- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Introduction
A 62-year-old man attends the emergency department with abdominal distension, abdominal pain and vomiting. Work through the case to reach a diagnosis.
UK Medical Licensing Assessment (UKMLA)
This clinical case maps to the following UKMLA presentations:
- Abdominal distension
- Acute abdominal pain
- Vomiting
History
Presenting complaint
“I’ve got stomach pain and my belly feels really swollen.”
History of presenting complaint
When did it start?
“I noticed it getting swollen yesterday night but it looks worse this morning”
Has anything like this happened before?
“No”
Do you have any pain in your abdomen?
“Yes”
Where is the pain?
“Feels like it’s mostly around my belly button but everywhere is sore”
When did the pain start?
“I started getting twangs of pain yesterday evening after dinner”
What were you doing when the pain started?
“Nothing, I was just sat on the sofa after eating”
What does the pain feel like?
“Like a tight-squeezing pain that gets really sharp and then eases off”
Does the pain go anywhere else?
“No”
Have you vomited since this started?
“I’ve vomited a couple of times this morning”
Was there any blood in the vomit?
“No”
Have you noticed any weight loss recently?
“No”
Have you had any change in your bowel habits?
“I last opened my bowels 3 days ago which is a little unusual”
Have you still been passing flatus/wind?
“I can’t remember if I’ve passed any wind today.”
Has the pain changed or progressed since it started?
“I got the first squeeze of pain yesterday evening and then it seems to get better and worse in waves every so often. My stomach feels generally sore all the time though.”
Have you taken any pain relief? And has it helped?
“I’ve not been able to keep any painkillers down.”
Are you able to eat still?
“I tried to have some cereal this morning but I was sick and it seemed to make the pain come on worse”
What would you score the pain out of 10?
“At the minute it’s about a 6, but at times it’s been a 10/10”
For more information, see the Geeky Medics guide to abdominal pain history taking.
Other parts of the history
Past medical and surgical history
- Have you got any other medical problems?
Specifically, ask:
- Have you ever had any surgery on your abdomen?
- Have you ever had anything like this happen before?
“I had surgery on my belly about 30 years ago after a car accident. I’m not sure what happened exactly but I’ve got this big scar down the middle. I get achey knees and hips but other than that I’m fine.”
Medication history/allergies
- Do you take any regular medication?
- Do you have any allergies?
“I take paracetamol and naproxen sometimes for my joint pains but nothing else. I’m not allergic to anything”
Family history
- Do any medical problems run in the family?
“Both my parents have had heart attacks but nothing else that I can think of”
Social history
- Do you live with anyone?
- Do you still work/what did you used to do for work?
- How do you manage at home?
- Do you smoke?
- Have you ever smoked?
- Do you drink alcohol? If yes, how many drinks would you say you have in a week?
“I live with my wife. I’m normally independent and do work as a gardener from time to time but I’m thinking about retiring. I don’t smoke and share a bottle of wine with my wife at the weekend.”
Clinical examination
Examination findings
- The abdomen is significantly distended, with evidence of previous surgery.
- There are no obvious masses or herniae seen or stigmata of liver disease.
- Cullen’s and Grey-Turner’s signs are negative.
- There are no stomas present.
- There is general abdominal tenderness on light palpation.
- There is no guarding or rebound tenderness, and no obvious masses felt.
- Deep palpation is not tolerated as it becomes increasingly painful and the patient feels nauseous.
- There is no palpable hepatosplenomegaly, and Murphy’s sign is negative.
- The kidneys, aorta and bladder are not palpable.
- There is no hepatosplenomegaly on percussion, and the bladder is not apparently distended.
- There is no shifting dullness.
- There is no significant tenderness on percussion.
- High-pitched bowel sounds are heard. There are no aortic or renal artery bruits heard.
Abdominal scar
An image of the patient’s abdomen is shown below.
