. Observe the speed and fluency by which the patient is able to carry out this sequence of rapidly alternating movements.
6. Repeat the assessment with the other hand.
Interpretation
Patients with cerebellar ataxia may struggle to carry out this task, with their movements appearing slow and irregular. The presence of dysdiadochokinesia suggests ipsilateral cerebellar pathology.
Lower limbs
Tone
Although tone can be re-assessed in the lower limbs, it is often not required in a cerebellar OSCE exam if you have already comprehensively assessed tone in the upper limbs.
Assessment
Briefly assess tone in the muscle groups of the hip, knee and ankle on each leg, comparing each side as you go:
1. With the patient lying on the examination couch, roll each leg to assess tone in the muscles responsible for the rotation of the hip.
2. Lift each knee briskly off the bed (warning the patient first) and observe the movement of the leg. In patients with normal tone, the knee should rise whilst the heel remains in contact with the bed (the heel will typically lift off the bed if there is increased tone).
Interpretation
Hypotonia can be caused by an ipsilateral cerebellar lesion. However, the ability to detect reduced muscle tone is highly subjective and in many cases, tone can feel ‘normal’ in cerebellar disease. As a result, it is advisable not to put too much weight on this sign or the lack of it.
Reflexes
Assess the knee-jerk reflex (L3, L4) in each of the patient’s lower limbs.
Explain to the patient that you are now going to assess their reflexes by tapping gently on their leg with a tendon hammer (it is useful to show the patient the tendon hammer at this stage).
For each of the reflexes, the patient’s lower limb needs to be completely relaxed.
Make sure to hold the tendon hammer handle at its end to allow gravity to aid a good swing.
If a reflex appears absent make sure the patient is fully relaxed and then perform a reinforcement manoeuvre by asking the patient to clench their teeth together whilst you simultaneously tap the tendon.
Assessment
1. Remove the weight from the patient’s lower limb by either supporting it or asking the patient to hang their legs over the side of the bed. Ensure the patient’s lower limb is completely relaxed before assessing the deep tendon reflex.
2. Tap the patellar tendon with the tendon hammer (making sure to hold the tendon hammer handle at its end to allow gravity to aid a good swing).
3. If a reflex appears absent make sure the patient is fully relaxed and then perform a reinforcement manoeuvre.
Interpretation
In cerebellar disease, reflexes are described as ‘pendular’, which means less brisk and slower in their rise and fall. However, similar to reduced tone, this sign is very subjective and often reflexes appear to be ‘normal’ in cerebellar disease.
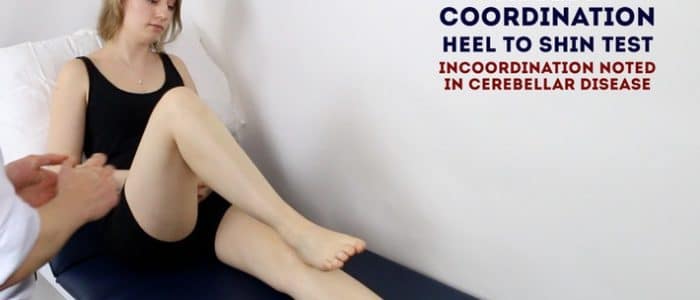
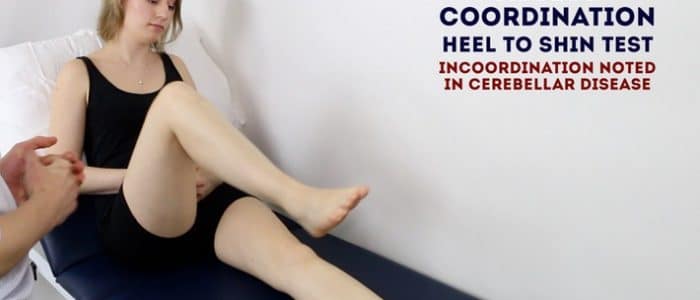
Heel-to-shin test
Assessment
The heel-to-shin test is a convenient method of assessing lower limb co-ordination:
1. Ask the patient to place their left heel on their right knee and then run it down their shin in a straight line.
2. Then ask them to return their left heel to the starting position over the right knee.
3. Now ask them to repeat this sequence of movements in a smooth motion until you tell them to stop.
4. Repeat the assessment with the right heel on the left leg.
Interpretation
Dysmetria (i.e. incoordination) whilst attempting to perform this task is suggestive of ipsilateral cerebellar pathology.
A note of caution: weakness (e.g. from an upper motor neuron lesion) can also produce apparent incoordination of this movement. As a result, power should be assessed before any diagnostic conclusions are drawn.
To complete the examination…
Explain to the patient that the examination is now finished.
Thank the patient for their time.
Dispose of PPE appropriately and wash your hands.
Summarise your findings.
Example summary
“Today I examined Mrs Smith, a 64-year-old female. On general inspection, the patient appeared comfortable at rest, with normal speech and no other stigmata of cerebellar disease. There were no objects or medical equipment around the bed of relevance.”
“Gait was normal and there was no evidence of nystagmus.”
“Assessment of the limbs revealed normal tone, reflexes and co-ordination.”
“In summary, these findings are consistent with a normal cerebellar examination.”
“For completeness, I would like to perform the following further assessments and investigations.”
Further assessments and investigations
- Full neurological examination including the cranial nerves and the upper and lower limbs.
- Neuroimaging (e.g. MRI head): if there are concerns about space-occupying lesions or demyelination.
- Formal hearing assessment (including pure tone audiometry): if there are concerns about vestibulocochlear nerve function (e.g. acoustic neuroma).
Reviewer
Dr Gemma Maxwell
Neurology Registrar