- 📖 Geeky Medics OSCE Book
- ⚡ Geeky Medics Bundles
- ✨ 1300+ OSCE Stations
- ✅ OSCE Checklist PDF Booklet
- 🧠 UKMLA AKT Question Bank
- 💊 PSA Question Bank
- 💉 Clinical Skills App
- 🗂️ Flashcard Collections | OSCE, Medicine, Surgery, Anatomy
- 💬 SCA Cases for MRCGP
To be the first to know about our latest videos subscribe to our YouTube channel 🙌
Introduction
A 23-year-old woman attends the emergency department with a headache and neck pain. Work through the case to reach a diagnosis.
UK Medical Licensing Assessment (UKMLA)
This clinical case maps to the following UKMLA presentations:
- Headache
- Neck pain/stiffness
History
Presenting complaint
“I’ve had this awful headache and just can’t get rid of it, and my neck is really sore too”
History of presenting complaint
When did the headache start?
“About 4 days ago”
What were you doing when it started?
“Just going about my day really, I can’t think of anything that set it off specifically”
Where do you feel the headache?
“It started at the back of my head but now I feel it throughout”
Can you describe the pain?
“Throbbing”
Does the pain travel or radiate anywhere?
“Down the back of my head to my neck”
Has the pain changed since it started?
“Yes, it has been progressively worsening”
Does anything relieve the headache?
“Lying down in a quiet room with the lights off”
Does anything worsen it?
“Bright lights, loud sounds”
On a scale of 1 to 10, 10 being the worst, how severe is the pain?
“5/10 at the moment”
Did you hit your head or suffer a head injury?
“No”
Have you taken any medication?
“Paracetamol, but it didn’t do much”
There are several red flag features that are important to ask about when taking a headache history:
Do you have a fever?
“I’ve had a fever of 38.4oC”
Do you feel confused or disorientated?
“My brain feels foggy”
Do you have any nausea, or have you vomited?
“I vomited once this morning”
How is your appetite?
“I have no appetite”
Have you had any changes to your eyesight?
“I feel a pressure in my eyes and bright lights bother me”
Have you had any changes to your hearing?
“I am very sensitive to loud noises”
Is anyone else at home feeling sick?
“I live with 6 housemates who are all nursing students. All are well”
Does anyone else have similar symptoms to you?
“No”
Have you been around anyone else who is unwell?
“I have placement in hospitals and I have been working with sick children for the last 3 weeks”
Clinical examination
- General examination
- Basic observations
- Neurological examination – including upper limb neurological examination, lower limb neurological examination, and cranial nerve examination
- Cardiovascular examination
Examination findings
- HR 118, RR 18, BP 102/54, Oxygen saturations 95% on air, Temperature 38.6oC
- GCS 14/15 (E4V4M6)
- No focal neurological deficit
- Pupils equal and reactive to light, 3mm
- Reflexes intact
- Normal tone
- Prolonged capillary refill time (>2 secs)
- Heart sounds normal
- Rash on lower limbs
Lower limb rash
While examining the patient, you find the rash shown below.
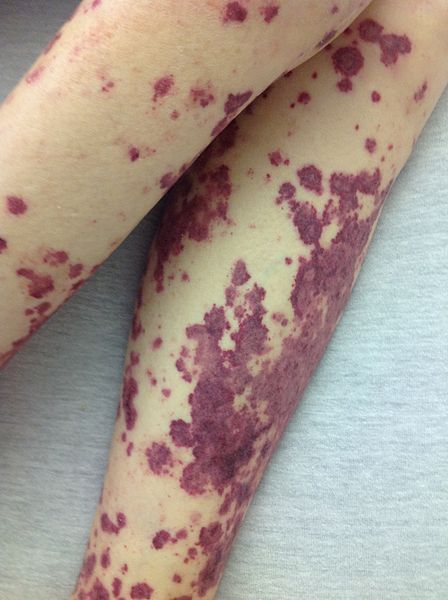
Non-blanching petechiae or purpura
Investigations
- Blood glucose measurement – this is always indicated in patients with altered consciousness.
- ECG – due to the patient’s tachycardia
Contraindications to LP include:
- Suspicion of raised intracranial pressure
- Anticoagulant therapy
- Thrombocytopaenia or other clotting disorders
- Suspicion of a spinal abscess
- Risk of herniation (i.e. Arnold-Chiari malformation)
- Acute spinal cord trauma
- Congenital spinal abnormalities
In these circumstances, imaging with CT or MRI should happen before considering lumbar puncture.
Diagnosis
- Meningitis: fever, headache, non-blanching rash, photophobia, and phonophobia are all highly suggest meningitis.
- Encephalitis: although this patient is disoriented, there are no features suggestive of impaired brain function (personality changes, behavioural changes, impaired speech).
- Cerebral abscess: this patient has no known risk factors (HIV, immunosuppression, traumatic head injury, chronic sinusitis) and has no focal neurological symptoms, so a cerebral abscess is less likely
- Tick-borne infection (Lyme disease): there is a reduced likelihood of tick-borne infection as she has no known exposure to wooded areas
- Influenza or other viral illness: symptoms are more suggestive of CNS infection
- CNS malignancy: the acute nature of symptoms is more suggestive of an infective aetiology
Lumbar puncture results
The results of the patient’s LP are as follows:
- Appearance: Turbid
- Protein: 300 mg/dL (Elevated)
- Glucose: 1.5 mmol /L (Low)
- Glucose CSF: Serum ratio: 0.40 (Low)
- WCC: 1.5 x 10^9/L (High)
- Cell predominance: Neutrophils
Bacterial meningitis. The most common organisms in this age group as neisseria meningitidis, streptococcus pneumoniae, and haemophilus influenzae type B.
Management
This patient should be managed as a potential sepsis patient, and the sepsis six should be started (IV fluids, oxygen if required, and empiric antibiotics). They should also receive antipyretics, analgesia, and nutrition support if needed.
For confirmed meningococcal cases, prophylactic antibiotics are indicated for close contacts (e.g. housemates) within 24 hours (usually ciprofloxacin or rifampicin).
Complications
Hearing loss is the most common complication seen in survivors of acute bacterial meningitis. Other complications include seizures, motor deficits, cognitive impairment, hydrocephalus, and visual disturbances.
Editor
Dr Jess Speller
References
- DrFO.Jr.Tn. Petechial rash. License: [CC BY-SA 3.0].
- NICE CKS. Meningitis – bacterial meningitis and meningococcal disease. Updated July 2019. Available from: [LINK]
- Van de Beek et al. Clinical features and prognostic factors in adults with bacterial meningitis. March 2005. Available from: [LINK]
- Patient.info. Lumbar Puncture. Updated October 2015. Available from: [LINK]