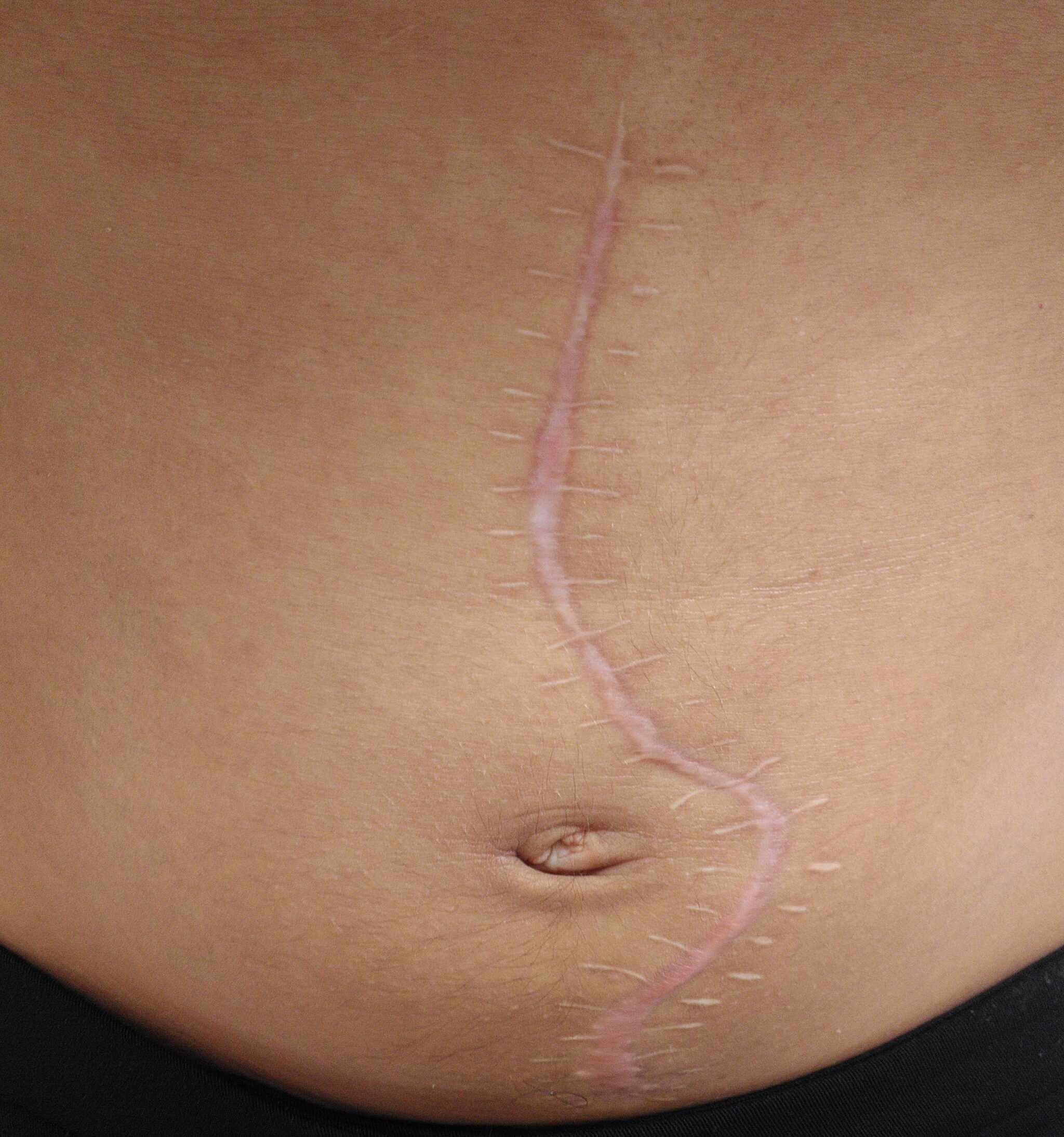
There is a midline laparotomy scar, in keeping with the patient’s previous emergency abdominal surgery.
Investigations
A CT abdomen/pelvis is the most appropriate investigation to establish a definitive diagnosis. This gives a cross-sectional view of the abdominal contents and can identify pathology as well as potentially identifying underlying aetiology.
CT is the imaging modality of choice for patients presenting with an acute surgical abdomen particularly if diagnoses such as ischaemic bowel, diverticulitis, malignancy, or bowel obstruction are suspected.
Diagnosis
Small bowel obstruction is the most likely diagnosis with the combination of abdominal distension, abdominal pain, vomiting, and absolute constipation.
Adhesions are the most likely cause in this patient with a history of previous abdominal surgery. Other less likely underlying causes include hernias, inflammatory bowel disease (Crohn’s disease or ulcerative colitis), and malignancy.
Management
In adhesional small bowel obstruction without signs of ischaemia or strangulation, conservative management via the ‘drip and suck’ approach is reasonable in the first instance.
This involves placing a wide-bore NG tube, giving intravenous fluids, keeping the patient nil-by-mouth, monitoring fluid balance with a urinary catheter, and ensuring adequate analgesia.
A water-soluble contrast (e.g. barium) study is indicated here. An x-ray is taken around 6 hours after ingestion to assess for passage of the contrast through to the colon. There is some suggestion of a therapeutic benefit associated with this although this is controversial.
If the contrast has not passed through to the colon after 6 hours it is unlikely that the patient will settle with conservative management and should be prepared for an operation. If, however, there is good transition of contrast through the bowel then ongoing conservative management is appropriate.
Outcome
Later that day, the patient begins to experience constant, worsening abdominal pain. He becomes increasingly tachycardic and spikes a temperature. A serum lactate level is measured and is significantly elevated.
The rise in serum lactate in combination with constant, worsening abdominal pain suggests that the patient is developing ischaemic bowel. This means that they have failed conservative management and require urgent surgery in the form of an emergency laparotomy to attempt to lyse the adhesions, decompress the bowel, and assess for necrotic/non-viable tissue and need for bowel resection.
Editor
Dr Jess Speller
References
- Jessica Raphaela. Emergency Laparotomy Scar. License: [CC BY-SA]
- Patient UK. Abdominal Pain. January 2023. Available from: [LINK]




